• By
Dr. Monia MN Kandilصناعة اسنان \ خامس
د. زينة م4
1-12-2016
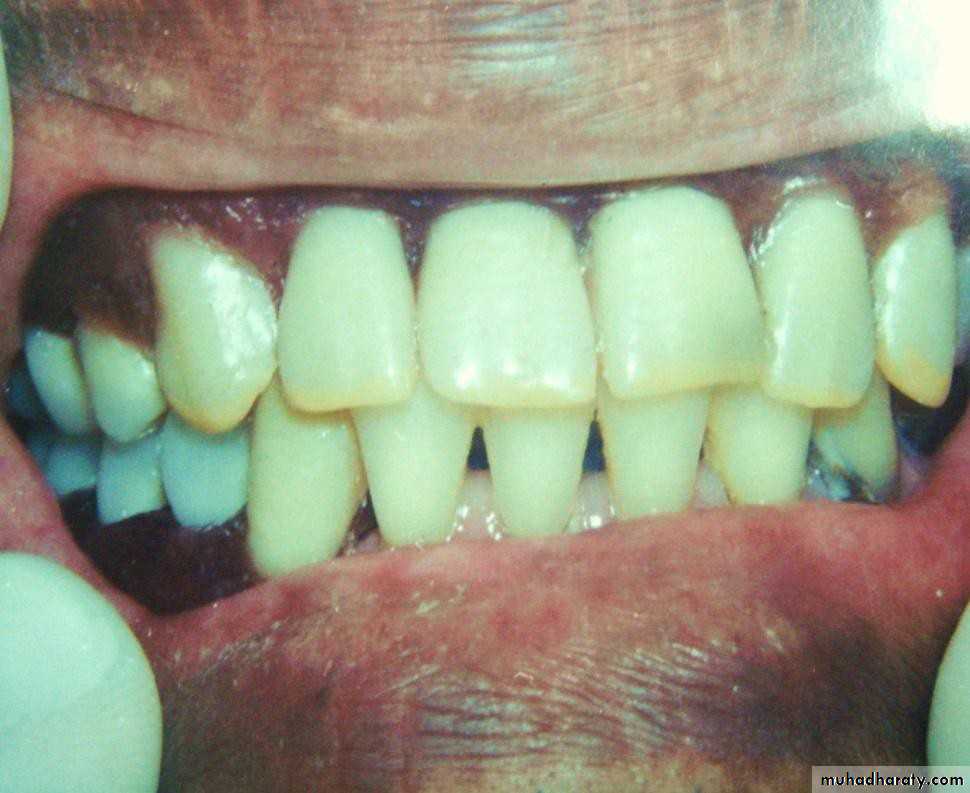
• Any removable dental prosthesis that
• completely or partially covers and rests on one or more remaining natural teeth, the roots of natural teeth, and/or dental implants; is called• overlay denture, overlay (superimposed)
• prosthesis .
• (Glossary of prosthodontic terms, 2005)
• Definition of Overdentures
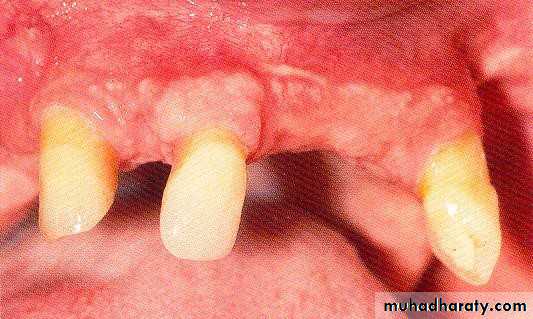
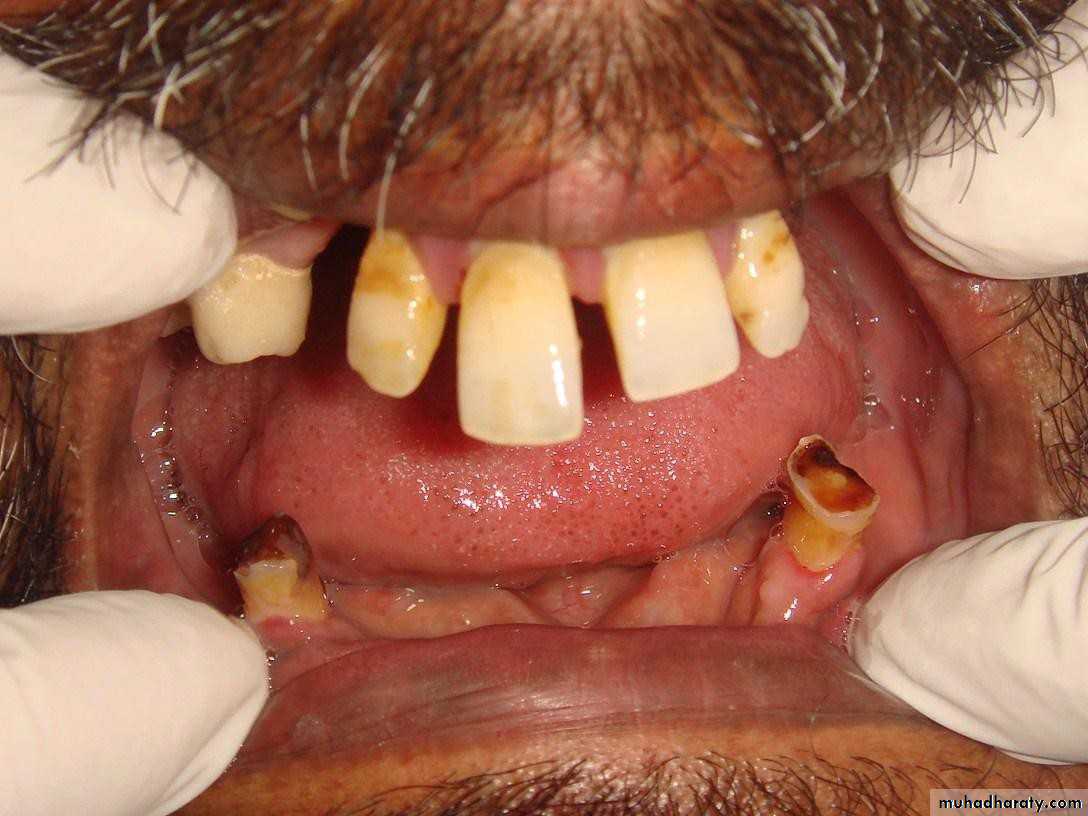
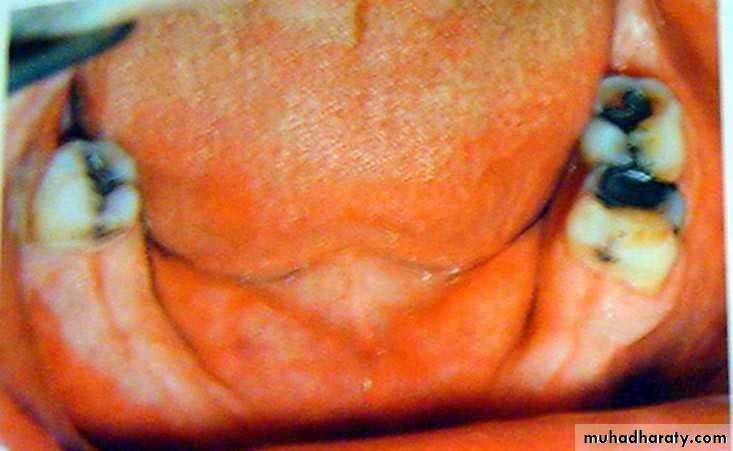
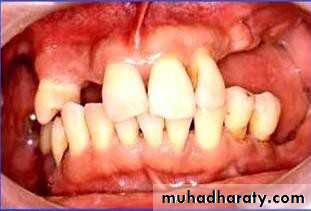
• 1) Few remaining teeth or teeth with an unfavourable distribution in the arch which precludes treatment with a removable P.D.
• 2) Severe loss of periodontal attachment in a patient who cannot afford a fixed partial denture
• 3) Complicated functional and aesthetic conditions due to tooth migration which make restoration with a removable or fixed partial denture difficult.
• 4) Significant tooth loss due to attrition.
• 5) Congenital absence of teeth i.e. Partial anodontia.
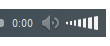
• 1) Preservation of the alveolar ridge.
• 2) Enhanced retention of the tooth in the jaw
