The Cardiovascular System
Composed of:transport medium (blood)
tubes (blood vessels)
pump (heart)
Role:
Provide nourishment to all body systems
Transport of waste products, hormones, etc.
There are important interactions between cardiovascular, pulmonary and renal systems
regulation:
autoregulation
extrinsic and intrinsic mechanisms of cardiac control
parameters of cardiac function:
blood pressure
cardiac output
The structure of the heart:
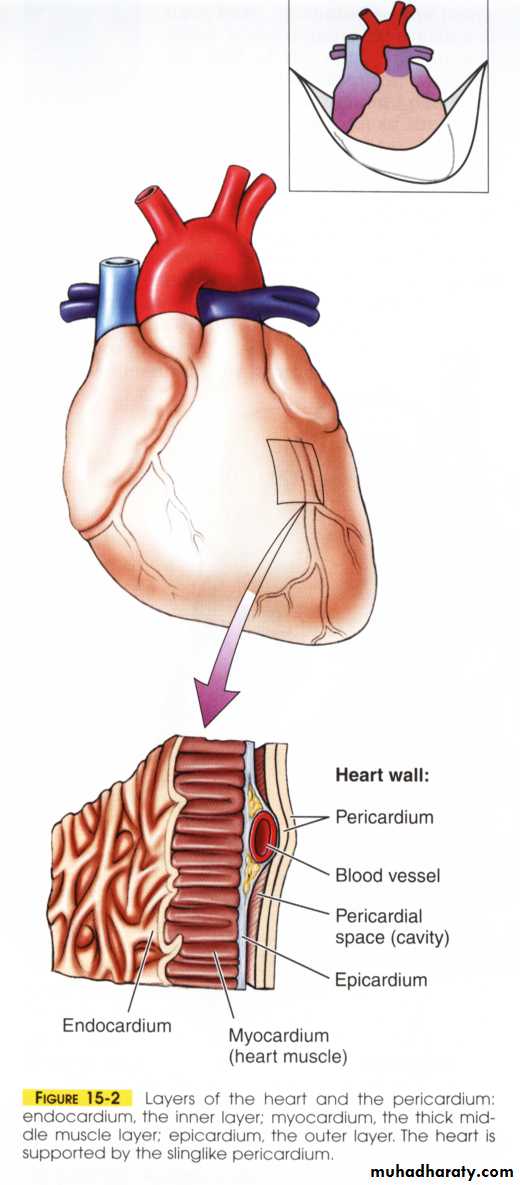
Heart consist of cardiac muscle covered by epicardium and lined by endocardium. The heart enclosed by pericardium, which contains fluid.Heart laying in the thorax resemble an inverted cone, the aspect of the heart where the vessels enter is called its base, the extremity of the ventricles is termed apex.
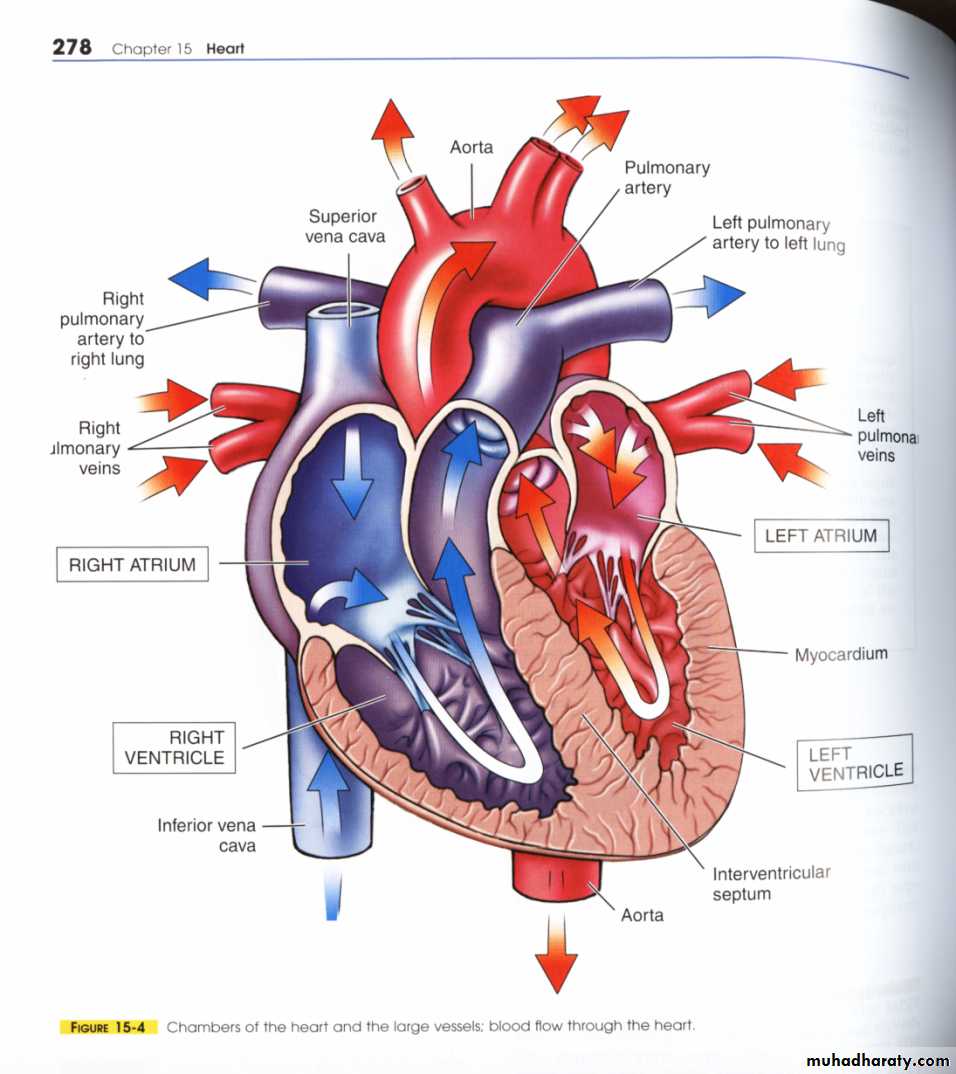
The heart divided into four chambers;
Right and left Atrium lie side by side in the upper part of heart.
