
Presenting problems in
gastrointestinal disease


It is defined
as difficulty in swallowing
It must be distinguished from:
Globus sensation
Odynophagia.
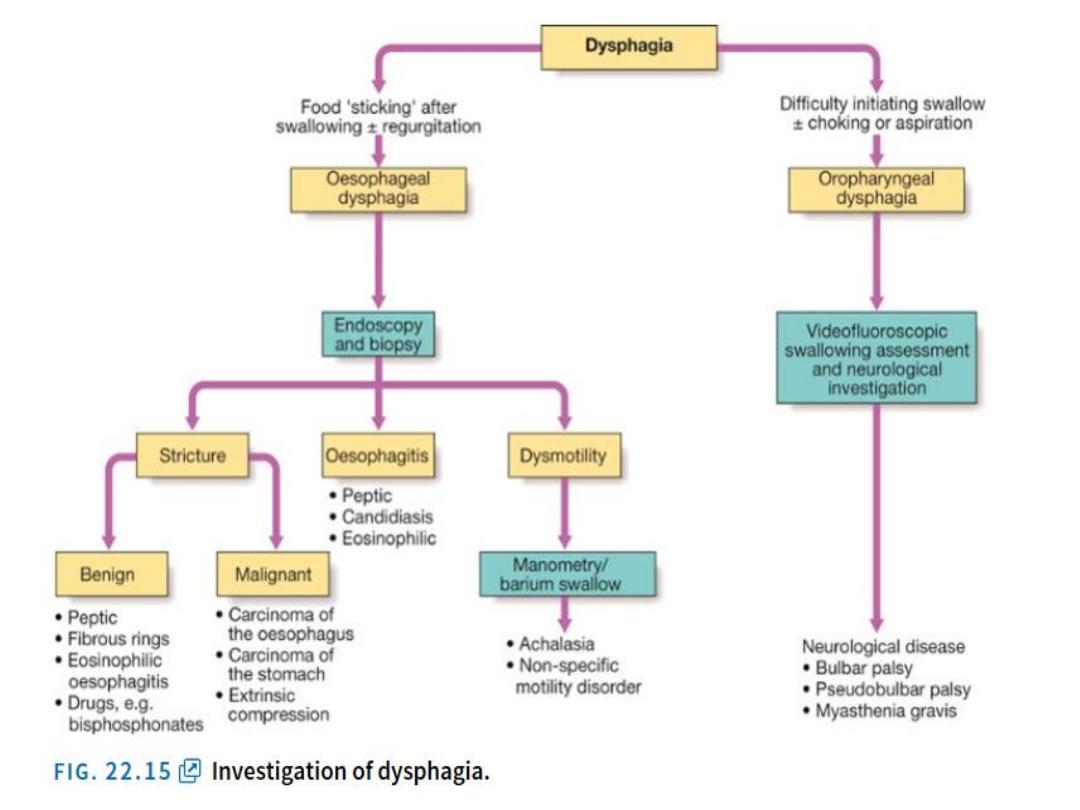

All esophageal dysphagia need
endoscopy .
Esophagitis & stricture could be
caused by
eosinophilic esophagitis
&
drugs
e.g bisphosphonates