• (reduced C/R ratio)• 3) Enhancement and maintenance of denture
• stability .• 4) Maintenance of the patient’s neuromuscular control and prevention of masticatory muscle atrophy .
• 5) Mental and functional comfort of the patient
• 6) Enhanced retention of the denture.• 1) Overdentures are occasionally bulkier than
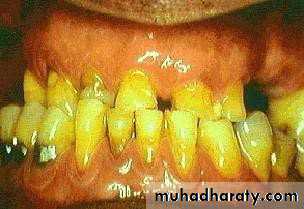
• conventional dentures.• 2) Susceptibility of the abutment teeth to caries periapical disease , periodontal disease and vertical root fractures.
• 3) Increased demand for
• the patient’s• motivation towards oral hygiene.
• 4) More time consuming chair-side , more recall visits and higher cost.
• 5) The patient applies more load on the overdenture which is inherently weaker due to the space occupied by the root(s).
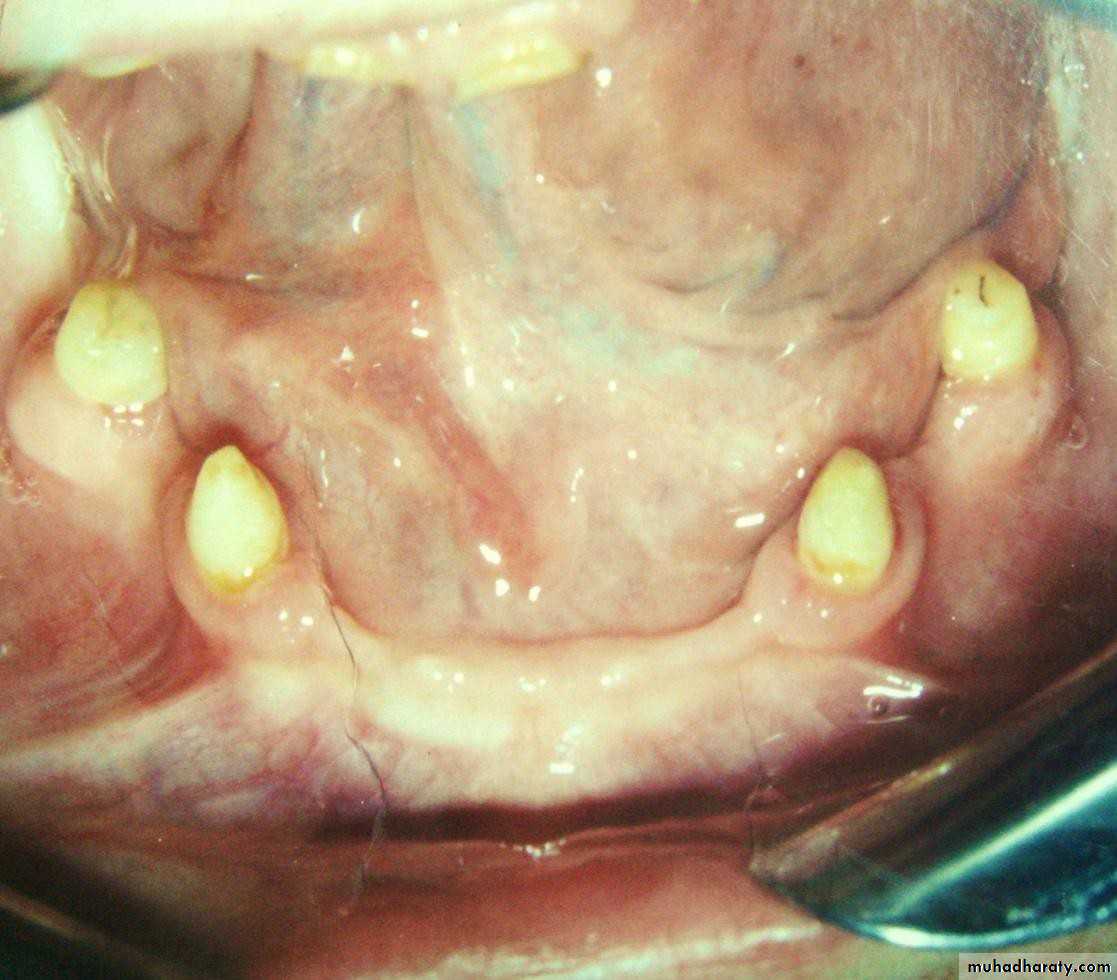
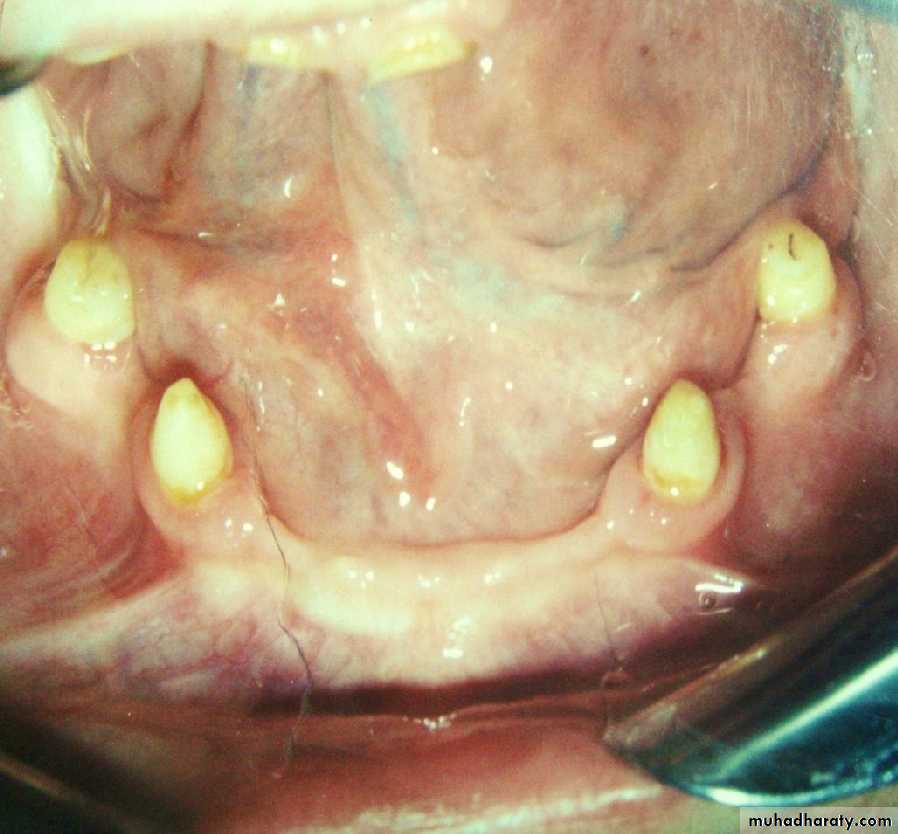
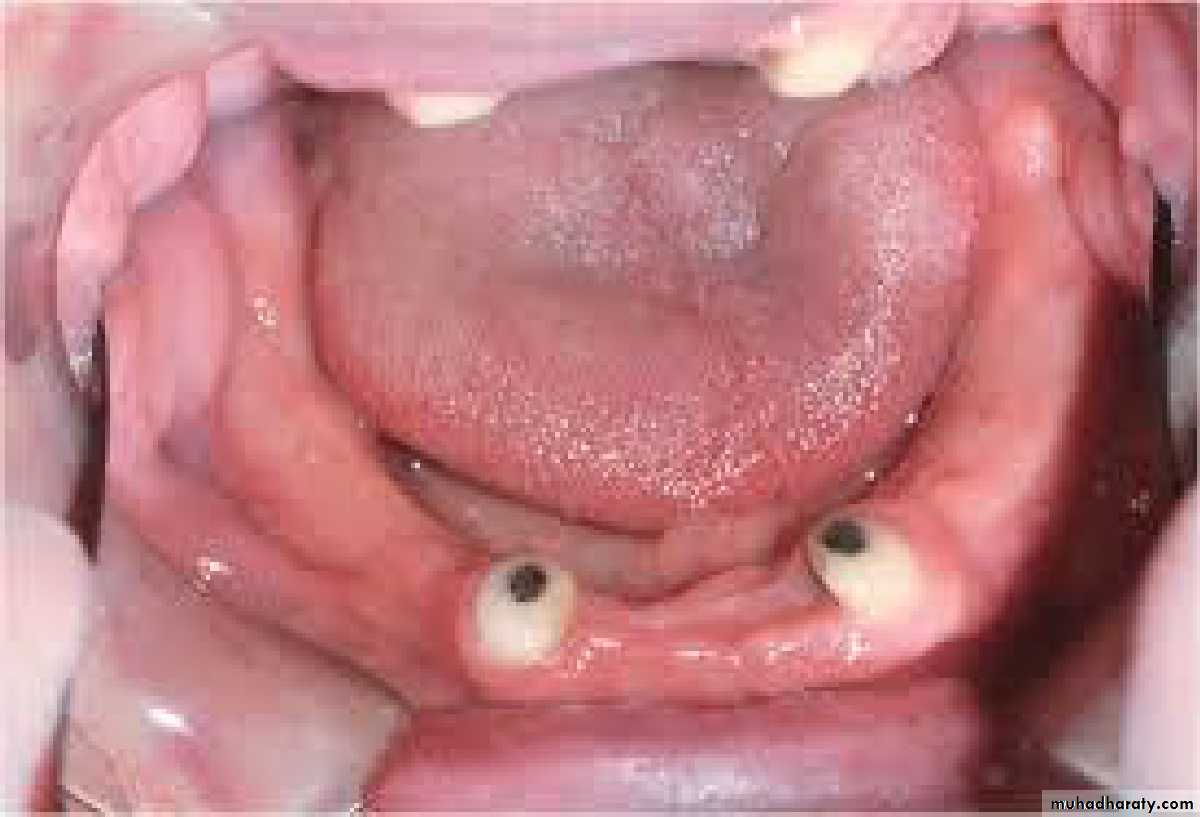
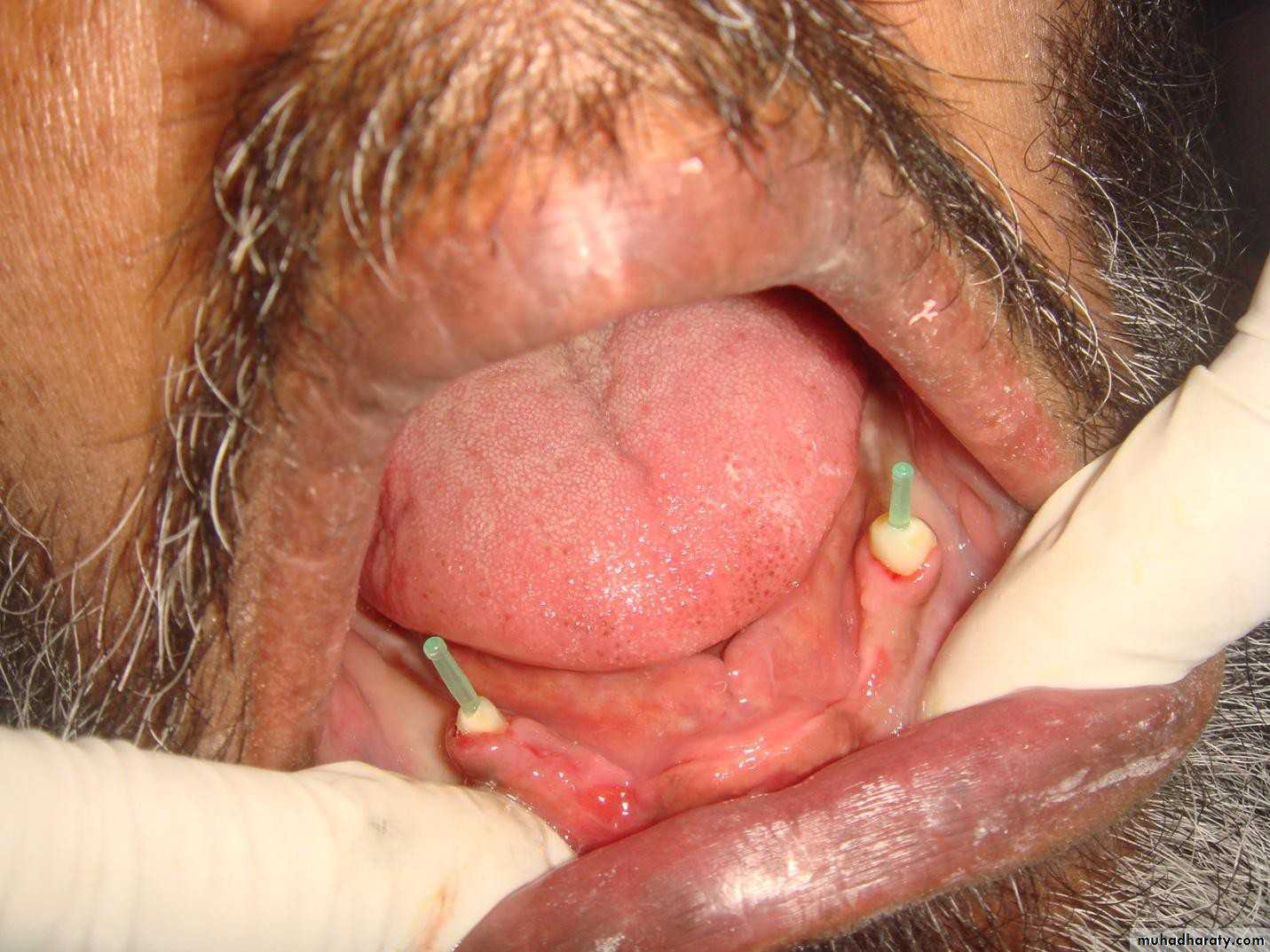
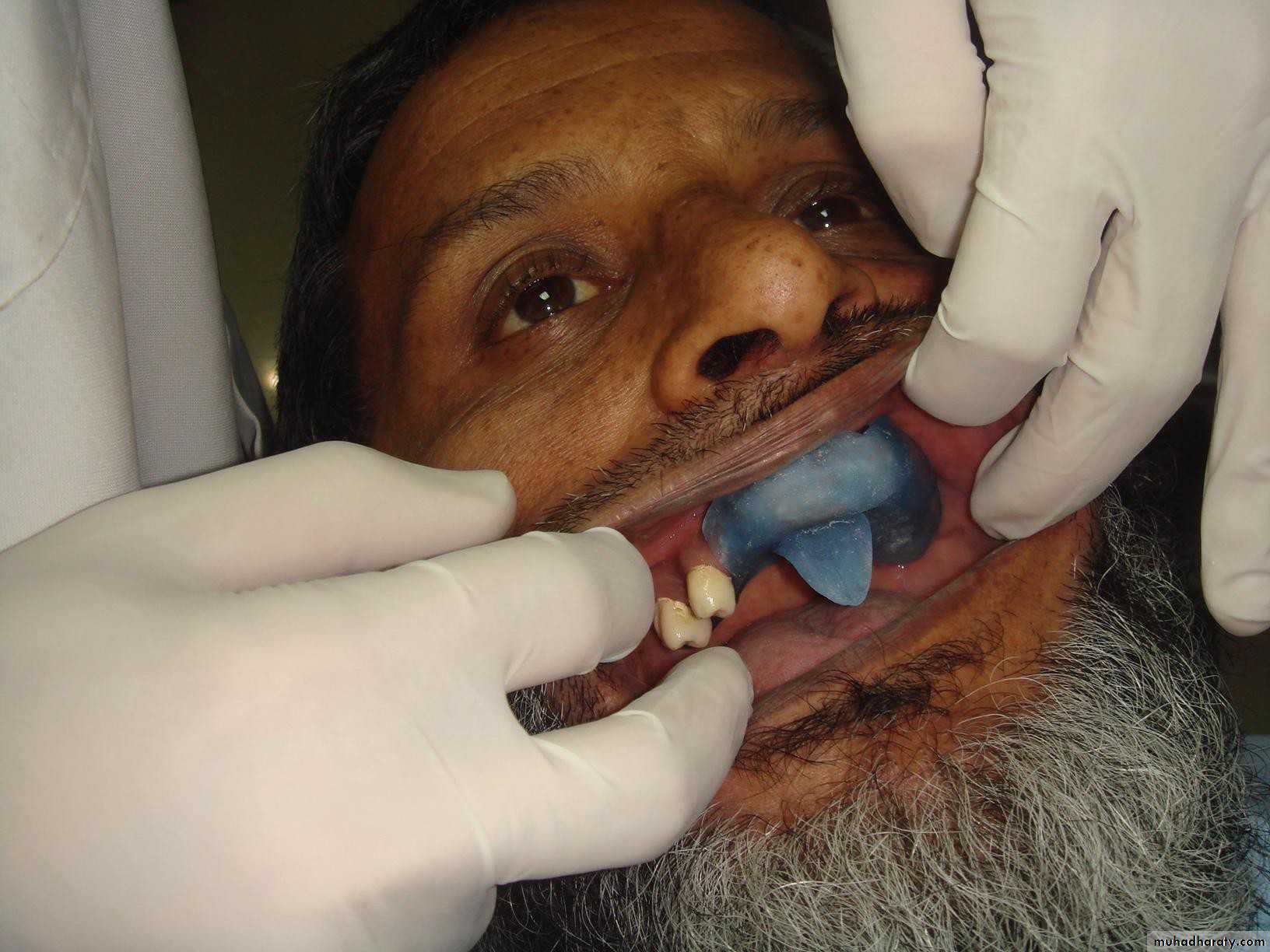
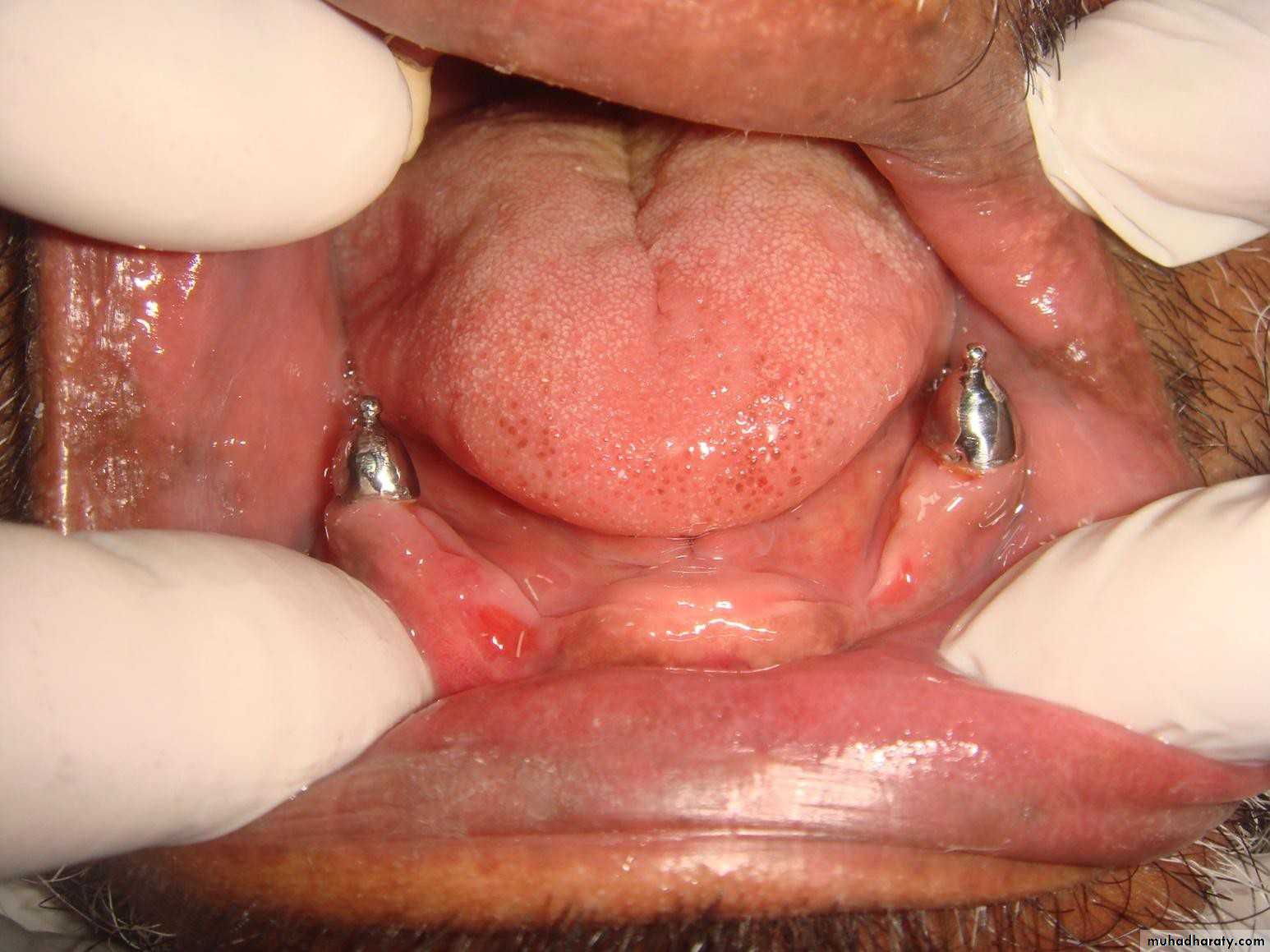
• Tooth supported
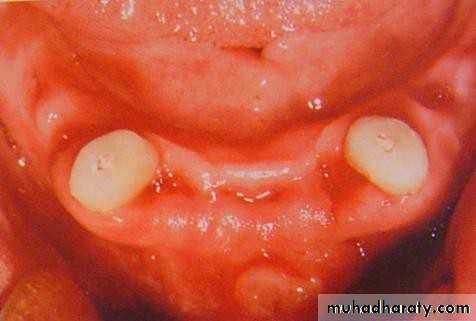
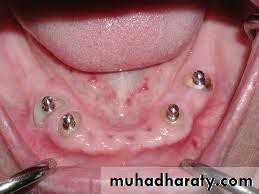
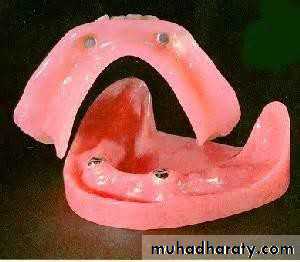
• Implant supported• 1) Tooth supported overdentures.
