
1
Hemodynamic Disorders, Thromboembolic
Disease, and Shock
OBJECTIVES
Edema
Hyperemia and Congestion
Hemorrhage
Hemostasis and Thrombosis
Embolism
Infarction
Shock

2
Definitions
Homeostasis
maintaining blood as a liquid
Thrombosis
Clotting at inappropriate sites
Hemostasis
Clotting at appropriate site (site of
injury)
Embolism
migration of clots
Infarction
obstruction of blood flow to tissues
and leads to cell death
Hemorrhage
inability to clot after vascular
injury
Shock
extensive hemorrhage can result in
hypotension and death

3
•Normal fluid homeostasis is
maintained by
vessel wall integrity
,
intravascular
pressure
and
osmolarity
within certain physiologic ranges.
•Changes in
intravascular volume
,
pressure
,or
protein content
, or
alterations in endothelial function
will affect the movement of water
across the vascular wall


5
Edema
=
Increased fluid in the interstitial tissue spaces
Anasarca:
Severe and generalized edema + profound
subcutaneous swelling
Pathophysiology
1.
Increased Hydrostatic Pressure
Most common cause -
Congestive heart failure
,
others - DVT
2. Decreased oncotic or osmotic Pressure
(hypoproteinemia)
Nephrotic syndrome, Cirrhosis, malnutrition, GIT.
3. Sodium retention
Renal failure, Renin- Angiotensin - Aldosterone
4. Inflammation: Acute or chronic,
5. Lymphatic obstruction
Type of edema
exudate
in inflammatory and
transudate
in non inflammatory conditions


• Increased Hydrostatic Pressure
• Localized increase in intravascular pressure
can result from impaired venous return
DVT, edema in distal portion of affected leg.
• Generalized increases in venous pressure with
resultant systemic edema occur most
commonly in congestive heart failure,
affecting right ventricular cardiac function
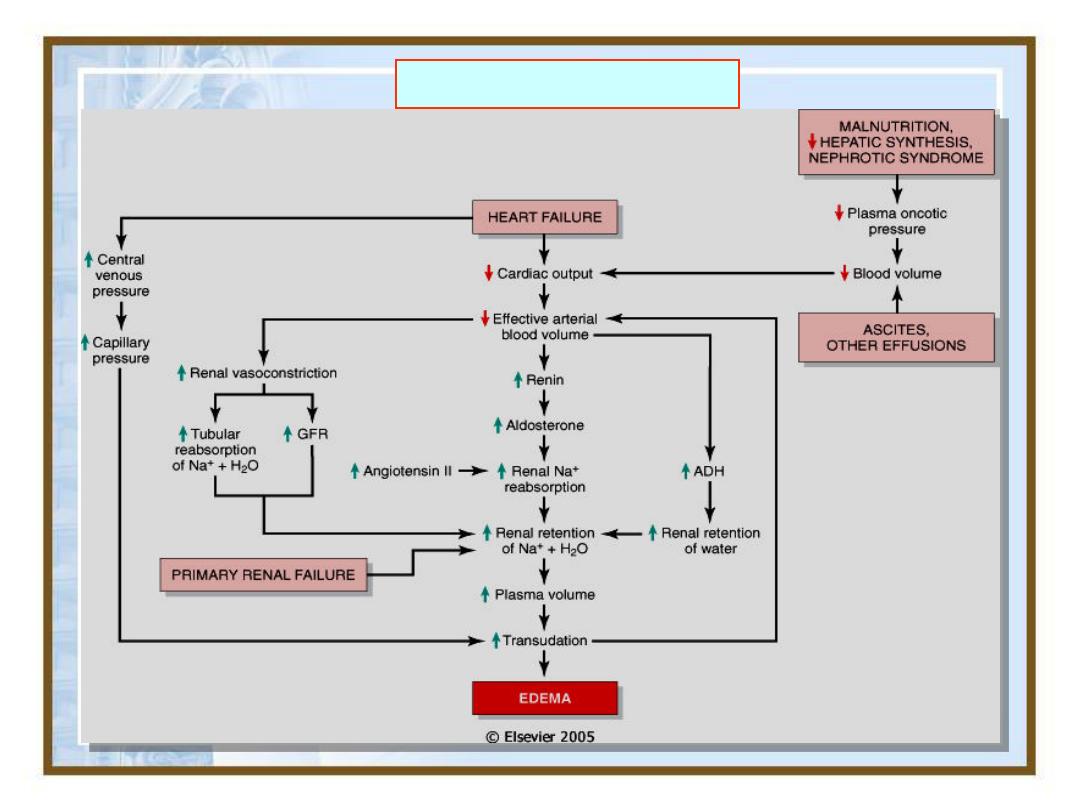
7

• In congestive heart failure, reduced cardiac
output translates into reduced renal perfusion
• Renal hypoperfusion triggers renin-
angiotensin- aldosterone axis, inducing
sodium and water retention by the kidneys.
• Mechanism normally increase intravascular
volume and thereby improve cardiac output
to restore normal renal perfusion.
• If the failing heart cannot increase cardiac
output, the extra fluid load causes increased
venous pressure and then edema
8
9
Edema - Pathogenesis

• Reduced plasma osmotic pressure: albumin
is the serum protein most responsible for
maintaining intravascular colloid osmotic
pressure.
• If there is albumin loss or inadequately
synthesized in diffuse liver disease, in each
case, reduced plasma osmotic pressure leads
to movement of fluid into interstitial tissues,
reduced intravascular volume leads to renal
hypoperfusion followed by secondary
aldosteronism. But the retained salt and
water cannot correct plasma volume deficit
generalized edema will occur.
10

11
Edema
Morphology
= Mostly involve
Subcutaneous tissues
,
Lung
,
Brain
Subcutaneous
– can be pitting (Cardiac or renal disorders) or
non
– pitting ( Thyroid disorders)
Pitting edema can be in dependent parts (at ankles in
ambulatory and Back or sacrum in bedridden patients-
cardiac disorders) nondependent area ( periorbital in renal
disorders)
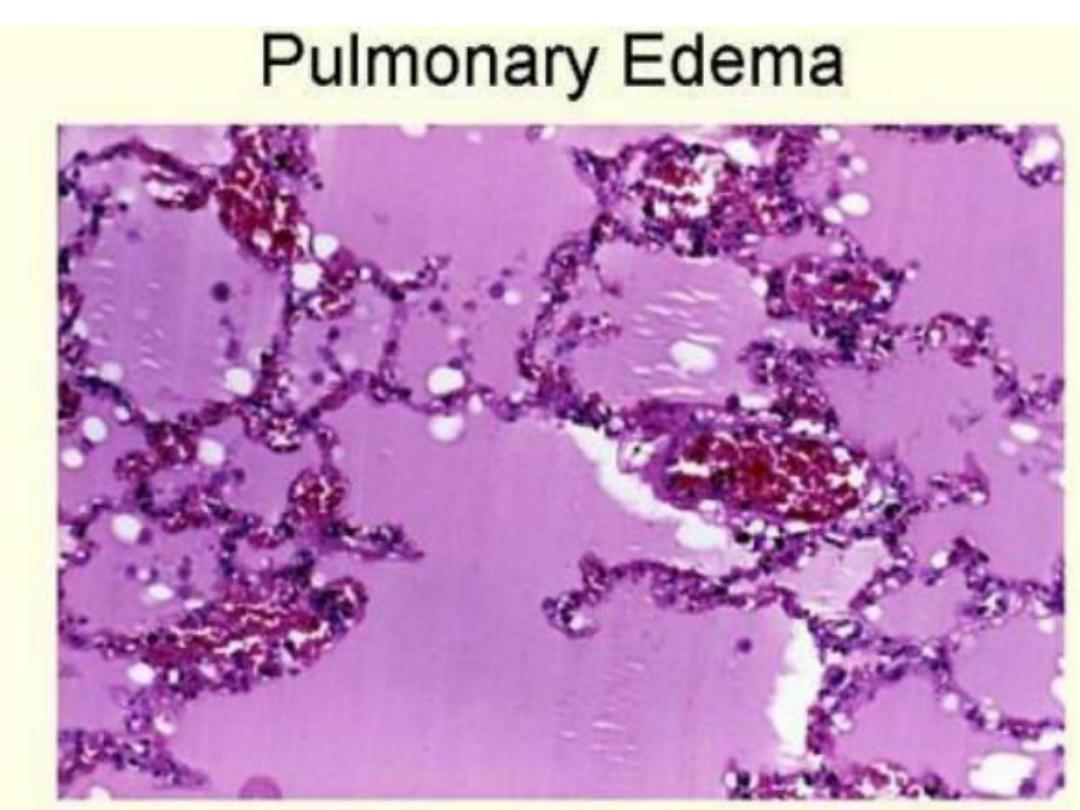
Lung or Pulmonary edema
– Most common in Left Heart
failure, lungs are wet and heavy, pink frothy fluid in alveoli
Cerebral edema
–
localized ( Abscess, Neoplasms) /
Generalized ( Encephalitis), narrowed sulci and distended gyri,
fatal if edema develops rapidly (due to cerebellar or Tonsillar
Herniation)
Clinical significance
In Almost disorders causing edema, excess sodium re-absorption
( via Renin Angiotensin-Aldosterone pathway) is key factor
Treatment
salt intake, Diuretics (↑sodium Excretion), Aldosterone
antagonists


13
Types of edema
•
Anasarca
:Generalized edema
•
Dependent edema:
Prominent feature of
congestive heart failure, particularly of the
right ventricle.
•
Renal edema:
Edema as aresult of renal
dysfunction or nephrotic syndrome is
generally more severe than cardiac
edema and affects all parts of the body
equally

14
•
Peri-orbital edema:
is acharacteristic
finding in severe renal disease.
•
Pitting
edema
:finger pressure over
substantially edematous
subcutaneous tissue displaces the
interstitial fluid and leaves a finger-
shaped depression
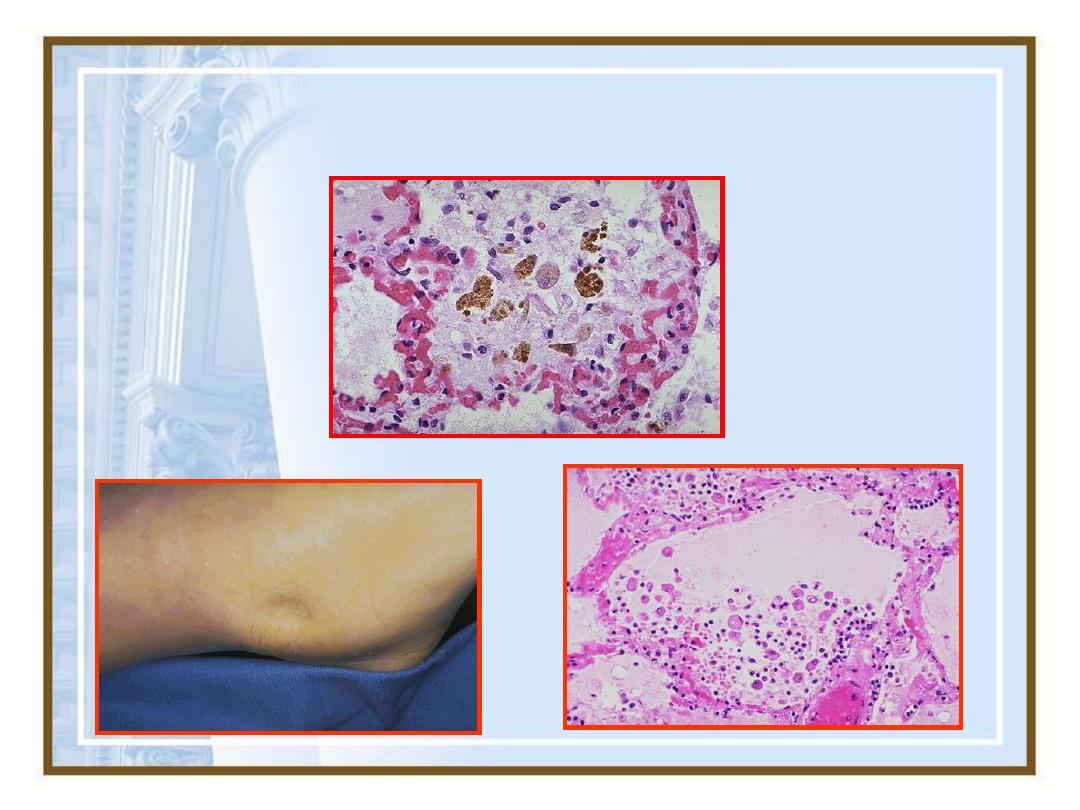
•
Pulmonary edema
: most typically
seen in the setting of left ventricular
failure
15
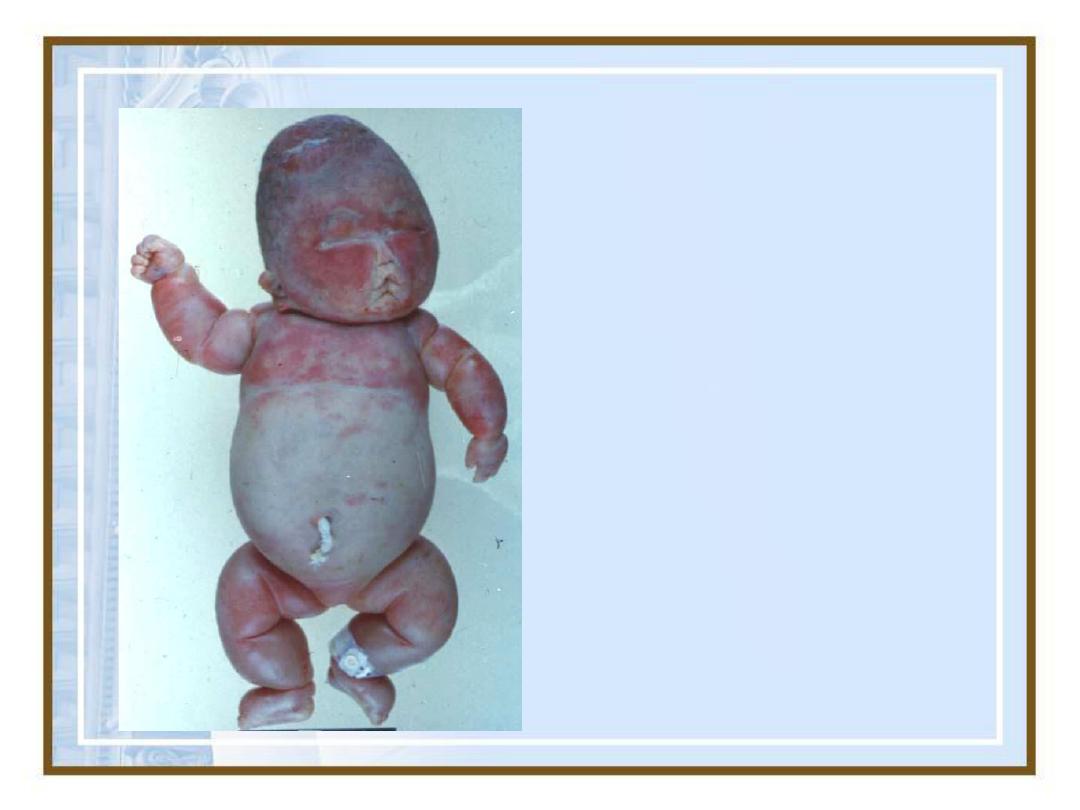
Fetal Anasarca
17

