Lecture-2 clinical immunologyimmune deficiency
Mechanisms of Immunodeficiency• Loss or reduction of:
• Cell type• Cell numbers
• Cell function
• Loss of Cell Function
• Receptors• Cell signaling
• Cytokine production
• Ig production
• Co stimulation impairment
• Intracellular killing
• Extravasation impairment
• Features of immunodeficiency diseases
• Primary or congenital immunodeficiencies
• Present at birth• Result from genetic abnormalities in one or more components of the immune system
• Secondary or acquired immunodeficiencies
• Later in life
• Much more common than primary immunodeficiency
• Result from infections, malnutrition, or treatments that cause loss or inadequate function of various components of the immune system
• Most common is acquired immunodeficiency syndrome, or AIDS
• Primary Immunodeficiency
• Myeloid lineage• Congenital agranulocytosis
• Leukocyte-adhesion deficiency
• Lymphoid lineage
• Severe combined immunodeficiency (SCID)
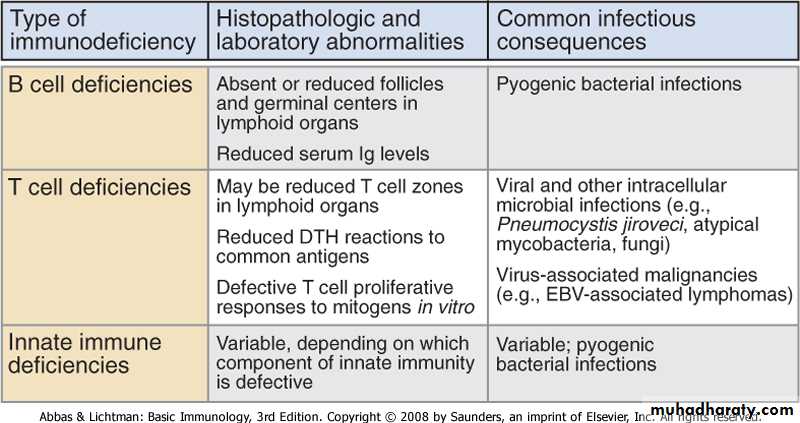
• B cells
• Agammaglobulinemia
• Hypogammaglobulinemia
• Specific Ig Deficiencies
• T cells
• DiGeorge Syndrome
• Wiskott Aldrich Syndrome
• 1/ Quantitative – decreased numbers of granulocytes –neutrophil elastase mutation
• Congenital chronic agranulocytosis
• Cyclic agranulocytosis (neutropenia)
• Myeloid lineage disorders – phagocytic cell defects
• 2/ Qualitative – phagocytes functional disorders, various enzyme deficits, inability of phagocytes to degrade the ingested material
• Chronic Granulomatous Disease (CGD)
• Approximately in 60% X-linked
• Enzymatic inability to generate toxic oxygen metabolites (H2O2) during oxygen consumption) - result of defect in neutrophilic cytochrome b (part of complex containing NADPH oxidase)
• Inability to kill bacteria such as Staph. aureus, Pseud.aeruginosa that produce catalase
• Clinical features: granulomas of skin, organs
• Treatment: long-term antibiotic administration
Another example of primary phagocyte def. are disorders of phagocyte migration because of failure to express adhesion molecules results in the inability of phagocytes to exit(go out) of blood stream. They cause recurrent bacterial infections &sites of infection lack pus or neutrophils infiltration.
Peripheral blood neutrophil count may be very high during acute infection because of the failure of mobilized neutrophils to exit blood vessels.
.
Defects in cytokine &cytokine receptors also result in failure of intracellular killing& such patients are susceptible to mycobacterial infection
Defects of common &classical pathway result in the susceptibility to infection by encapsulated bacteria like Neisseria
Mannose-binding lectin pathway def. is common& occur in 5% of general population &associated with infection in only individuals who are immune compromised..
