
بسم هللا الرحمن الرحيم
Water excretion
WATER EXCRETION
• Normally,
180 L
of fluid is filtered through the
glomeruli each day, while the average daily urine
volume is about
1 L
.
• The same load of solute can be excreted per 24
hours in a urine volume of
500 mL
with a
concentration of
1400 mosm/kg
or in a volume of
23.3 L
with a concentration of
30 mosm/kg
.
• These figures demonstrate two important facts:
– first, that at least
87%
of the filtered water is
reabsorbed, even when the urine volume is 23 L; and
– second, that the reabsorption of the
remainder
of the
filtered water can be
varied
without affecting total
solute excretion.
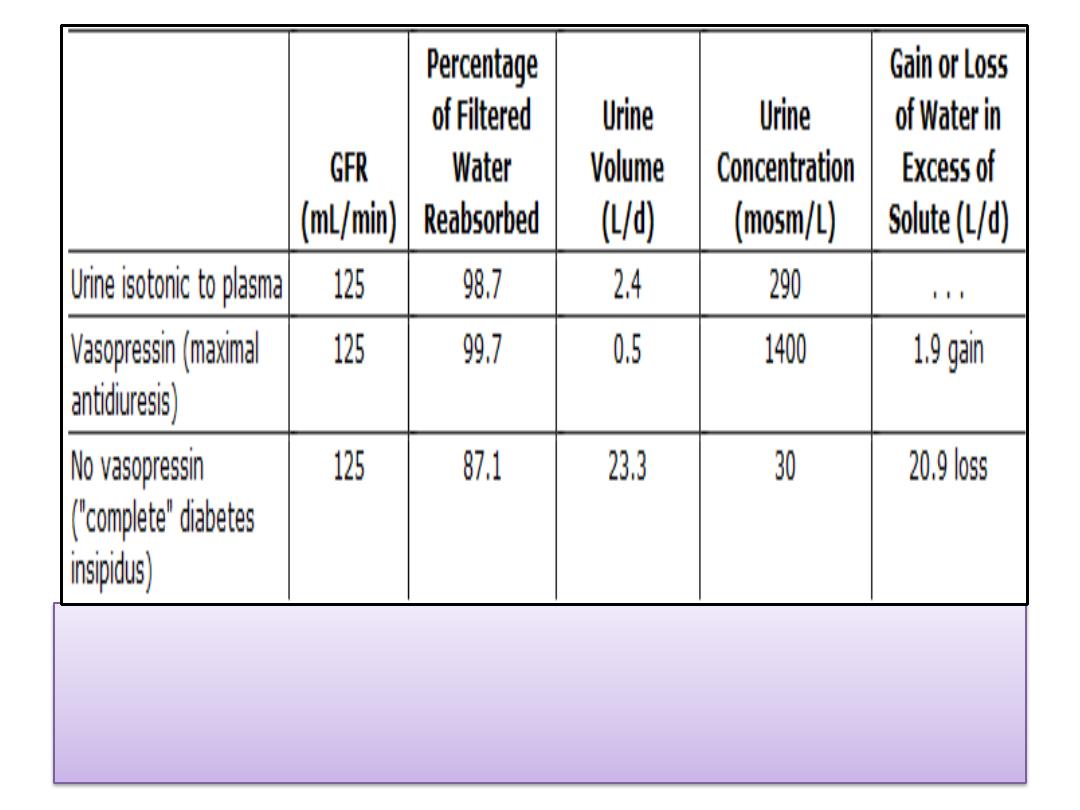
Alterations in water metabolism produced by
vasopressin in humans. In each case, the
osmotic load excreted is 700 mosm/d.
WATER EXCRETION
• Therefore, when the urine is concentrated,
water is retained in excess of solute
; and when
it is dilute, water is lost from the body in
excess of solute.
• Both facts have great importance in the
body
economy
and the regulation of the
osmolality
of the body fluids.
• A
key regulator
of water output is
vasopressin
acting
on the collecting ducts.

Aquaporins
• Research indicates that rapid diffusion of
water across cell membranes depends on
water channels
made up of proteins called
aquaporins
.
• Four aquaporins
—aquaporin-1, -2, -5, and -
9—have been characterized in humans.
• Most are found in the
kidneys
, though
aquaporin-9 is found in human
leukocytes
,
liver
,
lung
, and
spleen
; and aquaporin-5 is
found in human
lacrimal glands
.