18
2-
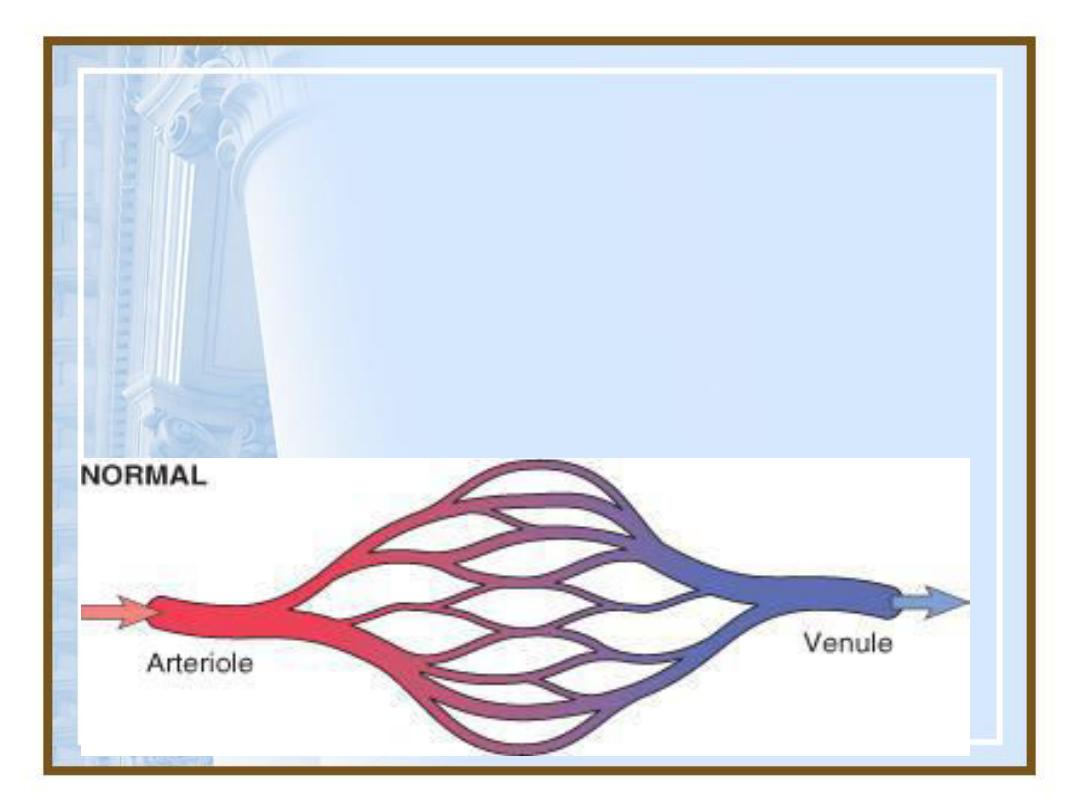
Hyperemia
and
Congestion
•Both indicate alocal increased
volume of blood in aparticular
tissue
19
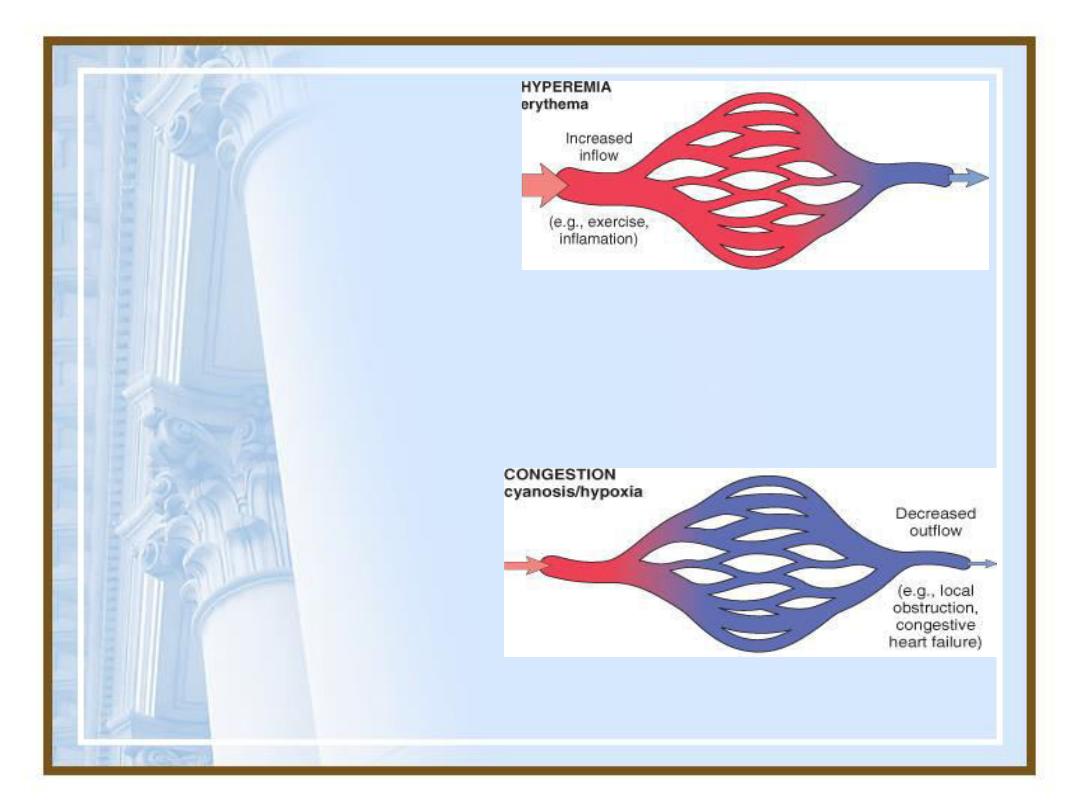
Hyperemia
versus
congestion.
In both cases there is an increased
volume and pressure of blood in a
given tissue with associated capillary
dilatation and apotential for fluid
extravsation
20
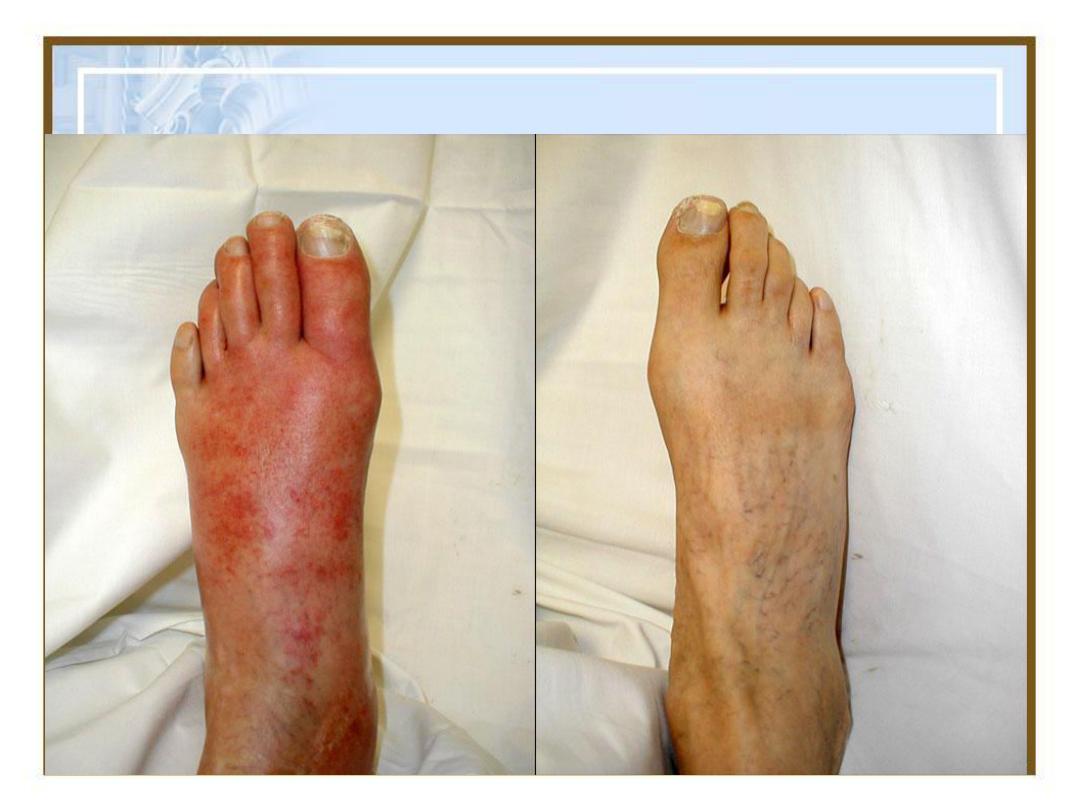
Hyperemia:
active
process, increased in
flow leads to
engorgement with
oxygenated blood,
resulting in
erythema.
Co
ngestion:
a
passive process
diminished outflow
leads to a capillary
bed swollen with
deoxygenated
venous blood and
resulting in
cyanosis.
21
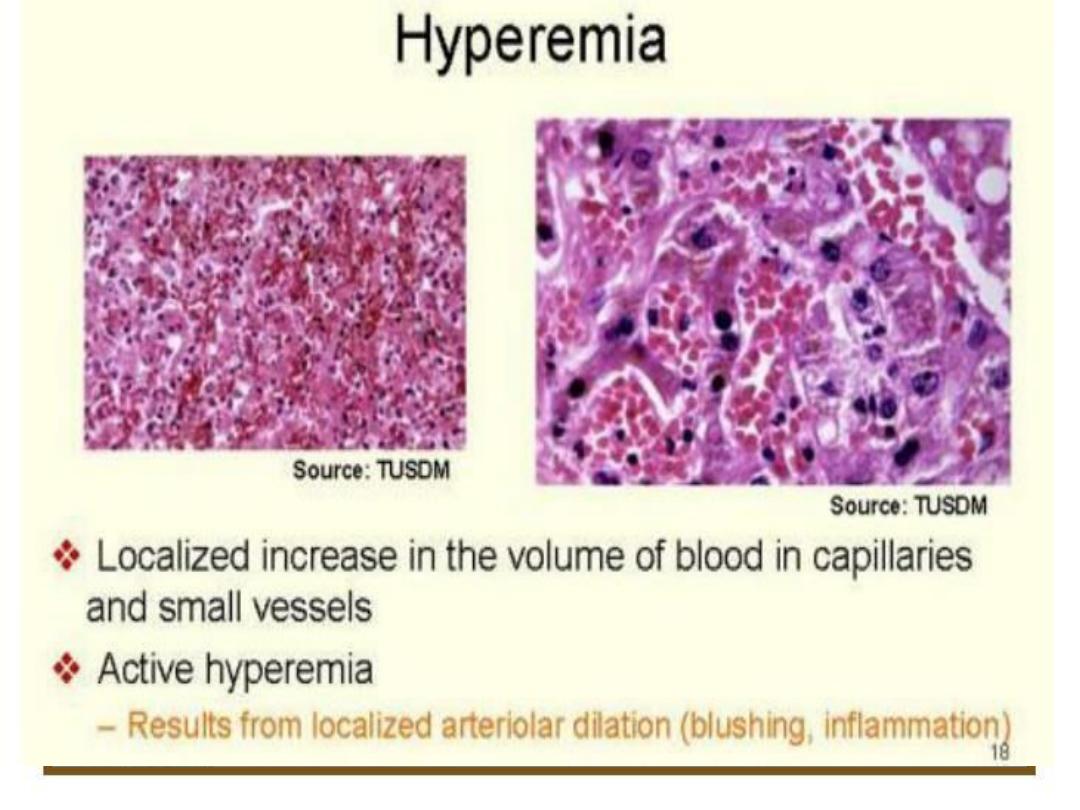
Hyperemia

• Congestion and edema commonly occur
together .
• Chronic passive congestion: or long-standing
congestion, stasis of poorly oxygenated blood
cause
chronic hypoxia, degeneration or death
of parenchymal cells and subsequent tissue
fibrosis.
• Capillary rupture cause small foci of
hemorrhage, phagocytosis and catabolism of
erythrocyte debris results in accumulation of
hemosiderin-laden macrophages.
23

• Acute pulmonary congestion
• Alveolar capillary engorged with blood.
• Alveolar septal edema, and focal intra-
alveolar hemorrhage
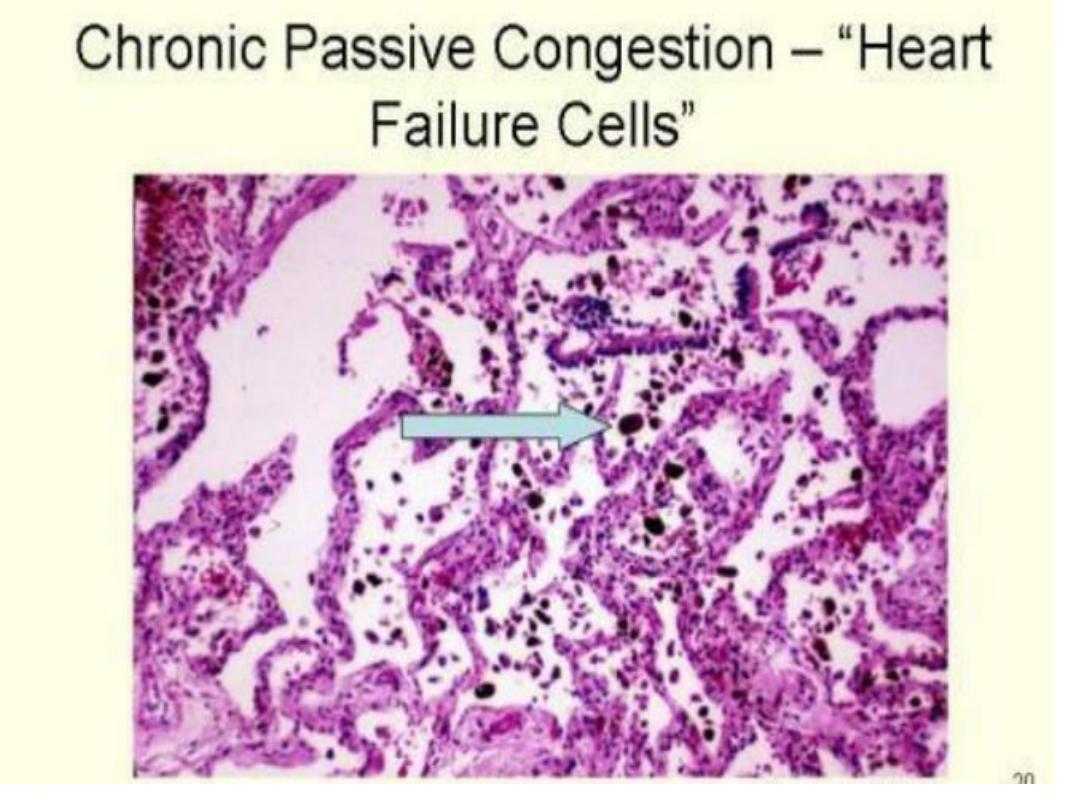
• Chronic pulmonary congestion
• Septa thickened and fibrotic, alveolar spaces
contain numerous hemosiderin-laden
macrophages(heart failure cells)
24