M
y
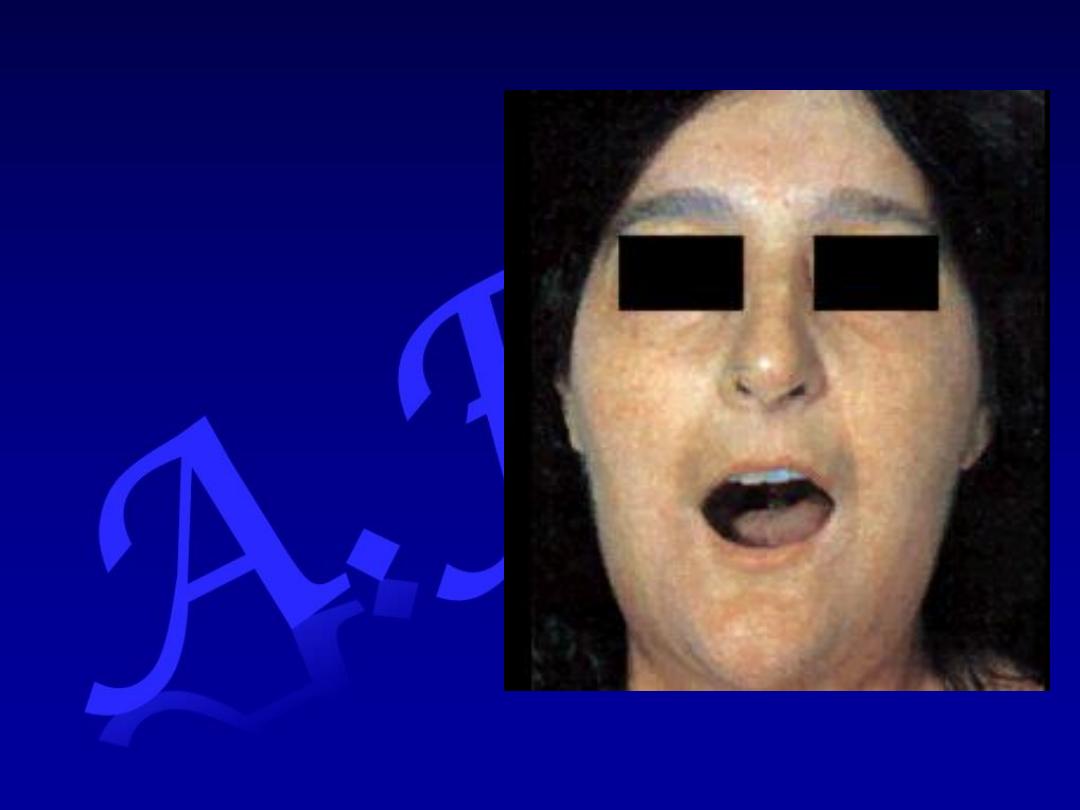
Systemic
sclerosis
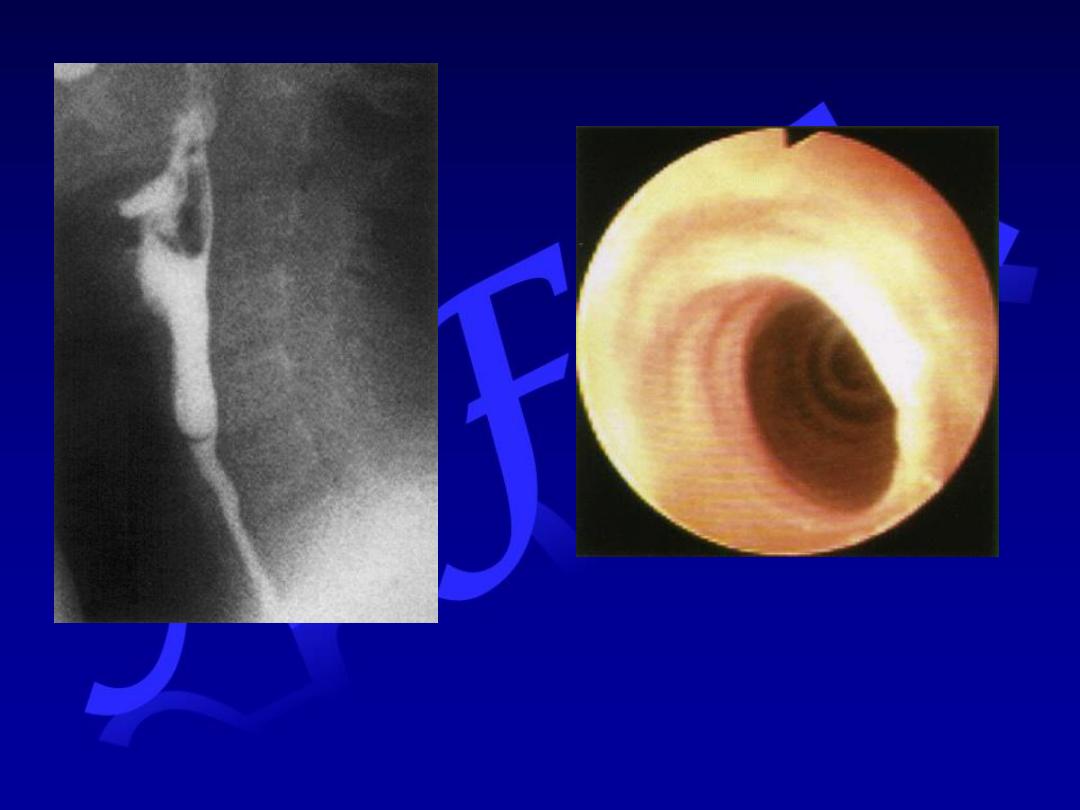
Sideropenic Web
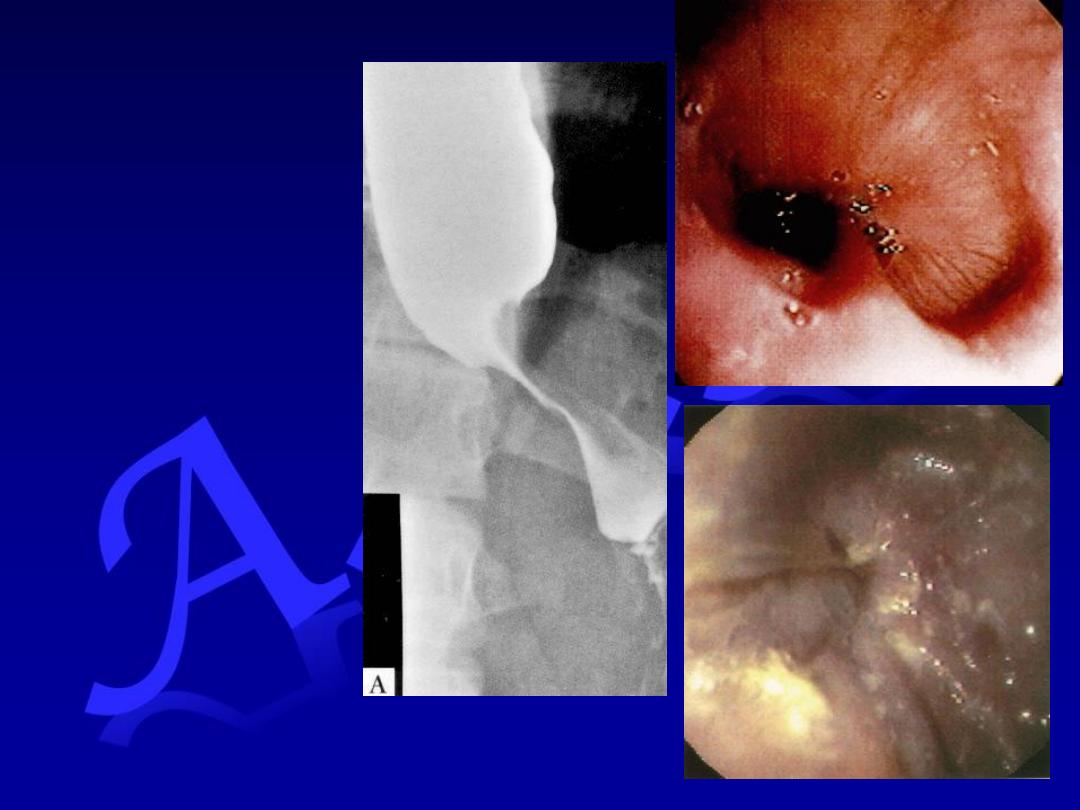