Proximal Tubule
• Many substances are
actively transported
out of the
fluid in the proximal tubule, but fluid obtained by
micropuncture remains essentially
isosmotic
to the end
of the proximal tubule .
• Therefore, in the proximal tubule
, water moves
passively
out of the tubule along the
osmotic gradients
set up by active transport of solutes, and
isotonicity is
maintained
.
• Since the
ratio
of the concentration in tubular fluid to
the concentration in plasma
(TF/P)
of the
nonreabsorbable substance
inulin
is
2.5-3.3
at the end
of the proximal tubule, it follows that
60-70%
of the
filtered solute and
60-70%
of the filtered water have
been removed by the time the filtrate reaches this
point .
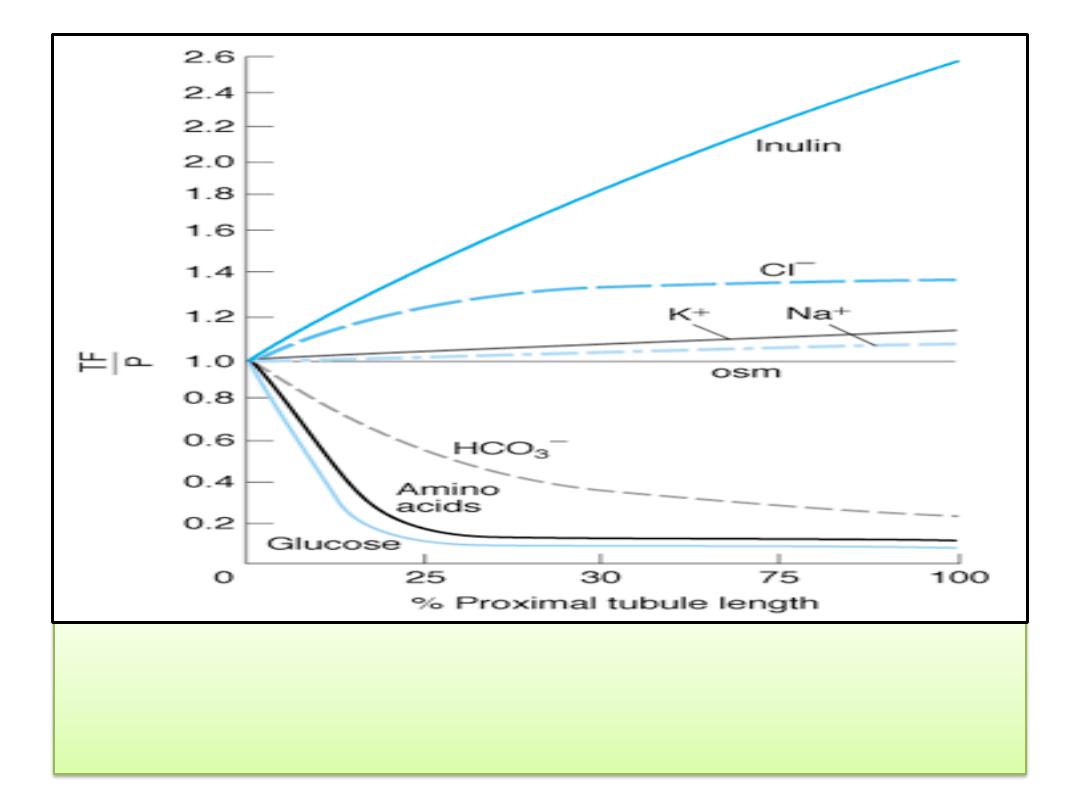
Reabsorption of various solutes in the proximal
tubule. TF/P, tubular fluid:plasma concentration
ratio.