Right and left Ventricle in the lower part of the heart.
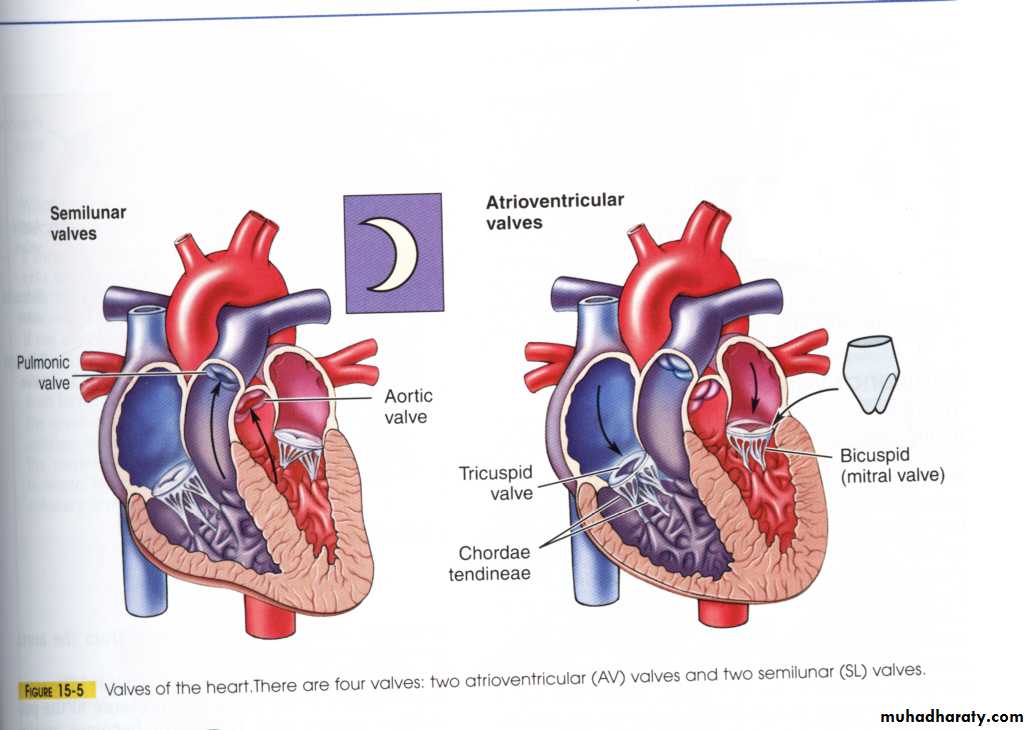
The left atria (L.A.) separated from the left ventricle (L.V.) by the mitral valve (M).
The Right Atria (R.A.) separated from the Right ventricle (R.V.) by the tricuspid valve (T).
Between L.V. and Aorta there is a valve called Aortic valve (A).
Between the R.V. and pulmonary artery there is pulmonary valve .
Chordae tendineae; The cusps are attached to the ventricular wall papillae by tough fibrous band tissue, when they stretched they prevent the cusps from blowing through into the atria.
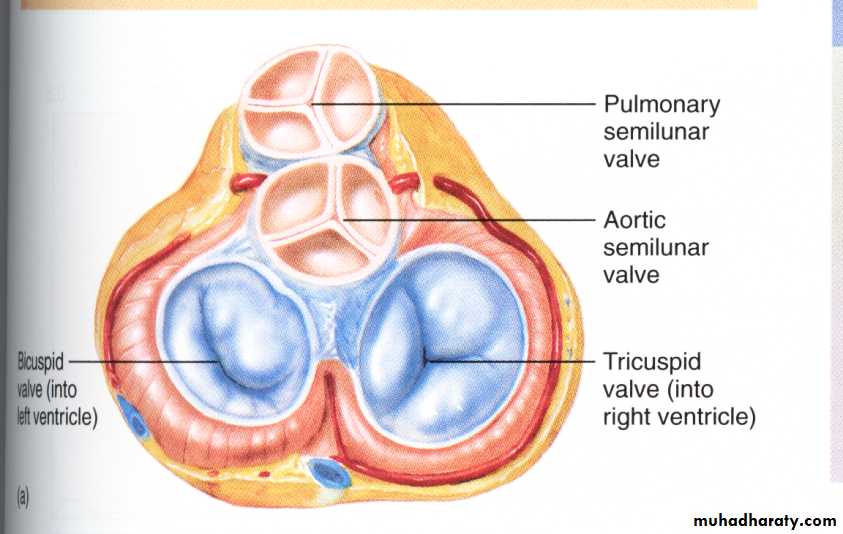
All the valves (4 valves) located in the same plane in the fibrous septum or ring which separate the Atria from ventricles.
Coronary artery
The heart supplied by blood from the coronary arteries which originated from the Aorta.
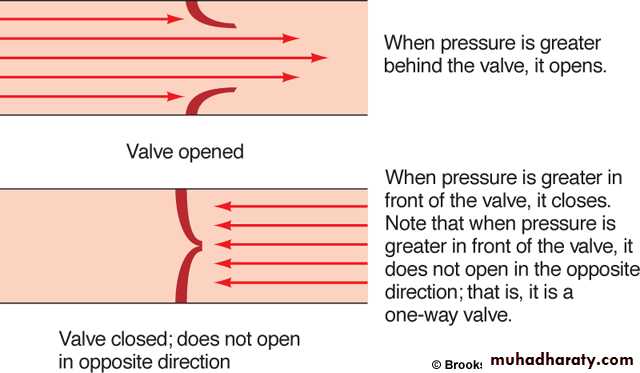
Valves ensures blood flows in one direction
Blood flows down a pressure gradient: Pressure gradient driving blood is determined by the difference in pressure between the left ventricle and the right atrium.
The heart as a pump:
The heart is basically a dual pump that provides the driving pressure for blood flow through out the pulmonary & the systemic circulation.
The blood which reach the R.A. via Superior Vena Cava (S.V.C) is dark blood because it contain CO2.
Blood passes from R.A. to the R.V. through the tricuspid value (T).
