
Chapter 12 - Labour
161
“” Cephalopelvic disproportion (CPD) “”
It is an anatomical disproportion between the fetal head and maternal pelvis; this is when
the head is too large for the pelvis. It is a common cause of obstructed labour.
Causes
Large baby (absolute disproportion): - Hereditary factors - post maturity - diabetes
- Multiparty: each succeeding baby (up to about the 5th baby) tends to be larger and heavier
Abnormal positions (relative disproportion)
The normal fetus delivers in the occipito-anterior position. If the head is well flexed in this
position then the head is presents with the suboccipito-bregmatic diameter (9.5 cm) and
easily passes through the pelvis. Other positions e.g. occipito-posterior, brow, present a
much larger diameter (11.5 cm and 13.5 cm respectively).
Small pelvis
Abnormal shape to pelvis e.g. rickety or trefoil pelvis
Abnormality of the genital tract
- Cervix: congenital rigidity, postsurgical scarring - Vagina: congenital septum
Fibroids may rarely cause obstruction to labour
In Cephalopelvic disproportion
A large pelvis may be inadequate for a very large baby.
A small baby can negotiate a small pelvis
Extreme cases of CPD can sometimes be identified at the onset of labour.
In others a trial or test of labour is required
In a trial of labour the conclusion that labour cannot continue normally is reached before
full dilatation.
Cephalopelvic disproportion is suspected if:
- Slow or arrest of progress of labor in spite of efficient uterine contractions
- No engagement of fetal head - Poorly applied head on the cervix
- Excessive molding and caput formation
Contracted pelvis
Definition
Anatomical definition: is a pelvis in which one or more of its diameters is reduced below
the normal by one or more centimeters. Obstetric definition: It is a pelvis in which one or