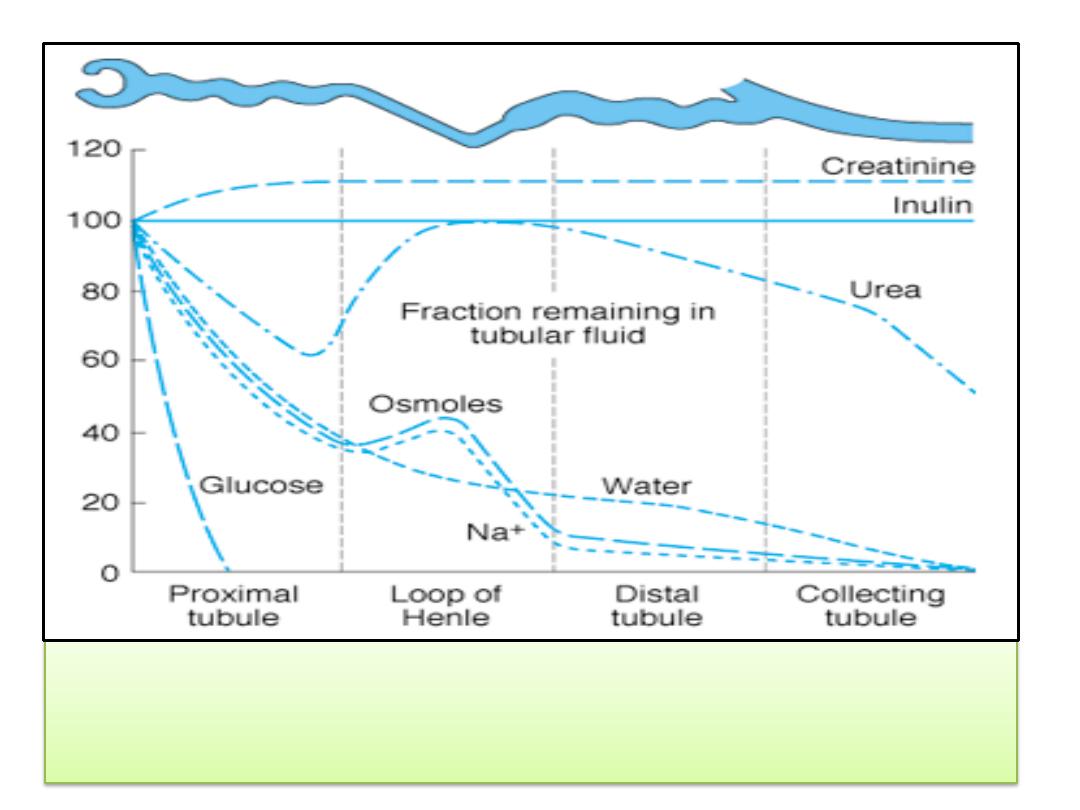
Changes in the percentage of the filtered amount of substances
remaining in the tubular fluid along the length of the nephron in the
presence of vasopressin.
Loop of Henle
• As noted , the loops of Henle of the
juxta-medullary
nephrons
dip deeply into the medullary pyramids before
draining into the distal convoluted tubules in the cortex,
and all of the collecting ducts descend back through the
medullary pyramids to drain at the
tips of the pyramids
into
the renal pelvis.
• There is a graded increase in the osmolality of the
interstitium of the pyramids
, the osmolality at the tips of
the papillae normally being about
1200 mosm/kg of H
2
O
,
approximately
four times
that of plasma.
• The
descending
limb of the loop of Henle is
permeable
to
water, but the
ascending
limb is
impermeable
.
• Na
+
, K
+
, and Cl
-
are cotransported out of the thick segment
of the ascending limb .
Loop of Henle
• Therefore, the fluid in the
descending
limb of the
loop of Henle becomes
hypertonic
as water
moves into the hypertonic interstitium.
• In the
ascending
limb it becomes more
dilute
,
and when it reaches the
top it is hypotonic to
plasma
because of the movement of Na
+
and Cl
-
out of the tubular lumen.
• In passing through the loop of Henle, another
15% of the filtered water is removed
, so
approximately 20% of the filtered water enters
the distal tubule, and the
TF/P of inulin
at this
point is about
5
.
Loop of Henle
• In the
thick ascending
limb, a carrier cotransports one Na
+
,
one K
+
, and 2 Cl
-
from the tubular lumen into the tubular
cells.
• This is another example of
secondary active transport
; the
Na
+
is actively transported from the cells into the
interstitium by
Na
+
-K
+
ATPase
in the basolateral membranes
of the cells, keeping the intracellular Na
+
low.
• The K
+
diffuses back
into the tubular lumen and back into
the interstitium via
ROMK and other K
+
channels
.
• The Cl
-
diffuses into the interstitium via ClC-Kb channels .
• This K
+
recycles across the luminal and the basolateral
membrane, while there is no transport of Na
+
and Cl
-
into
the interstitium.