Then it pumped by the R.V. through the pulmonary valve (P.V.) into the pulmonary artery (P.A.) which carry it to the lungs where gas exchange occur and the blood became bright red in color due to oxygen .
Blood transported to the L.A. through the four pulmonary veins, ( this is the pulmonary circulation ) .
Then it pumped to the L.V. through the mitral valve.
The L.V. pumps the blood out through the aortic valve (A) into the Aorta which carry blood to the body (This is the systemic circulation).
Each time the heart beats, each ventricle pumps out a bout 70 ml of blood this is termed Stroke Volume.
The heart beats about 70 times a minute this is termed the Heart Rate (Is the number of times the heart beat each minute, it reflect the rhythmic firing of the Sino Atrial node ''S-A node'', It commonly measured as pulse).
Cardiac Muscle:
The heart beat because it is made of cardiac muscle which can contract with out extrinsic stimulation from a motor nerve (the impulse arises from& within cardiac tissue).
Each cardiac muscle cell has the property of;
Rhythmicity; That is it alternately contract and relaxes or beats. The cardiac tissue fires a cardiac impulse regularly.
Conduction; Each cardiac muscle fiber branches and comes in very close contact with several other cardiac muscles.
A contraction-wave starting in one part of the heart spreads rapidly to all other cardiac muscle.
SPECIALIZATIONS OF CONTRACTILE CARDIAC MYOCYTES:
Properties of contractile cells:
-small unicellular fibers
-myofibrils arranged into sarcomeres similar to skeletal muscle.
-cells joined end to end by intercalated disks
-extensive T-tubule system
-abundance of mitochondria
-almost only dependent on ATP generated by oxidative metabolism
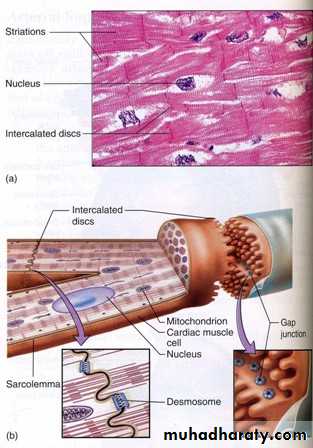
INTERCALATED DISK
-complex consisting of desmosome and gap junctionDesmosomes within the intercalated provide mechanical stability
Gap junctions within the intercalated disk allows rapid conduction of AP
This ensures synchronous depolarization of all contractile cells to produce contraction
INTRINSIC CONDUCTION SYSTEM:
Cardiac conduction system:Provides the stimulus for muscle contraction.
Coordinates the pumping activity of the atria& ventricles.
Pacemaker cells:
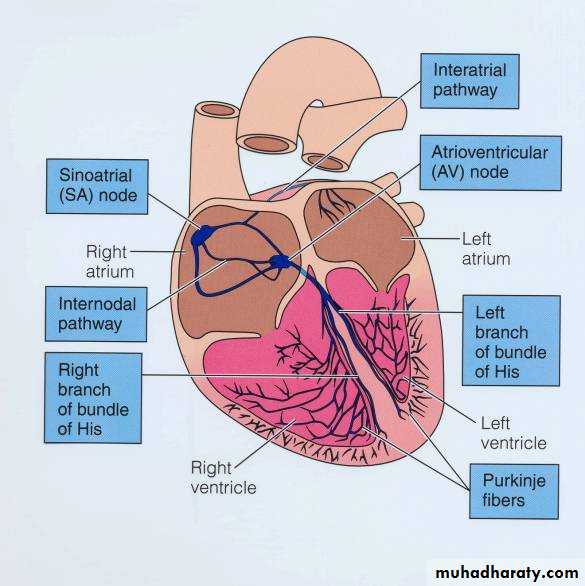
Pacemakers concentrated on specific locations:
-SA node- in the right atrium near the opening of the vena cava.
-AV node- located at base of right atrium near the AV septum
-Bundle of His- originates at the AV node and enters interventricular septum where it divides to form right and left bundle branches that travel to apex and curve upward
-Purkinje fibers- small terminal fibers that extend from the bundle of His and spread
throughout to all ventricular myocytes
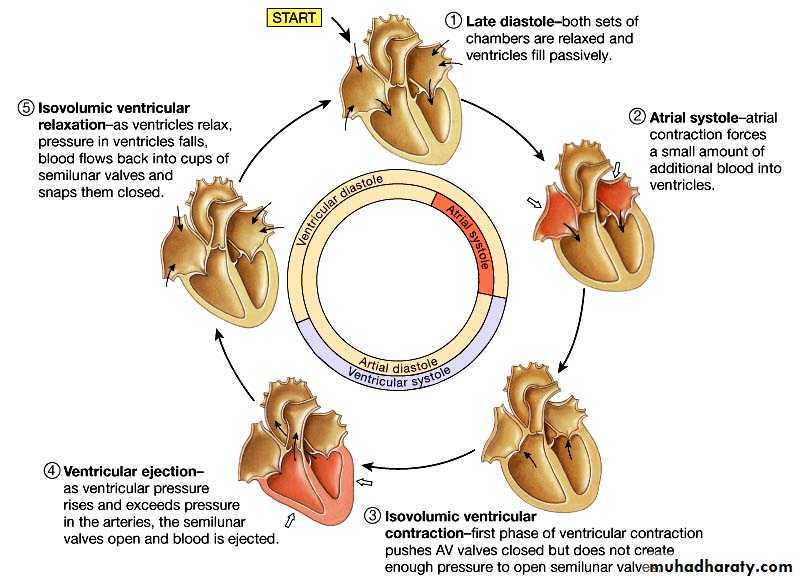
The Cardiac Cycle:
-period of time between two successive heart beats.-two alternating phases:
-systole- period during which heart is contracting and emptying lasts for 0.3 second.
-Pressure developed by the heart exceeds pressure in the aorta and PA
- blood flows into the aorta and pulmonary artery following ventricular contraction.
-diastole- period during which the heart is relaxing and filling it lasts 0.5 second.
-Pressure in heart is lower than in the vasculature.
- blood returns to the heart.
-diastole is longer than systole (2/3 of cardiac cycle).