more of its diameters is reduced so that it interferes with the normal mechanism of labour.
Any contraction in pelvic diameters can diminish pelvic capacity & create dystocia during labor
Chapter 12 - Labour
162
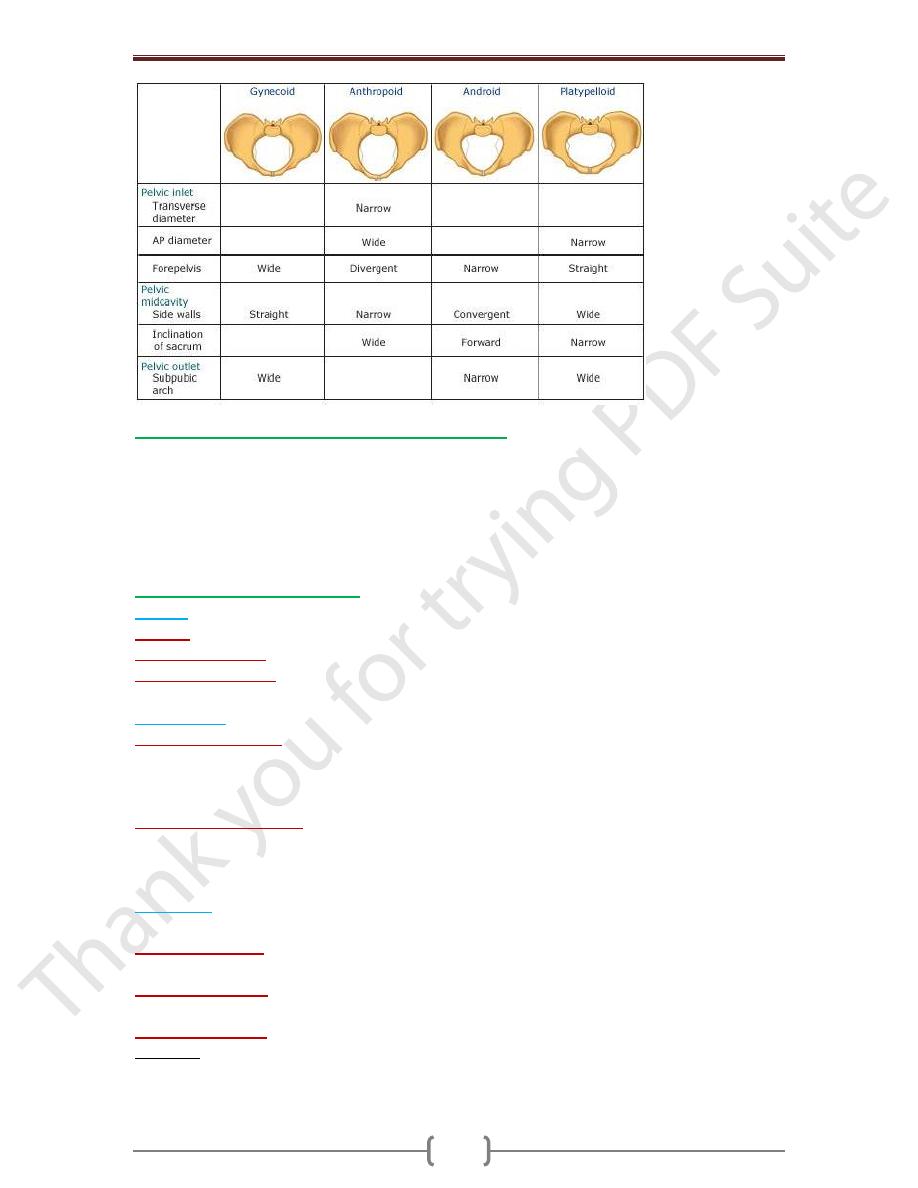
Factors influencing the size and shape of the pelvis
Developmental factor: hereditary or congenital.
Racial factor.
Nutritional: malnutrition results in small pelvis.
Sexual: as excessive androgen may produce android pelvis.
Metabolic factor: as rickets and osteomalacia.
Trauma, diseases or tumors of the bony pelvis, legs or spines
Diagnosis of Contracted Pelvis
History
o Rickets:
is expected if there is a history of delayed walking and dentition.
o Trauma or diseases
: of the pelvis, spines or lower limbs.
o Bad obstetric history
: e.g. prolonged labour ended by;
- difficult forceps, - CS or - Still birth.
Examination
o General examination:
Gait: abnormal gait suggesting abnormalities in the pelvis, spines or lower limbs.
Stature: women with less than 150 cm height usually have contracted pelvis.
Spines and lower limbs: may have a disease or lesion.
o Abdominal examination:
No engagement of the head: in the last 3-4 wks in primigra.
Pendulous abdomen: in a primigravida.
Malpresentations: are more common.
Pelvimetry
It is assessment of the pelvic diameters and capacity done at 38-39 weeks. It includes:
o Clinical pelvimetry:
Internal pelvimetry for: inlet, cavity, and Outlet.
External pelvimetry for: inlet and Outlet.
o Imaging pelvimetry
: X-ray, CT, MRI. CT & MRI are recent & accurate but expensive &
not always available so they are not in common use.
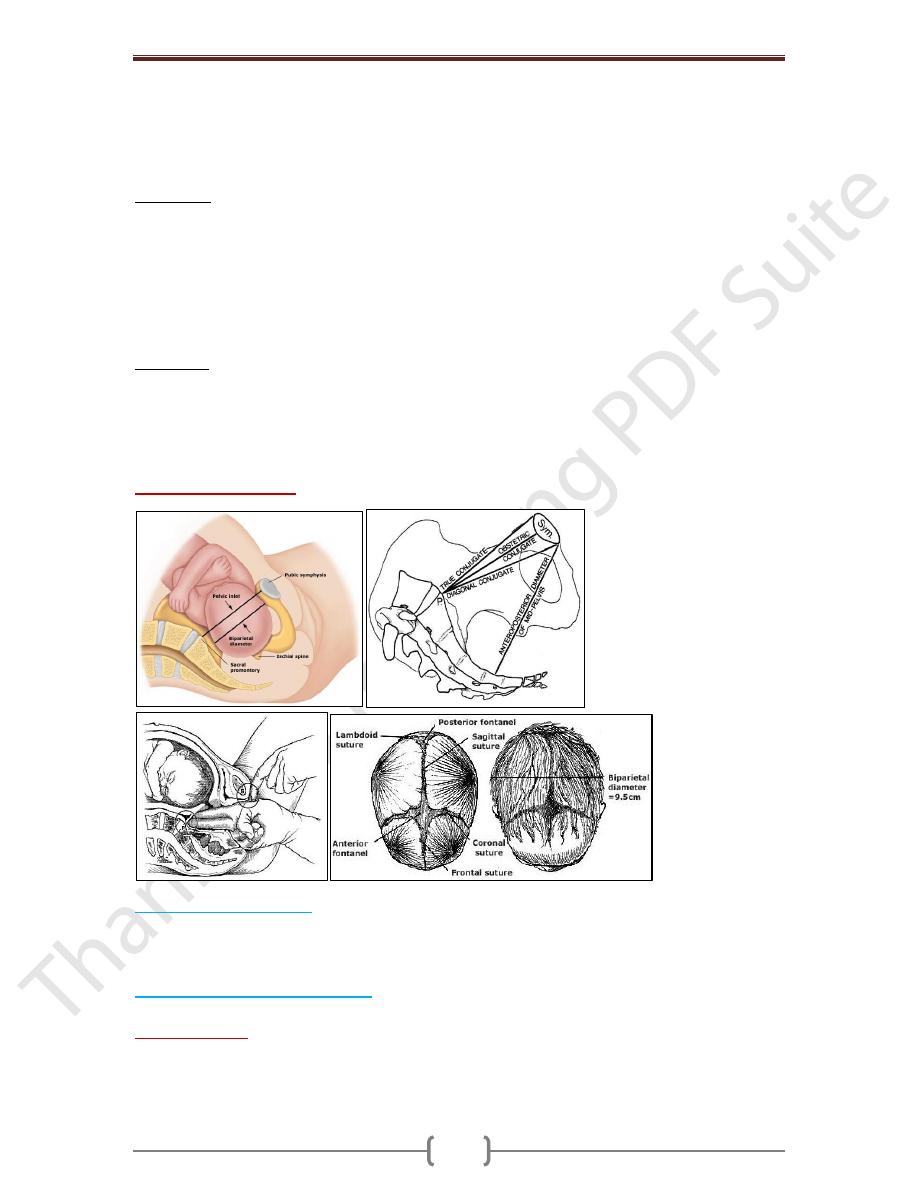
o Internal pelvimetry
is done through vaginal examination
The inlet: ̶ Palpation of the pelvic brim: The index & middle fingers are moved along