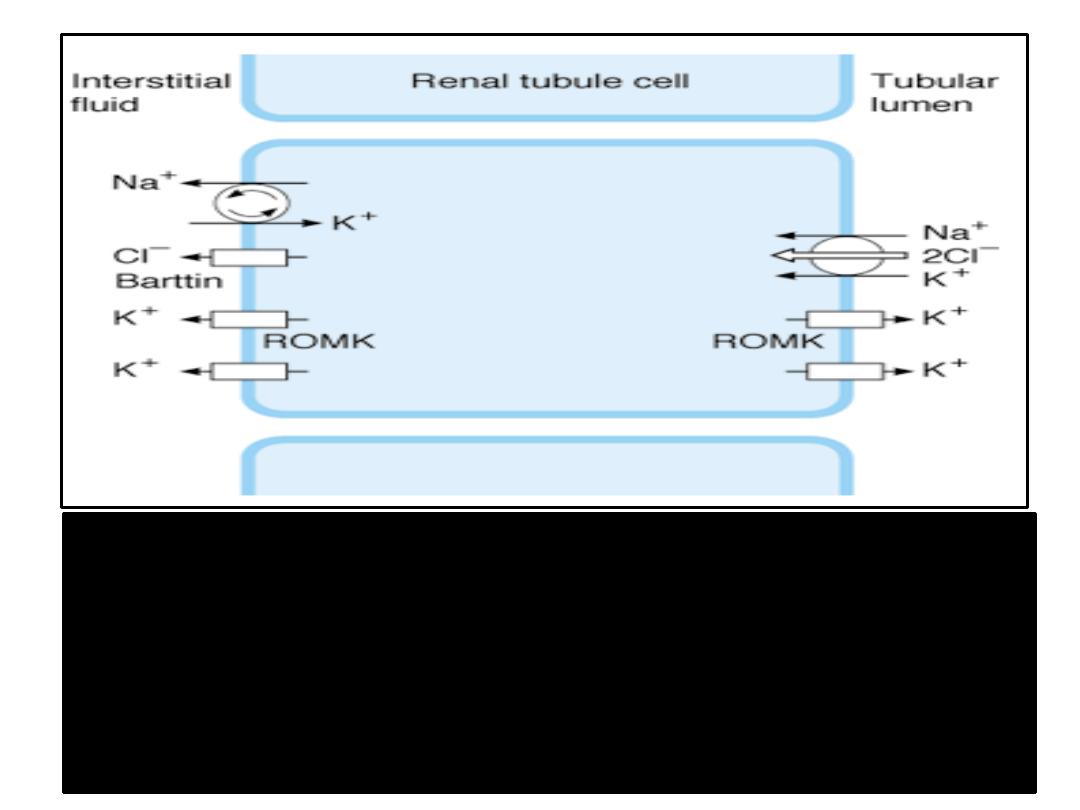
NaCl transport in the thick ascending limb of the loop of Henle. The
Na
+
, K
+
,
2Cl
-
cotransporter moves these ions into the tubular cell by secondary active
transport. Na
+
is transported out of the cell into the interstitium by
Na
+
-K
+
ATPase
in the basolateral membrane of the cell. Cl
-
exits in basolateral ClC-Kb
Cl
-
channels.
Barttin
, a protein in the cell membrane, is essential for normal
ClC-Kb function.
K
+
moves from the cell to the interstitium and the tubular
lumen by
ROMK
and other K
+
channels.
Distal Tubule
• The distal tubule, particularly its first part, is in
effect an
extension of the thick segment
of the
ascending limb.
• It is relatively
impermeable to water
, and
continued removal of the solute in excess of
solvent further dilutes the tubular fluid.
• About
5%
of the filtered water is removed in
this segment.
Collecting Ducts
• The collecting ducts have
two portions
:
– a cortical portion and
– a medullary portion.
• The changes in osmolality and volume in the collecting
ducts depend on the amount of
vasopressin
acting on the
ducts.
• This
antidiuretic hormone
from the posterior pituitary
gland increases the
permeability
of the
collecting ducts
to
water.
• The key to the action of vasopressin on the collecting ducts
is aquaporin-2.
• The effect is mediated via the
vasopressin V
2
receptor,
cyclic AMP
,
protein kinase A
, and
a molecular motor
, one of
the dyneins .
Collecting Ducts
• In the presence of
enough vasopressin
to produce maximal
antidiuresis, water moves out of the hypotonic fluid
entering the cortical collecting ducts into the interstitium of
the cortex, and the tubular fluid becomes isotonic.
• In this fashion
, as much as
10%
of the filtered water is
removed.
• The isotonic fluid then enters the medullary collecting
ducts with a
TF/P inulin
of about
20
.
• An additional 4.7% or more of the filtrate is reabsorbed into
the hypertonic interstitium of the medulla, producing a
concentrated urine with
a TF/P
inulin of over
300
.