Achalasia
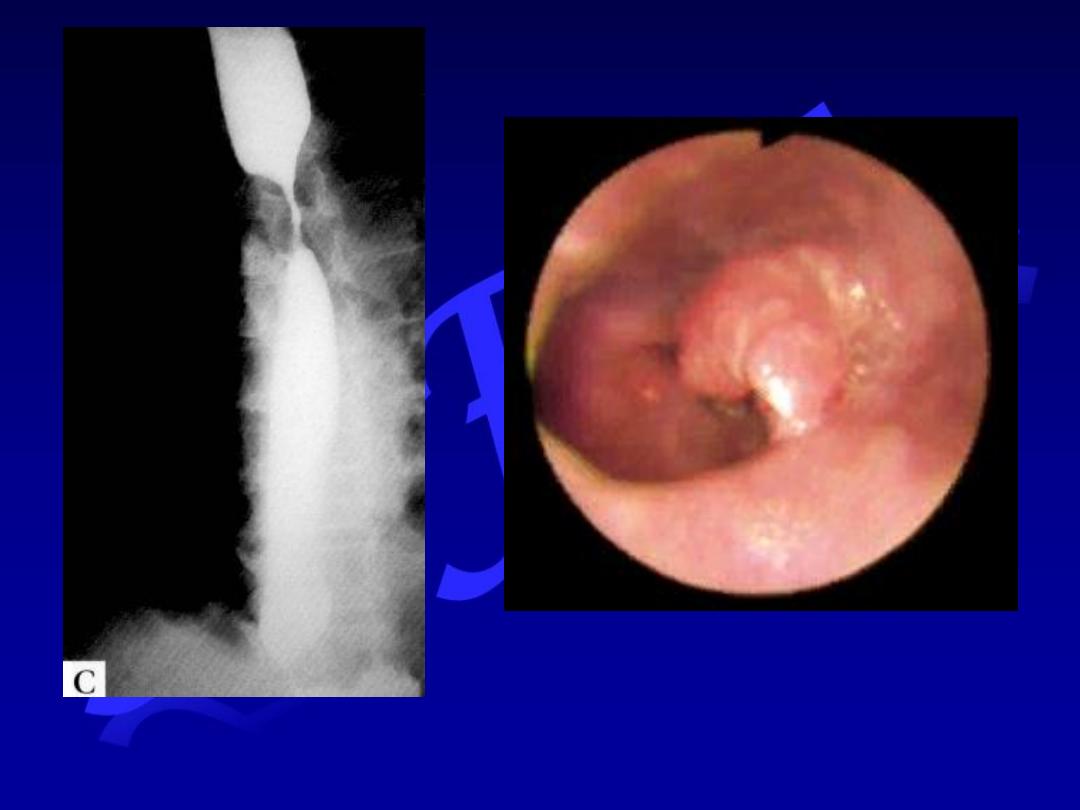
Malignant stricture
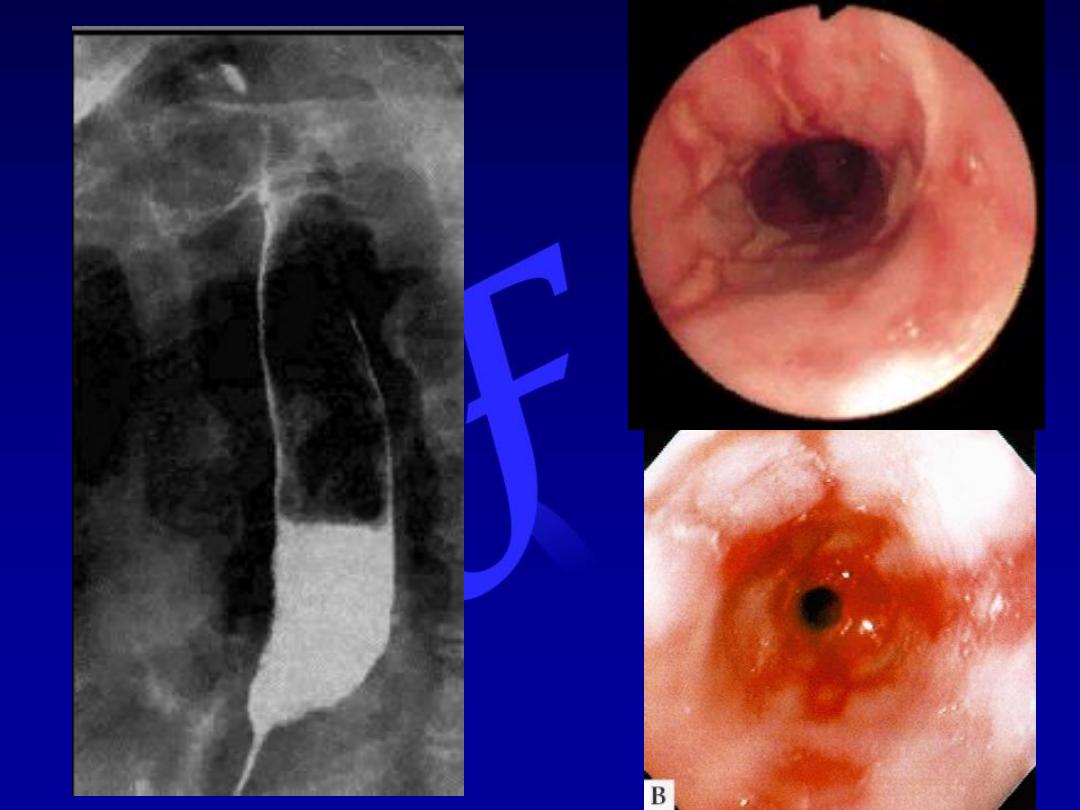
Peptic
stricture