• Acute hepatic congestion
• Central vein and sinusoids distended with blood,
and central hepatocyte degenerated but periportal
hepatocytes better oxygenate may develop fatty
change
• Chronic passive congestion
• Gross: central regions of hepatic lobule are red-
brown and depressed because of a loss of cells and
are accentuated against the surrounding zones of
uncongested tan, sometimes fattyliver (nutmeg liver)
• Mic: centrilobular necrosis, hemorrhage and
hemosiderin-laden macrophages.
• Hepatic fibrosis: (cardiac cirrhosis) in long standing
cases sever hepatic congestion in case of heart failure
25

28
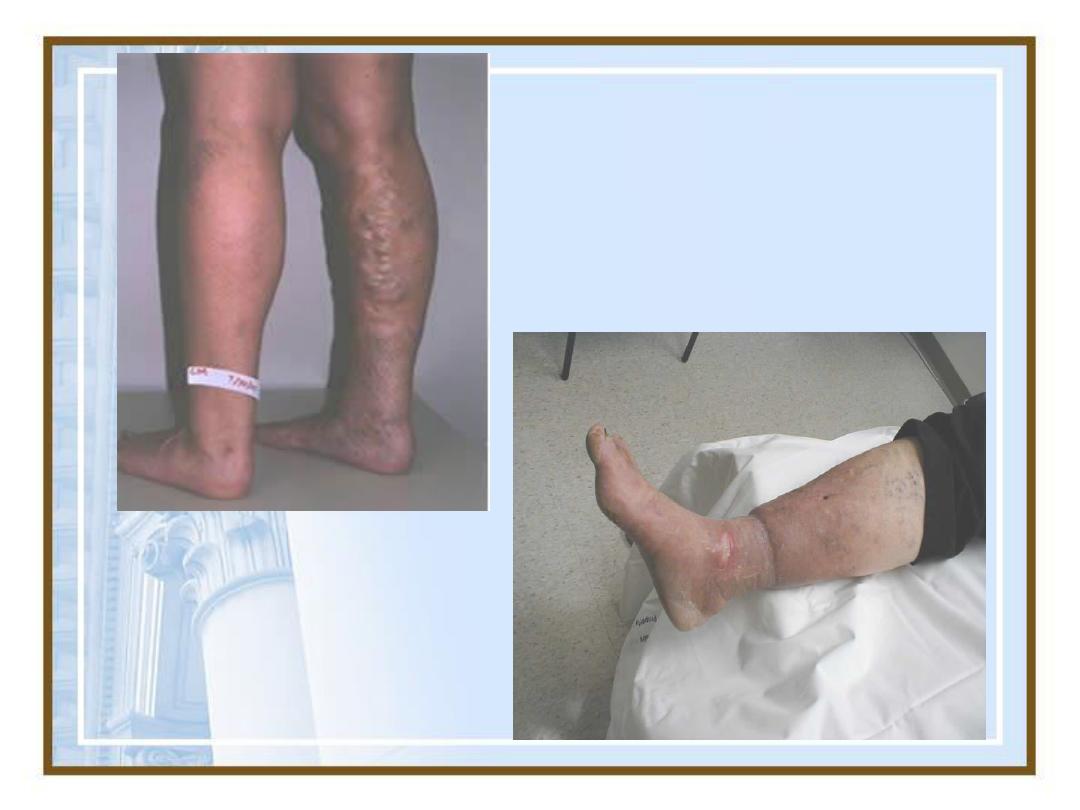
Congestion
Varicose Veins

29
3-Hemorrhage
Extravasation of blood due to vessel
rupture .
Chronic congestion.
Rupture of a large A. due to vascular
injury, trauma, atherosclerosis,
inflammatory or neoplastic erosion

30
Types
•
Hematoma: accumulation
of blood
within tissue.
•
Petechiae:
minute 1 to 2 mm
hemorrhages into skin, mucous
membranes, or serosal surfaces.
•
Purpura:
slightly larger (≥3mm)
hemorrhages

31
Ecchymoses:
larger (>1to2cm)
subcutaneous hematomas (i.e.,bruises)
•
Hemothorax, hemopericardium,
hemoperitoneum, or hemarthrosis
(injoints):
Large accumulations of blood
in one of the body cavities


34
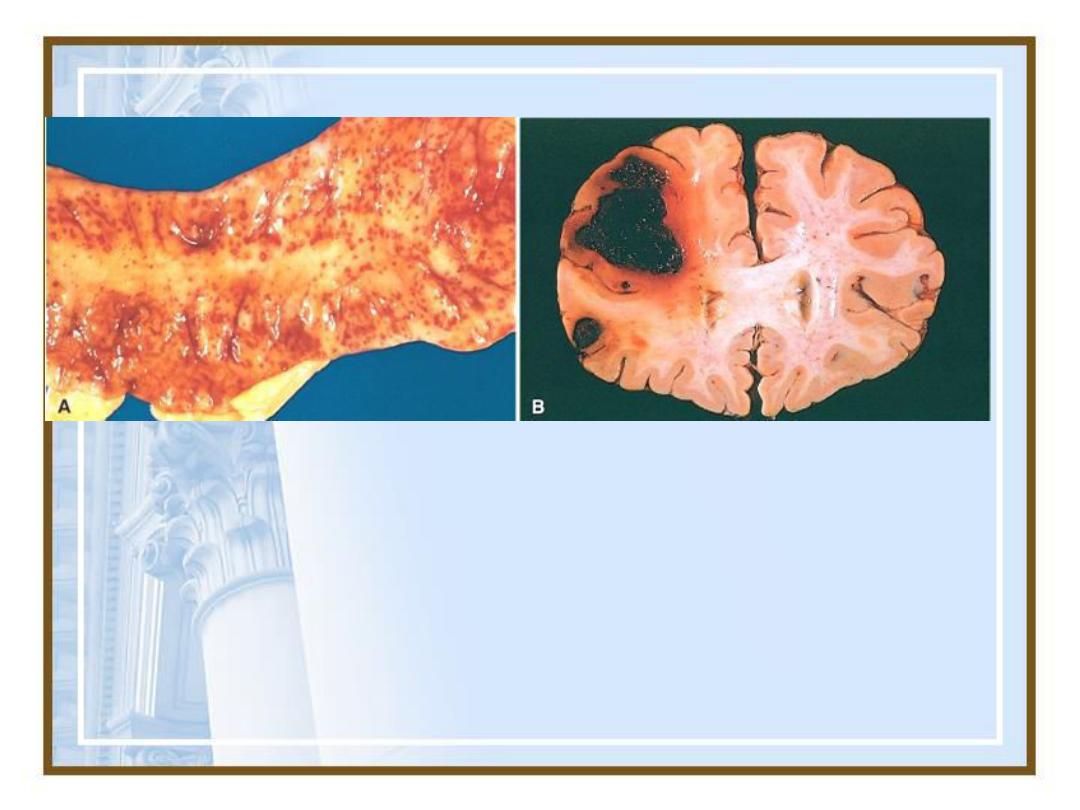
Petechial hemorrhages of the
colonic mucosa
Intracerebral bleeding
35
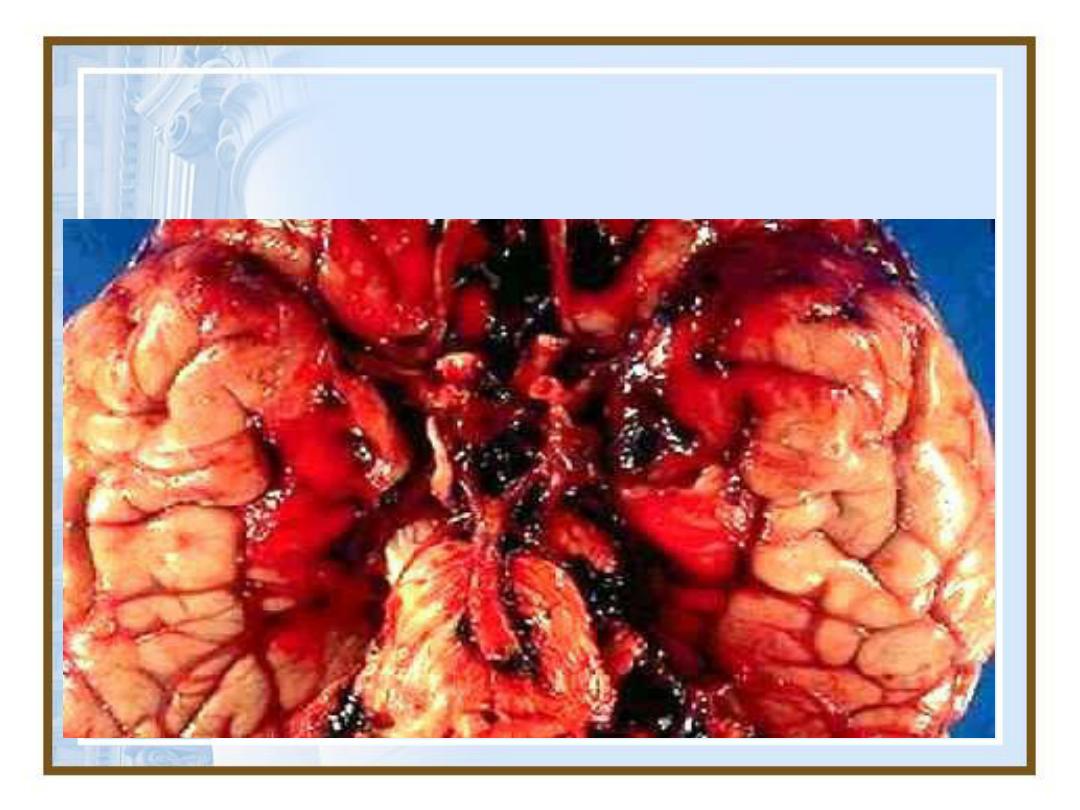
Subarachnoid Haemorrhage:
36
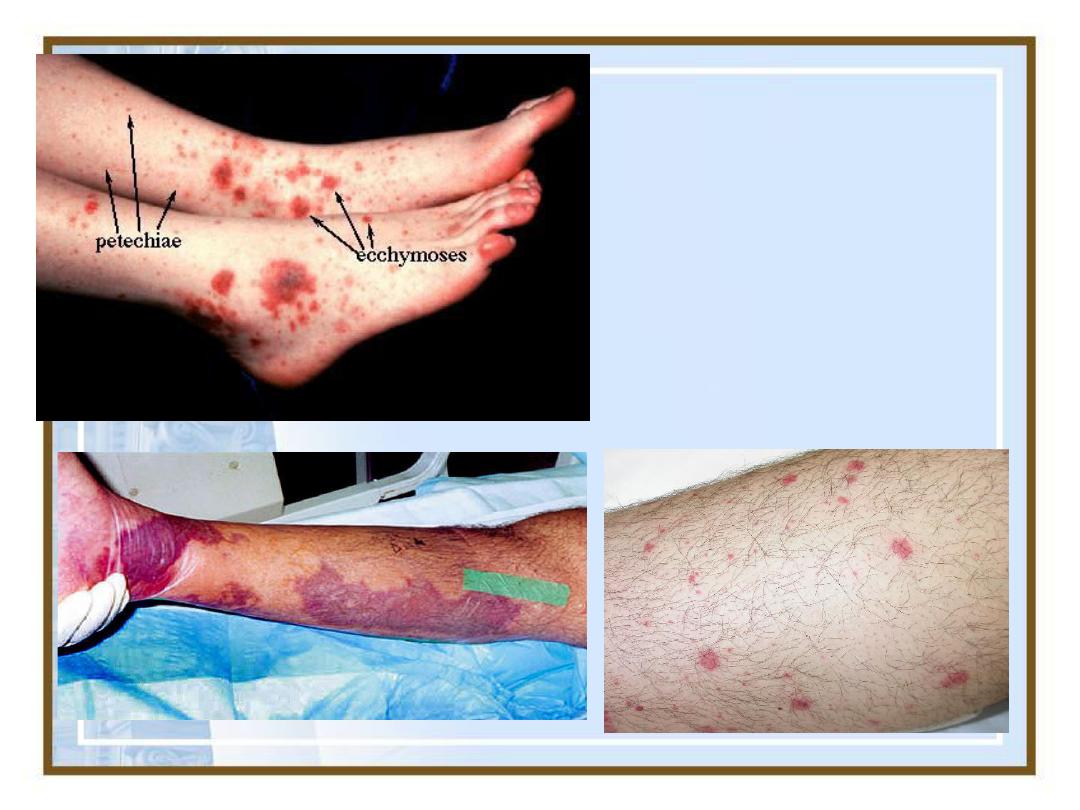
Petechiae &
Ecchymoses
37
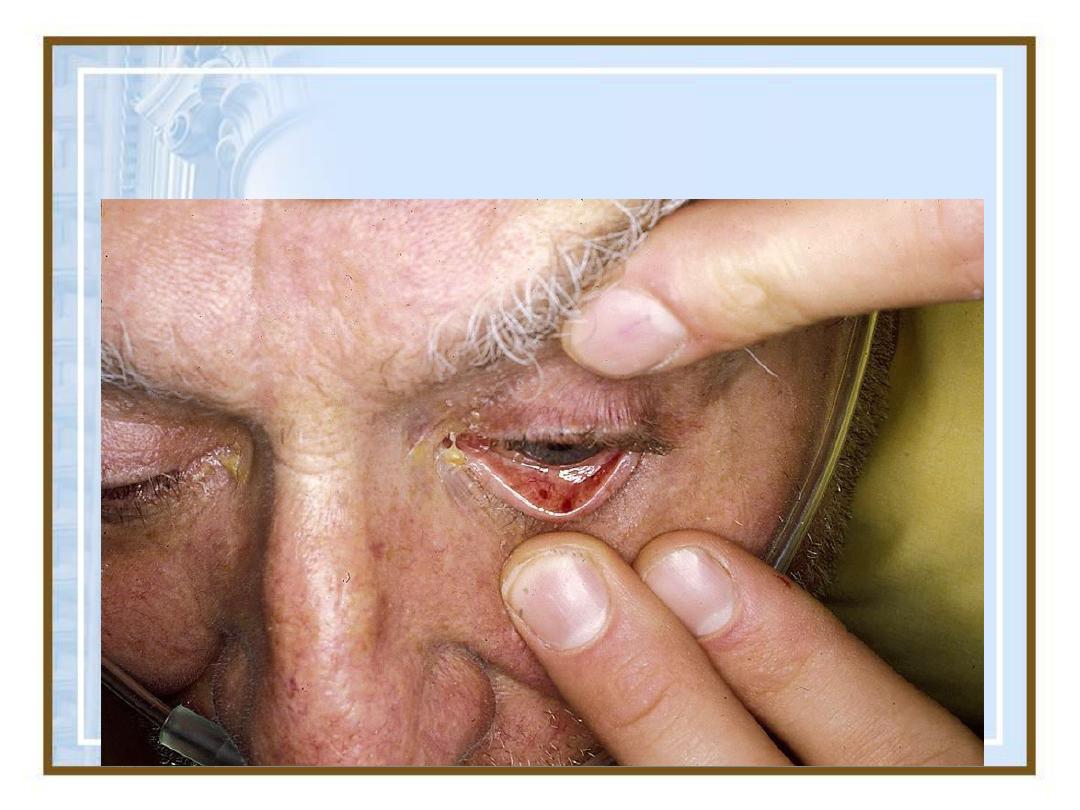
Conjunctival Petechiae
38
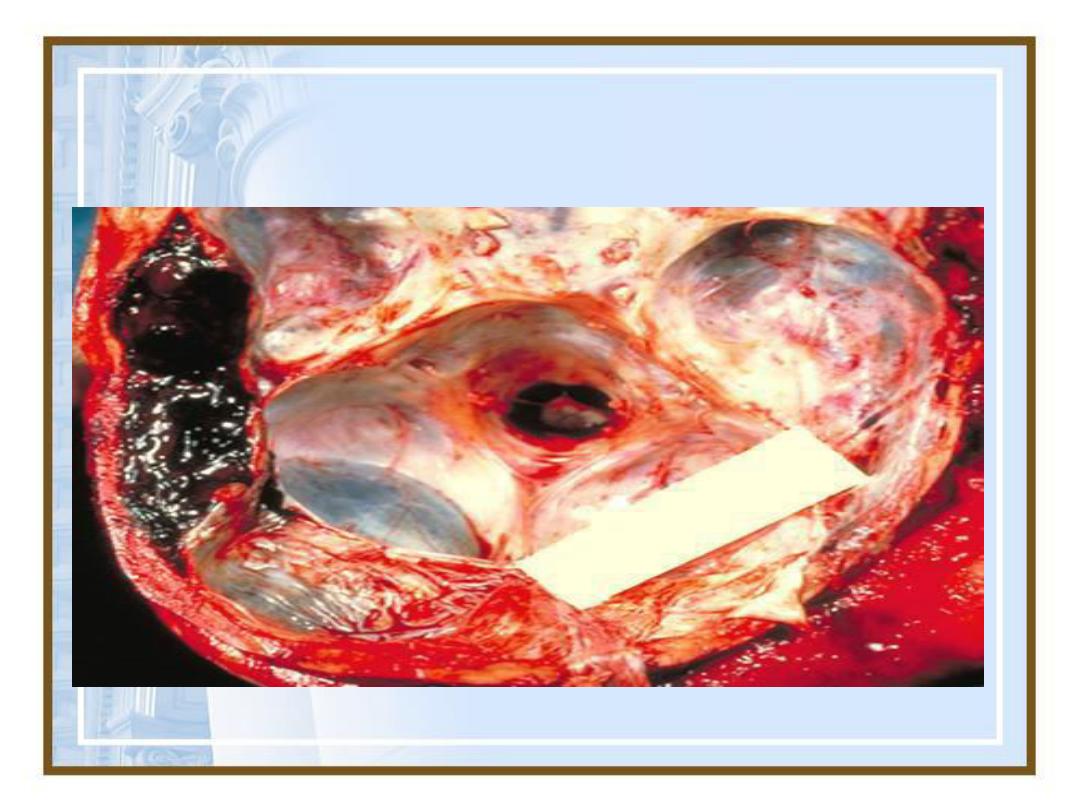
Hemorrhage: Epidural hematoma
39
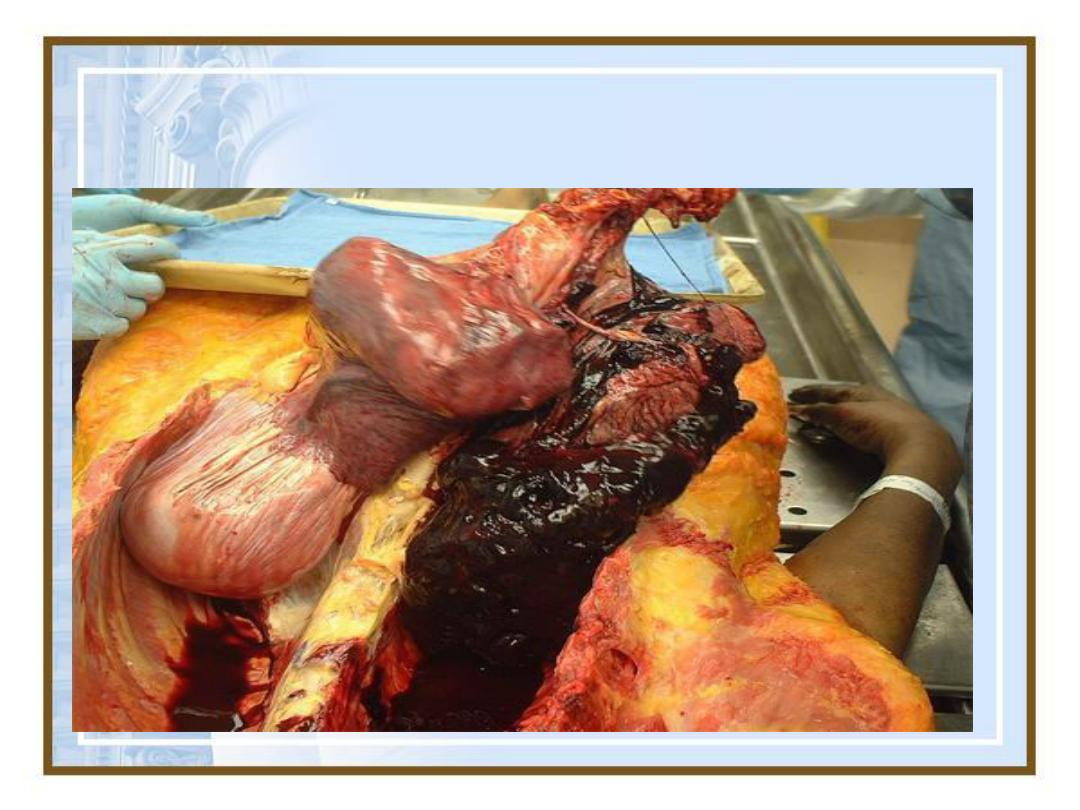
Hemothorax