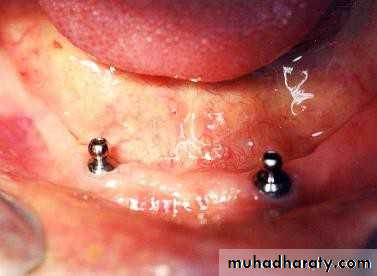
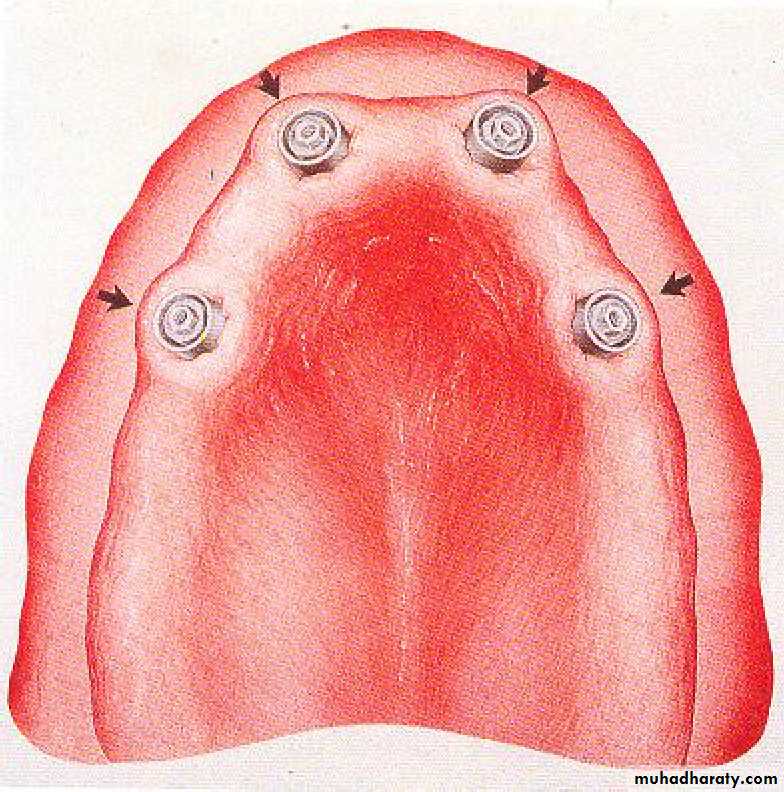
• 2) Implant supported overdentures.
• “According to design and technique of
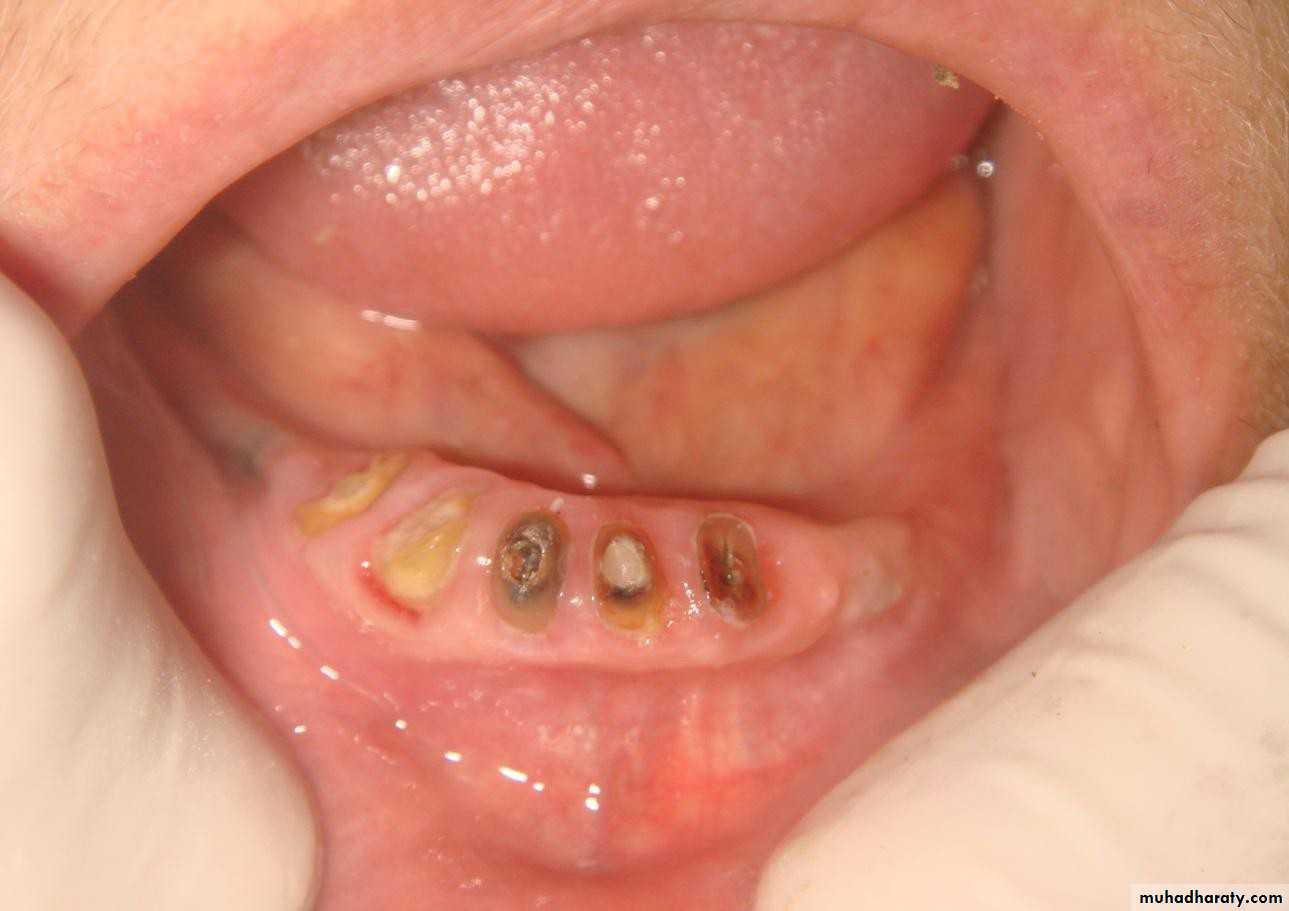
• abutment preparation”• 1- Simple tooth reduction of vital abutment. 2- Tooth reduction and cast coping of
• vital
• abutment / thimble or dome- shaped.
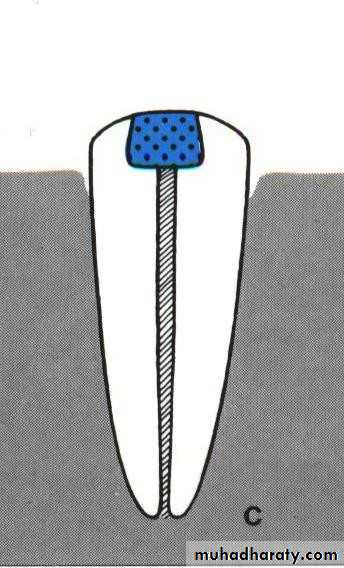
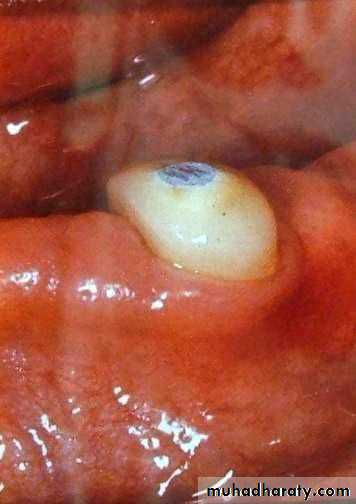
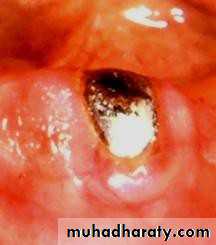
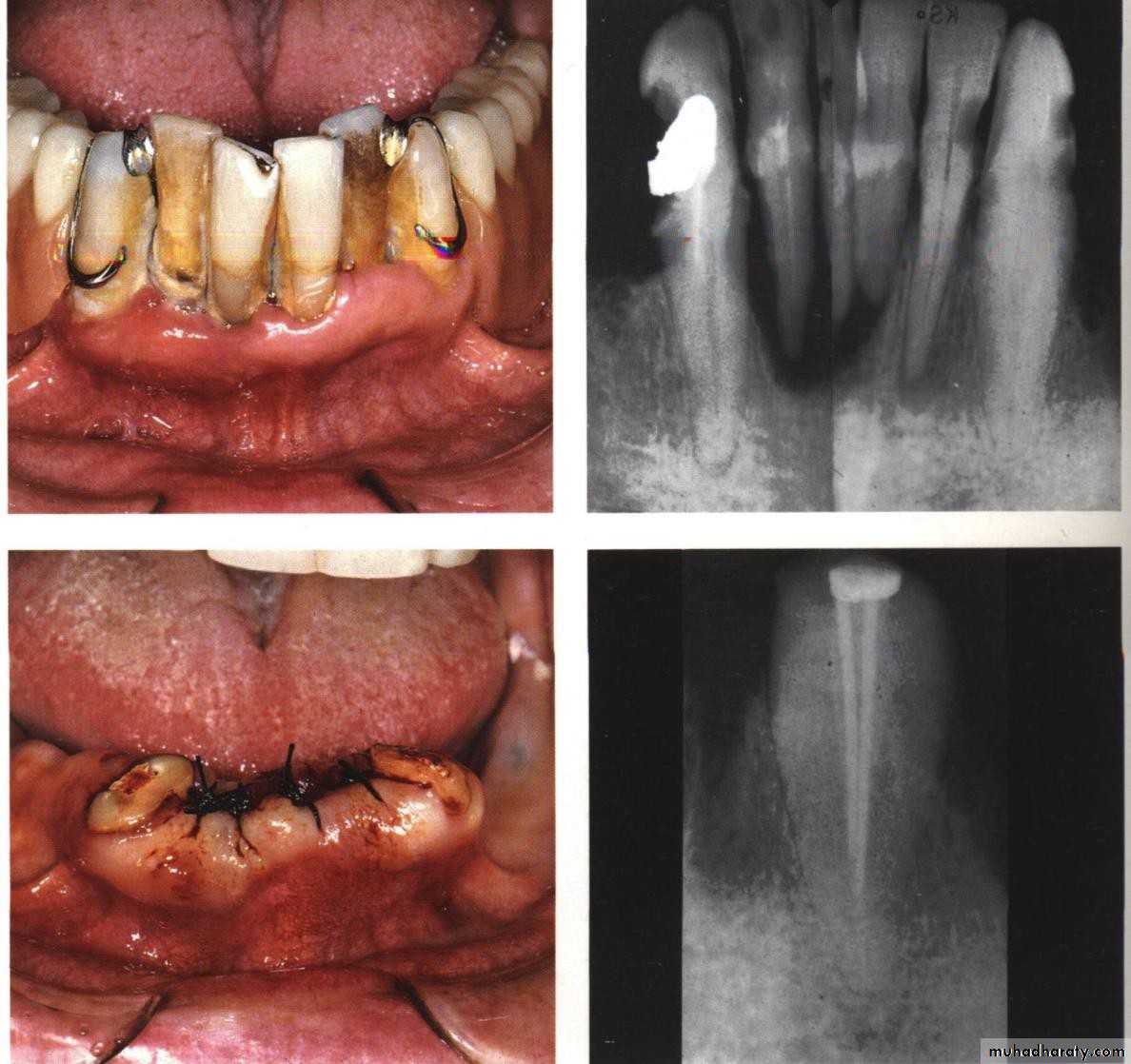
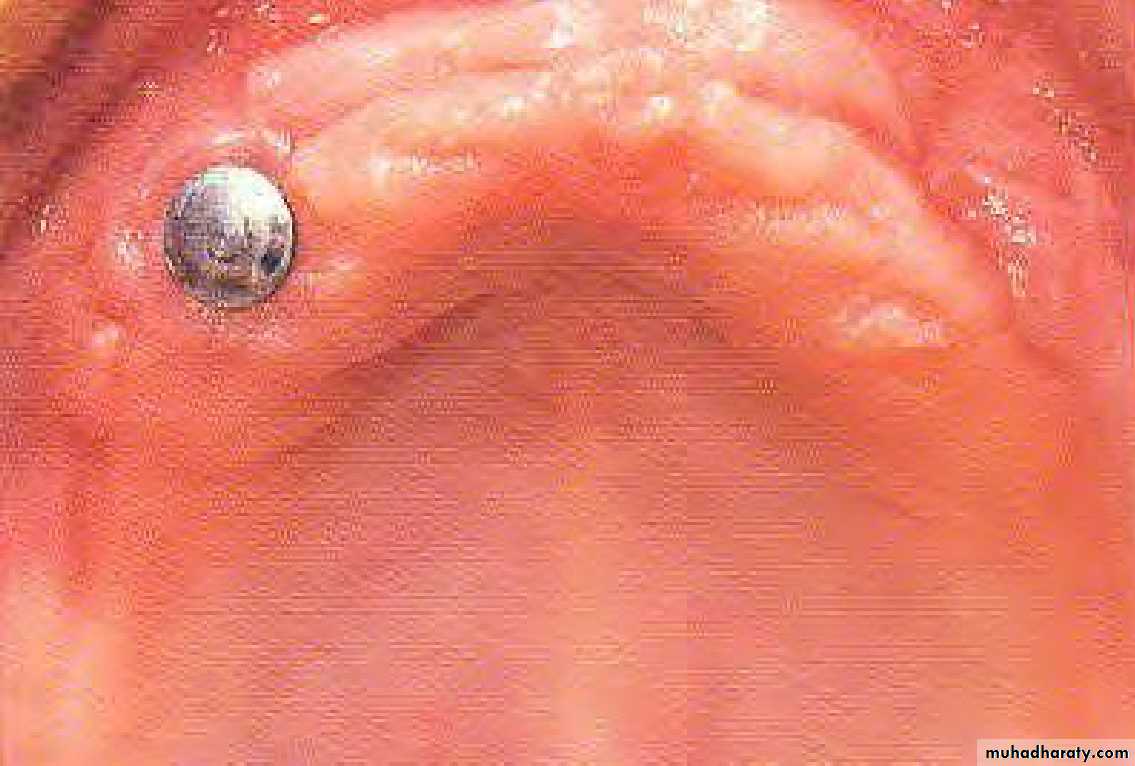
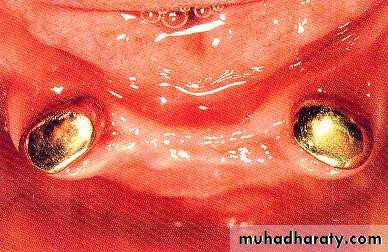
• Endodontic therapy and amalgam plug.