Dyspepsia
(indigestion) is a collective term for any
symptoms thought to originate from the upper GIT.
Although symptoms often correlate poorly with the
underlying diagnosis, a careful history is important to:
Elicit symptoms classical of specific disorders like peptic
ulcer.
Detect alarm features requiring urgent investigation
Detect atypical symptoms more suggestive of other disorders
e.g. myocardial ischemia
.

Upper GI disorders:
Peptic ulcer disease
Acute gastritis
Gallstones
Motility e.g.
esophageal
spasm
Functional
(non-ulcer
dyspepsia & IBS)
Other GI disorders:
Pancreatic disease
(cancer,
chronic pancreatitis)
Hepatic disease
(hepatitis,
metastases)
Colonic carcinoma

Systemic disease:
Renal failure
Hypercalcemia
Drugs:
NSAIDs
Iron & potassium supplements
Corticosteroids
Digoxin
Others
:
Alcohol
Psychological e.g. anxiety, depression

Weight loss
Anemia
Vomiting
Hematemesis and/or malena
Dysphagia
Palpable abdominal mass
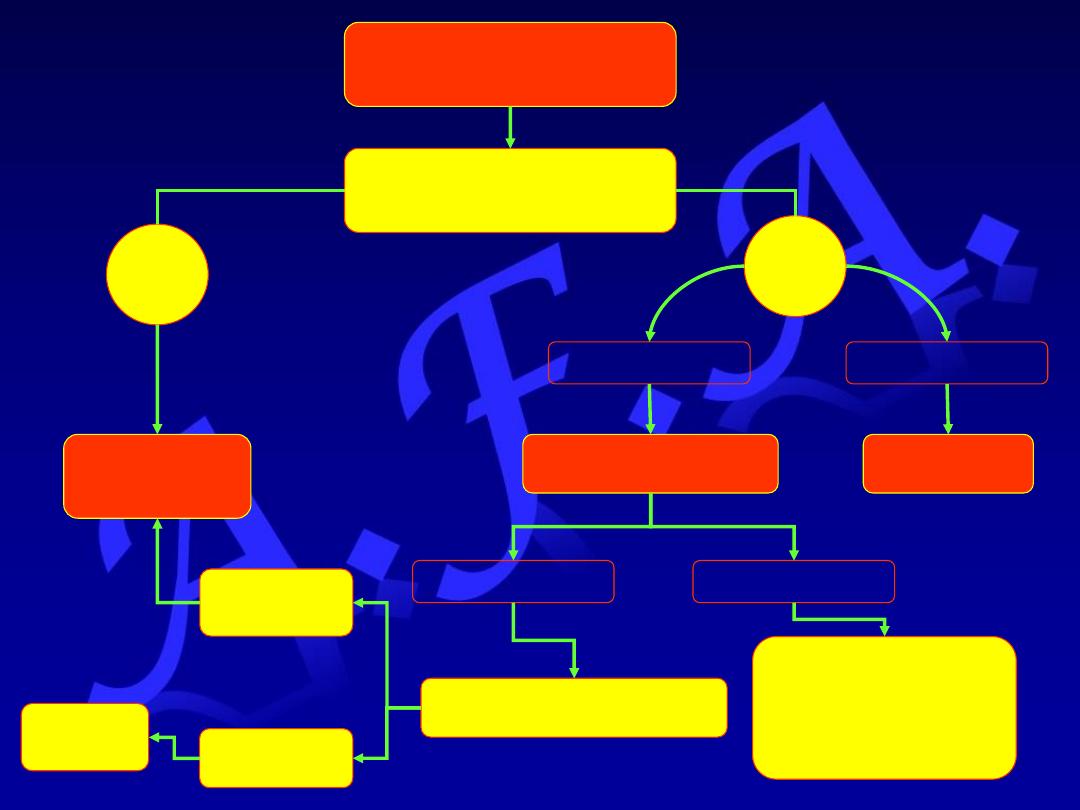
Dyspepsia
Are there
“alarm features”?
No
Yes
Endoscopy
> 55 years
< 55 years
Endoscopy
Test for H pylori
Negative
Positive
Treat
Symptomatically
or
Consider
other diagnosis
H pylori eradication
Symptoms
resolve
Symptoms
persist
No
follow up

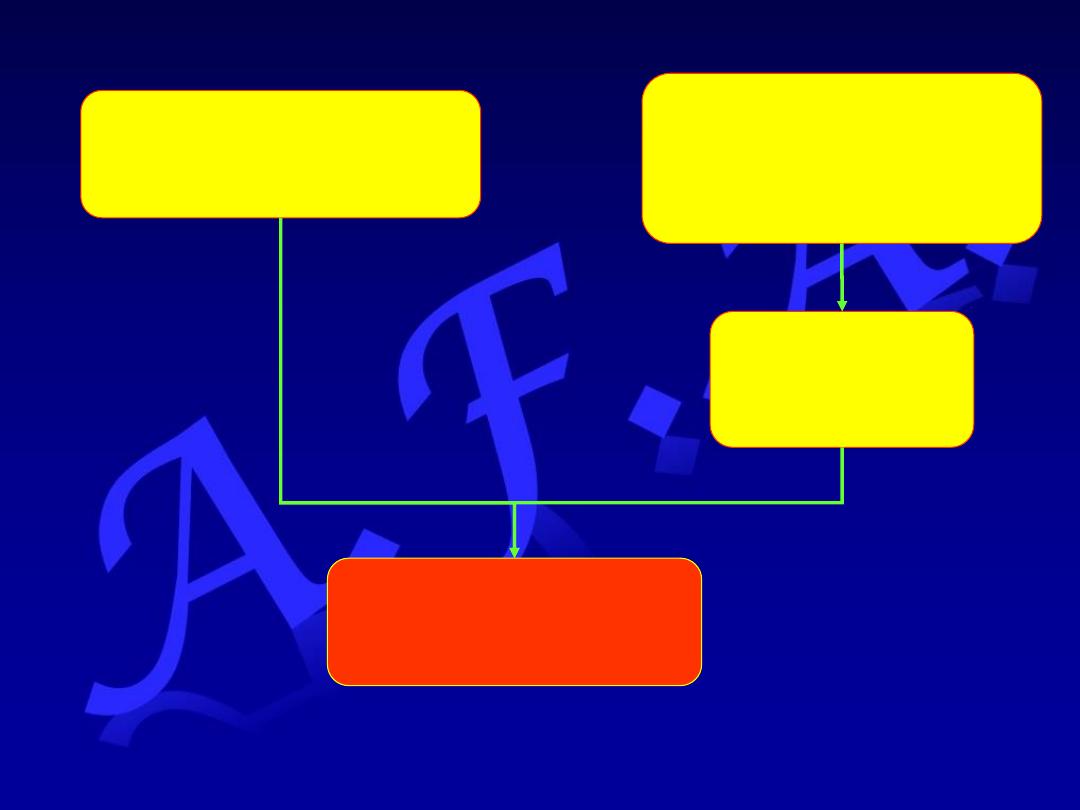
Synchronous contraction
of the diaphragm,
intercostal muscles,
& abdominal muscles
Increases
intra-abdominal
pressure
Relaxation of the lower
Esophageal sphincter
Forcible ejection of
Gastric contents