40
4-Thrombosis

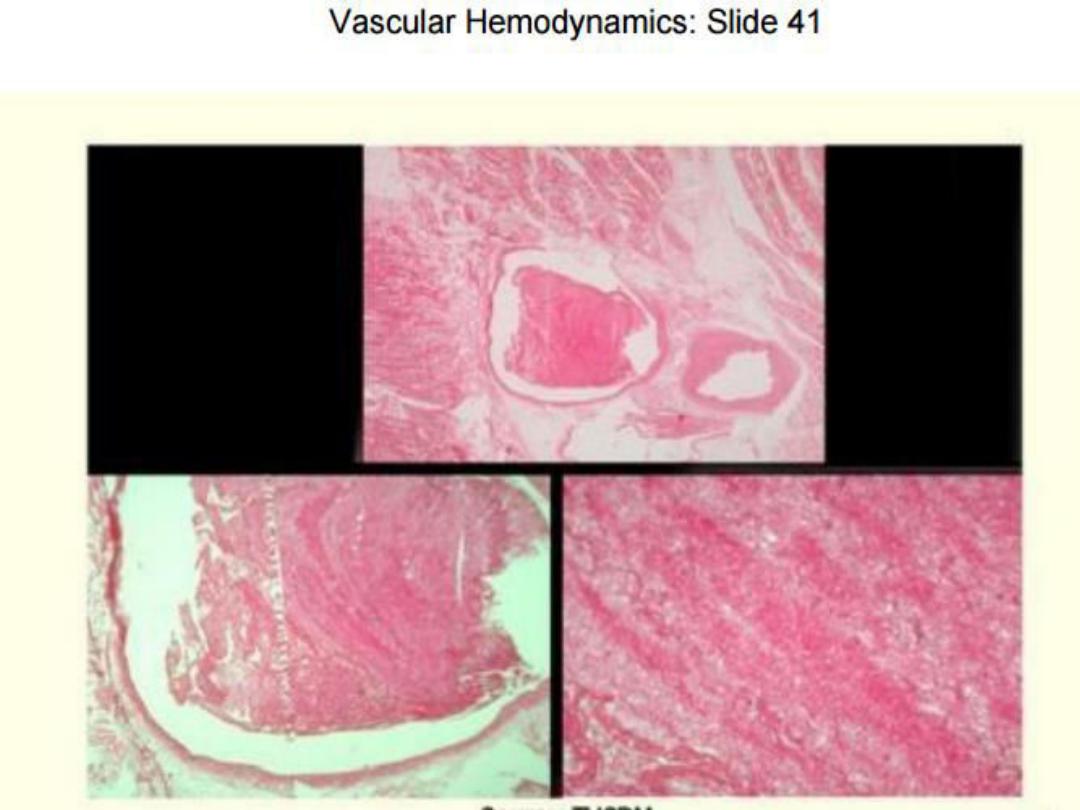
41
Hemostasis and Thrombosis
Normal hemostasis result of a set of
well regulated processes that
accomplish two important functions:
(1)
They maintain blood in a fluid, clot-
free state in normal vessels.
(2)
They are aimed to induce a rapid
and localized hemostatic plug at a site
of vascular injury

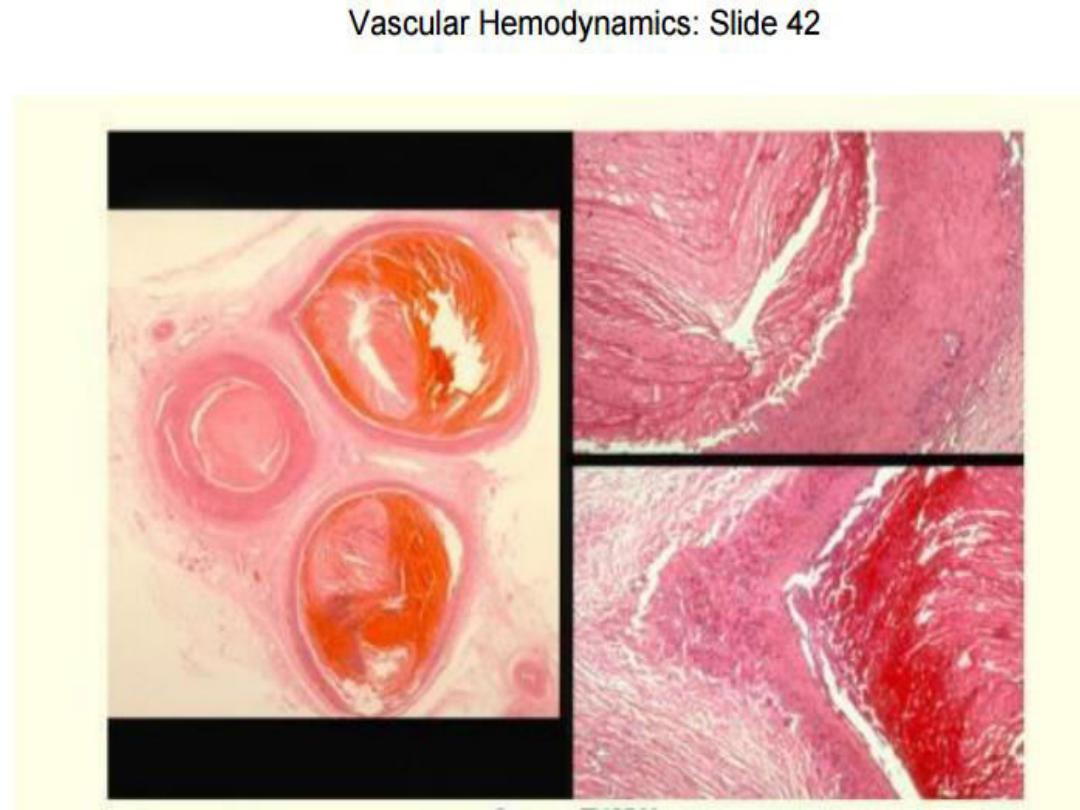
42
•
Thrombosis:
an inappropriate
activation of normal hemostatic
processes, such as the formation
of a blood clot
(thrombus)
in
uninjured vasculature
or
thrombotic occlusion of a vessel
after relatively
minor injury
.

43
Both
hemostasis
and
thrombosis
are
regulated by three general
components:-
–the vascular wall
–platelets
–the coagulation factors