The complete sequence of events (the cardiac cycle) lasts for 0.8 seconds.
(So that cycle /min = heart rate).
When heart rate speeds up as in exercise and emotional excitement, the whole cardiac cycle completed in a shorter time, this reduction in duration is mainly in diastole
-Changes in HR are primarily manifested by changes in diastolic interval.
- HR decreases diastolic interval
- HR increases diastolic interval
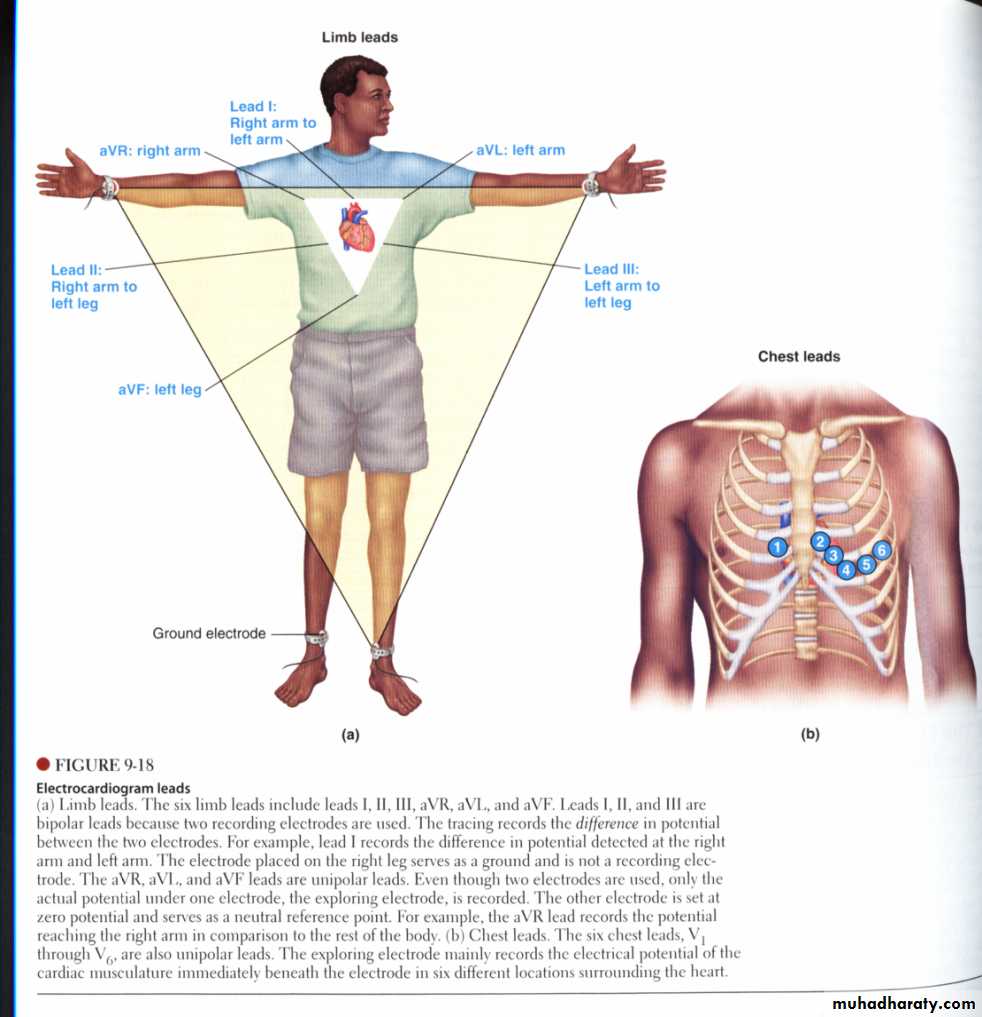
Electro Cardio Gram (ECG):