Infections:
Gastroenteritis
Hepatitis
Urinary tract infection
Drugs:
NSAIDs
Antibiotics
Opiates
Digoxin
Cytotoxic drugs
Gastroduodenal disease:
Chronic peptic ulcer
disease (± gastric outlet
obstruction)
Gastric cancer
Gastroparesis e.g.
diabetes, scleroderma,
drugs

Acute abdominal
disorders:
Appendicitis
Cholecystitis
Pancreatitis
Intestinal obstruction
CNS disorders:
Vestibular neuritis
Migraine
Meningitis
Raised intracranial
pressure
Metabolic:
Diabetic ketoacidosis
Uremia
Addison’s disease.
Others:
Any severe pain e.g.
myocardial infarction.
Psychogenic
Alcoholism
pregnancy

Vomiting is usually
associated with:
Nausea
Retching
Salivation
Anorexia
Or dyspepsia
You must distinguish
between:
True vomiting & regurgitation
Acute & chronic vomiting.
You must ask about:
Abdominal pain
Fever
Diarrhea
Relationship to food
Drug ingestion
Headache
Vertigo
Weight loss

Examination may reveal:
Signs of dehydration, fever & infection.
Evidence of abdominal mass
Evidence of peritonitis
Evidence of intestinal obstruction
Neurological signs including:
Papilledema
Nystagmus
Photophobia
Neck stiffness.
Other findings suggestive of:
Alcoholism
Pregnancy or
Bulimia

GIT Bleeding
Acute Upper
GIT Hemorrhage
Lower GIT
Bleeding
Occult GIT
Bleeding

This is the most common GIT emergency
Accounting for 50-120 admissions to
hospital per 100 000 of the population
each year in the United Kingdom.
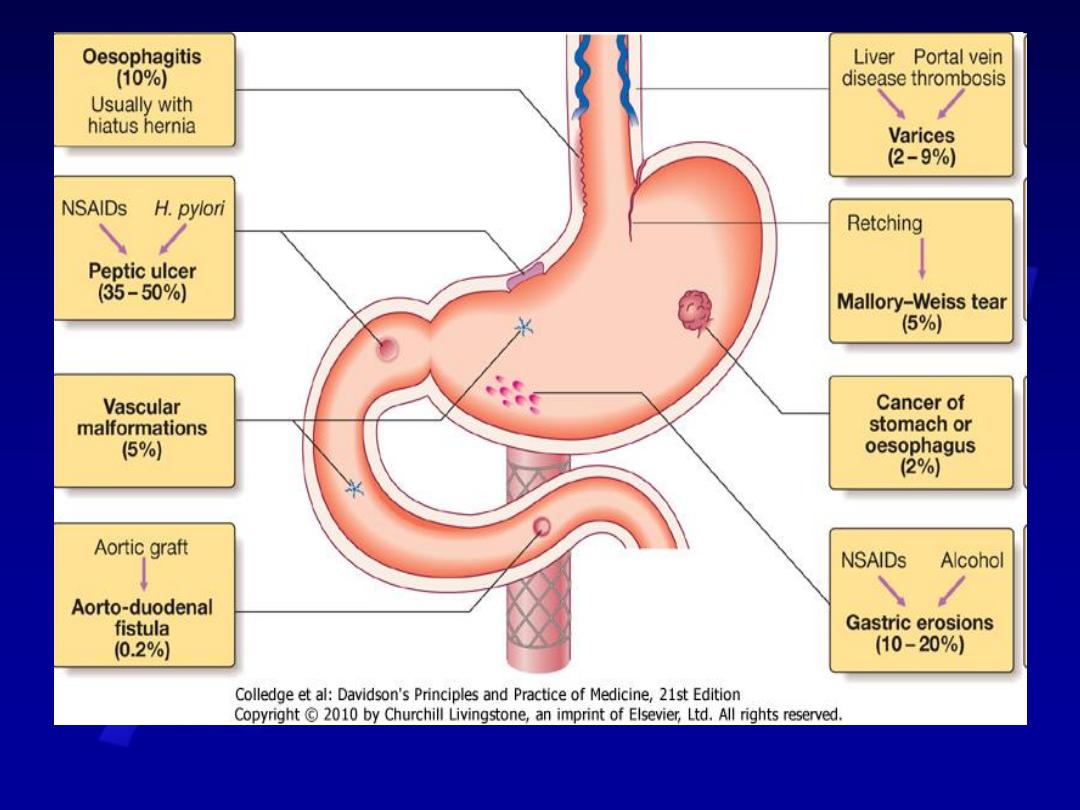

Comments
%
Diagnosis
Dyspepsia or history of peptic
ulcer
Bleeding may be precipitated
with NSAIDs or alcohol
35-50%
Peptic ulcer
Associated with NSAIDs &
Alcohol
10-20%
Gastric
erosions
Heartburn not invariable &
bleeding usually not severe
10%
Esophagitis
Follows vomiting or
retching e.g. after alcohol
binge
5%
Mallory
Weis tear

Comments
%
Diagnosis
Associated with aortic valve
disease or hereditary
hemorrhagic telangiectasia
5%
Vascular
malformations
Usually with evidence of
liver disease
2-4%
Varices
Chronic blood loss
usually present
2%
Carcinoma
(esophagus
or stomach)
Consider in any patient
who presents after aortic
graft surgery
1%
Aorto-enteric
fistula

Hematemesis may be:
– Red with clots when bleeding is profuse
OR
– Black “Coffee ground” when bleeding is less severe.
Syncope
Symptoms of anemia (chronic bleeding).
Melaena is the term used to describe the passage of
black, tarry stools containing altered blood. It is due to:
– Bleeding from the upper GIT (usually)
– Hemorrhage from the right side of the colon (occasionally)
Hematochezia (maroon or bright red stool) may be found
sometimes in cases of severe acute upper GIT bleeding.
Acute upper GIT
Bleeding
Resuscitation
Intravenous
access
Endoscopy
Initial clinical
assessment
Oxygen
Blood Tests
Monitoring

The first step is to gain intravenous access
using at least one large bore canula.