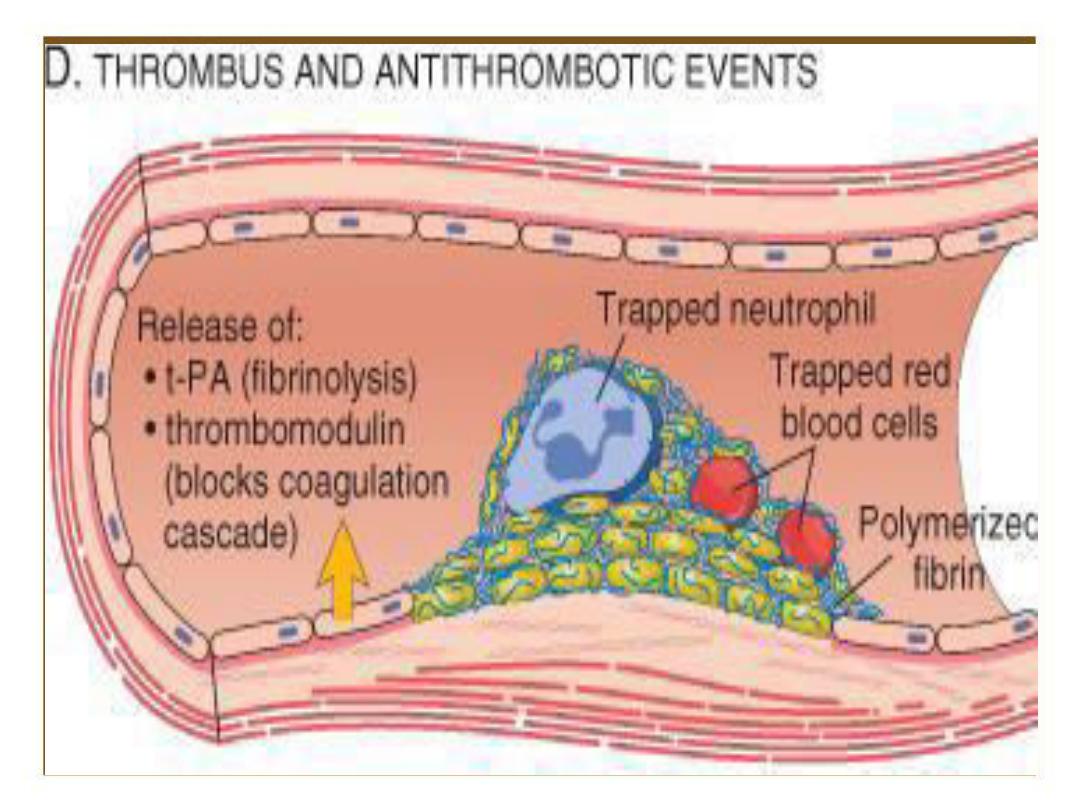
Absence of B.V damage:
• Platelets repelled from each other and from
endothelium of B.V which is a simple squamous epi.
That overlies C.T collagen and other proteins that
are capable of activating platelets , so it separates
blood from collagen and other platelet activator.
• Endothelial cells also secrete prostacyclin PGI2(type
of prostaglandin) and nitric oxide(NO) which act as
vasodilators and also inhibit platelet aggregation.
• Plasma mem. of endothelial cells contains enzyme
CD39 which breakdown ADP in blood to AMP and
P1 (ADP is released from activated platelets and
promotes platelet aggregation)
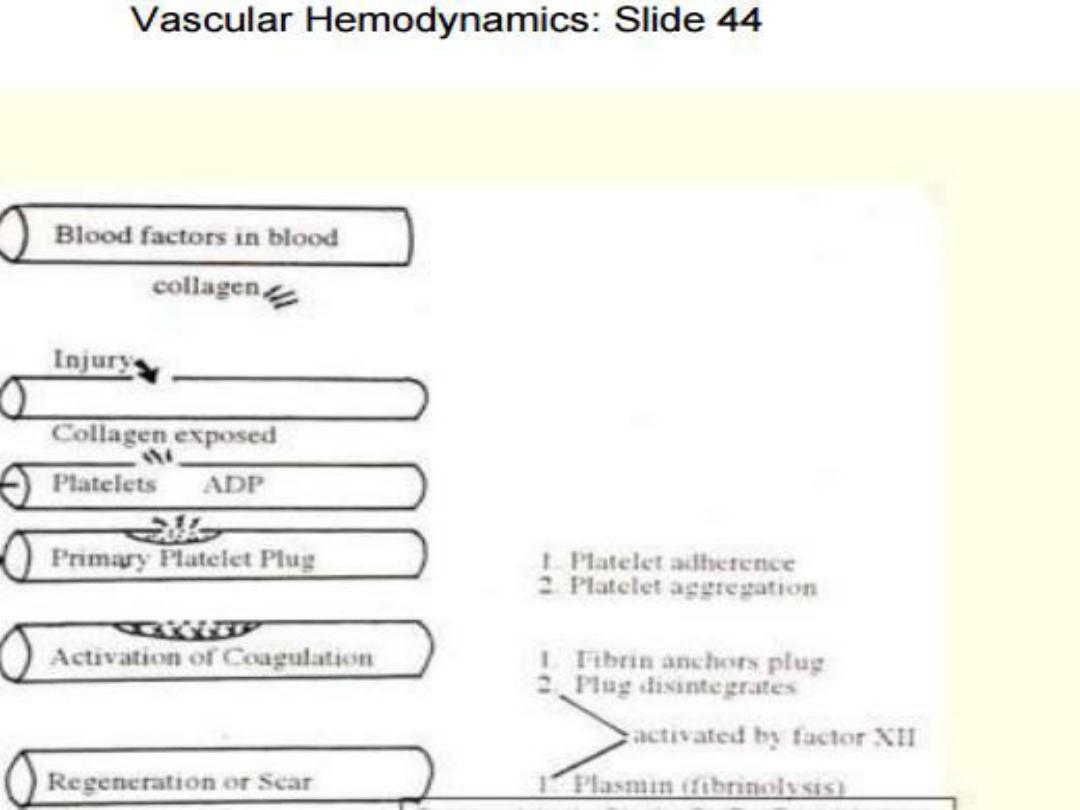
44
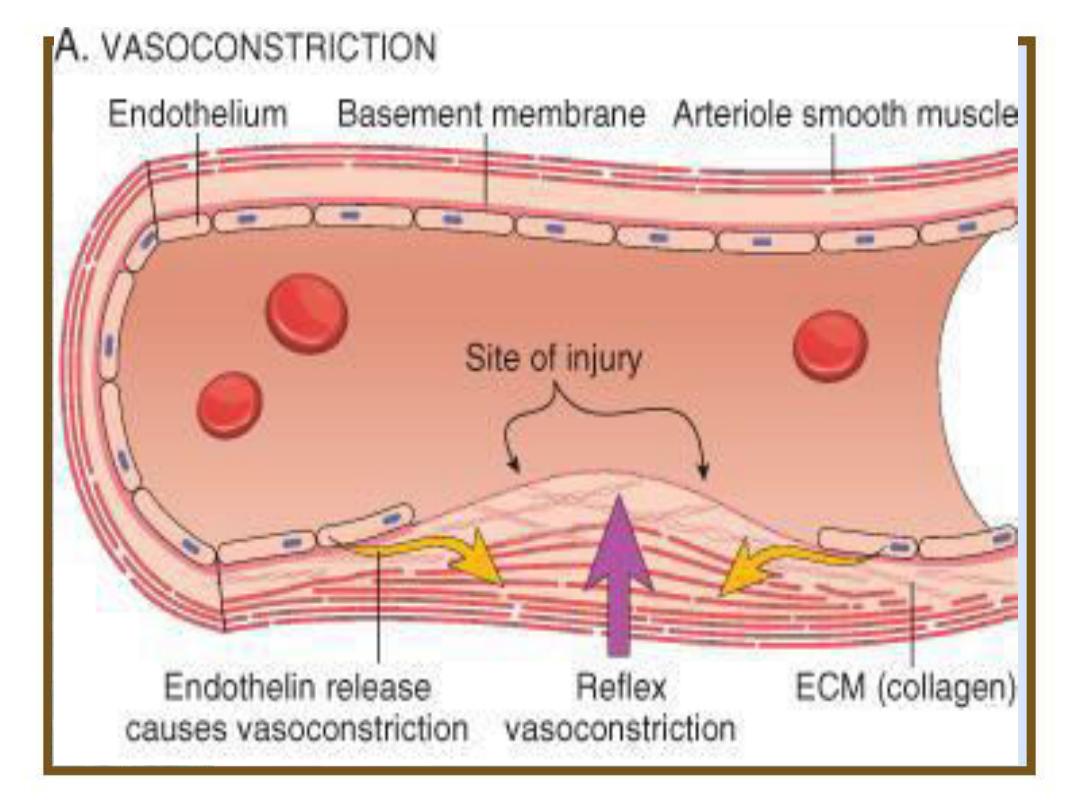
45

Injury of blood vessel
• Platelet plasma mem. now able to bind to exposed collagen
fibers but the force of blood flow might pull the platelets off the
collagen
• Another protein produced by endothelial cells VON
WILLEBRAND factor which binds to both collagen andplatelet
• Platelet contains secretary granules when they stick to collagen,
they degranulate and release their products which include
(ADP, serotonin, and prostaglandin called thromboxane A2).
These products recruits new platelet to the vicinity and make
them sticky and stuck on other platelets on the collagen, and
those on 2
nd
layer release their products and additional
platelets aggregate at the site of injury, this produce platelet
plug.
46
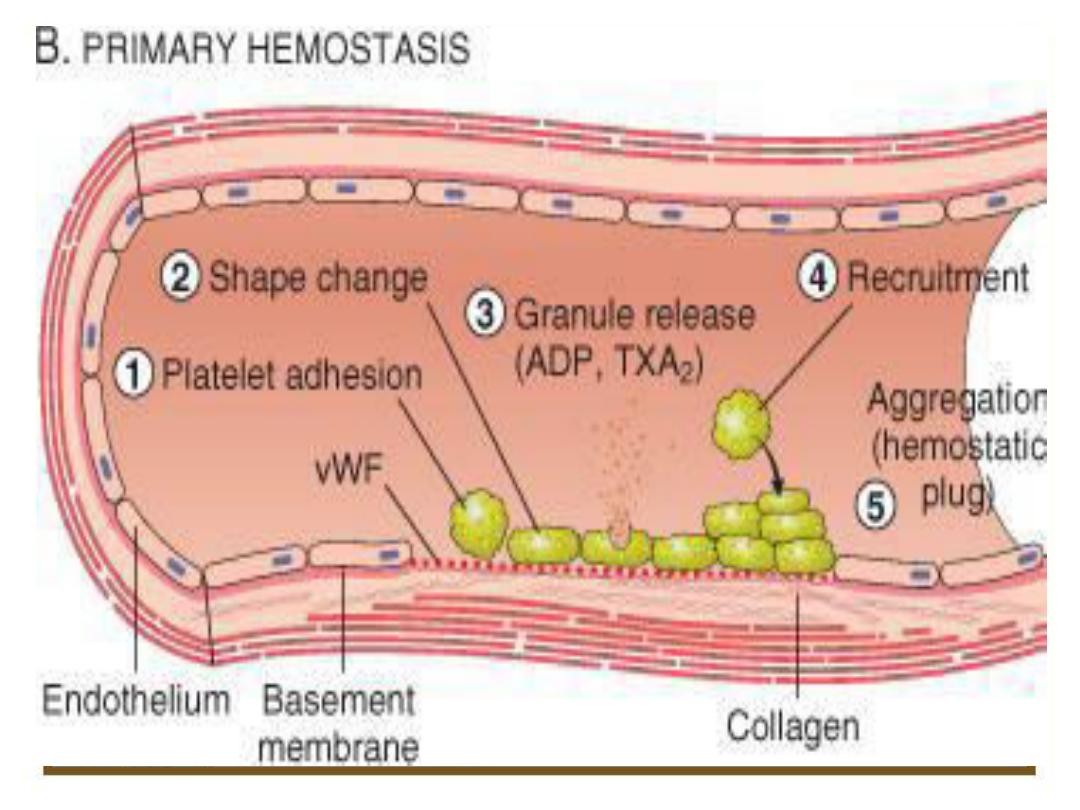
47

Platelet plug
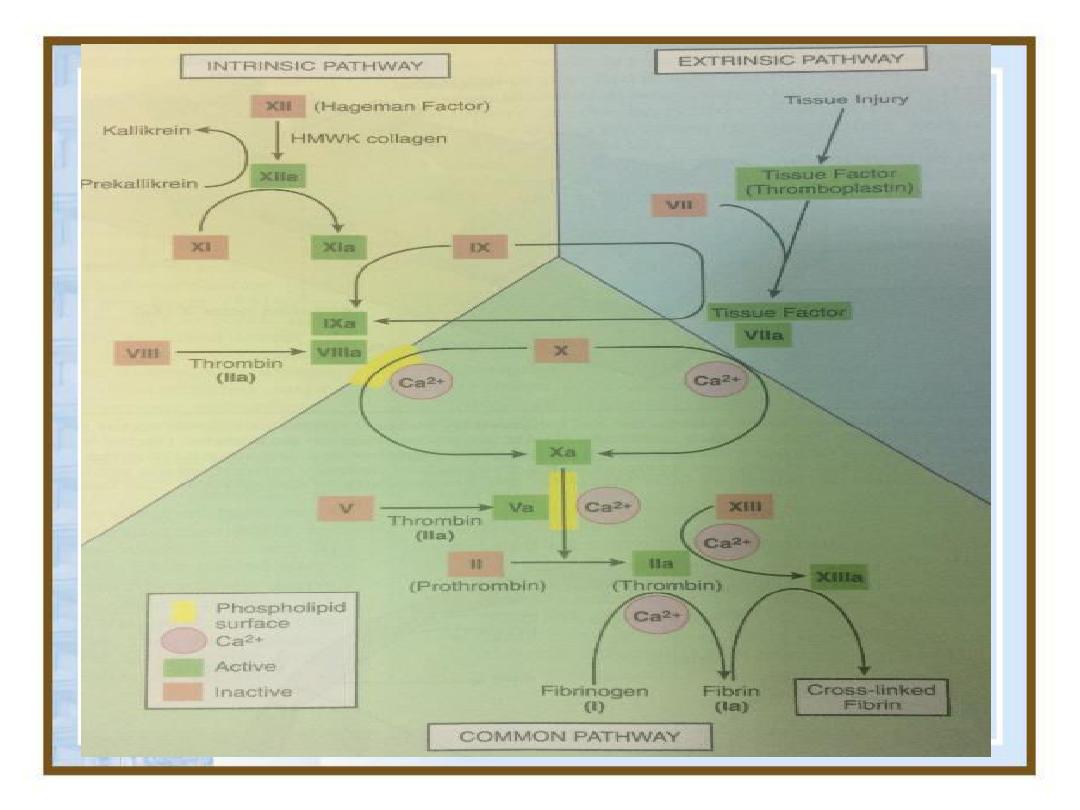
• Activated platelets help to activate plasma clotting factors.
• Exposure of plasma to a negatively charged surface such as
collagen at the site of a wound, This activates a plasma protein
called factor X11 Hagmen factor which is a protein digesting
enzyme (protease).
• Active factor X11 I in turn activate another clotting factor, it
requires Ca and phospholipids which is provided by platelets,
these resulted in conversion of an inactive glycoprotein
prothrombin into active enzyme thrombin.
• Thrombin converts a soluble plasma protein fibrinogen into
insoluble fibrous protein fibrin, binding sites on platelets
plasma mem. Binds to fibrinogen and fibrin, which helps to join
them together and strengthen the plug.
48
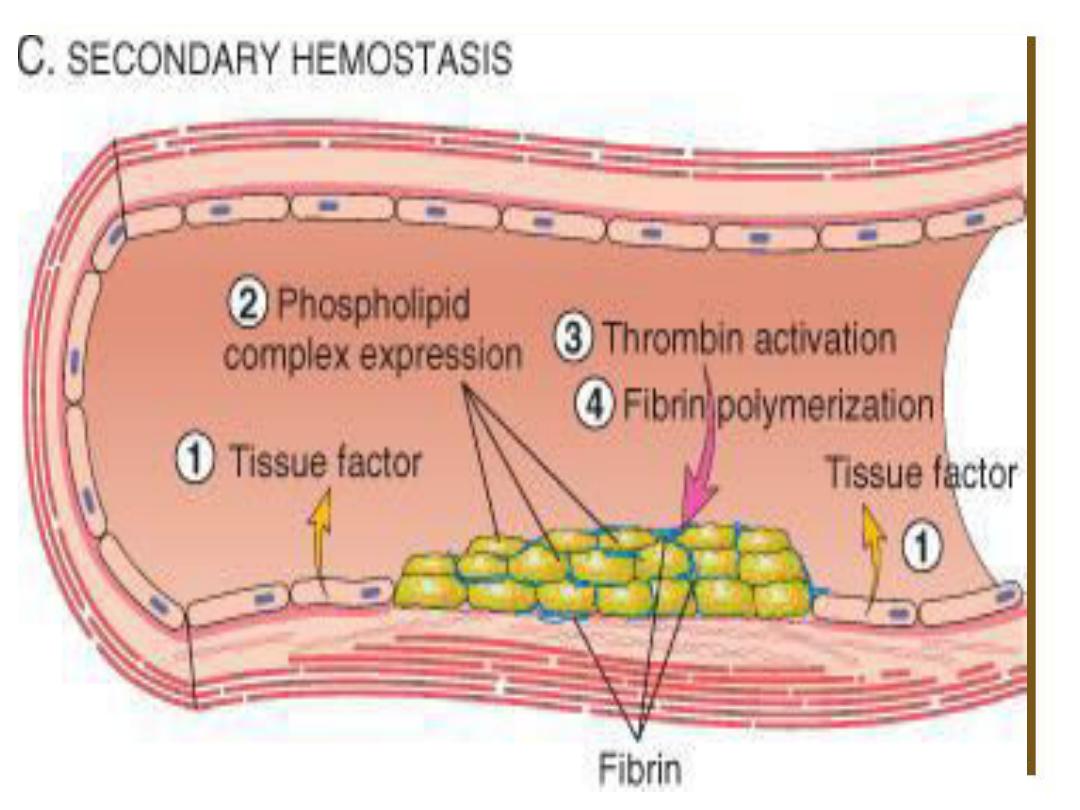
49