The spread of the heart beat from the S-A node to atria to atrioventricular bundle and finally to the ventricles, is associated with an electrical voltage change which can be recorded at distances remote from the heart, this electrical record is termed Electro Cardiogram (ECG) .
Electro Cardiograph: Is an apparatus used to amplify the voltage electronically in ECG recording
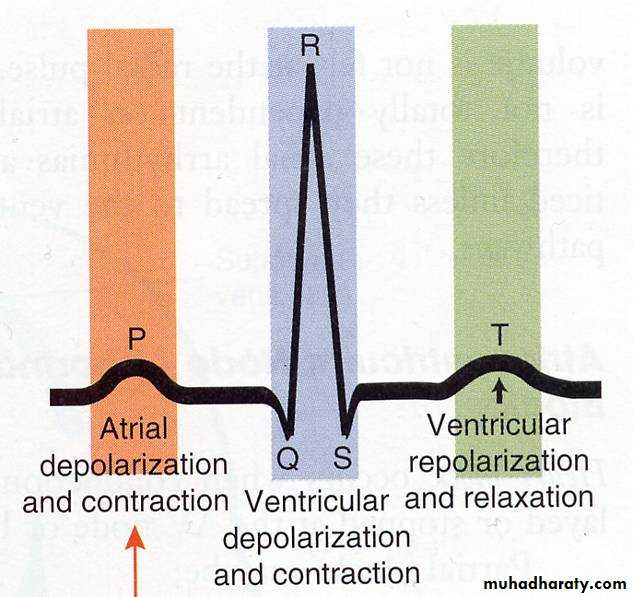
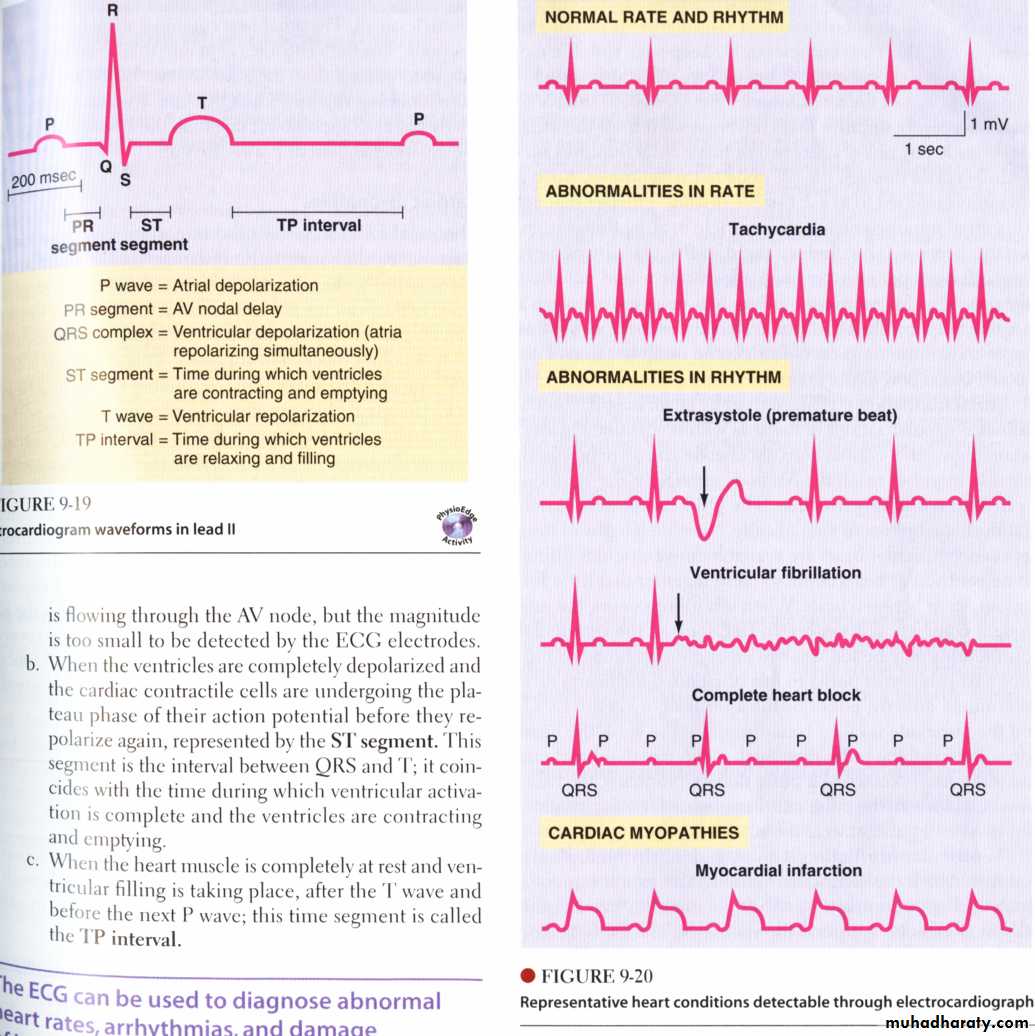
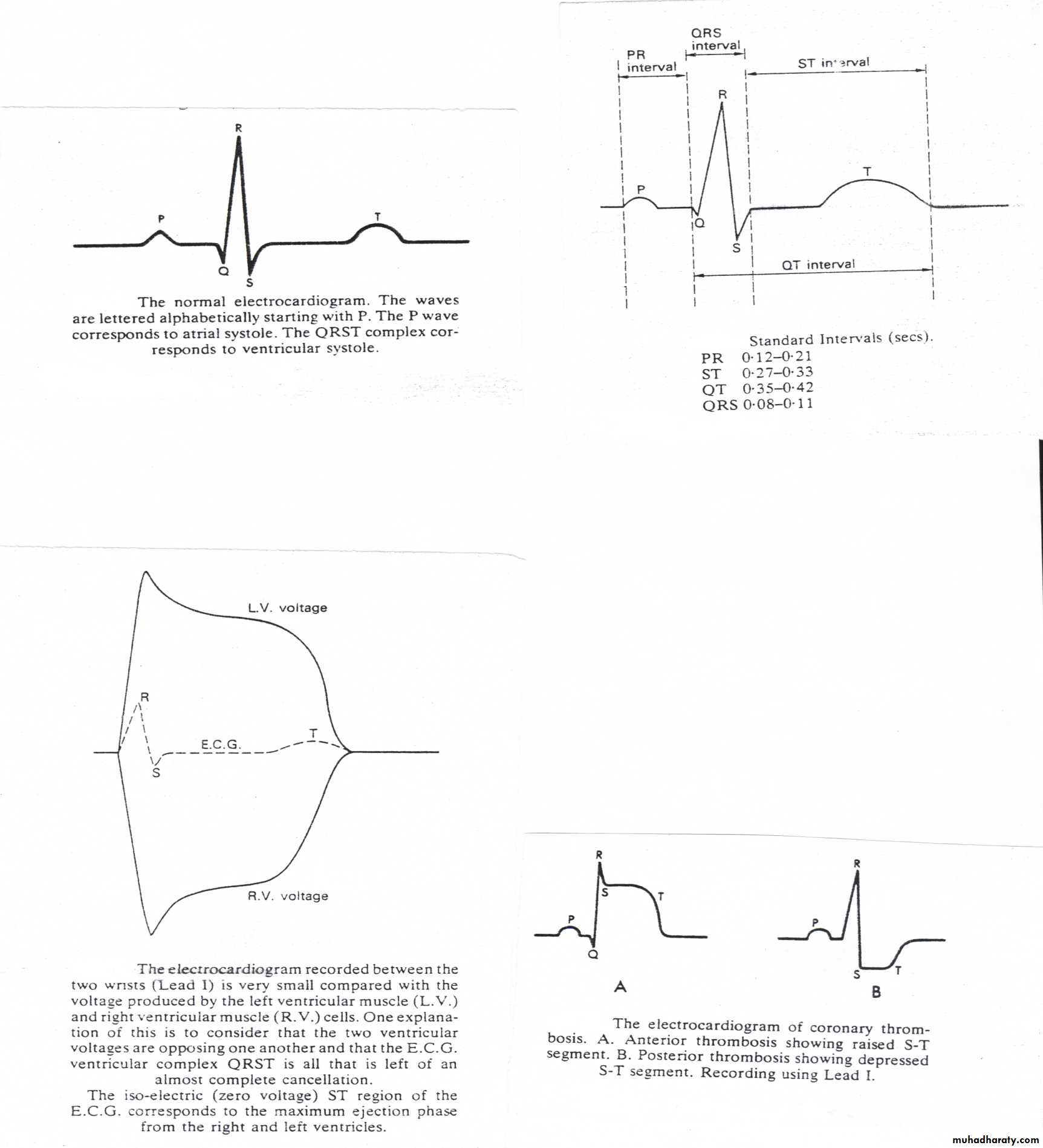
* The recording shows fluctuations throughout the cardiac cycle which are known as waves and complexes (series of waves) .