Define circulatory status:
– Severe bleeding causes tachycardia, with hypotension
and oliguria
– The patient is cold, sweating and may be agitated.
Seek evidence of liver disease:
– Jaundice
– Cutaneous stigmata
– Hepatomegaly
– Ascites
Define comorbidity (cardio-respiratory,
cerebrovascular & renal):
– They might be worsened by upper GIT bleeding
– They increase the hazards of Endoscopy & surgical
operations.

Full Blood Count:
– Chronic or Subacute bleeding may cause
anemia
– Hb concentration might be normal in cases of
sudden , major bleeding until hemodilution
occurs.
Urea & electrolytes.
Liver function tests
Prothrombin time: (if there is clinical
suggestion of liver disease or in
anticoagulated patients)
Cross matching of at least 2 units of blood.

IV crystalloid or colloid:
– They are given to restore blood volume:
Blood transfusion if:
– The patient is shocked
– Hb concentration < 10 gm/dl.
Normal saline must be avoided in patients with
liver disease
Central Venous Pressure (CVP) monitoring
(severe bleeding, patients with heart disease)
– It help to define the volume of fluid replacement
– It help in identification of rebleeding.

This should be given by facemask to all
patients in shock

Should be carried out after adequate resuscitation
Can reach diagnosis in 80% of cases
Can be used in treatment of patients with major
endoscopic stigmata of recent hemorrhage
including:
– Active spurting hemorrhage
– Visible vessel (pseudo-aneurysm)
Endoscopic treatment modalities include:
– Thermal modality e.g. heater probe
– Injection of dilute adrenalin into the bleeding point
– Application of metallic clips

Endoscopic therapy are useful for:
– Stopping active bleeding
– Preventing rebleeding
– Avoiding the need for surgery
Endoscopic therapy is also used for:
– Varices
– Vascular malformations
– Mallory-Weiss tears.

If endoscopy is normal despite active bleeding:
– Radiolabelled red cell scanning or visceral
angiography (if the patient is actively bleeding by at
least 1 ml/minute)
– Colonoscopy (for bleeding of lesser severity) – the
most common cause is vascular malformations
–
99
Tc-pertechnate scan may show bleeding from
Meckel’s diverticulum. Wireless cap.prior to enterosc.
• Patients are closely observed with hourly:
•Pulse rate
•Blood pressure
•Urine output

An urgent surgical operation is undertaken
when:
– Endoscopic hemostasis fails to stop active
bleeding
– Rebleeding occurs on:
One occasion in an elderly or frail patient
Twice in younger, fitter patients.

ACUTE UPPER GIT HEMORRHAGE
role of endoscopic therapy
Meta-analysis of 21 RCTs shows that
endoscopic therapy (injection of adrenalin
into the bleeding point, application of
thermal energy or electrocoagulation)
reduces:
– Ulcer rebleeding rate
– The need for urgent surgery
– Hospital mortality rates.

Bleeding Ulcers
adjunctive drug therapy
“intravenous proton pump inhibitor”
infusions, when given to patients who
have been subjected to endoscopic
therapy for major peptic ulcer hemorrhage,
reduce:
– Rebleeding rate
– Need for surgery
– BUT NOT mortality

Mortality after admission to hospital is
approximately 10%
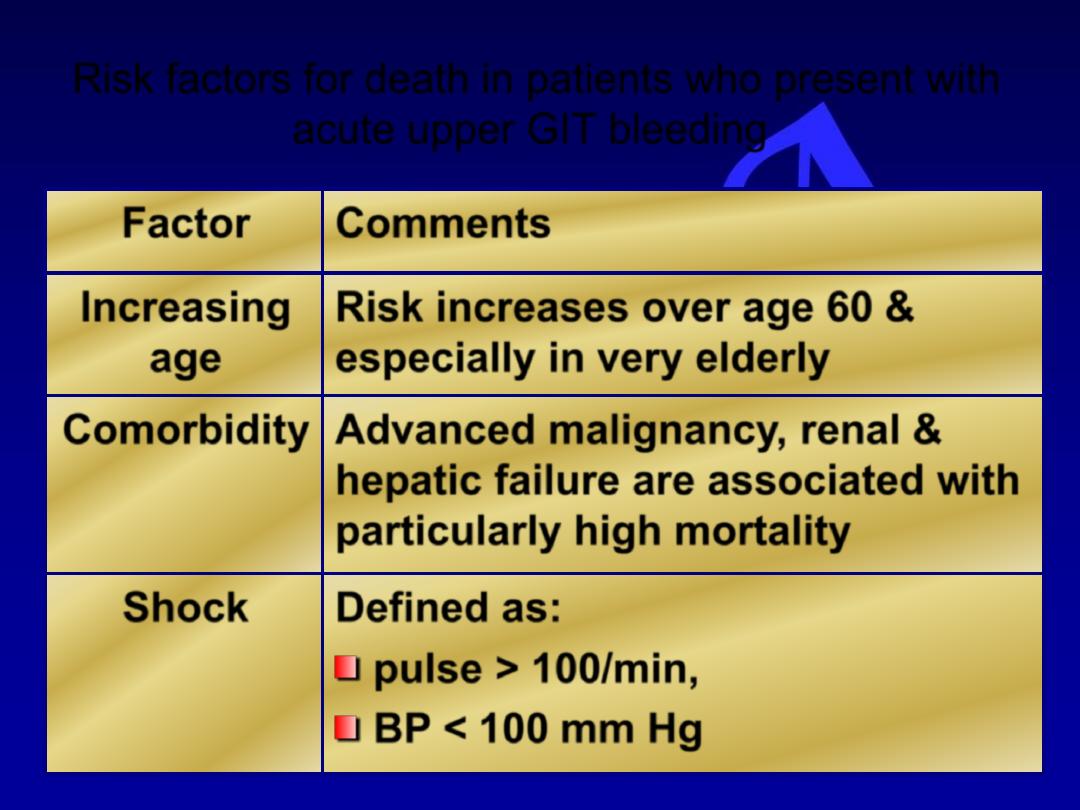