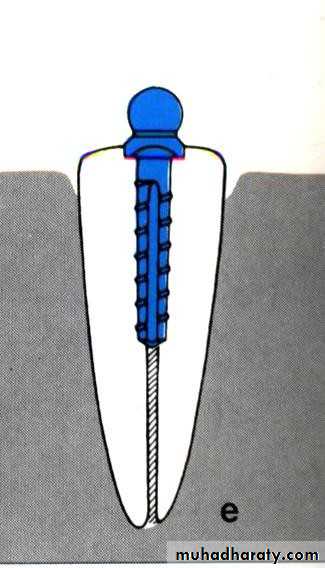
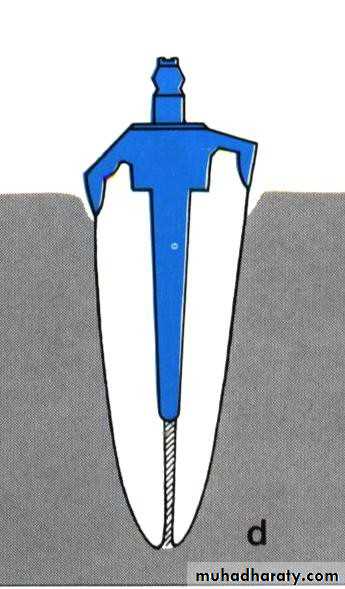
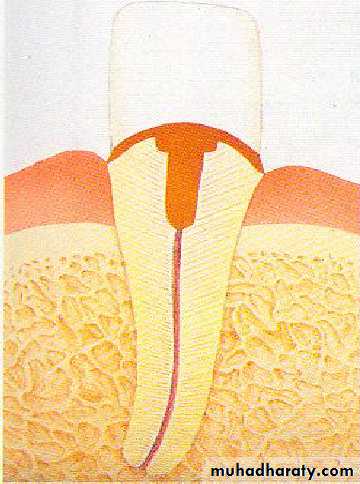
• Endodontic therapy with post and coping.
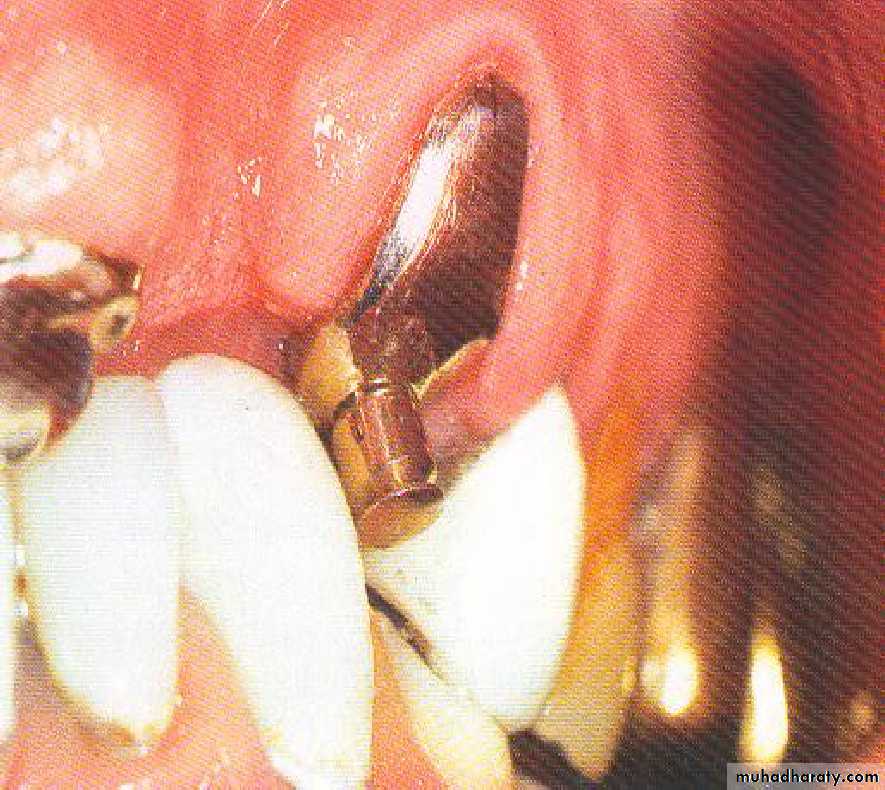
• Endodontic therapy with cast coping and attachments.
• Telescopic Overdenture.
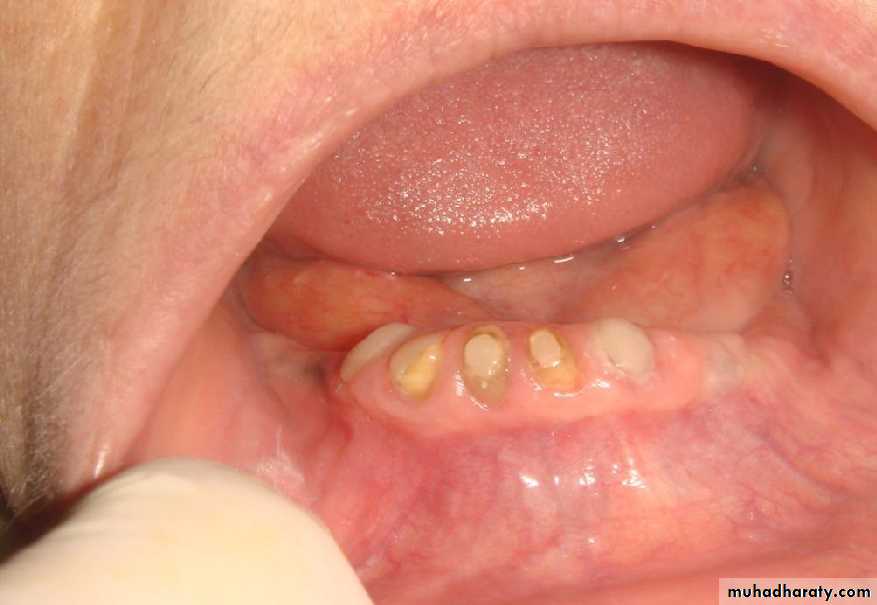
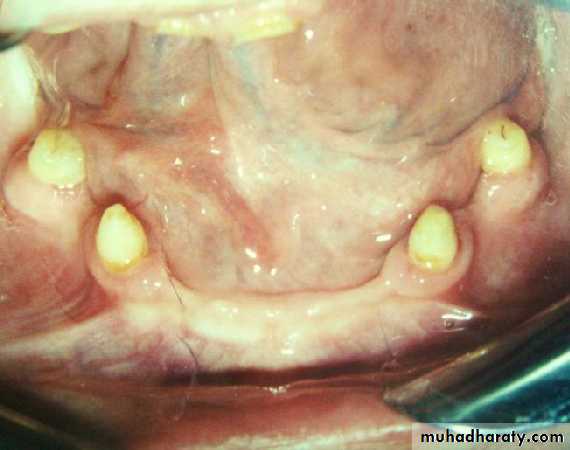
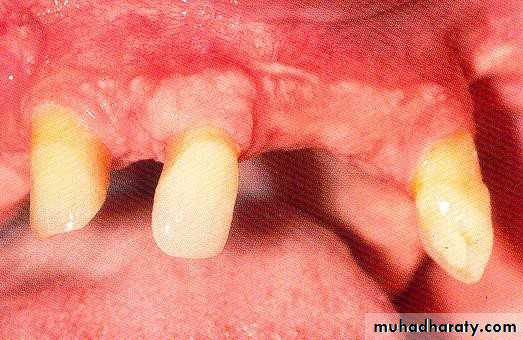
• 1- Simple tooth modification of vital abutment.
• A- Thimble-shaped
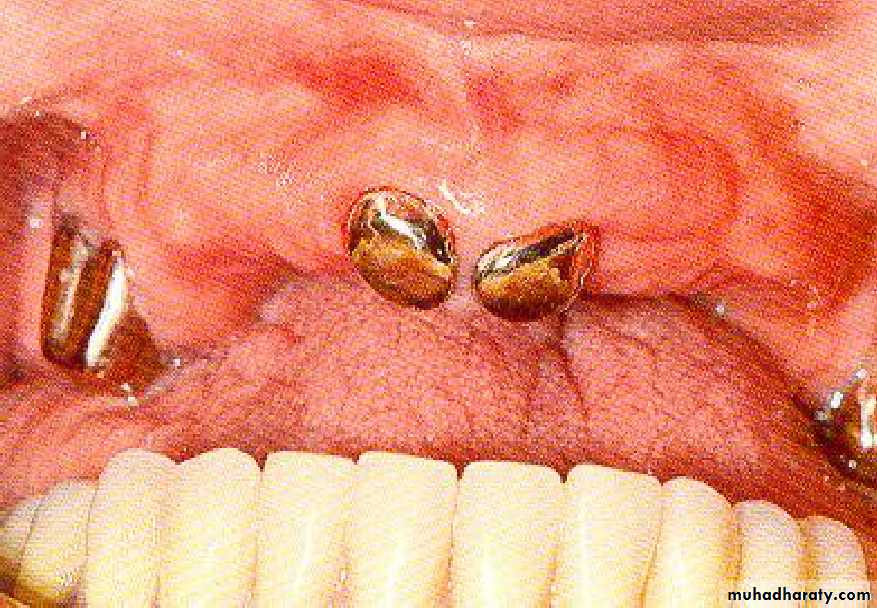
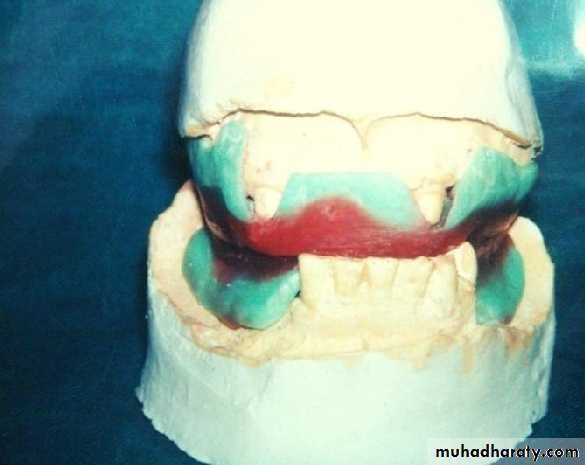
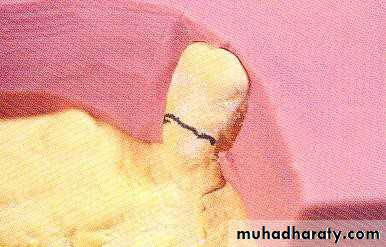
• coping• 2- Tooth reduction and cast coping of vital abutment
• B- Tooth reduction• and cast coping
• 2- Tooth reduction and cast coping of vital abutment
• .Endodontic therapy and amalgam plug
• .Endodontic therapy with post and cast coping• 5- Endodontic therapy with cast
• coping and attachments• 6- Telescopic overdenture