* The P wave corresponds to atrial systole it’s followed by QRST complex which corresponds to ventricular systole.
* The duration of waves and complexes of electrocardiogram varies from beat to beat and from person to person.
* The QRS complex is the result of the heart beat arriving at different parts of the ventricles at slightly different times.
* The Q wave is not always present as some parts of the heart relaxing slightly before other parts.
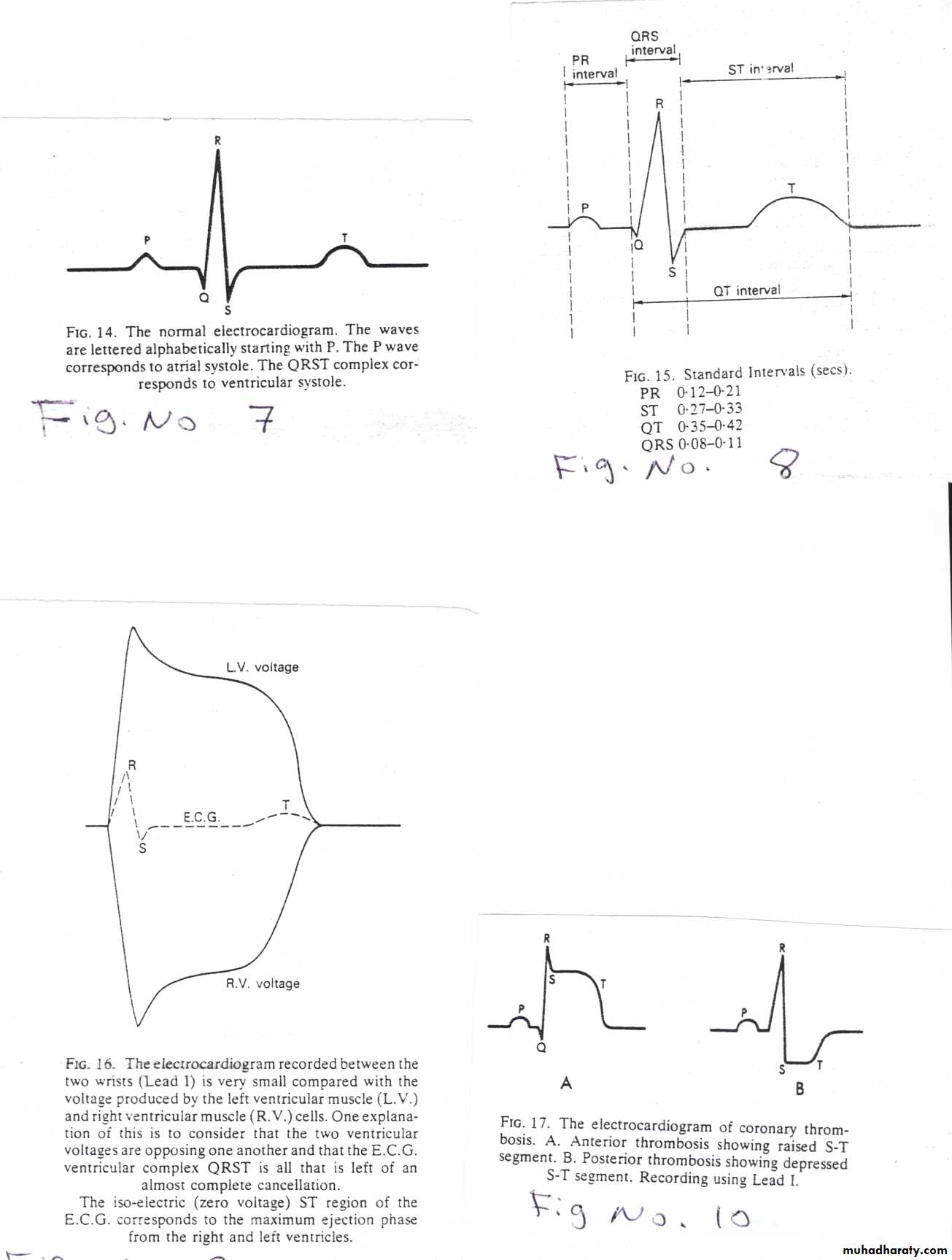
* The QRST complex recorded during ventricular systole is very small compared with the voltage which is actually produced by each cardiac muscle cell through out the whole ventricular systole; this is because the voltage produced by the L.V. tends to cancel out the voltage produced by R.V. under normal circumstances.
* If one ventricle does not produce it’s full voltage then the cancellation will not be so complete (this will occur if the ventricle has an insufficient blood supply from the coronary arteries, Ischemic heart disease, myocardial infarction, coronary thrombosis)
* The failure of cancellation is seen most clearly in the part of electrocardiograph tracing between S wave and the T wave, which is known as ST segment, which is normally isoelectric region ( no voltage is recorded ).
* Following coronary thrombosis this region will raised or depressed.
* Anterior thrombosis cause raised segment (A).
* Posterior thrombosis cause depressedsegment (B)
Heart Block :
If there is damage in Atrioventriculer bundle then the heart beat which originate in S-A node will spread to the atria and to the A-V node but will not spread to the ventricles.Heart sound:
1-The first heart sound; it is like the word “lubb” spoken very softly. This sound marks the on set of the ventricular systole.
It occurs due to the closure of the mitral and tricuspid values.
It can be heard by placing a stethoscope to the chest.
2-The second heart sound which is like the word “dupp” spoken softly, this marks the end of ventricular systole and the start of ventricular diastole.
It occurs due to the closure of the aortic and pulmonary valves.
The beating of the heart has a characteristic rhythm; lubb-dupp-pause- lubb-dupp-pause
3-A third heart sound can some times be distinguished –occur during ventricular filling it, more audible in heart failure than in healthy person.