Risk factors for death in patients who present with
acute upper GIT bleeding
Comments
Factor
Risk increases over age 60 &
especially in very elderly
Increasing
age
Advanced malignancy, renal &
hepatic failure are associated with
particularly high mortality
Comorbidity
Defined as:
pulse > 100/min,
BP < 100 mm Hg
Shock

Risk factors for death in patients who present with
acute upper GIT bleeding
Comments
Factor
Varices & cancer have the worst
prognosis
Diagnosis
Active bleeding & non-bleeding
visible vessel at Endoscopy are
associated with a high risk of
continuing bleeding
Endoscopic
findings
Associated with 10 folds rise in
mortality
Rebleeding*
*defined as fresh hematemesis or melena associated
with shock or fall of Hb > 2 gm/dl over 24 hours


It may be due to hemorrhage from:
– Small bowel
– Colon
– Anal canal
You must distinguish between:
– Profuse acute bleeding
– Chronic or subacute bleeding

Severe acute:
– Diverticular disease
– Angiodysplasia
– Ischemia
– Meckel’s diverticulum
Moderate,
chronic/subacute:
– Anal disease e.g.
fissure, hemorrhoids
– Inflammatory bowel
disease
– Carcinoma
– Large poylps
– Angiodyplasia
– Radiation enteritis
– Solitary rectal ulcer

This is an unusual medical emergency
Patients present with profuse red or
maroon diarrhea and with shock
Diverticular disease:
– It is the most common cause
– Acute bleeding is due to erosion of an
artery within the mouth of a diverticulum
– Bleeding almost always stops
spontaneously.

Angiodysplasia:
– It is disease of elderly, in which vascular malformations
develop in the proximal colon
– It is most commonly seen in patients receiving
anticoagulants following aortic valve replacement.
– Can be acute and profuse bleeding
– It usually stops spontaneously but usually recurs.
– Diagnosis:
Colonoscopy: vascular spots (reminiscent of spider naevi)
Visceral angiography: Bleeding into the intestinal lumen & an
abnormal large draining vein
Laparotomy with on-table colonoscopy
– Treatment:
Endoscopic thermal ablation
Right hemicolectomy (sometimes necessary in severe cases).

Ischemia:
– It is due t occlusion of the inferior mesentric
artery
– It presents with abdominal colic and rectal
bleeding
– It should be considered in patients
(particularly the elderly) who have evidence of
generalized atherosclerosis.

Meckel’s diverticulum:
– Meckel’s diverticulum with ectopic gastric
epithelium may ulcerate and erode into a
major artery.
– The diagnosis should be considered in
children or adolescent present with profuse or
recurrent lower GIT bleeding
– Meckel’s scan is sometimes positive
– The diagnosis is commonly made by
laparotomy only at which time the diverticulum
is excised

It is extremely common at all ages
It is usually due to hemorrhoids or anal fissures
Hemorrhoidal bleeding is:
– Bright red
– Occurs during or after defecation
– Proctoscopy is used to reach diagnosis
– Colonoscopy or barium enema is necessary to
exclude coexisting colorectal carcinoma, is indicated
in:
Patients who also have altered bowel habits
All patients presenting over 40 years of age.
Anal fissure should be suspected when fresh
rectal bleeding and anal pain occur during
defecation

Occult means that blood or its breakdown
products are present in the stool but can
not be seen
It may reach 200 ml/day
It causes iron deficiency anemia
It signifies serious GIT disease
The most important cause is colorectal
carcinoma
Diagnosis initially by fecal occult blood
(FOB) test

DIARRHOEA
Acute Diarrhea
< 10 d infective ,drugs ( antibio. , NSAID,
PPI,Cytotoxic )
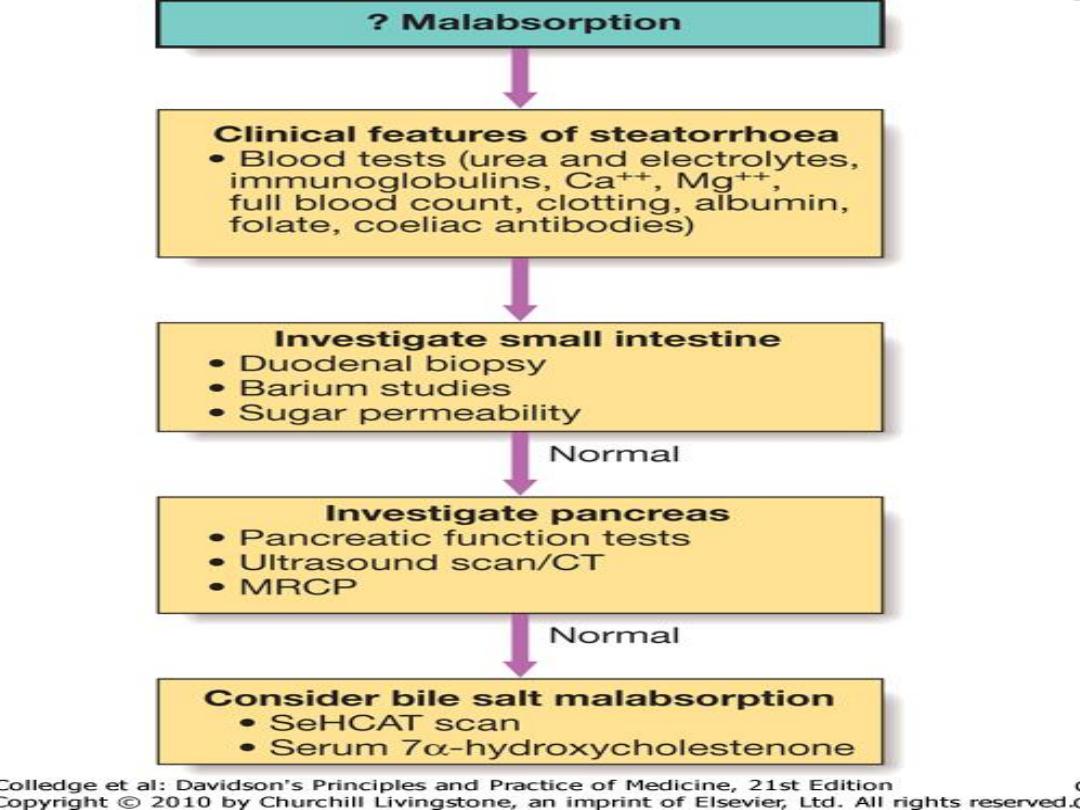
Chronic or Relapsing Diarrhea
Colonic Small Bowel Malabsorption
Clinical feature ,causes , investigation