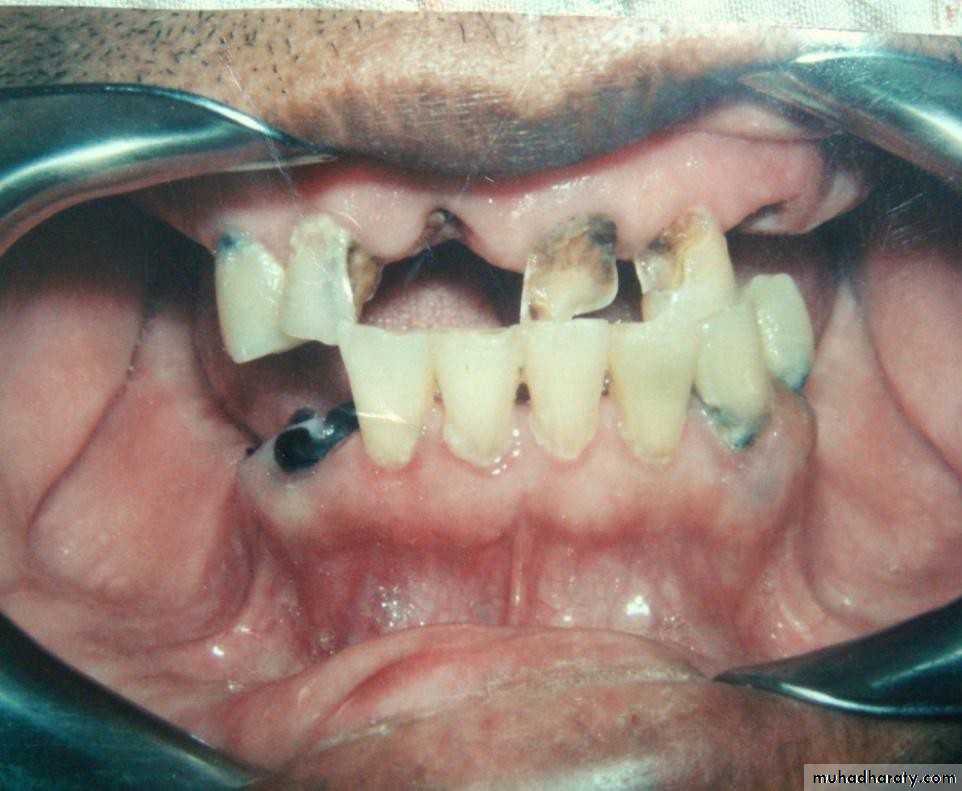
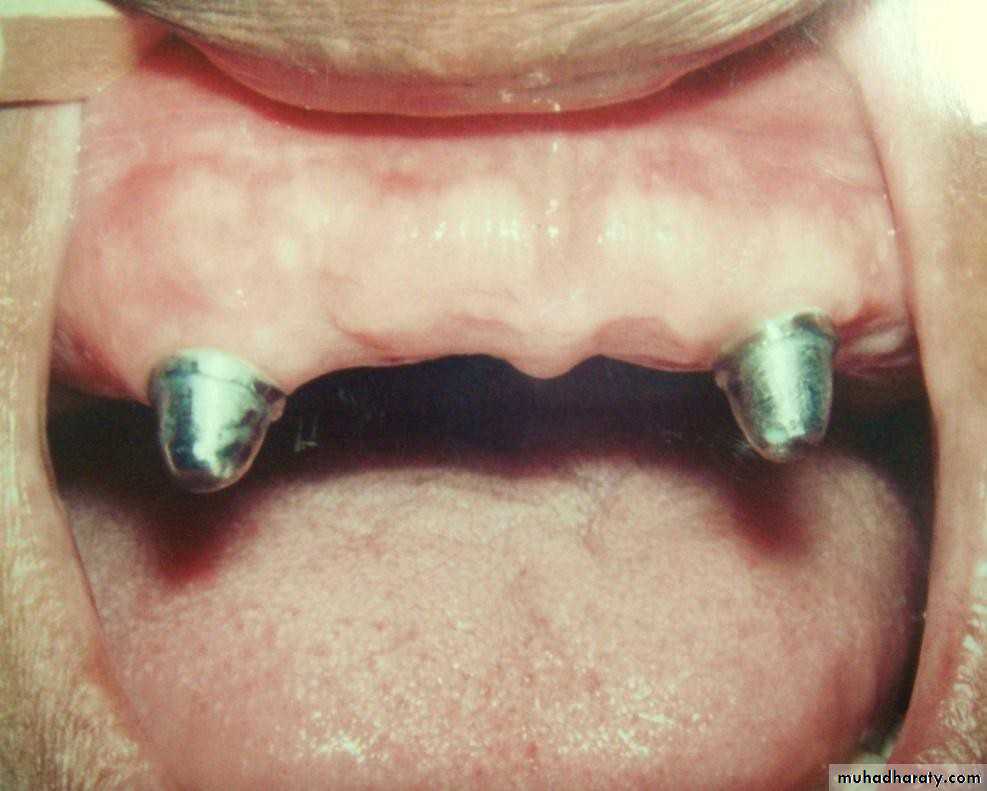
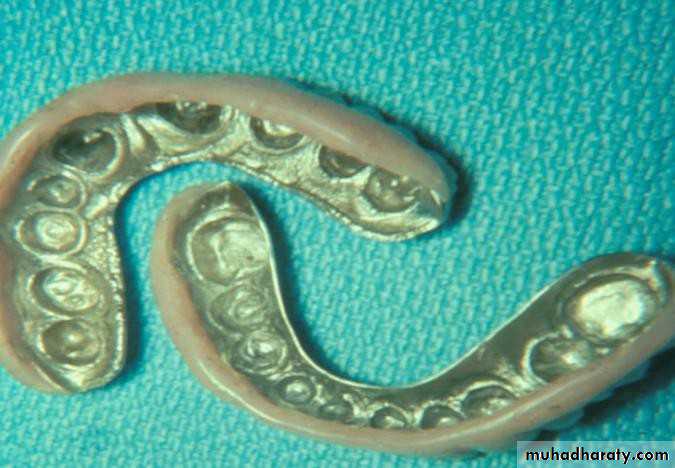
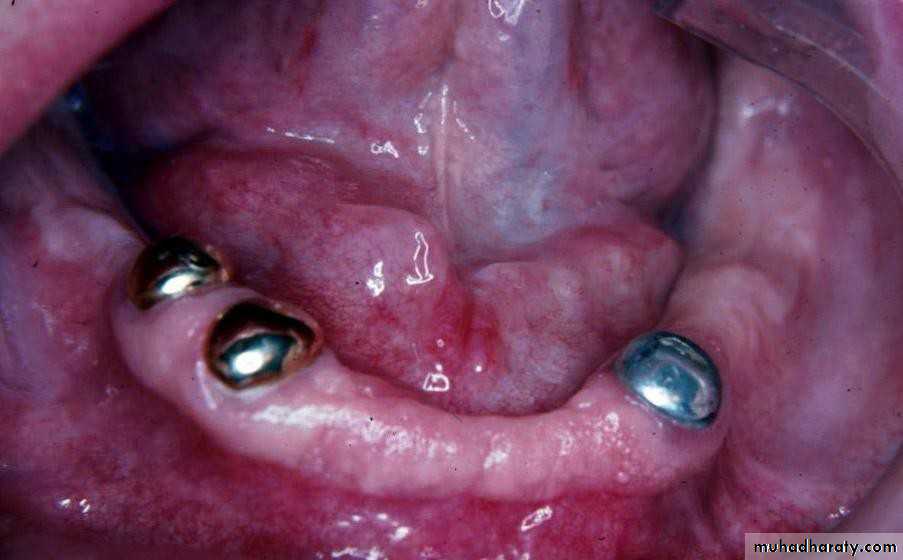
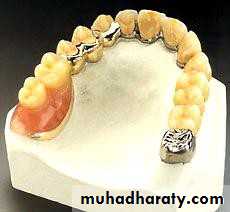
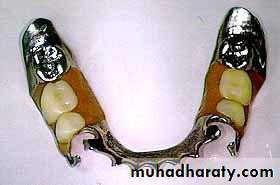
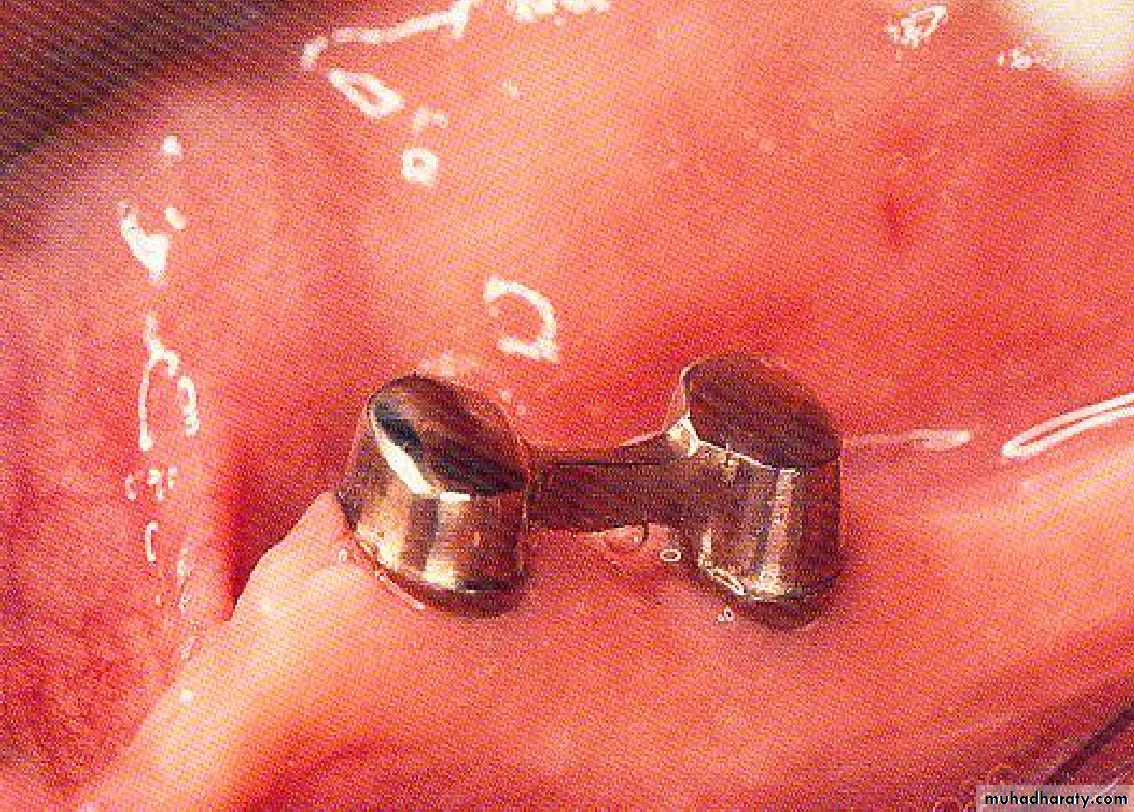
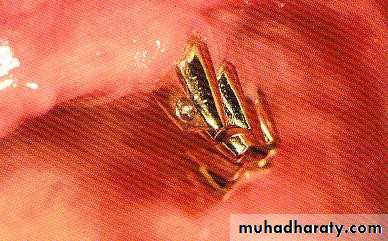
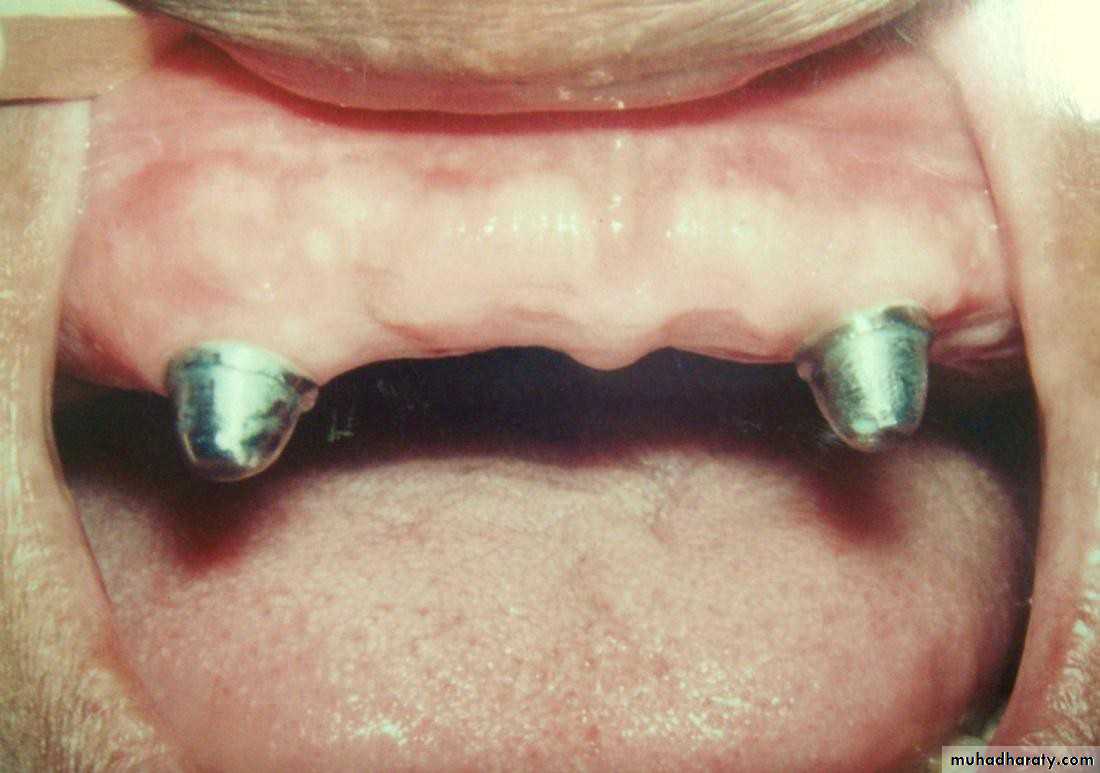
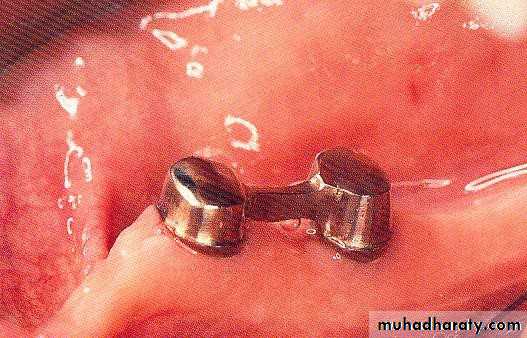
• Gold or metallic cast Copings and telescopic crowns are a method of improving overdenture retention. These
• may be conical crowns (semi- parallel wall) with a friction adaptation at the marginal area of the abutment, or Milled crowns for larger areas and parallel surfaces.
• Friction retention is more commonly used in exclusively tooth-supported overdentures
that are not supported by soft
tissue.
Transitional
OverdenturesImmediate
Overdentures
• Definitive Overdentures
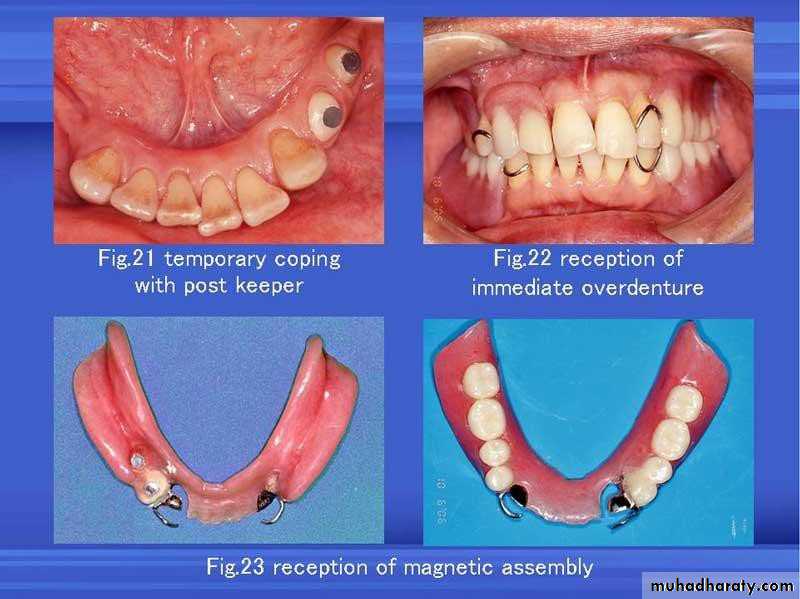
• 1) Immediate overdenture.
