parenchymal lung disease
Dr. Ghazi F. HajiSenior lecturer of cardiology
Al-Kindy College of Medicine
1
Agenda
@Diffuse parenchymal lung diseasesIdiopathic pulmonary fibrosis,(cryptogenic fibrosing alveolitis)
Sarcoidosis and granulomatous disorder with vasculitis *DPLD due to systemic inflammatory disease
@Lung diseases due to organic dusts
Hypersensitivity pneumonitis (extrinsic allergic alveolitis)
@Lung diseases due to inorganic Dusts(asbestosis,silicosis)
@Pulmonary eosinophilia and vasculitide
@Lung diseases due to irradiation and drugs
2
True or false
3
True or false
4
Definition of DPLD
The diffuse parenchymal lung diseases (DPLDs) are a heterogeneous group of conditions affecting the pulmonary interstitium and/or alveolar lumen.5
Classification
DPLDDiffuse parenchymal lung diseases
Idiopathic interstitial pneumonias
Sarcoidosis and granulomatous disorder WITH VASCULITISDPLD due to systemic inflammatory disease
Rare interstitial lung diseases
Idiopathic pulmonary fibrosis
6
Idiopathic pulmonary fibrosis (IPF)
@was previously known as cryptogenic fibrosing alveolitis(CFA).
It is relatively rare with a mean onset in the late sixties and is more common in males.
@The cause is unknown but cigarette smoking, chronic aspiration, antidepressants, wood and metal dusts and infections, e.g. Epstein–Barr virus, may play a part.7
Pathogenesis & Pathology
Disruption of the alveolar epithelium and basement membrane lead to activate inflammatory cells, which release proinflammatory cytokines and chemokines, growth factors and endothelin-1 from endothelial cells that lead to A patchy fibrosis ,acute fibroblastic proliferation and collagen deposition (fibroblastic foci)8
Clinical features
The main features are :@Progressive breathlessness,
@Nonproductive cough
@Cyanosis ,
@Gross finger clubbing
@Fine bilateral end-inspiratory crackles
@ Respiratory failure, pulmonary hypertension and cor pulmonale.
A number of autoimmune diseases are seen in association with this condition likes coeliac disease, ulcerative colitis and renal tubular acidosis.
9
investigations
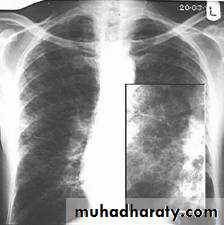
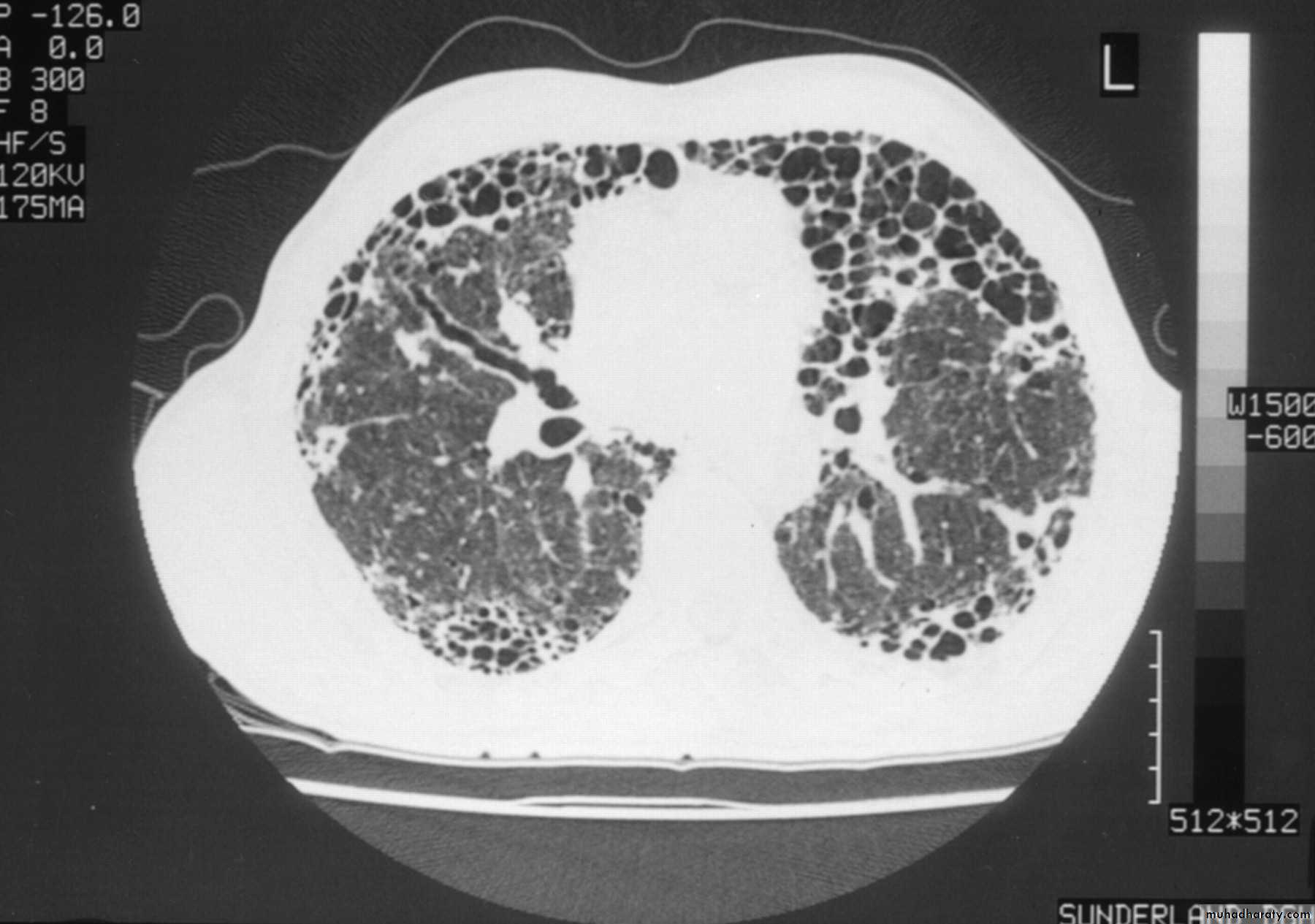
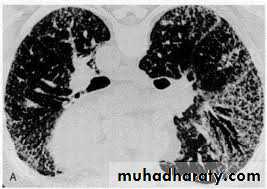
Chest X-ray -irregular reticulonodular shadowing (often maximal in the lower zones) and finally a honeycomb lung■ High-resolution CT scan (HRCT) shows characteristic features (diagnostic accuracy of approximately 90%).