the pelvic brim. Note whether it is round or angulated, causing the fingers to dip into a V-
shaped depression behind the symphysis.
Chapter 12 - Labour
163
- Diagonal conjugate: Try to palpate the sacral promontory to measure the diagonal
conjugate. Normally, it is 12.5 cm & cannot be reached. If it is felt the pelvis is considered
contracted & the true conjugate can be calculated by subtracting 1.5 cm from the diagonal
conjugate. Contracted inlet when AP diameter is less than 10 cm or if the greatest
transvers diameter less than 12 cm
The cavity:
- Height, thickness and inclination of the symphysis.
- Shape and inclination of the sacrum.
- Side walls: To determine whether it is straight, convergent or divergent starting from the
pelvic brim down to the base of ischial spines.
- Ischial spines: Whether it is blunt, prominent or very prominent. The ischial spines can be
located by following the sacrospinous ligament to its lateral end.
- Interspinous diameter: Contracted mid pelvis if Interspinous diameter is ˂ 10 cm
The outlet:
- Subpubic angle: Normally, it admits 2 fingers.
- Bituberous diameter: Normally, it admits the closed fist of the hand (4 knuckles).
- Mobility of the coccyx. - Anteroposterior diameter of the outlet: From the tip of the
sacrum to the inferior edge of the symphysis. - Contracted outlet when narrow
subpubic angle is less than 60 & Interischial tuberous diameter is ˂ 8 cm
o Radiological pelvimetry
: indicated mainly in borderline pelvic contraction.
Cephalometry (fetal size)
Ultrasonography: is the safe accurate and easy method and can detect:
- The biparietal diameter (BPD). - The occipito-frontal diameter.
- The circumference of the head. - Abdominal circumference
Cephalopelvic disproportion tests
Are done to detect contracted inlet if the head is not engaged in the last 3-4 wks in a primigravida.