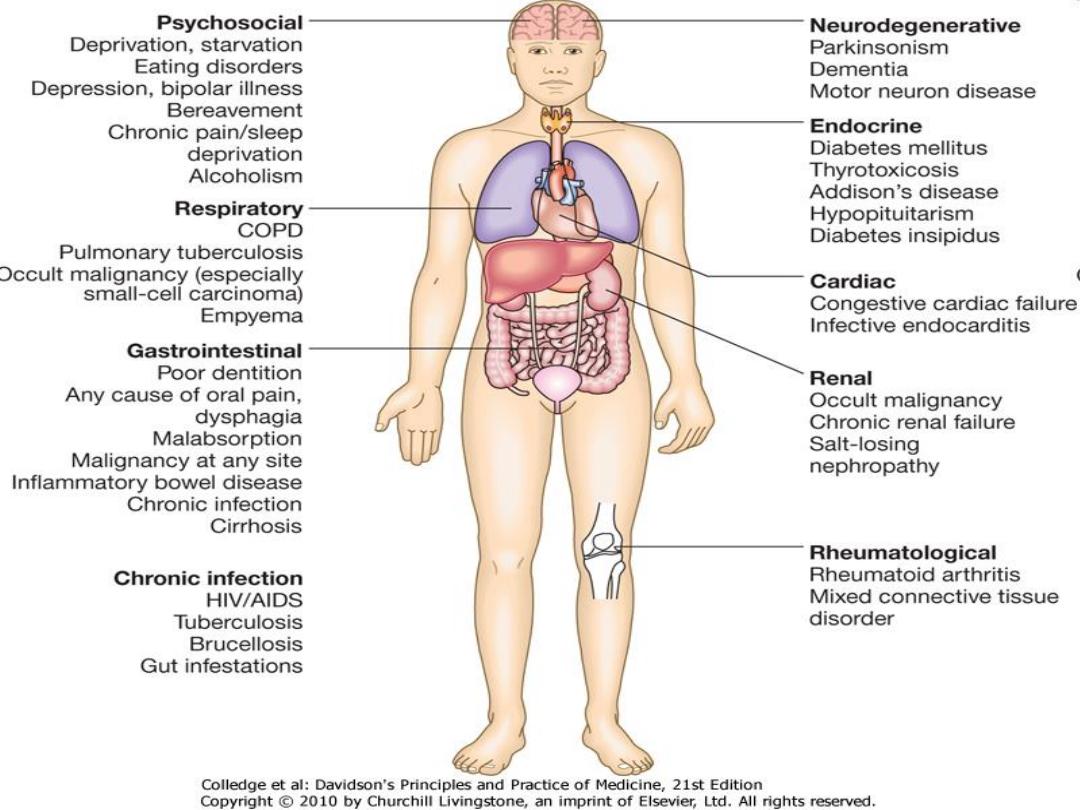
Loss of
weight

Gastro Esophageal
Reflux Disease
GERD

GERD resulting in heartburn affects
approximately 30% of the general
population
Gastroesophageal reflux
Defective
Esophageal Clearance
Dietary
Factors
Hiatus Hernia
Abnormal lower Esophageal Sphincter
•Reduced tone
•Abnormal relaxation
Delayed gastric
Emptying
Increased
intra-abdominal
pressure
Reflux of
acid pepsin
(bile)

Abnormalities of
Lower Esophageal sphincter
reduced lower esophageal sphincter tone
inappropriate sphincter relaxation

Hiatus Hernia
Occurs in 30% of the population over the age of 50 years
Often asymptomatic
Heartburn & regurgitation may occur
Gastric volvulus may complicate large para-esophageal
hernias
It causes GERD because:
– The pressure gradient between the abdominal & thoracic cavities
is lost
– The oblique angle between the cardia and esophagus
disappears
Almost all patients who develop esophagitis, Barret’s
esophagus or peptic strictures have hiatus hernia

Delayed esophageal clearance
Defective esophageal peristaltic activity
It is a primary abnormality
Poor esophageal clearance leads to
increased acid exposure time

Gastric Contents
– Gastric acid is the most important esophageal
irritant
– There is close relationship between acid
exposure time & symptoms
Defective gastric emptying

Dietary & environmental factors
Material that cause relaxation of the lower
esophageal sphincter:
– Dietary fat
– Chocolate
– Alcohol
– Coffee
There is little evidence to incriminate
smoking or NSAIDs as causes of GERD

Clinical features
Heartburn & Regurgitation:
– Often provoked by:
Bending
Straining
Lying down
Waterbrash (Salivation due to reflex salivary gland
stimulation as acid enter the gullet)
History of weight gain
Chocking due to laryngeal irritation by refluxed fluid
Odynophagia & dysphagia
Atypical chest pain which:
– Might be severe
– Might mimic anginal chest pain
– Is due to reflux induced esophageal spasm.