■ pulmonary function tests show a restrictive ventilatory defect ,the lung volumes are reduced, the FEV1 to FVC ratio is normal to high and carbon monoxide gas transfer is reduced.
@Blood gases show an arterial hypoxaemia.
#10
@ Anti-nuclear antibodies and rheumatoid
factors are present in one-third of patients.The ESR mildly elevated
@bronchoscopy :Bronchoalveolar lavage shows increased numbers of cells, particularly neutrophils and macrophages.
■ lung biopsy :Histological confirmation is necessary in some patients..
1112
13
14
Prognosis and treatment
#The median survival time is approximately 5 years.#Treatment with prednisolone (30 mg daily) is usually prescribed for disabling disease.
#Azathioprine or cyclophosphamide may be added if there is no response.#Supportive treatment includes domiciliary oxygen therapy.
In severe disease, single lung transplantation can be offered.
15GRANULOMATOUS LUNG DISEASE Sarcoidosis
@Sarcoidosis is a multisystem disease of unknown aetiology that is characterised by the presence of non-caseating granulomas .@The condition is more frequently in northern Europe.; Arabs and Chinese are rarely affected. .
@Genetic susceptibility is supported by familial clustering;
@Sarcoidosis occurs less frequently in smokers.16
Presentation of sarcoidosis
@Asymptomatic: abnormal routine chest X-ray (∼30%) or abnormal liver function tests@Cough, exertional breathlessness
Pleural disease is uncommon and finger clubbing is not a feature.
@Erythema nodosum( Löfgren's syndrome- (BHL), )and arthralgia
@Ocular symptoms -uveitis
@Skin sarcoid (including lupus pernio)
@Superficial lymphadenopathy
@Other , e.g. hypercalcaemia, diabetes insipidus, cranial nerve palsies, cardiac arrhythmias, nephrocalcinosis
17
Investigations
@Chest X-ray changes in sarcoidosisBHL (usually symmetrical); paratracheal nodes often enlarged and pulmonary fibrosis
@Characteristic HRCT appearances include reticulonodular opacities
@pulmonary function testing :may show a restrictive defect. @Lymphopenia is characteristic and liver function tests may be mildly deranged.
@Hypercalcaemia ,Hypercalciuria may also be seen and may lead to nephrocalcinosis.
@Serum angiotensin-converting enzyme (ACE) is a non-specific marker of disease activity and can assist in follow up
@Bronchoscopy:The BAL fluid typically contains an increased CD4:CD8 T-cell ratio.
@Lung biopsy biopsies show non-caseating granulomas
.
.