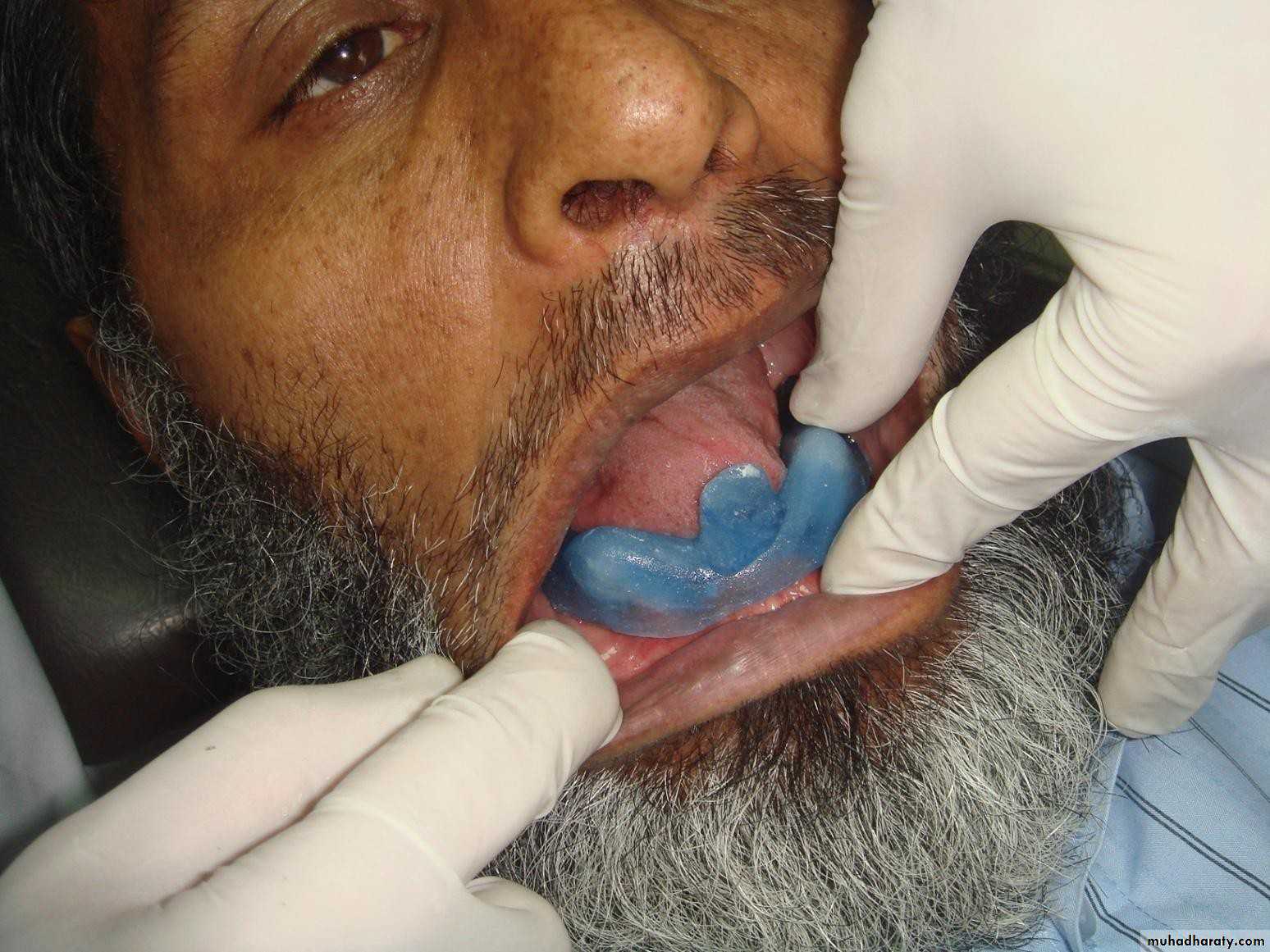
• Immediate Overdenture
• It’s constructed prior to the preparation of abutment teeth and inserted after the preparation.
• When the processed denture is fitted, it is relined with cold cured acrylic in the areas around the abutment teeth to make it fit as well as possible.
• 2) Transitional Overdentures
• Obtaining by Converting an already existing RPD to an O.D.
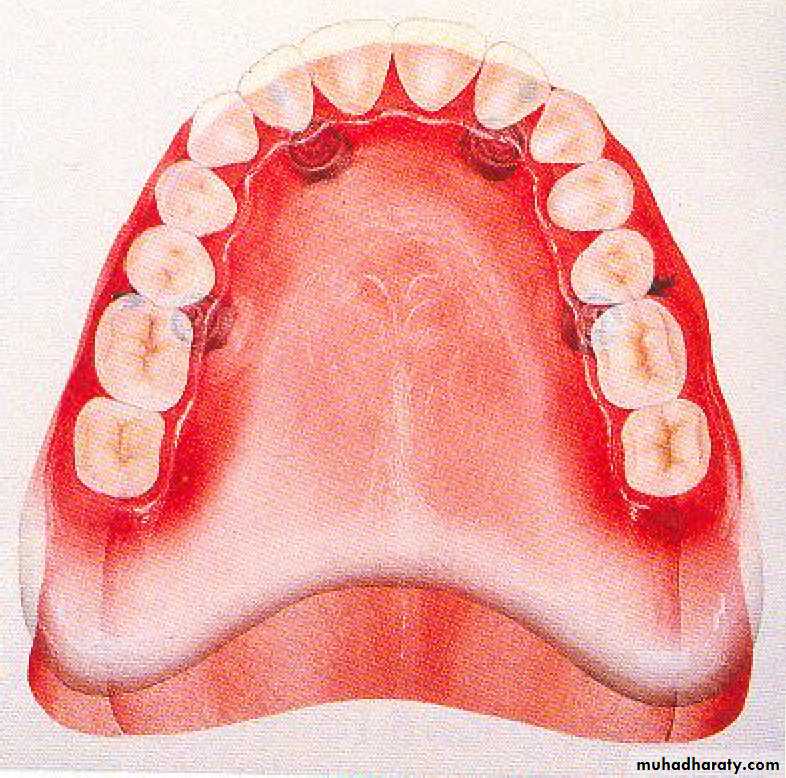
• 3) Definitive overdenture.• Complete overdenture
• Partial overdenture
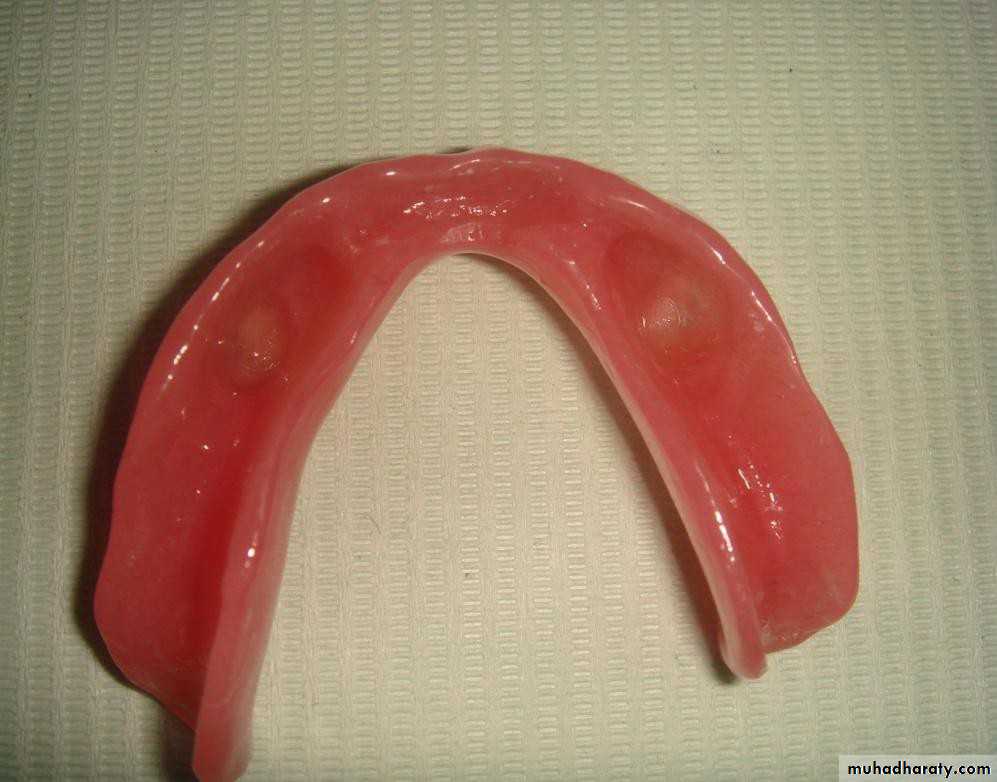
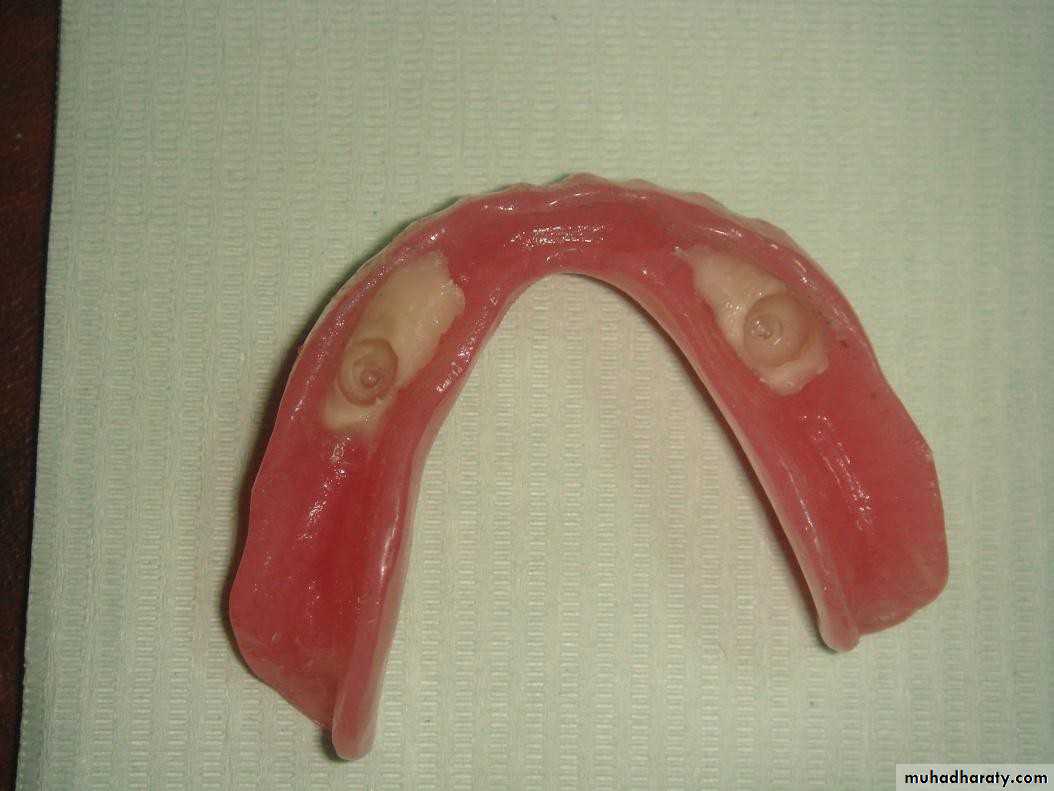
• Simple overdentures.
• Attachment retained overdentures.• 1) Simple overdenture.
• b) with copings.
• a) without copings.• Attachment retained overdenture.