1) Pinard’s method:
The patient evacuates her bladder and rectum. The patient is placed in
semi-sitting position to bring the foetal axis perpendicular to the brim. The left hand pushes
the head downwards and backwards into the pelvis while the fingers of the right hand are
put on the symphysis to detect disproportion.

Chapter 12 - Labour
164
2) Muller - Kerr’s method:
- It is more valuable in detection of the degree of disproportion.
- The patient evacuates her bladder and rectum.
- The patient is placed in the dorsal position.
- The left hand pushes the head into the pelvis and vaginal examination is done by the right
hand while its thumb is placed over the symphysis to detect disproportion.
Degrees of Disproportion
Minor disproportion
:
The anterior surface of the head is in line with the posterior surface
of the symphysis. During labour the head is engaged due to molding and vaginal delivery
can be achieved.
Moderate disproportion (1st degree):
The anterior surface of the head is in line with the
anterior surface of the symphysis. Vaginal delivery may or may not occur.
Marked disproportion (2nd degree disproportion):
The head overrides the anterior
surface of the symphysis. Vaginal delivery cannot occur.
Management of Contracted Pelvis
It depends mainly on the degree of disproportion.
o Minor disproportion (minor degree of contracted pelvis): vaginal delivery.
o Moderate disproportion (moderate degree of contracted pelvis): trial labour, if failed do
caesarean section.
o Marked disproportion (severe or extreme degree of contracted pelvis): caesarean section.
Trial of Labour
o It is a clinical test for the factors that cannot be determined before start of labour as:
- Efficiency of uterine contractions - Molding of the head - Yielding of the pelvis & soft tissues.
o Procedure:
- Carried out in a hospital where facilities for C.S are available - Adequate
analgesia. - Nothing by mouth. - Avoid premature rupture of membranes by: rest in bed,
avoid high enema & Minimize vaginal examinations. - The patient is left for 2 hrs in the
2nd stage with good uterine contractions under close supervision to the mother and fetus.
o Suitable cases for trial of labour:
- Young primigravida of good health. - Moderate disproportion. - Vertex presentation.
- No outlet contractions. - Average sized baby.
o When trial of labor has failed:
- Failure of progress with good uterine contractions. - Development of retraction ring, pain
and tenderness over the lower uterine segment or fetal distress
o Termination of trial of labour:
Vaginal delivery: Either spontaneously or by forceps if the head is engaged.

Chapter 12 - Labour
165
Caesarean section if:
- Failed trial of labour i.e. the head did not engage or
- Complications occur during trial as fetal distress or prolapsed pulsating cord before full
cervical dilatation.
- Indications of caesarean section in contracted pelvis
1) Moderate disproportion if trial of labour is contraindicated or failed.
2) Marked disproportion.
3) Extreme disproportion whether the fetus is living or dead.
4) Contracted outlet.
5) Contracted pelvis with other indications as; elderly primigravida, Malpresentations,
or placenta praevia.
Special management:
o Forceps delivery and vacuum
o Craniotomy
o Symphisiotomy: division of the ligaments holding the pubic bones together at symphysis
pubis to produce an increase in the pelvic diameters
Complications of Contracted Pelvis
Maternal:
o During pregnancy:
- Incarcerated retroverted gravid uterus - Malpresentations – Pendulous abdomen.
- No engagement. - Pyelonephritis especially in high assimilation pelvis due to more
compression of the ureter.
o During labour:
- Inertia, slow cervical dilatation and prolonged labour.
- PROMs and cord prolapse.
- Obstructed labour and rupture uterus.
- Necrotic genito-urinary fistula.
- Injury to pelvic joints or nerves from difficult forceps deliver
- Postpartum hemorrhage.
Fetal:
- Intracranial hemorrhage. - Asphyxia. - Fracture skull.
- Nerve injuries. - Intra-amniotic infection.
Summary
• Mild (minor) degree CPD corresponds to minor degree of CP: spontaneous vaginal
delivery is the rule forceps may be needed for shortening of the 2nd stage of labour –
• Moderate degree (1st degree) CPD corresponds to moderate degree CP: trial labour if
failed CS –
• Severe degree CPD (2nd degree) corresponds to major and extreme of CP: CS is the rule
for living babies. For dead babies craniotomy is trial in major degree only if trained
obstetrician is available and CS is done in extreme degree even with dead baby