18
Management
#Prednisolone is indicated 1-in presence of hypercalcaemia,2- pulmonary impairment, 3-renal impairment 4-uveitisIn patients with severe disease methotrexate (10-20 mg/week), azathioprine (50-150 mg/day) and specific TNF-α inhibitors have been effective.
#Chloroquine, hydroxychloroquine and low-dose thalidomide may be useful in cutaneous sarcoid with limited pulmonary involvement.
#Features suggesting a bad prognosis include1- age > 40 years, 2-persistent symptoms for more than 6 months, 3-the involvement of more than three organs, 4-lupus pernio
5-a stage III/IV chest X-ray.
.
19
GRANULOMATOUS LUNG DISEASEWITH VASCULITIS
The respiratory disorders associated with the presence of anti-neutrophil cytoplasmic antibodies (ANCAs)(ANCAs) are found in the acute phase of vasculitides, particularly:
Wegener’s granulomatosis
Churg– Strauss syndrome
microscopic polyangiitis (polyarteritis)
associated with neutrophil infiltration of the vessel wall.
.
20
Wegener's granulomatosis (WG) & Goodpasture's syndrome(GP)
@IN WG :upper respiratory tract manifestations include nasal discharge and crusting, saddle nose deformity..,and otitis media. Fever, weight loss and anaemia are common.Radiological features include multiple nodules and cavitation which may resemble primary or metastatic carcinoma
GP:This describes the association of pulmonary haemorrhage and glomerulonephritis, in which IgG antibodies bind to the glomerular or alveolar basement membranes
21
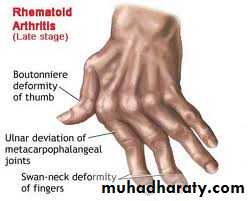
Lung diseases due to systemic inflammatory disease -Rheumatoid arthritis
@Pulmonary involvement is around 10-20%
#Pulmonary fibrosis is the most common pulmonary manifestation.
#Pleural effusion is common,Effusions are usually small and unilateral but can be large and bilateral.
# Rheumatoid pulmonary nodules might be mimic primary bronchial carcinoma..
22
Cont,
@Cavitation, Bronchitis and bronchiectasis, the potentially fatal condition called obliterative bronchiolitis may develop.@The combination of rheumatoid nodules and pneumoconiosis is known as Caplan's syndrome .
&corticosteroid therapy predisposes to infections, methotrexate may cause pulmonary fibrosis, and anti-TNF therapy may precipitate the reactivation of tuberculosis.23
24
Systemic lupus erythematosus
#Pleuropulmonary involvement is more common in SLE. Up to two-thirds of patients have repeated episodes of pleurisy, with or without effusions. Effusions may be bilateral and may also involve the pericardium. Pulmonary fibrosis is a relatively uncommon manifestation
#The chest X-ray reveals elevated diaphragms,.This condition has been described as 'shrinking lungs' and attributed to diaphragmatic myopathy.
#SLE patients with antiphospholipid antibodies are at increased risk of venous and pulmonary thromboembolism and these patients require life-long anticoagulation.
25
Lung diseases due to organic dusts
Disease results from a local immune complex reaction in the walls of the alveoli and bronchioles due to inhalation animal proteins (e.g. bird fancier's lung) or fungal antigens in mouldyHypersensitivity pneumonitis is the most common of these conditions ( called extrinsic allergic alveolitis) .
Common causes include
Farmer's lung ( Aspergillus fumigatus)
Bird fancier's lung (Avian serum proteins)
Byssinosis(Cotton)
.
26
Pathogenesis and pathology
Is consistent with both type III and type IV immunological mechanisms(Type I Immediate hypersensitivity , Type11 Antibody-mediated , Type III Immune complex-mediated Type IV Delayed type).
@Precipitating IgG antibodies may be detected in the serum
Chronic forms of the disease may be accompanied by fibrosis.
@there is a lower incidence of HP in smokers compared to non-smokers.
27
Clinical features
The acute form of the disease should be suspected when anyone who is exposed to organic dust complains, within a few hours of re-exposure to the same dust, of influenza-like symptoms such as headache, myalgia, malaise, pyrexia, dry cough and breathlessness.Chest auscultation reveals widespread end-inspiratory crackles and squeaks.
HP may progress to cause severe respiratory disability, hypoxaemia, pulmonary hypertension, cor pulmonale and eventually death.28
Investigations
@The classical chest X-ray shows typically bilateral with upper and middle lobe predominance diffuse micronodular shadowing.@HRCT is more sensitive
@Pulmonary function tests show a restrictive ventilatory defect with reduced lung volumes and impaired gas transfer,.
