Paracoccidioidomycosis
(South American Blastomycosis)
Paracoccidioidomycosis is progressive mycosis of the lungs, skin, mucous
membranes, lymph nodes, and internal organs caused by Paracoccidioides
brasiliensis. Symptoms are skin ulcers, adenitis, and pain due to abdominal organ
involvement. Diagnosis is clinical and microscopic, confirmed by culture. Treatment
is with azoles (eg, itraconazole), amphotericin B, or sulfonamides.
Infections occur only in discrete foci in South and Central America, most often in
men aged 20 to 50, especially coffee growers of Colombia, Venezuela, and Brazil. An
estimated 10 million people in South America are infected. Although a relatively
unusual opportunistic infection, paracoccidioidomycosis sometimes occurs in
immunocompromised patients, including those with AIDS. Although specific natural
sites for Paracoccidioides brasiliensis remain undefined, it is presumed to exist in soil
as a mold, with infection due to inhalation of conidia (spores produced by the
mycelial form of the fungus). Conidia convert to invasive yeasts in the lungs and are
assumed to spread to other sites via blood and lymphatics.
Symptoms and Signs
Most people who inhale conidia of P. brasiliensis do not become ill; illness, if it
occurs, usually manifests as acute pneumonia, which may spontaneously resolve.
Clinically apparent infections can become chronic and progressive but are not usually
fatal. There are 3 patterns:
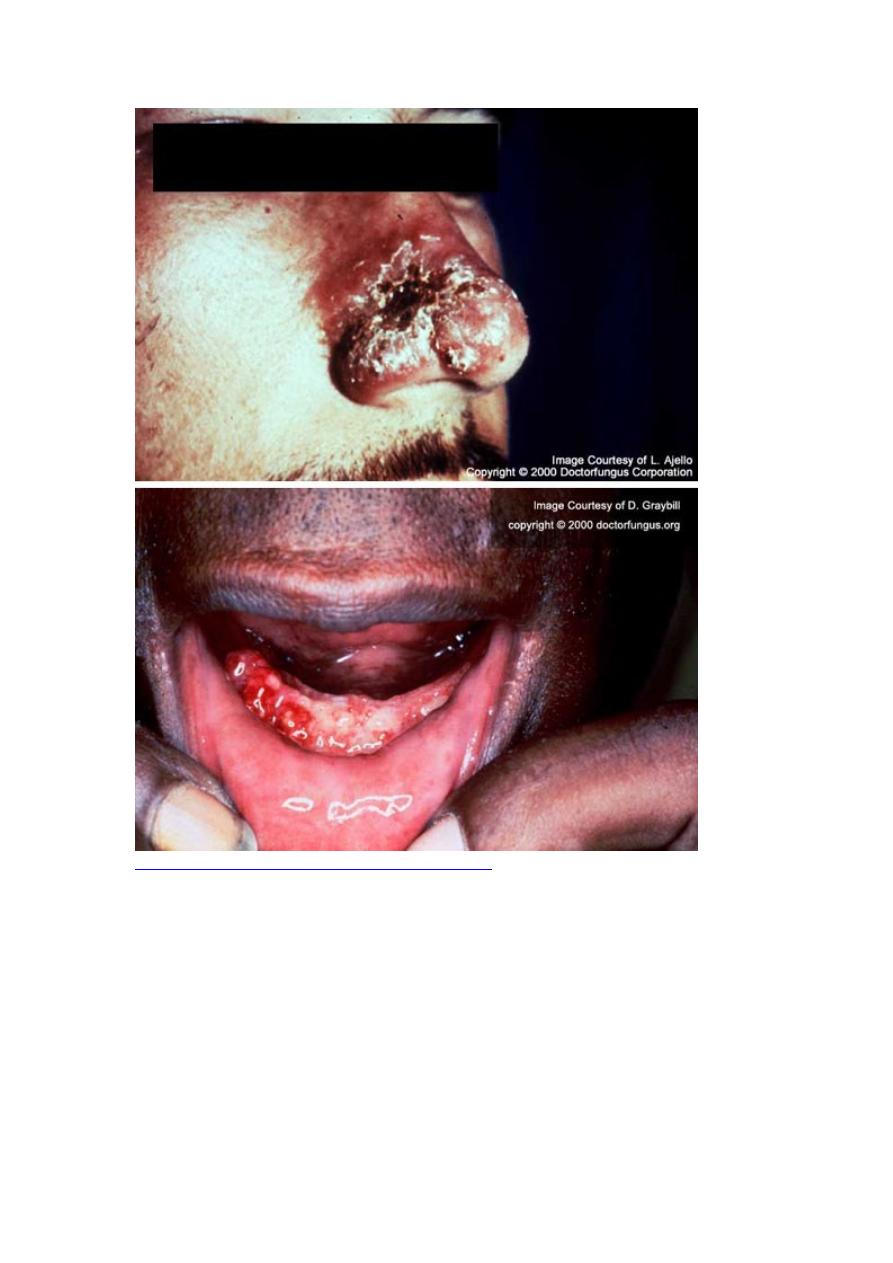
Mucocutaneous: Infections most often involve the face, especially at the
nasal and oral mucocutaneous borders. Yeasts are usually abundantly present
within pinpoint lesions throughout granular bases of slowly expanding ulcers.