• In humans, the osmolality of urine may reach
1400
mosm/kg
of H
2
O, almost
five times
the osmolality of
plasma, with a total of
99.7%
of the filtered water being
reabsorbed
Collecting Ducts
• When
vasopressin
is absent, the collecting duct epithelium is
relatively impermeable to water.
• The fluid therefore
remains hypotonic
, and large amounts
flow into the renal pelvis.
• In humans, the urine osmolality may be as low as
30
mosm/kg
of H
2
O.
• The
impermeability
of the distal portions of the nephron is
not absolute
; along with the salt that is pumped out of the
collecting duct fluid, about
2%
of the filtered
water
is
reabsorbed
in the absence of vasopressin.
• However, as much as
13%
of the filtered water may be
excreted, and urine flow may reach
15 mL/min
or more.

Role of Urea
• Urea contributes to the establishment of the
osmotic gradient
in the medullary pyramids and
to the ability to form a concentrated urine in the
collecting ducts.
• Urea transport is mediated by
urea transporters
,
presumably by
facilitated diffusion
.
• The amount of urea in the
medullary interstitium
and, consequently, in the urine varies with the
amount of urea , and this in turn varies with the
dietary
intake of protein
.
• Therefore,
a high-protein diet
increases the
ability of the kidneys to
concentrate the
urine.

Water Diuresis
• The
water diuresis
produced by drinking large
amounts of hypotonic fluid begins about
15
minutes
after ingestion of a water load and
reaches its maximum in about
40 minutes
.
• The
act of drinking
produces a small decrease
in
vasopressin
secretion before the water is
absorbed, but most of the inhibition is
produced
by the decrease in plasma
osmolality
after the water is absorbed.
Water Intoxication
• During excretion of an average osmotic load, the maximal
urine flow that can be produced during a
water diuresis is
about 16 mL/min
.
• If water is ingested at a higher rate than this for any length
of time, swelling of the cells because of the uptake of water
from the hypotonic ECF becomes severe and, rarely, the
symptoms of water intoxication
may develop.
• Swelling of the cells in the brain causes
convulsions
and
coma
and leads eventually to
death
.
• Water intoxication can also occur when water intake is not
reduced after administration of
exogenous vasopressin
or
secretion of
endogenous vasopressin
in response to
nonosmotic stimuli such as surgical trauma.

Osmotic Diuresis
• The presence of large quantities of
unreabsorbed
solutes
in the renal tubules causes an increase in
urine volume called
osmotic diuresis
.
• Solutes that are not reabsorbed in the proximal
tubules exert an
appreciable osmotic
effect as the
volume of tubular fluid decreases and their
concentration rises.
• Therefore, they "
hold water in the tubules
.“
• In addition, there is a limit to the concentration
gradient against which Na
+
can be pumped out of
the proximal tubules.

• Normally, the movement of water out of the
proximal tubule prevents any appreciable
gradient from developing, but
Na
+
concentration
in the fluid falls when water
reabsorption is decreased because of the
presence in the tubular fluid of increased
amounts of unreabsorbable solutes.
Osmotic Diuresis

Osmotic Diuresis
• The
limiting concentration gradient
is
reached, and further proximal reabsorption of
Na
+
is prevented; more Na
+
remains in the
tubule, and water stays with it.
• The result is that the loop of Henle is
presented with a greatly increased volume of
isotonic fluid.
Osmotic Diuresis
• This fluid has a
decreased Na
+
concentration
, but
the
total amount of Na
+
reaching the loop per
unit time is increased.
• In the loop, reabsorption of water and Na
+
is
decreased because the
medullary hypertonicity
is
decreased
.
• The decrease is due primarily to
decreased
reabsorption of Na
+
, K
+
, and Cl
-
in the ascending
limb of the loop because the limiting
concentration gradient for Na
+
reabsorption is
reached.

•
More fluid passes
through the distal tubule,
and because of the decrease in the osmotic
gradient along the medullary pyramids,
less
water is reabsorbed
in the collecting ducts.
• The result is a marked increase in urine
volume and excretion of Na
+
and other
electrolytes.
Osmotic Diuresis
Osmotic Diuresis
• Osmotic diuresis is produced by the administration of
compounds such as
mannitol
and related
polysaccharides that are
filtered
but
not reabsorbed
.
• It is also produced by
naturally
occurring substances
when they are present in amounts exceeding the
capacity of the tubules
to reabsorb them.