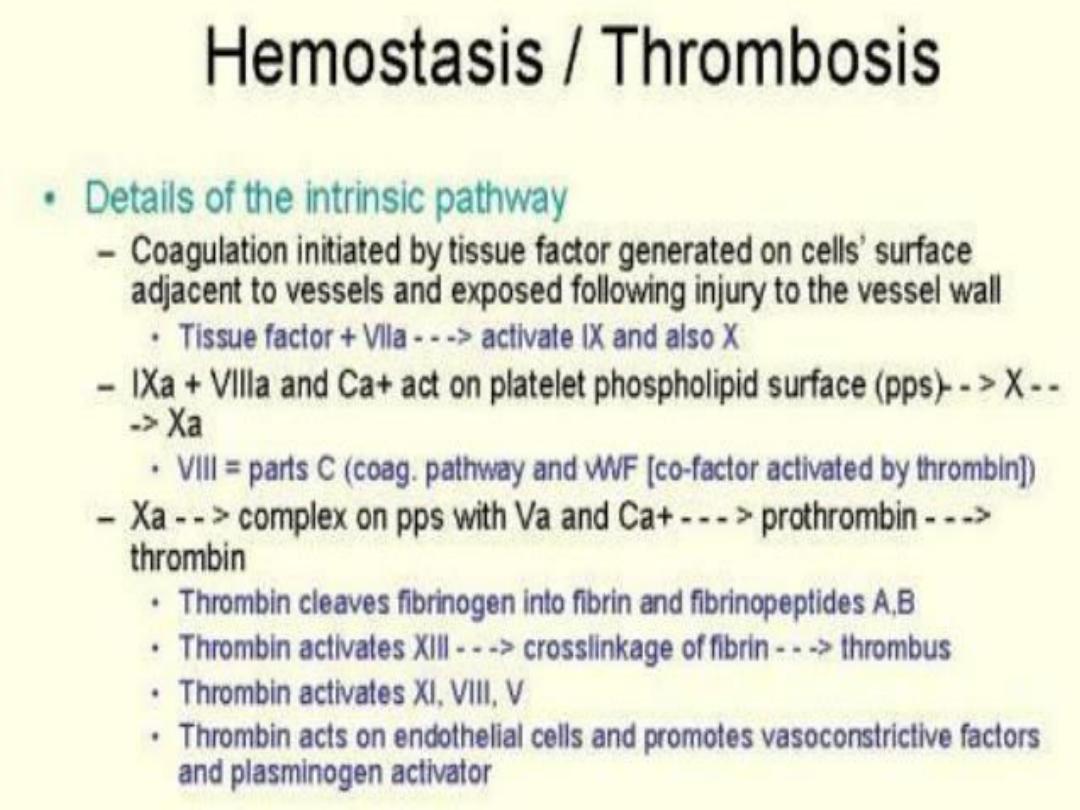
54

56
58



65
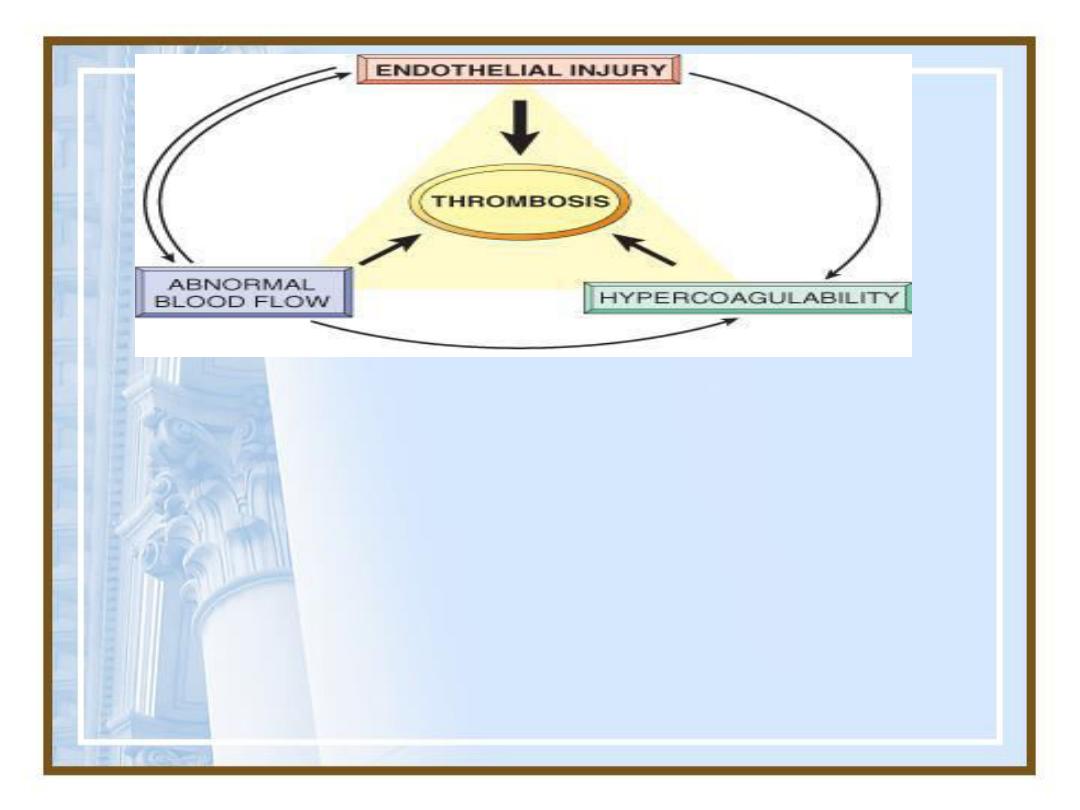
•Three primary causes for thrombus
formation, theso-called
Virchow
triad:
(1)Endothelial injury
(2)Stasis or slowing of blood flow
(3)Blood hyper-coagulability
66
•
Virchow triad
in thrombosis.
Endothelial integrity
is the
single most important factor. Note that
injury to
endothelial
cells can affect local blood flow and/or
coagulability;
abnormal blood flow
(stasis or
turbulence) can, in turn, cause endothelial injury. The
elements of the triad may act independently or may
combine to cause thrombus formation.

• High blood flow rates might hamper
clotting by preventing platelet adhesion or
diluting coagulation factors.
•An area of attachment to the underlying
vessel or heart wall, frequently firmest at
the point of origin, is characteristic of all
thrombosis
67

68
•Thrombi may develop anywhere in the
cardiovascular system, but stasis is a
major factor in the development of
venous thrombi
Abnormal aortic and arterial dilations called
aneurysms create local stasis and a fertile site
for thrombosis
Acute myocardial infarction results in focally
noncontractile myocardium, ventricular
remodeling can lead to aneurysm formation

• Measurement of fibrin D-dimer are helpful in
diagnosing abnormal thrombotic states including
disseminated intravascular coagulation CIC, deep
venous thrombosis DVT, or pulmonary
thromboembolism PTI.
• Thrombus formation within the cardiac chambers
after endocardial injury due to myocardial
infarction, over ulcerated plaques in atherosclerotic
arteries, or at sites of traumatic or inflammatory
vascular injury, is largely a function of endothelial
injury. So exposure of subendothelial ECM, adhesion
of platelets, release of tissue factor, and local
deplation of PGI2, and plasminogen activators.
69

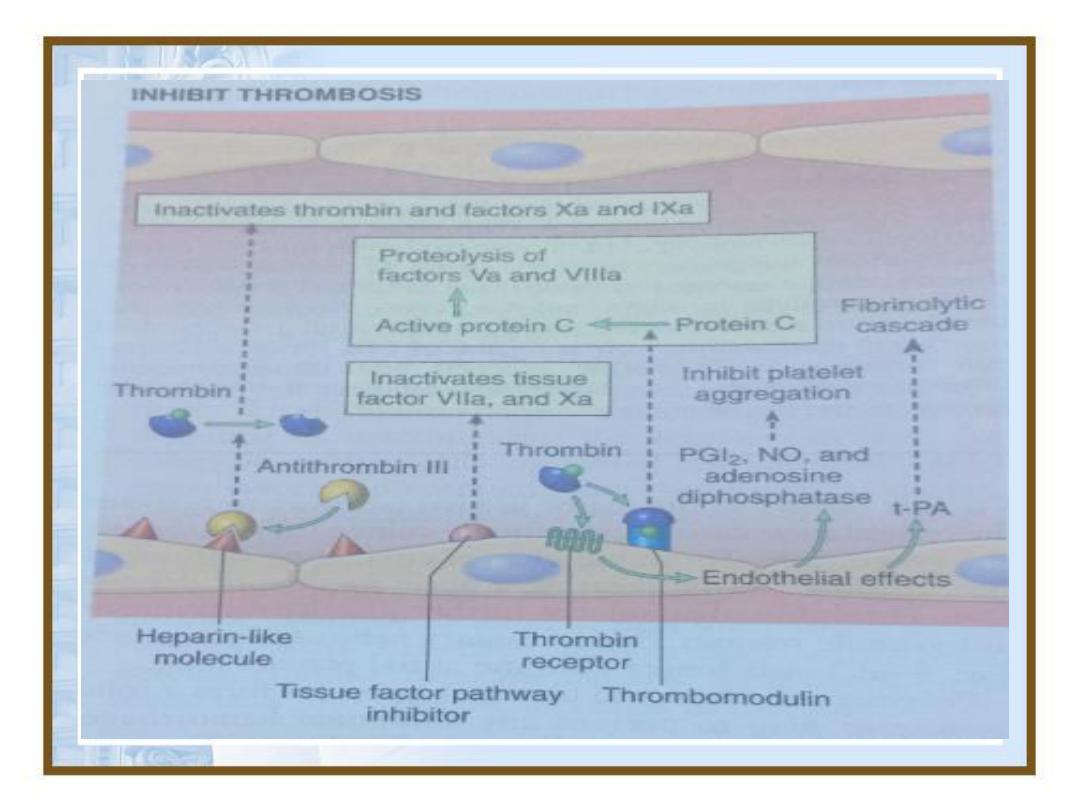
• However, it is important to note that endothelium
need not to denuded or physically disrupted to
contribute to the development of thrombosis, any
perturbation in the dynamic balance of the
prothrombotic and antithrombotic activities of
endothelium can influence local clotting events.
• Dysfunctional endothelium may elaborate greater
amounts of procoagulant factors like platelet
adhesion molecules, tissue factor, plasminogen
activator inhibitors or may synthesize fewer
anticoagulant effectors (thrombomodulin, PG2, t-PA)
• Endothelial dysfunction may occur with
hypertension, turbulent flow over scarred valves, or
by the action of bacterial endotoxins.
70

71
•The propagating tail may not be well
attached and, particularly in veins, is
prone to fragmentation, creating an
embolus.
•Mural thrombi-arterial thrombi that
arise in heart chambers or in the aortic
lumen, that usually adhere to the wall
of the underlying structure


73
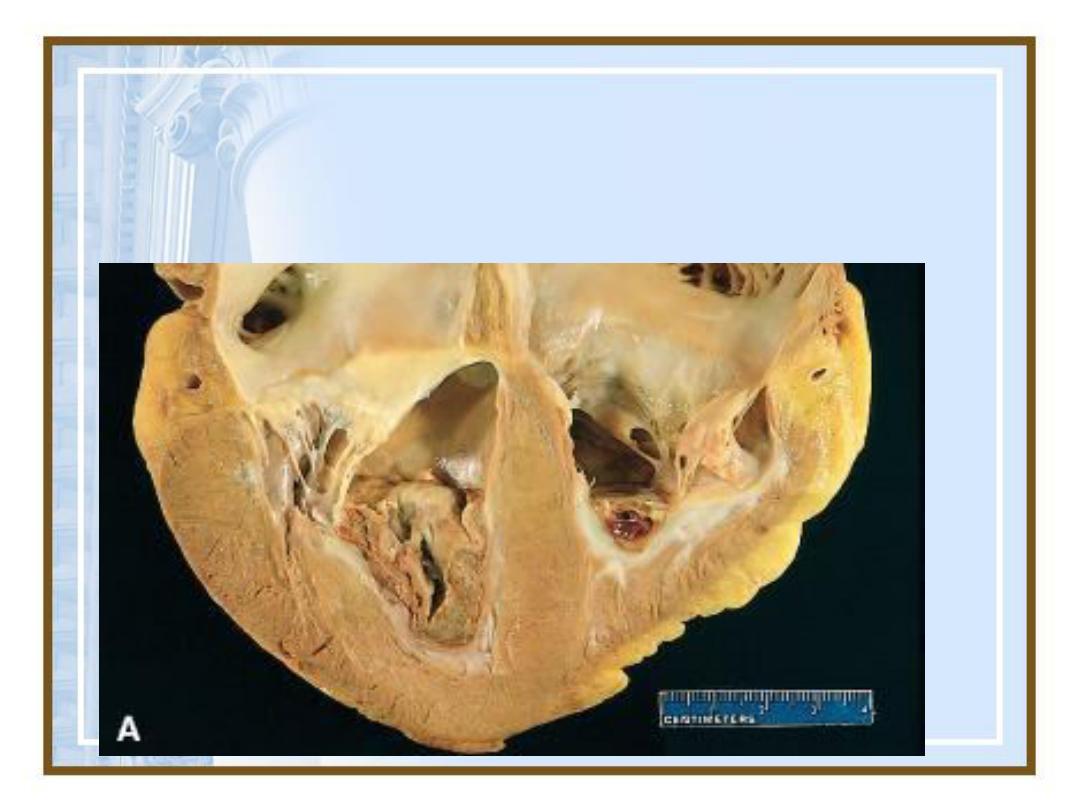
Lines of Zahn:
alternating layers
of platelets and
fibrin in the
thrombus