Regional lymph nodes enlarge, become necrotic, and discharge necrotic
material through the skin.
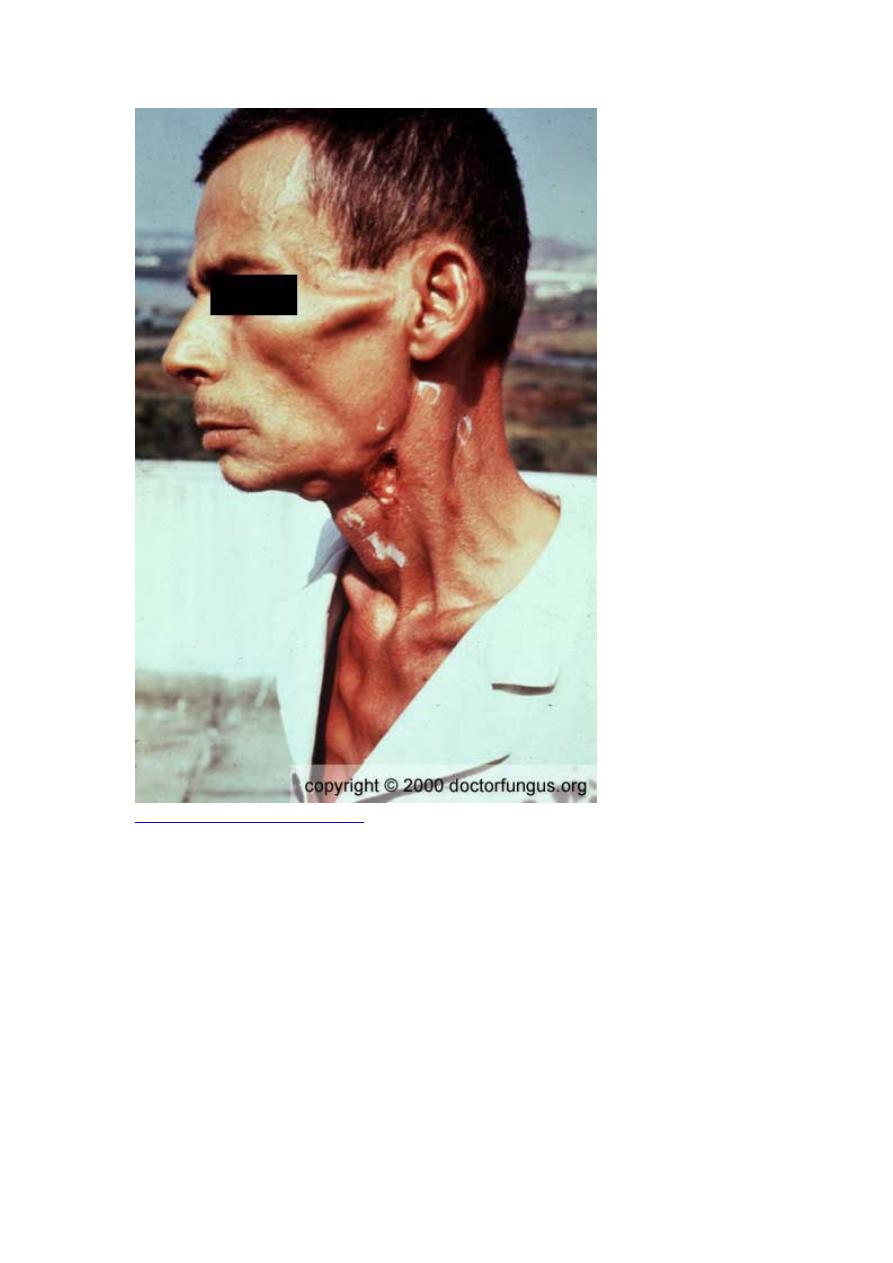
Lymphatic: Cervical, supraclavicular, or axillary nodes enlarge but are
painless.
Visceral: Typically, focal lesions cause enlargement mainly of the liver,
spleen, and abdominal lymph nodes, sometimes causing abdominal pain.
Infections may be mixed, involving combinations of all 3 patterns.
Diagnosis
Culture and/or histopathology
Clinical findings suggest the diagnosis. Culture is diagnostic, although observation of
large (often > 15 μm) yeasts that form characteristic multiple buds (pilot wheel) in
specimens provides strong presumptive evidence. Because culturing P. brasiliensis
can pose a severe biohazard to laboratory personnel, the laboratory should be notified
of the suspected diagnosis.
Treatment
Itraconazole

Azoles are highly effective. Oral itraconazole is generally considered the drug of
choice, primarily because it costs less than other azoles that are available in endemic
areas. IV amphotericin B can also eliminate the infection and is often used in very
severe cases. Sulfonamides, which are widely used in some countries because they are
inexpensive, can suppress growth of Paracoccidioides and cause lesions to regress but
are not curative and must be given for up to 5 yr.