29
Diagnosis
Predictive factors in the identification of hypersensitivity pneumonitis1-Exposure to a known offending antigen
2-Positive precipitating antibodies to offending antigen
3-Recurrent episodes of symptoms
4-Inspiratory crackles on examination
5-Symptoms occurring 4-8 hours after exposure
30
Management
1-The patient should cease exposure to the inciting agent.Dust masks with appropriate filters may minimise exposure
2-In acute cases prednisolone should be given for 3-4 weeks, starting with an oral dose of 40 mg per day.
3-Severely hypoxaemic patients may require high-concentration oxygen therapy initially.
Most patients recover completely, but the development of interstitial fibrosis is usually accompanied by permanent disability.31
Lung diseases due to inorganic dusts
#Definition: The inhalation of inorganic dusts, fumes or other noxious substances leads to specific pathological changes in the lungs including pulmonary oedema and asthma.
#In general, prolonged exposure to inorganic dusts leads to diffuse pulmonary fibrosis (the pneumoconioses),.
#In The most important types of pneumoconiosis are coal worker's pneumoconiosis, silicosis and asbestosis Beryllium (atomic energy and electronics industries),.
@A detailed occupational history is essential
32Coal worker's pneumoconiosis
@follows prolonged inhalation of coal dust, is asymptomatic.#PMF refers to the formation of large dense masses (mainly in the upper lobes);
@ is usually associated with cough, black sputum(melanoptysis), and breathlessness. It may progress to respiratory failure and right ventricular failure.
#Caplan's syndrome describes the coexistence of rheumatoid arthritis and pneumoconiosis, with rounded fibrotic nodules 0.5-5 cm in diameter..
33
Silicosis
@Silicosis results from the inhalation of crystalline or free silica, usually in the form of quartz, by workers cutting, grinding and polishing stone.The Classic silicosis is most common and usually manifests after 10-20 years of continuous silica exposure, during which time the patient remains asymptomatic.
Typical symptoms include cough, with sputum and breathlessness..
@Radiological feature - multiple nodular opacities predominantly in the mid- and upper zones.
@Enlargement of the hilar glands with an 'eggshell' pattern of calcification
@The disease is associated with an increased risk of tuberculosis (silicotuberculosis), lung cancer;.
34
Asbestosis
$The main types of the fibrous mineral asbestos are (white asbestos), (blue asbestos) and (brown asbestos)$Patients usually present with :
exertional breathlessnessfine, late inspiratory crackles over the lower zones.
Digital clubbing (reported in 40% of patients)
.
35
Management and investigations of asbestosis:
@$The chest X-ray shows bi-basal reticulonodular shadowing and honeycombing may be present.@HRCT is more sensitive .
@Pulmonary function tests typically show a restrictive defect with decreased lung volumes and reduced gas transfer factor.
@No specific treatment is available and asbestosis is usually slowly progressive.
36Complication of asbestosis
*In advanced cases, respiratory failure and cor pulmonale may develop..*Pleural plaques
*Diffuse pleural thickening
*Acute benign pleurisy
*Carcinoma of lung About 40% of patients (who usually smoke) develop carcinoma of the lung
*Interstitial fibrosis
*Mesothelioma 10% may develop mesothelioma
37
Pulmonary eosinophilia
Pulmonary eosinophilia refers to the association of radiographic (usually pneumonic) abnormalities and peripheral blood eosinophilia(sputum or BAL).Extrinsic (cause known)
*Helminths: e.g. Ascaris, Filaria
*Drugs: nitrofurantoin, para-aminosalicylic acid )
*Fungi: e.g. bronchopulmonary aspergillosis
Intrinsic (cause unknown)
*Cryptogenic eosinophilic pneumonia
38
Pulmonary eosinophilia and vasculitides
*Churg-Strauss syndrome (diagnosed on the basis of four or more of the following features:1-Asthma,
2-Peripheral blood eosinophilia (or > 10% of a total white cell count),3-Mononeuropathy or polyneuropathy,
4-Pulmonary infiltrates,
5-Paranasal sinus disease
39
Lung diseases due to irradiation and drugs
@Drugs cause Non-cardiogenic pulmonary oedema (ARDS) Hydrochlorothiazide ,Thrombolytics (streptokinase) Aspirin and opiates (in overdose)@Drugs cause Pulmonary eosinophilia (Antimicrobials -Antirheumatic agents-Cytotoxic drugs - (Psychotropic drugs -Anticonvulsants
@Drugs cause Pleural disease (Bromocriptine, amiodarone, methotrexate, methysergide)
drugs cause SLE-phenytoin, hydralazine, isoniazid
@ Drugs cause Asthma (β-blockers, cholinergic agonists, aspirin and NSAIDs)
40
True or false
41
True or false
42
Thank you for attention
43