4-The third sound may also accompanied by fourth sound preceding the first sound. (Third& fourth sounds are abnormal sounds).
Heart Murmurs:-
The flow of the blood through the heart is normally silent, but should be a valve fail to open completely it will acts as partial obstruction.
The blood will speed up and reach a high velocity as it pass through the narrow opening, this will lead to turbulence and to sound and vibrations in the chest. These sounds are termed Heart murmurs.
Examples for murmurs:-
Heart Thrills: - If the vibration have low frequency they may not audible but can be felt if the hand is applied to the chest wall.
Stenosis: - When the valve is narrow so that it doesn’t open completely leading to stenosis.
Incompetence or Regurgitation: - Failure of a valve to close completely thus leaving a small aperture through which the blood flows very rapidly in reverse direction to normal.
Control of the heart:
1. Heart function can be regulated with regards to:a. chronotropy (rate of contraction)
b. inotropy (force of contraction)
positive (increased) or negative (decreased) modulation
2. Changes in systemic blood pressure elicit reflex control of heart function
a. baroreceptors (pressure sensors) present in carotid body, aortic arch
b. cardiac control centre present in medulla
3. Presence of specific receptors in the heart are targets for neurotransmitters, hormones, and drugs:
a. muscarinic (negative chronotropy)
b. -adrenoceptors (positive chronotropy and inotropy)
4. Four essential mechanisms controlling heart function:
neural
humoral
drugs
intrinsic
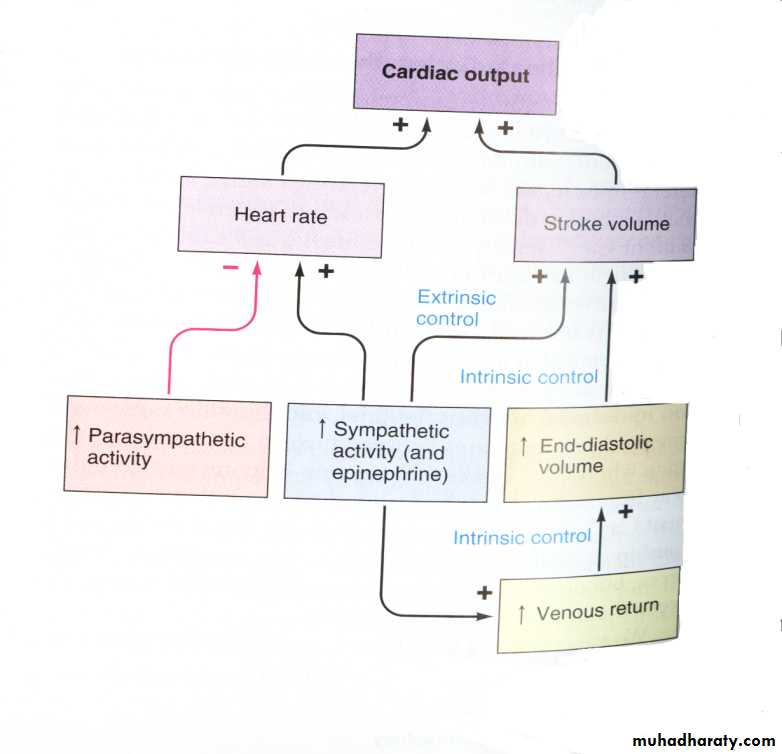
The four essential mechanisms controlling heart function, mechanisms:
neural (via neurotransmitters)
sympathetic nervous system (SNS): positive chronotropy , positive inotropy
parasympathetic nervous system (PNS): negative chronotropy
humoral (via hormones)
catecholamines (e.g. epinephrine): positive chronotropy, positive inotropy
drugs
many drugs act on the heart resulting in modulation of cardiac function (e.g. digoxin, -blockers, calcium channel blockers)
COMPARISON OF SYMPATHETIC AND PARASYMPATHETIC EFFECTS ON THE HEART
Sympathetic nervous system
Parasympathetic nervous system
-predominates in exercise and stress
-predominates at rest
-norepinephrine, epinephrine
-acetylcholine
-adrenergic receptors
muscarinic receptors
-cAMP,
-cGMP
-increases intracellular calcium
decreases intracellular calcium
-decreases potassium conductance
-increases potassium conductance
-positive inotropic
(increases contractility)
-negative inotropic (mild)
(decreases contractility)
-positive chronotropic
(increases heart rate)
-negative inotropic
(decreases heart rate)
Ions and the Heart :
In addition to sodium ions, the beating of the heart required the correct level of potassium perfusing the coronary arteries.
Without K+ and Ca2+ the heart ceases to beat.
Increase or excess Ca2+ stops the heart in systole while excess K+ stops the heart in diastole. So care must be taken with an intra venous infusion containing K+ or Ca2+ to ensure that an excess of these ions is not given.
[Some of calcium is released from internal stores ( sarcoplasmic reticulum ) an important fraction of the calcium enters from out side ] .
Arterial pulse:
The blood forces into the aorta during systole not only moves the blood in the vessels forward but also setup a pressure wave that travels along the arteries.
The pressure wave expands the arterial walls as it travel and the expansion is palpable as pulse at a speed of about six meter/second and take about 1/10 of second to reach the wrist.
The strength of the pulse is determined by the pulse pressure and bears little relation to the mean pressure (pulse is weak in shock and strong in case of exercise).
When we take pulse we determine the heart rate, then number of complete cardiac cycle/min.