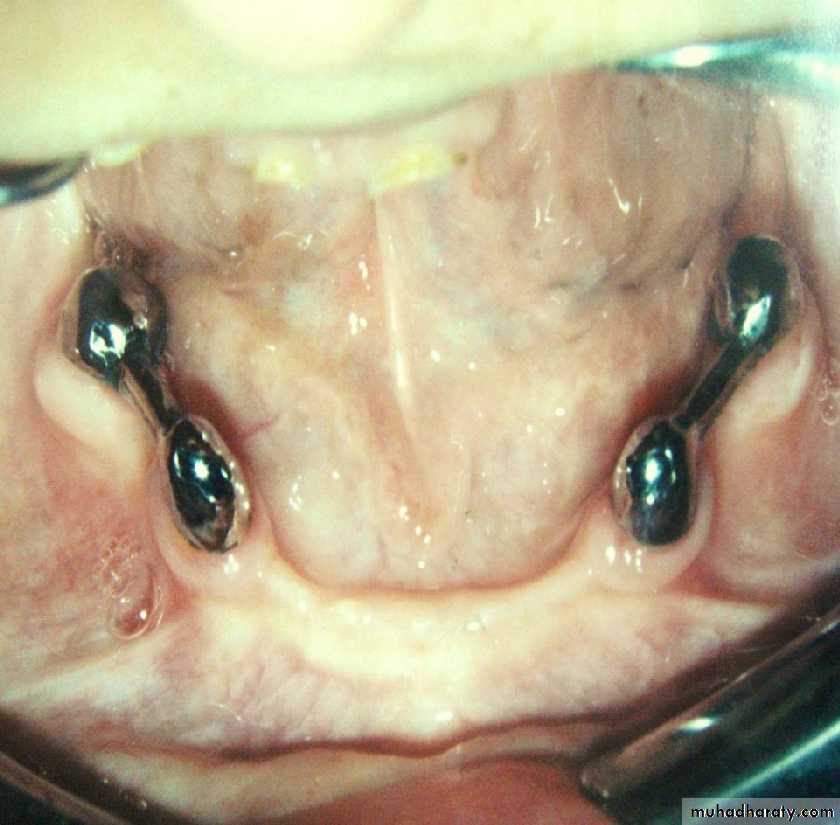
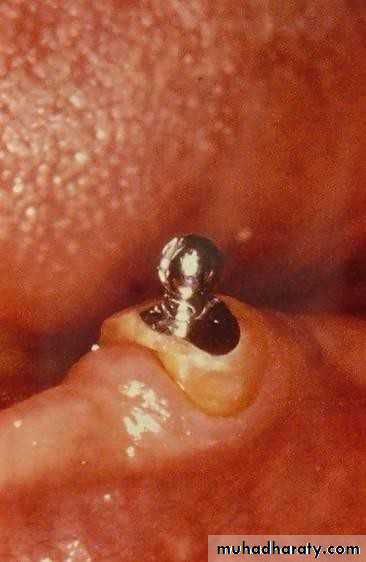
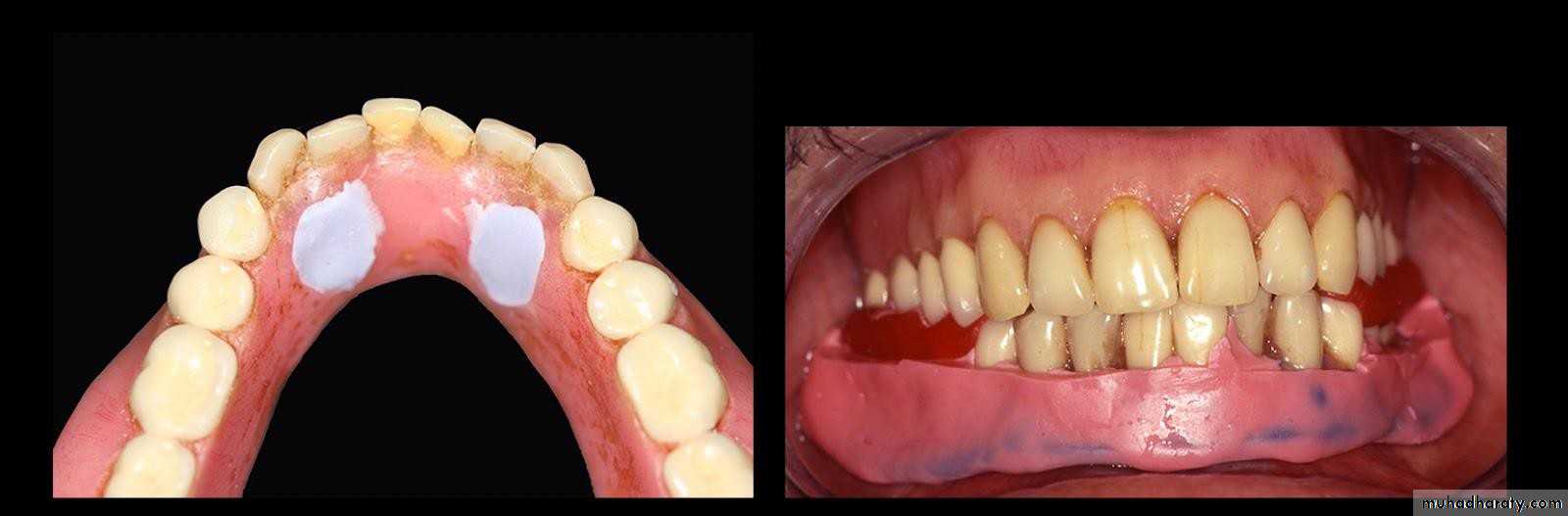
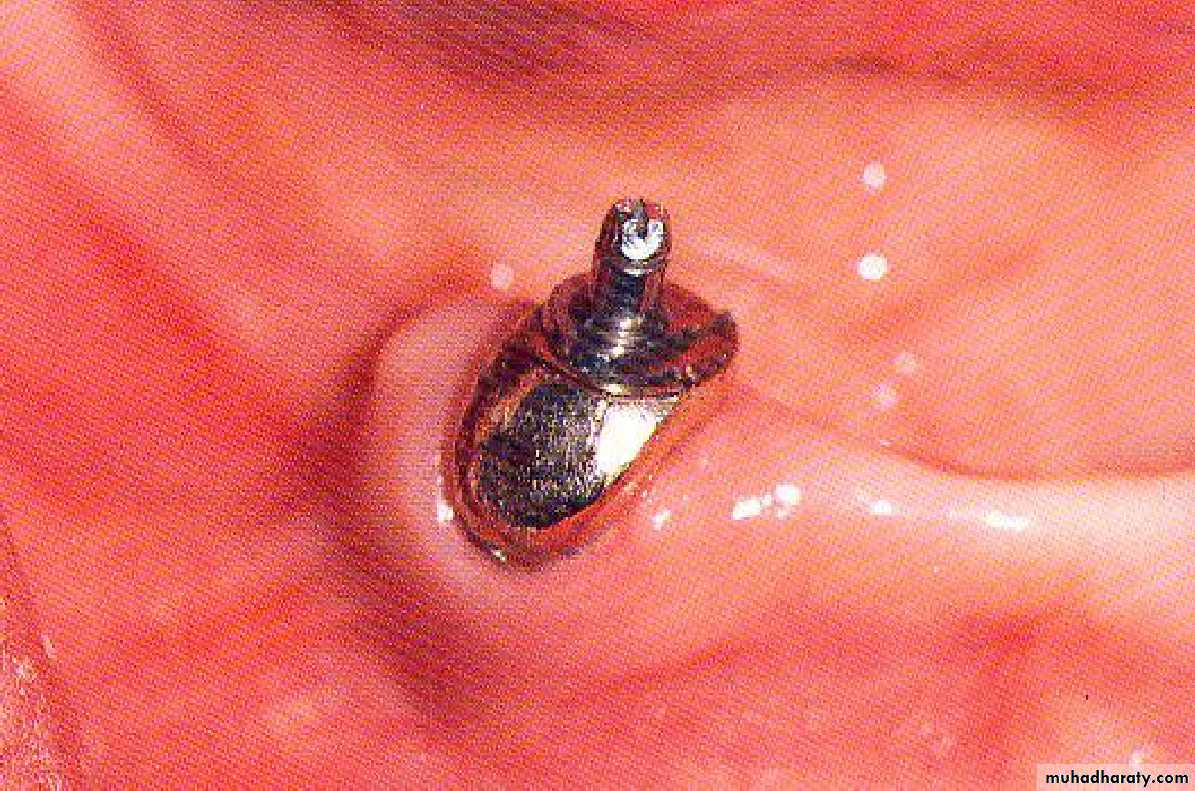
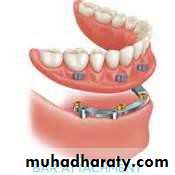
• a) stud attachment• b) bar attachment
• c) magnet attachment
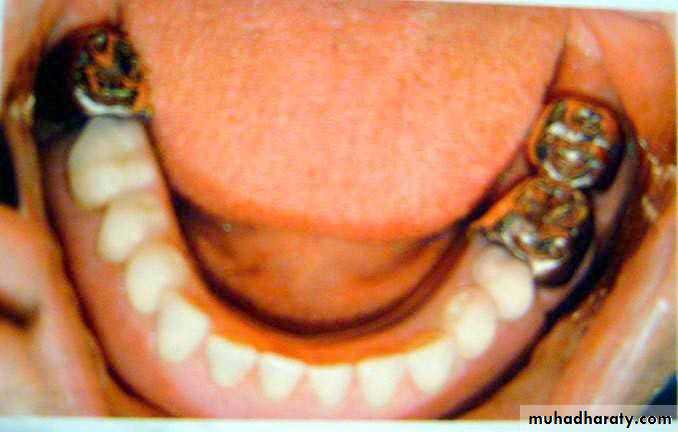
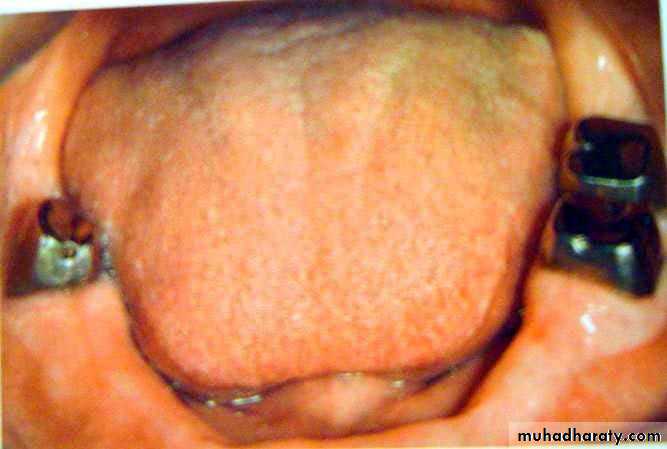
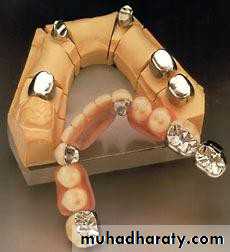
• d) telescopic attachment
• Attachment retained overdenture.
• a) stud attachments• Attachment retained overdenture.
• b) bar attachment• Attachment retained overdenture.
• c) magnet attachment• Attachment retained overdenture.
• d) telescopic attachment• 1) Medical history.
• 2) Dental history.• 3) Patient’s oral hygiene and anticipated cooperation and motivation.
• 4) Examination and proper abutment selection.
• 1) Bilateral distribution (avoid unilateral and diagonal).
2) Natural teeth orimplants as antagonists.
• 3) Endodontic treatment
• possible.• 4) min. 5mm periodontal
• attachment• min. 3mm attached gingiva.
• min. 2-3mm abutment height.
• no bony undercuts interfere
• with the insertion.
• 5) sufficient space between the abutment
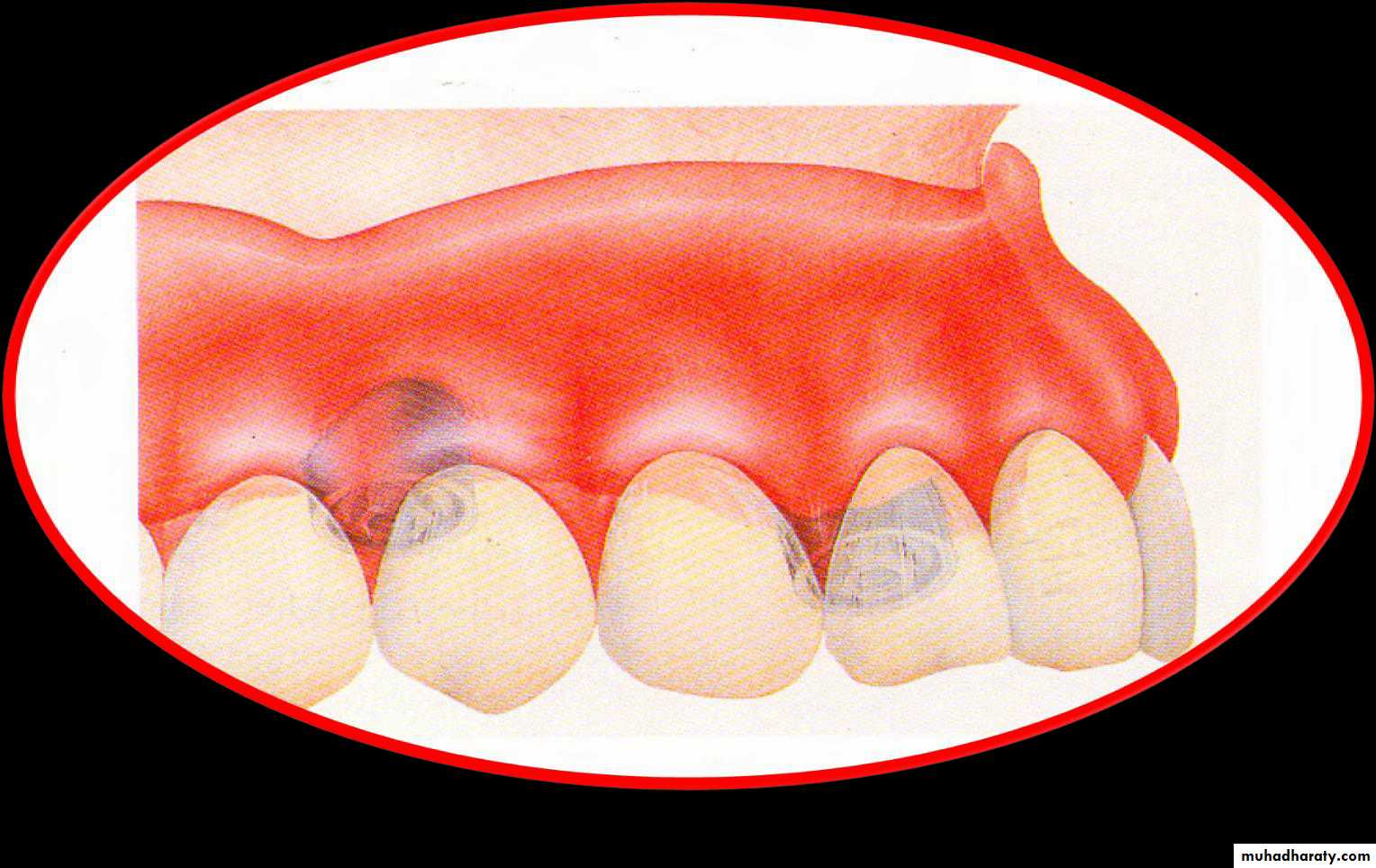
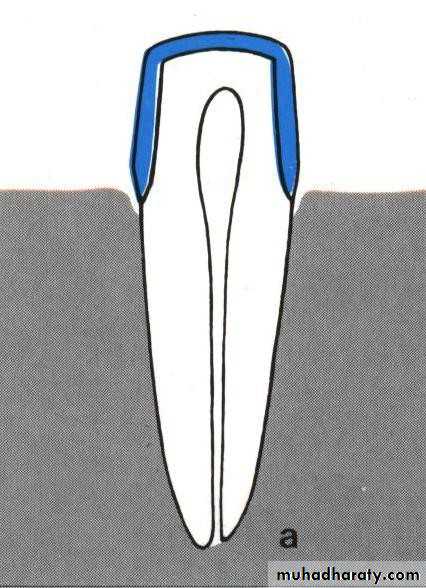
• and the opposing.• 1) Long (6-8mm):
•
•
•
•
• heavily tapered facially.
• less tapered lingually.
• gingival 1/3 approximately parallel.
• a heavy shoulder at the gingival margin , if a secondary metal coping will be placed.
• teeth are usually vital.
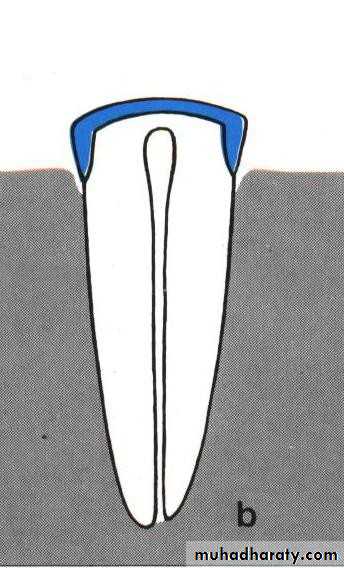
• 2) Medium (4-6mm):
• a) usually conical with greater taper on all surfaces.• b)usually used with a bar.
• c) tooth may or may not be vital.