Genetic def. Of C1,C2&C4 classical pathway result in autoimmune disease of sever type like SLE.
Def. Of regulatory protein C1 inhibitor cause angioedema.
SEVERE COMBINED IMMUNODEFICENCY
• In about 50% of SCID patients the immunodeficiency is x-linked whereas in the other half the deficiency is autosomal.• They are both characterized by an absence of T cell and B cell immunity and absence (or very low numbers) of circulating T and B lymphocytes.
• Patients with SCID are susceptible to a variety of bacterial, viral, mycotic and protozoan infections.
• Diagnosis
• Is based on enumeration of T and B cells and immunoglobulin measurement.• Severe combined immunodeficiency can be treated with bone marrow transplant &recently with gene therapy.
• B cell disorders
• Selective IgA deficiency• Disorder of B cell function
• Recurrent mild/moderate infections (respiratory, GIT, urinary tract) or asymptomatic
• Risk of reaction to live attenuated vaccines or generation of anti-IgA antibodies after a blood transfusion
• Selective IgG subclasses or specific IgG deficiency
• B cell function disorder
• Onset of symptoms in childhood, mostly respiratory tract infections caused by encapsulated bacteria (H.influenzae, Pneumococci)
• Transient hypogammaglobulinemia of infancy
• Common Variable Immunodeficiency (CVID)
There are defect in T cell signaling to B cellsAcquired agammaglobulinemia in the 2nd or 3rd decade of life
May follow viral infection
Pyogenic infection
80% of patients have B cells that are not functioning
B cells are not defective. They fail to receive signaling from T lymphocytes
Unknown
In X-LA early maturation of B cells fails
Affect malesFew or no B cells in blood
Very small lymph nodes and tonsils
No Ig
Small amount of Ig G in early age
Recurrent pyogenic infection
• X-linked agammaglobulinaemia
With an exception of selective IgA def., immunization is generally not effective because of the defect in IgG antibody production.
As with all primary immune deficiencies, live vaccines should be avoided.
T-cell disorders
• DiGeorge syndrome• Disorder of prethymocytes maturation due to absence of thymus (disorder of development of 3rd and 4th branchial pouch)
• Congenital heart diseases
• The onset of symptoms after the birth – hypocalcemic spasms and manifestations of cong.heart disease
• Immunodeficiency could be only mild, the numbers of T lymphocytes later usually become normal
• Treatment symptomatic
• Wiskott-Aldrich syndrome:
• Associated with normal T cell numbers with reduced functions, which get progressively worse.• IgM concentrations are reduced but IgG levels are normal
• Both IgA and IgE levels are elevated.
• Boys with this syndrome develop severe eczema.
• They respond poorly to polysaccharide antigens and are prone to pyogenic infection.
Patients with suspected T-cell immune deficiencies should receive anti-Pneumocystis and antifungal prophylaxis, and require aggressive management of specific infection. Thymic transplantation may be used for treatment of DiGeorge syndrome.
Secondary Immunodeficiency
Causes of secondary immune deficiency1-physiological immune deficiency.
Ageing pregnancy prematurity2-infection
HIV measles TB
3-Iatrogenic
Immunosuppressive therapy , antineoplastic agents , corticosteroids , stem cell transplantation& radiation therapy
4-malignancy
B-cell malignancies including leukemia, lymphoma & multiple myeloma, solid tumors & thymoma5-Biochemical and nutritional disorders
Malnutrition, renal insufficiency/dialysis ,DM, specific mineral deficiencies, eg. iron , zinc.
6- other conditions
Burns, asplenia / hyposplenism .
Warning signs of immune deficiency
1-8 respiratory tract infections/year in a child, or more than 4 respiratory tract infections/year in an adult
2->1 infection requiring hospital admission or IV antibiotics
3-infections with unusual organisms.
4- infections at unusual sites
5-chronic infection unresponsive to usual treatment.6-early end organ damage(eg. Bronchiectasis).
7-family history of immune deficiency.