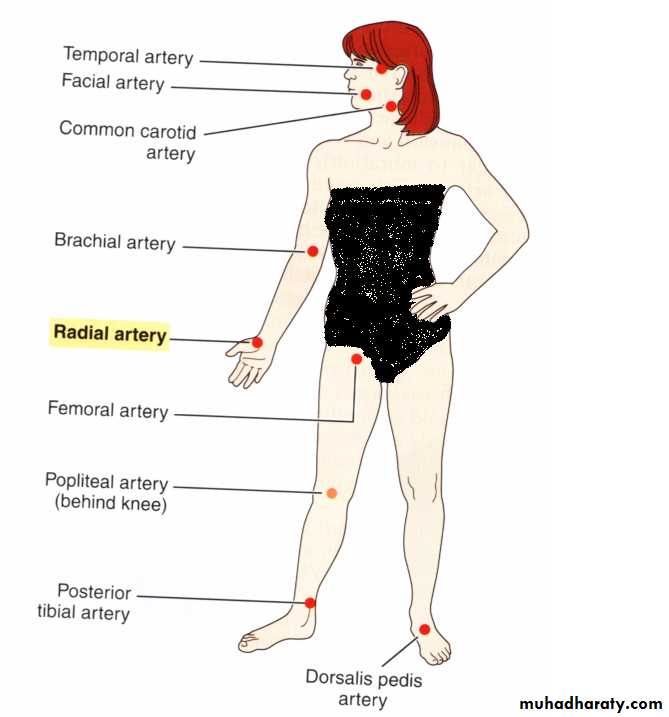
Pulse can be determined from radial, posterior tibial, femoral and carotid arteries& other locations.
The fluctuation of blood pressure 120/80 mm Hg gives rise to the pulse, if systolic and diastolic pressure will be equal blood flow will decreased but pulse can’t detected .
Pulse pressure: The difference between systolic & diastolic pressure 120/80 mmHg.
Cardiac out put:
Cardiac out put is the amount of blood pressured by each ventricle per minute, it depend on the products of two factors; The heart rate & The stork volume.Cardiac out put (C.O.) =heart rate (H.R.)* Stroke Volume (S.V.)
Stroke Volume; Is the amount of blood pumped out of each ventricle per beat its about 70ml at rest (form each ventricles) and it determined in part by neural in put.
Sympathetic stimuli making the myocardial muscle fiber contract with great strength at any given length and Parasympathetic have opposite effect.
Heart Rate: - is determined by the rate at which the S-A node beats, which has it’s own rhythmicity.
Naturally S-A node beats much higher than the rate normally found (70 beat/min.) this is because of the action of the vagus nerve (parasympathetic n.) which supplies the heart, its function to break S-A node beats. This inhibitory activity it’s termed vagal tone.
During sleeping increased vagal tone lead to decrease heart rate.
Factors affecting heart rate:
Size; H.R. is faster in small size bodies as it need large amount of oxygen for the high metabolism rate .
Females have faster H.R. than Males.
Higher centers in brain control or affects cardiac center in medulla. Cardiac center
originate the vagal tone. (Seen in emotional stress, or waiting for a race to start).
Para sympathetic influences include vagal tone which decrease S-A node beat.
Sympathetic influence causes the S-A node to beat at faster rate. Sympathetic nervous system also act on the ventricular muscles leading to more powerful contraction of the ventricle (adrenalin and nor adrenaline which increased in exercise and emotions).
Catecholamine (adrenalin and nor–adrenalin) from adrenal gland medulla will increase heart rate in case of excitement and emotional state.
Increased temperature (fever) will increase heart rat.
Hormones; Increased activity of Thyroid gland will increase Thyroxin (T4) and triiodothyronine (T3) which increase heart rate.
Baroreceptors act on cardiac center, its action to slow heart when blood pressure increases.
10. Sensory nerve has variable effect on heart rate.
Slight pain will increase H.R., while sever pain lead to decrease H.R.
Brady cardia: - Slow heart rate during sleep and some diseases.
Tachy cardia: - Increased or accelerate heart rate during exercise, emotions& fever.
C.O. = HR x SV
= 72 beats/min x 70 ml/beat
= 5040 ml/min 5L/min
C.O. of the right and left ventricles are exactly matched.
C.O. becomes mismatched in heart failure. Failing ventricle pumps less blood than healthy ventricle
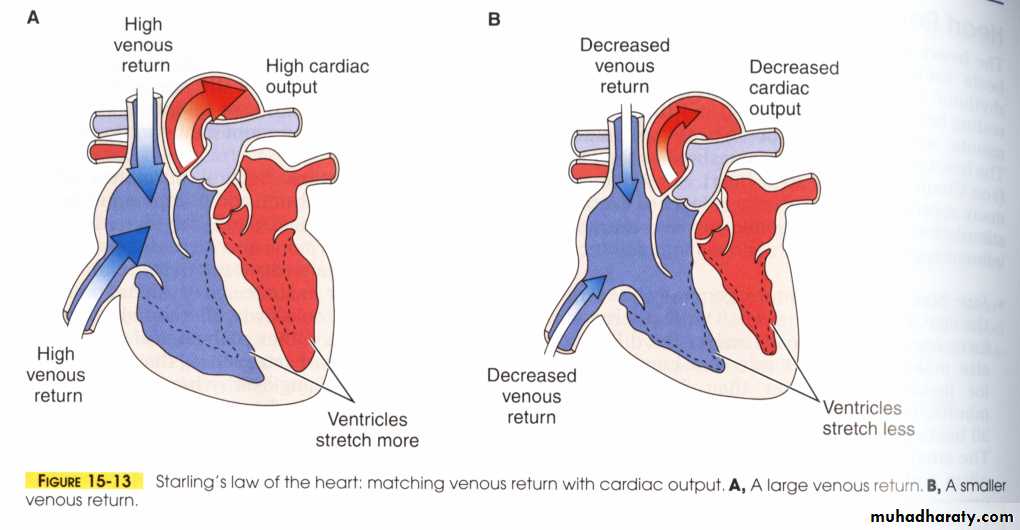
intrinsic (as described by Frank and Starling)
volume of blood in ventricles = more forceful contraction
stroke volume automatically increases in response to increased preload (amount of blood in the ventricles prior to contraction; increased venous return)
relates to the physiological properties of cardiac muscle in that increased stretch results in increased force of contraction
but, if the muscle is stretched too much, force of contraction
Frank-Starling Curve:
C.O. increases in case at anxiety and excitement (50-100%), Eating (30%), Exercise, high environmental temperature, pregnancy (especially late pregnancy), Epinephrine and histamine release.
While it decreased in: heart disease, rapid arrhythmias, Sitting or standing from laying position (20-30%).
In summary Factors influencing SV are:
1. Contractility
2. Preload (Venous return)
3. Afterload
4. HR