75
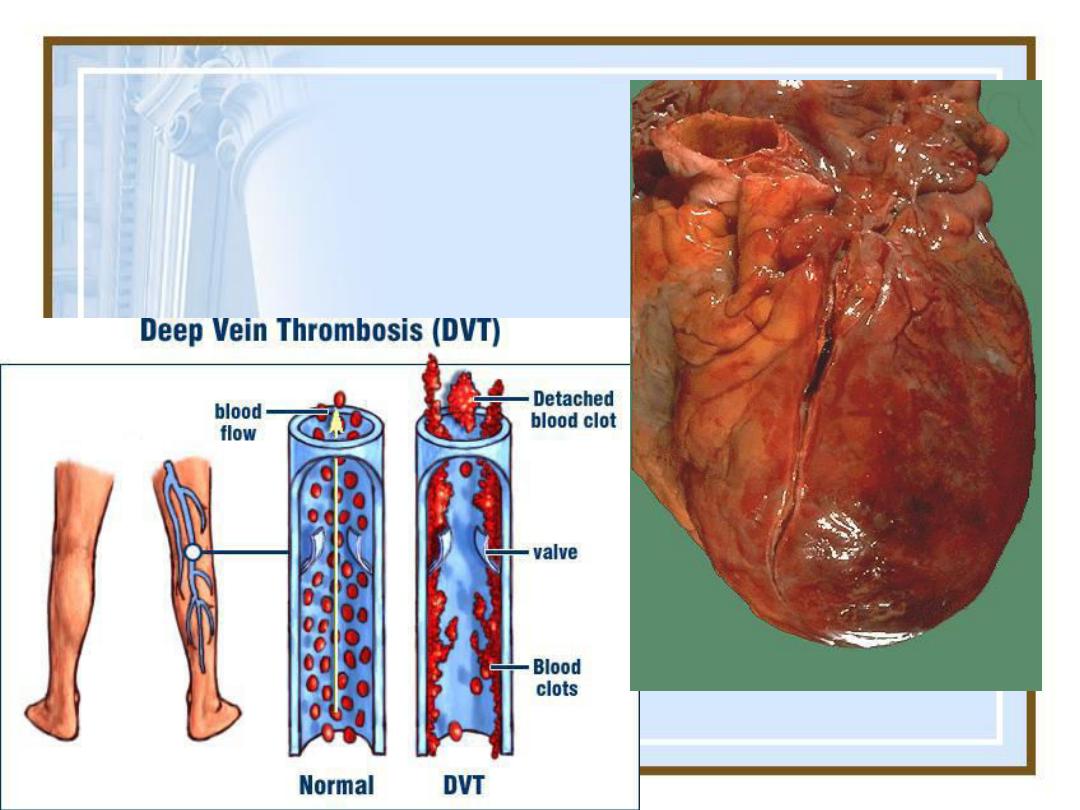
•Mural thrombi. Thrombus in the left and
right ventricular apices, overlying awhite
fibrous scar.
76
Thrombosis

77
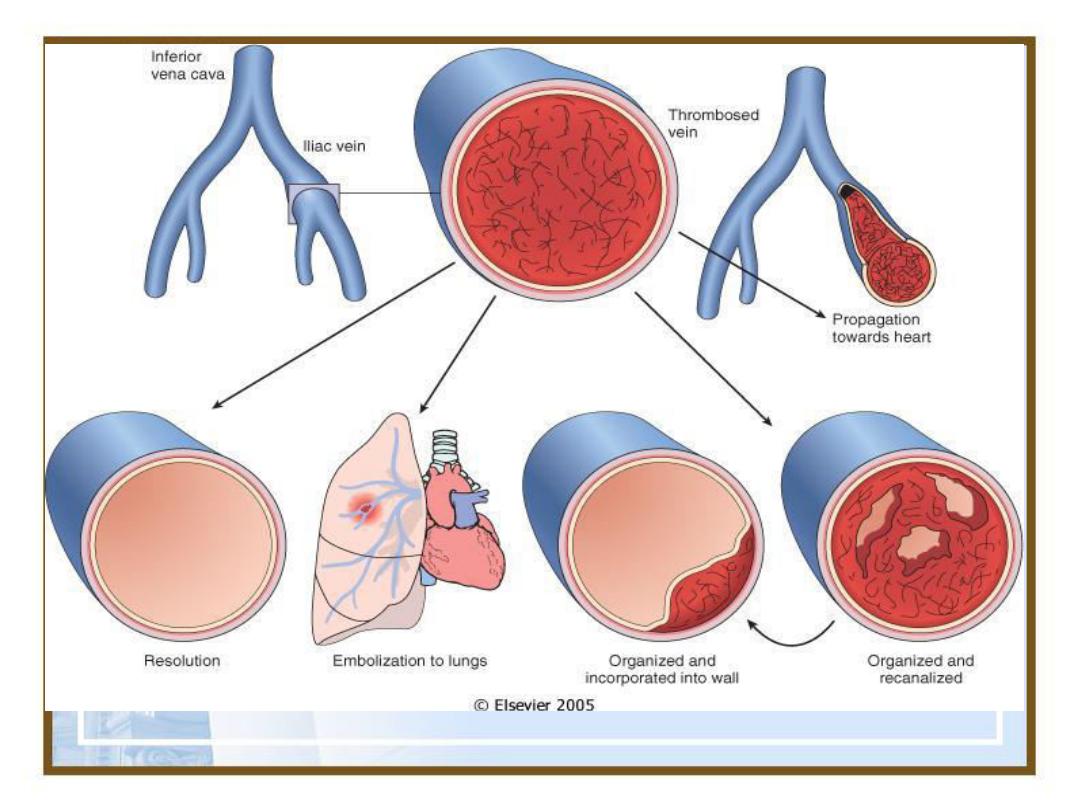
•Fate of the Thrombus.
1. Propagation: Thrombi accumulate additional
platelet and fibrin
2. Embolization: Thrombi dislodge or fragment
are transported elsewhere in the vasculature
3. Dissolution: Thrombi removed by fibrinolytic
activity
4. Organization and recanalization: Thrombi
induce inflammation and fibrosis, these can
eventually recanalize, or they can be
incorporated into a thickened vessel wall
78
•Potential outcomes of venous thrombosis.
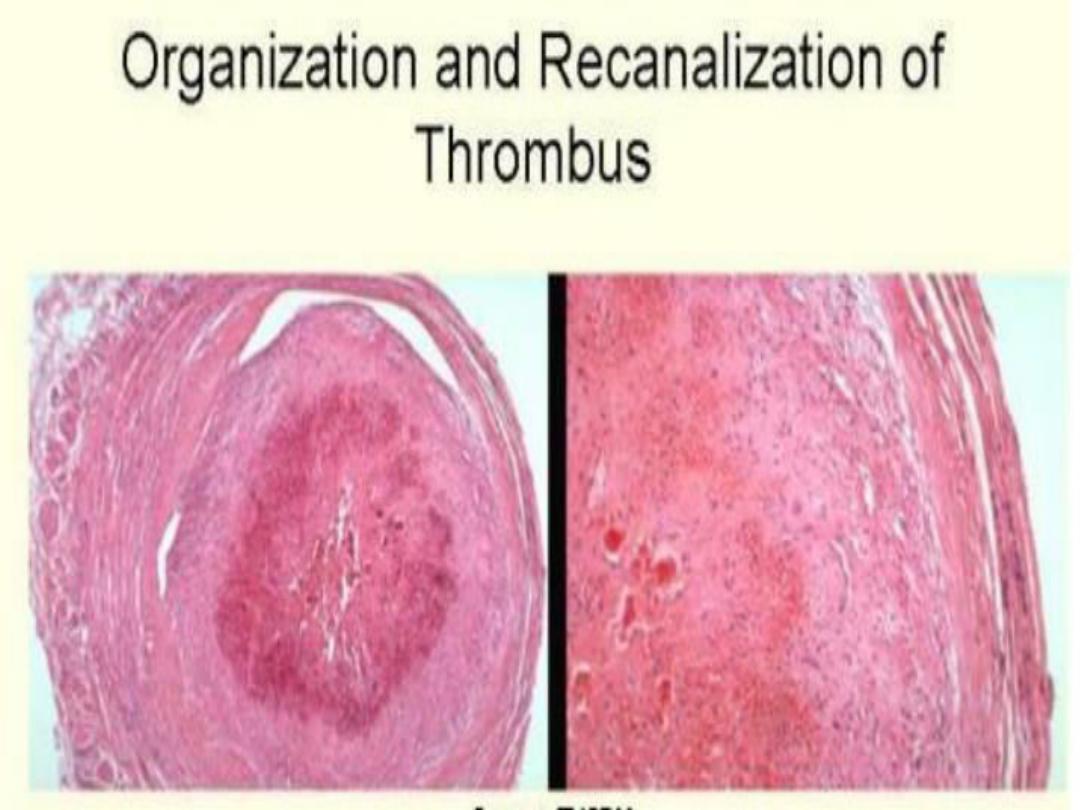
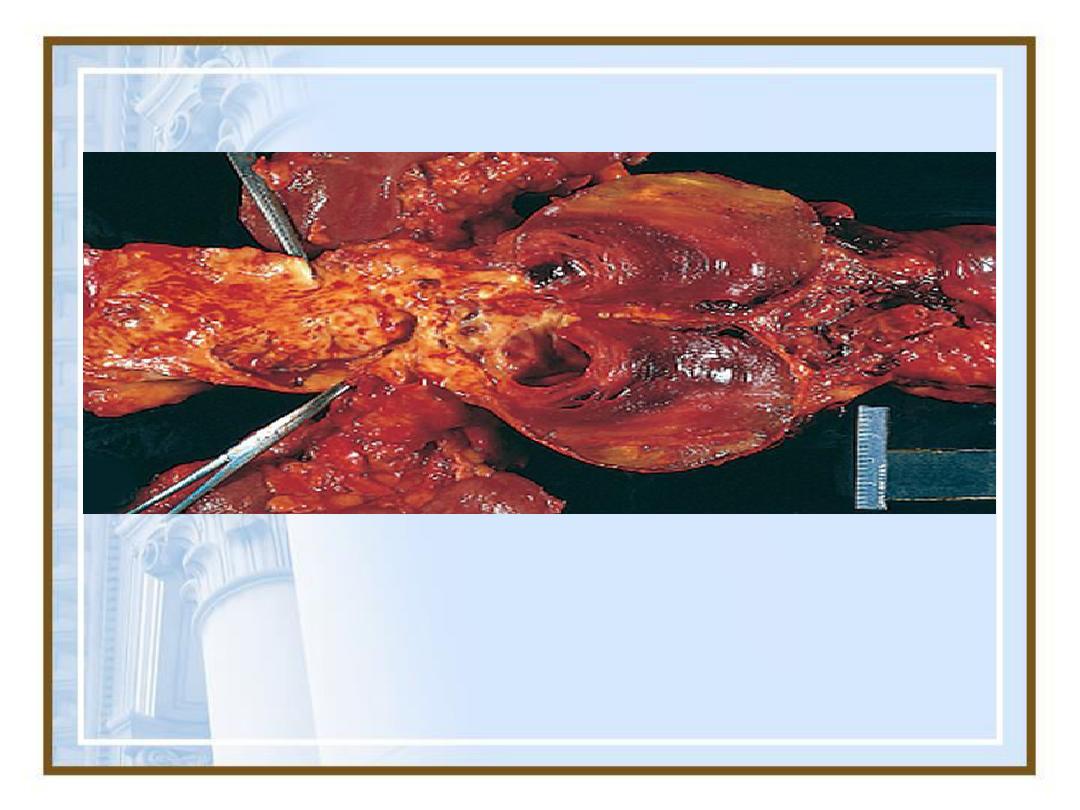
80
Mural thrombi.
Laminated thrombus in a dilated abdominal
aortic aneurysm.
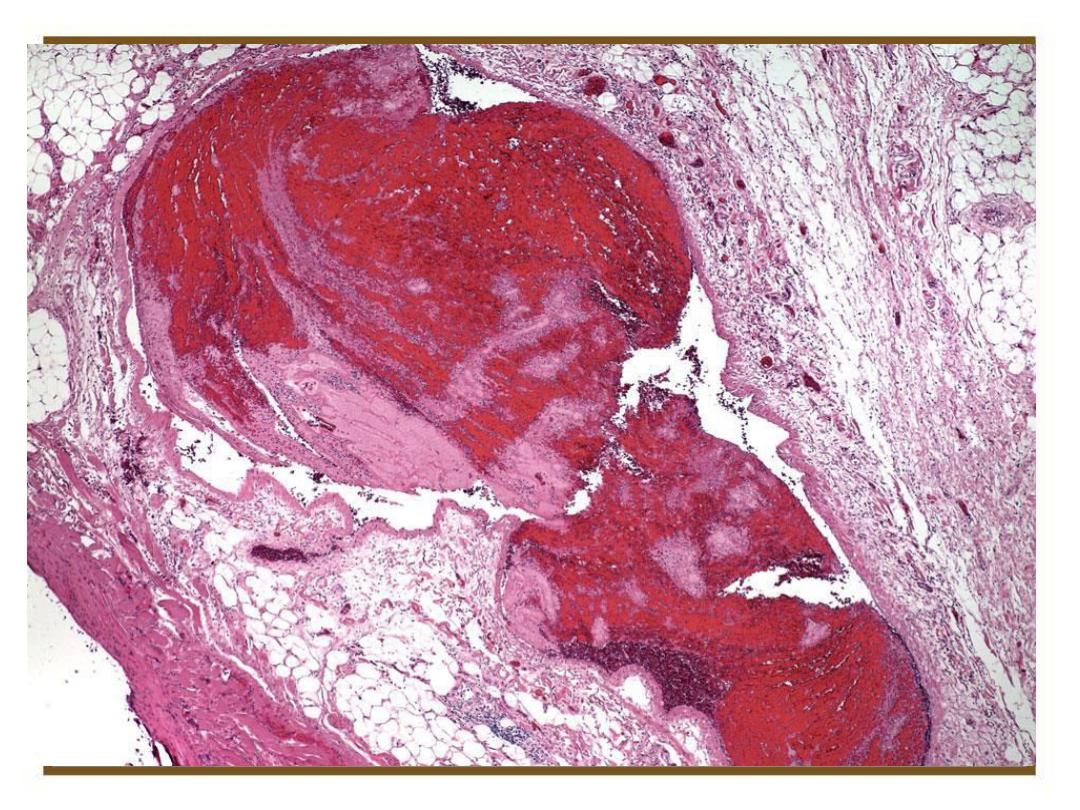
81