• In diabetes mellitus, for example, the
glucose
that
remains in the tubules when the filtered load exceeds
the
Tm
G
causes
polyuria
.
• Osmotic diuresis can also be produced by the infusion
of large amounts of
sodium chloride or urea.
Osmotic Diuresis
• It is important to recognize the difference between
osmotic diuresis and water diuresis.
• In
water diuresis
, the amount of water reabsorbed in
the proximal portions of the nephron
is normal
, and
the maximal urine flow that can be produced is about
16 mL/min.
• In osmotic diuresis, increased urine flow is due to
decreased water reabsorption
in the proximal tubules
and loops and very large urine flows can be produced.
• As the load of excreted solute is increased, the
concentration of the urine approaches that of plasma
in spite of maximal vasopressin secretion, because an
increasingly large fraction of the excreted urine
is
isotonic proximal tubular fluid
.
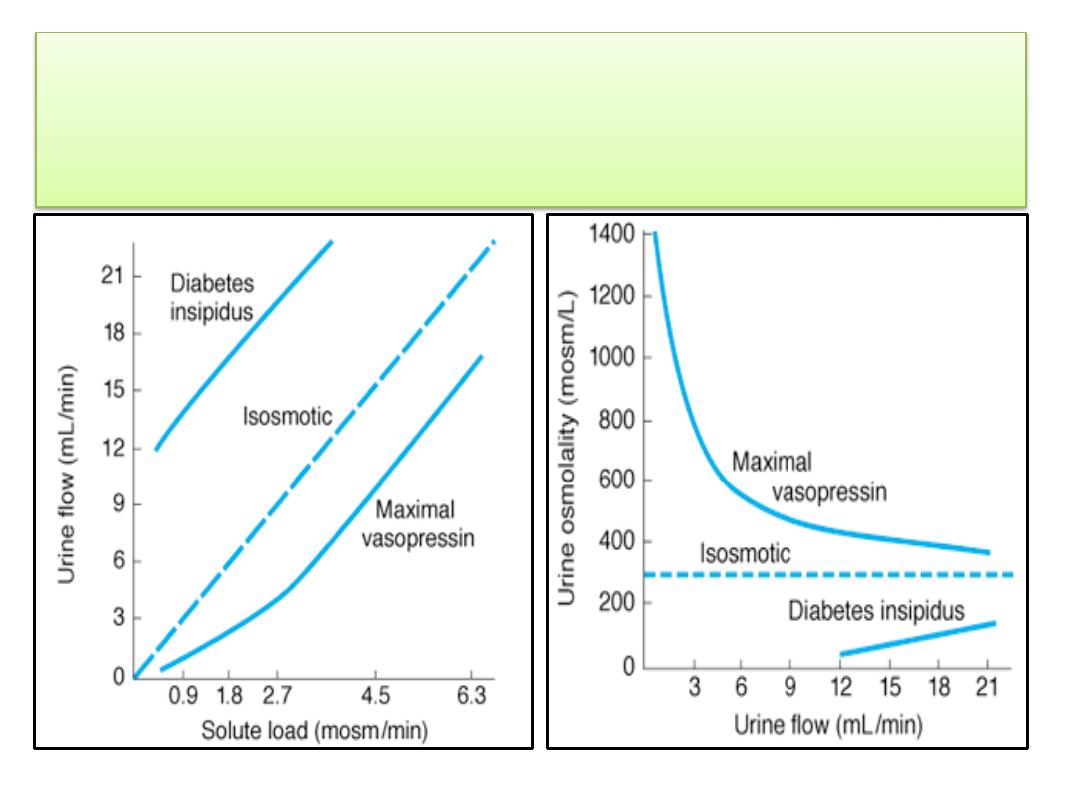
Approximate relationship between urine concentration and urine
flow in osmotic diuresis in humans. The dashed line in the lower
diagram indicates the concentration at which the urine is
isosmotic with plasma.
Relation of Urine Concentration to GFR
• The
magnitude
of the
osmotic gradient
along the
medullary pyramids is increased when the
rate of
flow
of fluid through the loops of Henle is
decreased
.
• A reduction in GFR such as that caused by
dehydration
produces a decrease in the volume
of fluid presented to the countercurrent
mechanism, so that the
rate of flow
in the loops
declines and the urine becomes
more
concentrated
.
• When the GFR is low, the urine can become
quite concentrated in the absence of
vasopressin.

Thank you