• 3) Medium short (2-4mm):
• a) proximal walls should be parallel for max. frictional fit• b) adjacent abutments better to be splinted
• c) tooth is non vital
• d) used when a favourable C/R ratio
• is needed
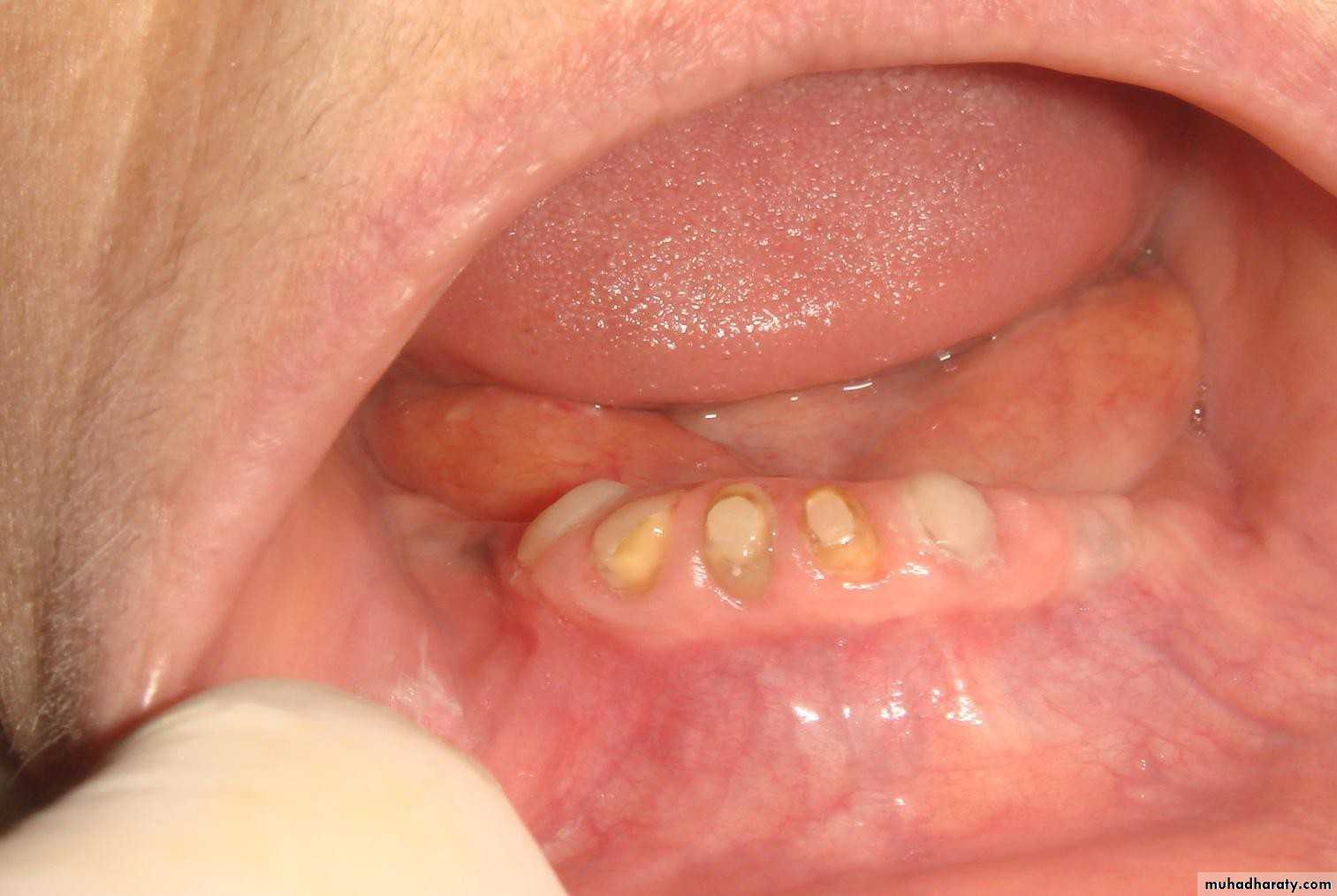
• 4) Short (1-2mm):
• a) conform to the curvature of the alveolar ridge (Dum-shape).• b) very low profile.
• c) indicated for max. favourable C/R
• ratio.
• d) can be used with the stud
• attachment.
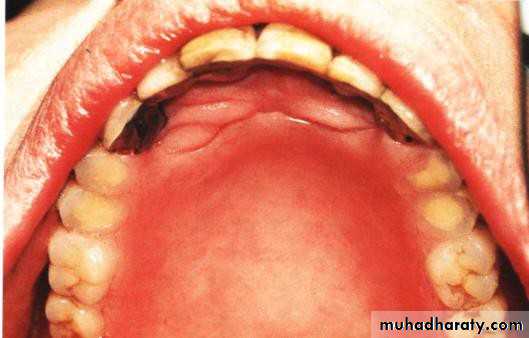
• May be with or without amalgam plug.
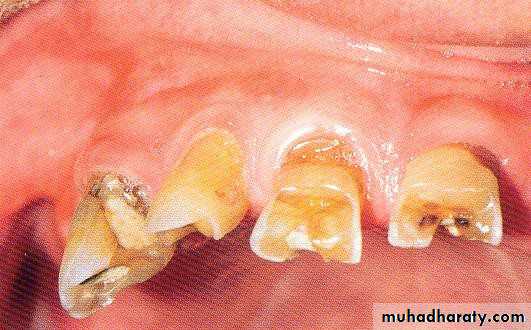
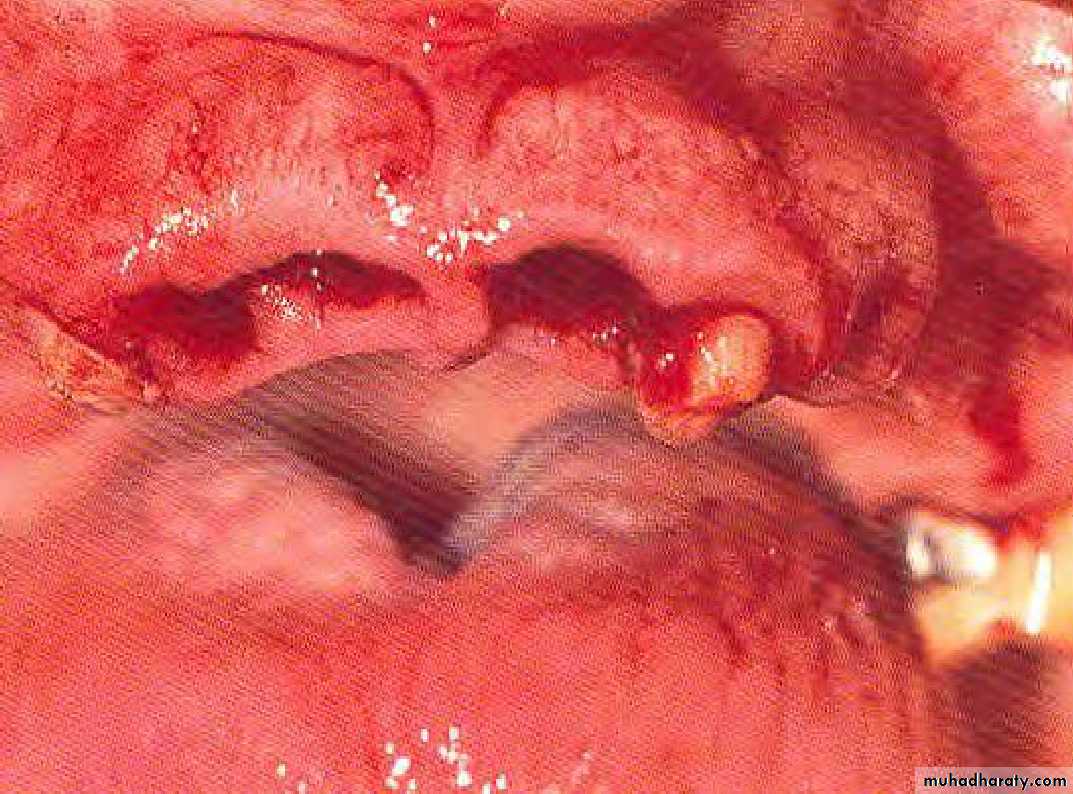
• 5) Submerged root:
• Abutment reduced to level below gingival margin, so need extra retentive attachment (intracoronally).• RCF .... if needed
• If planned…
• Centric & vertical relation registrations.
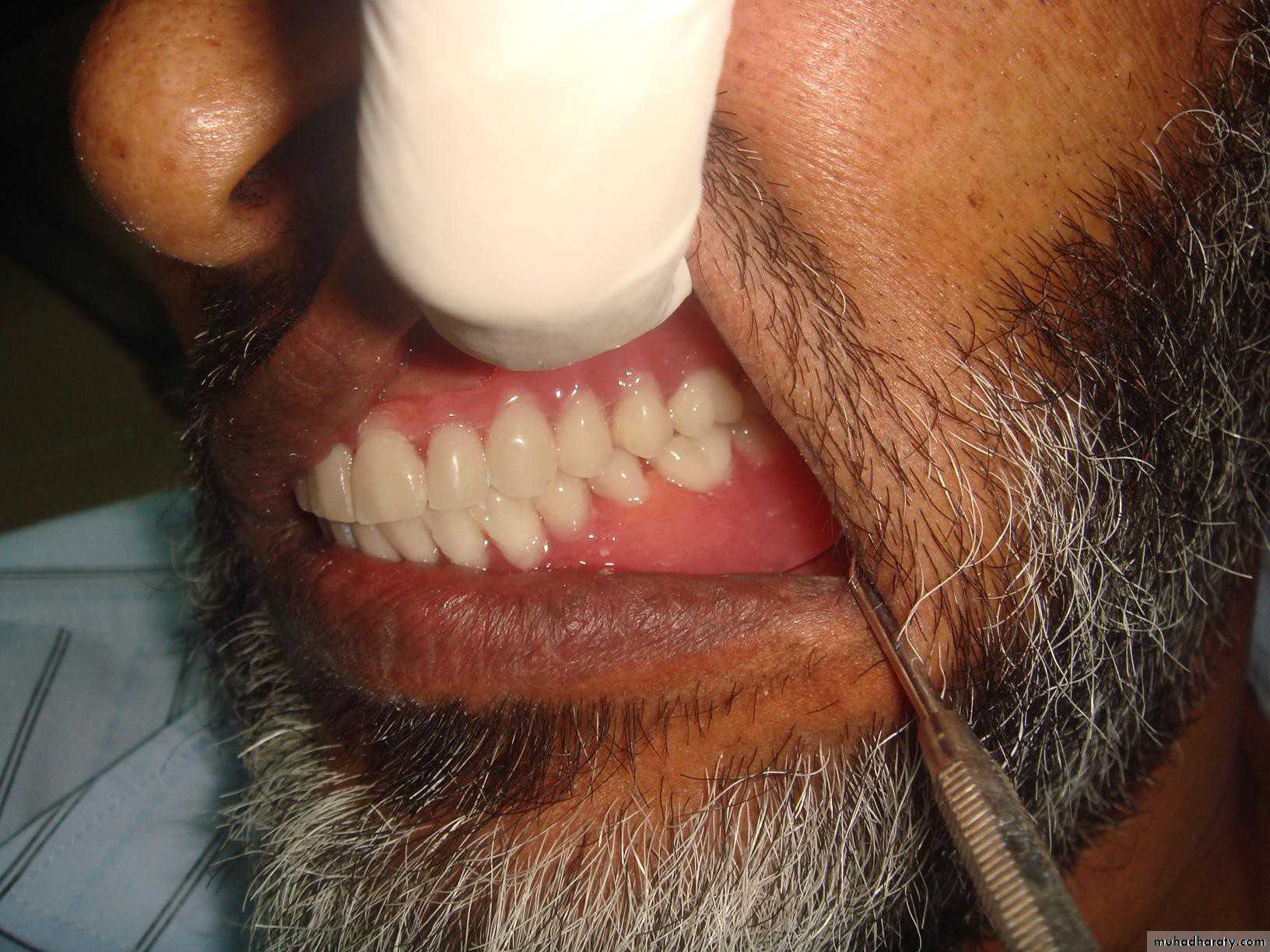
• Arrangements of the artificial teeth, according to aesthetic & functional (occlusal) considerations.• Try in the unfinished denture.
• Deliver the prosthesis, after patient constructed conversation.• Nearly same steps mentioned with the tooth supported OD, except the step of tooth reduction.
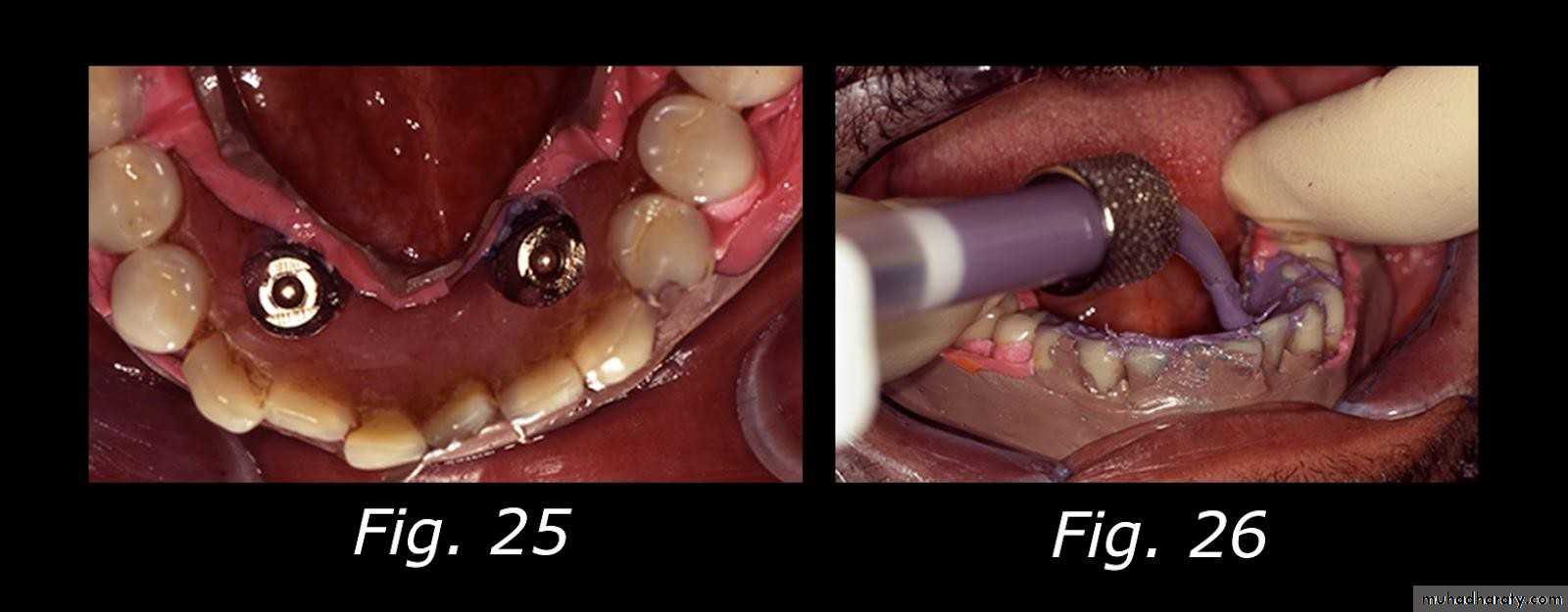
• If using an attachment with the implant, the direct pick up procedure for the female part within the denture base is favourable.
• Same as conventional overdenture, except:
• Choose the retaining clasp (simplest design): Light-guage wrought wire clasp is the best choice to allow easy release of direct retainer if occ. load to be applied on the distal extension base.• Continue as conv. RPD (mouth prep., imp. making, fitting of the framework).
• Altered cast impression tech. by rubber base if
• there is undercut in the POD abutment.