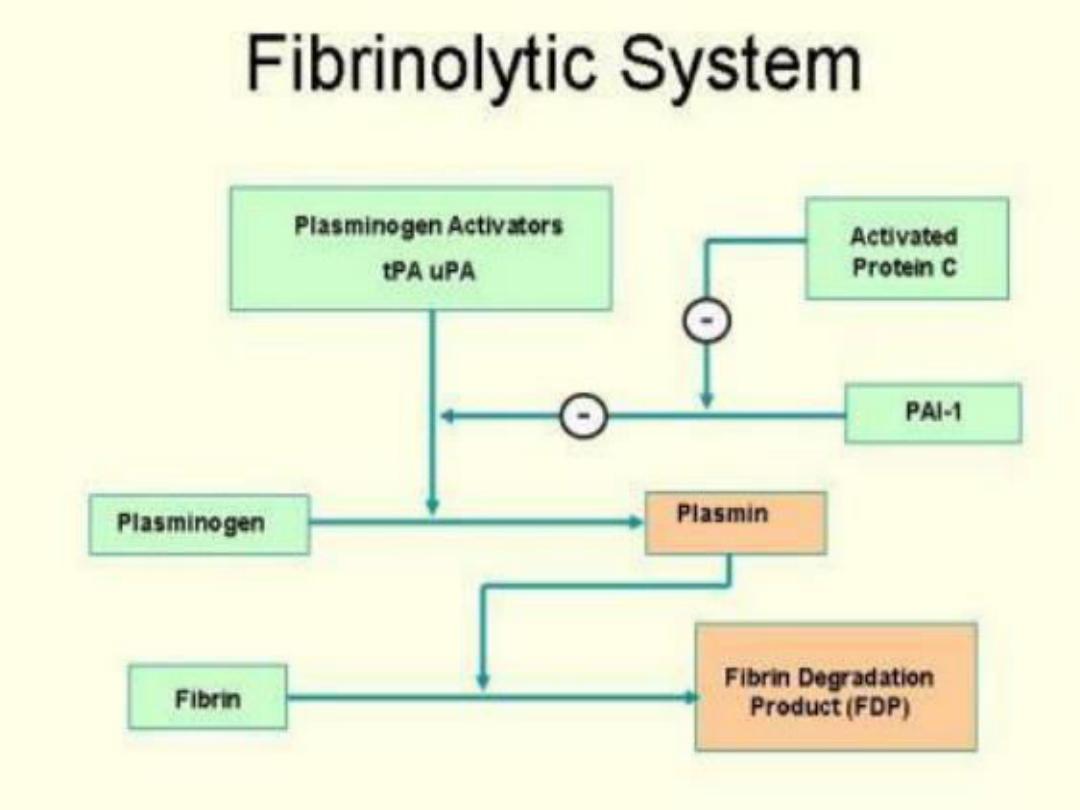
Dissolution of clots
• As damaged B.V wall is repaired, activated
factor X11 promotes the conversion of an
inactive molecule in plasma into the active
form called Kallikrein which in turn
catalyzes the conversion of inactive
plasminogen into the active molecule
plasmin .
• Plasmin is an enzyme that digests fibrin into
split products, promoting dissolution of the
clot.
82

83
5-Embolism

84
•An
embolus
is a detached intravascular solid,
liquid, or gaseous mass that is carried by the
blood to a site distant from its point of origin.
•
Emboli
lodge in vessels too small to permit
further passage, resulting in partial or complete
vascular occlusion

85
Pulmonary Thrombo-embolism
•95% of venous emboli originate from deep
leg vein thrombi above the level of knee,
carried through large channels and pass
through right side of the heart before entering
pulmonary vasculature.
May occlude the main pulmonary artery
impact across the bifurcation, saddle
embolus, or pass out into the smaller
branching arterioles.
patient who has had one pulmonary embolus
is at high risk of having more
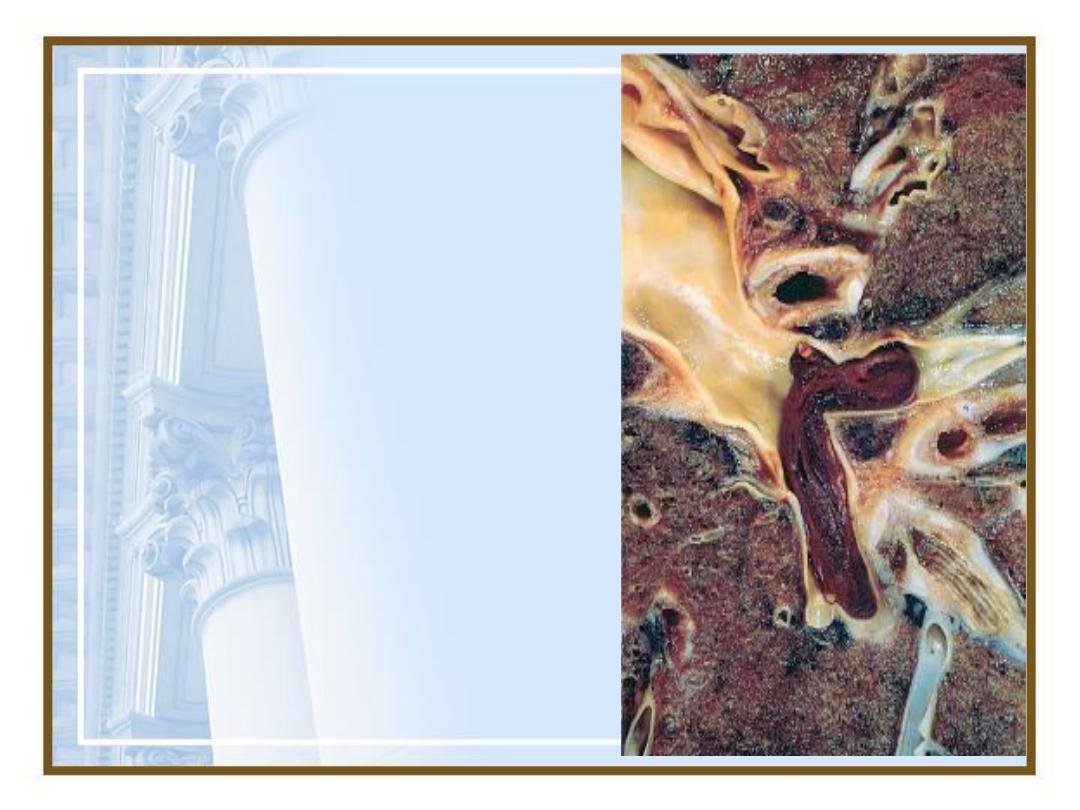
86
•Large embolus
derived from a lower
extremity deep venous
thrombosis and now
impacted in a
pulmonary artery
branch.

87
Systemic Thromboembolism
•Emboli traveling within the arterial circulation.
•Most (80%) arise from intra-cardiac mural
thrombi,
•Two thirds of which are associated with left
ventricular wall infarcts and another quarter with
dilated left atria
•The major sites for arteriolar embolization:
1.
Lower extremities (75%)
2.
Brain (10%)

88
A-Fat Embolism
•Microscopic fat globules may be
found in the circulation after fractures
of long bones (which have fatty
marrow) or, rarely, in the setting of soft
tissue trauma and burns
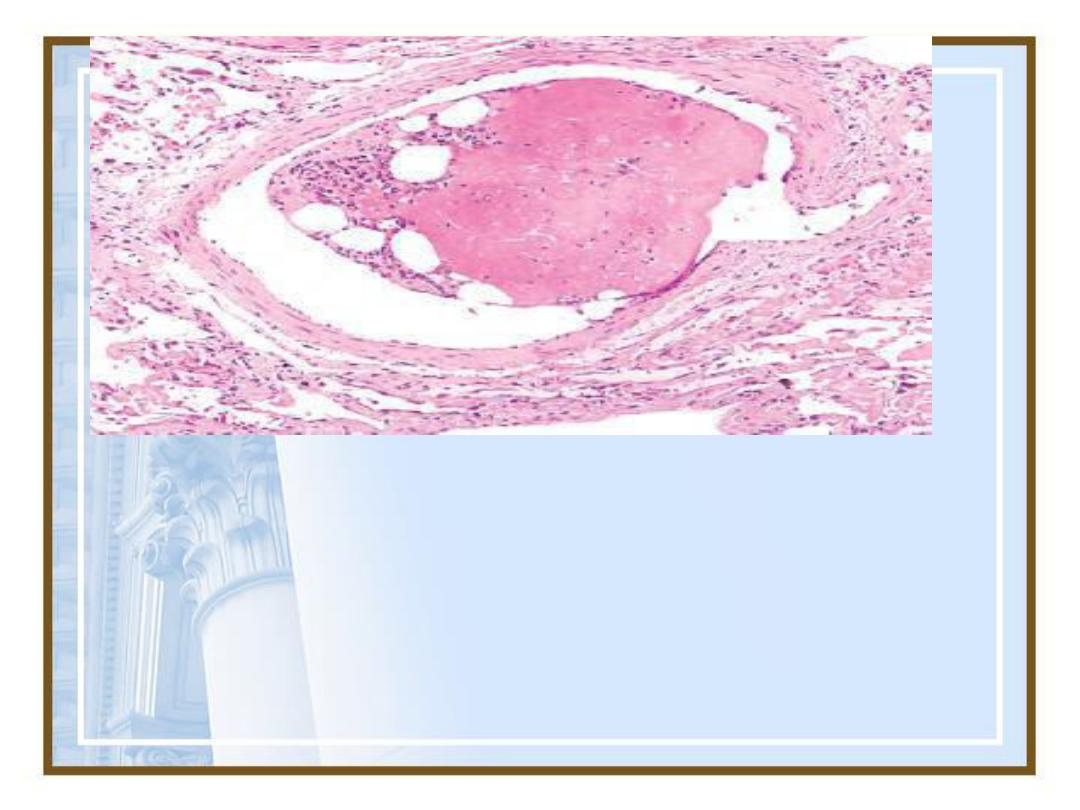
89
•Bone marrow embolus in the pulmonary circulation.
The cleared vacuoles represent marrow fat that is now
impacted in a distal vessel along with the cellular
hematopoietic precursors.

90
B-Air Embolism
•Gas bubbles within the circulation
can obstruct vascular flow.
•Enter the circulation during
obstetric procedures or as
aconsequence of chest wall injury.
•In excess of 100mL is required to
have a clinical effect

91
C-Amniotic Fluid Embolism
•Underlying cause is the infusion of
amniotic fluid or fetal tissue into the
maternal circulation via a tear in the
placental membranes or rupture of
uterine veins.
•Characterized by sudden severe
dyspnea, cyanosis, and hypotensive
shock, followed by seizures and coma.

92
6-Infarction

93
•An
infarct
is an area of ischemic necrosis
caused by occlusion of either the
arterial
supply
or
the venous
drainage
in a
particular tissue.
•Nearly 99% of all infarcts result from
thrombotic or embolic events, and almost
all result from arterial occlusion

94
•Infarcts are classified on the basis
of their
color
(reflecting the amount
of hemorrhage) and
the presence or
absence of microbial infection

95
•Red (hemorrhagic) infarcts occur
(1)
With venous occlusions (such as in
ovarian torsion);
(2)
In loose tissues (such as lung)
(3)
In tissues with dual circulations
(e.g.,lung and small intestine).

96
•White (anemic) infarcts occur
With arterial occlusions in solid organs
with end-arterial circulation (such as
heart,spleen,and kidney)
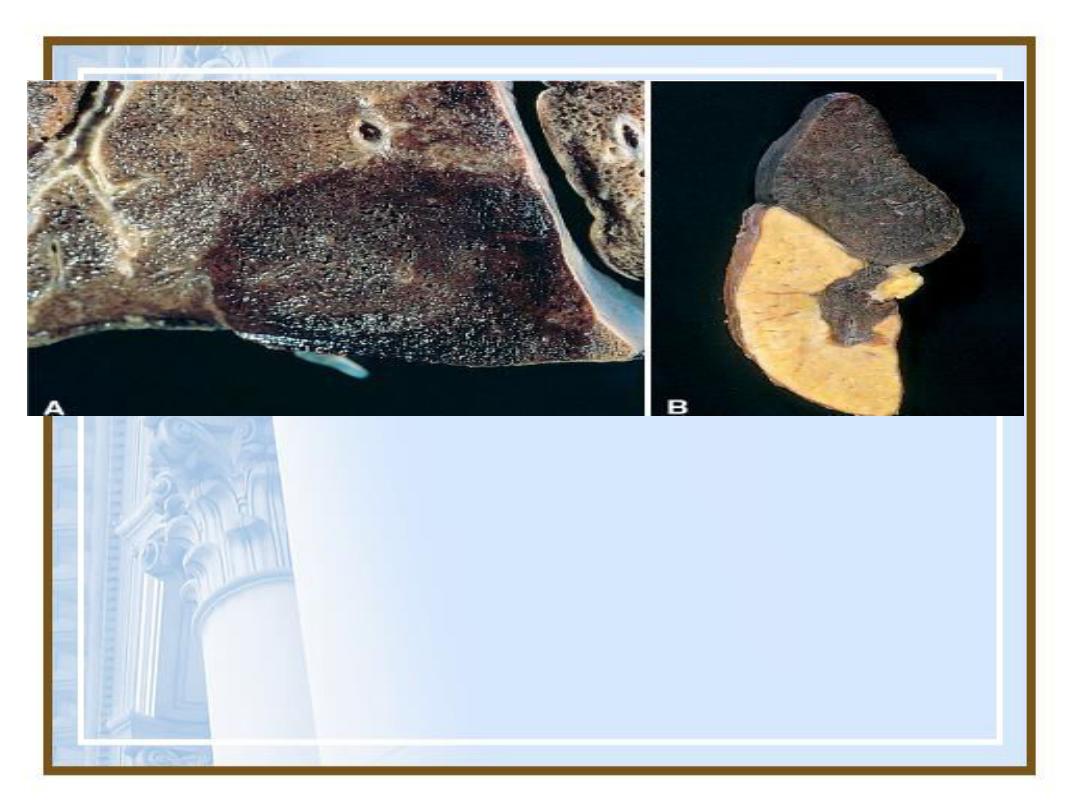
97
Examples of infarcts. (A)
Hemorrhagic, roughly wedge-
shaped pulmonary infarct. (B)
Sharply demarcated white infarct in
the spleen.

98
•The dominant histologic
characteristic of infarction is
ischemic coagulative necrosis
•most infarcts are ultimately replaced
by
scar tissue
.
•The brain is an exception to these
generalizations; ischemic injury in
the central nervous system results in
liquefactive necrosis

99
•
Septic infarctions
may develop
when embolization occurs by
fragmentation of a bacterial
vegetation from a heart valve or
when microbes seed an area of
necrotic tissue.

100
7-Shock

101
•Shock
, or
cardiovascular collapse
,
is the final common pathway for a
number of potentially lethal clinical
events, including severe
hemorrhage, extensive trauma or
burns, large myocardial infarction,
massive pulmonary embolism, and
microbial sepsis.

102
•gives rise to systemic hypo-
perfusion caused by reduction in:
1.Cardiac output
2.The effective circulating blood
volume.
•The end results are hypotension,
followed by impaired tissue
perfusion and cellular hypoxia
103
Type of shock
Clinical examples
Principal mechanism
Cardiogenic
-ventricular rupture
-arrythmia
-cardiac tamponade
-pulmonary embolism
-M.I
Failure of myocardial
pumps owing to intrinsic
myocardial damage,
extrinsic pressure,
or outflow obstruction in
pulmonary Embolism.
Hypo-volemic
-hemorrhage
-fluid loss ; e.g . Vomiting ,
diarrhea , burns , trauma
Inadequate blood or
plasma volume
Septic
-overwhelming microbial
infection
-endotoxic shock
-Gram positive septicemia
-Fungal sepsis.
Peripheral vasodilatation &
pooling of blood,
endothelial activation /
injury;leukocytes induced
damage;DIC ;activation of
cytokine cascade

104
Less commonly:
1.Neurogenic shock
-in the setting of
anesthetic accident or spinal cord injury,
owing to loss of vascular tone and
peripheral pooling of blood.
2.Anaphylactic shock,
initiated by a
generalized IgE-mediated
hypersensitivity response, is associated
with systemic vasodilatation and
increased vascular permeability

105
Clinical Course
•The clinical manifestations depend on the
precipitating insult.
•In
hypovolemic
and
cardiogenic shock
,
the patient presents with hypotension;
aweak, rapid pulse; tachypnea; and cool,
clammy, cyanotic skin.
•In
septic shock
, the skin may initially be
warm and flushed because of peripheral
vasodilation
