
1
Disorders of the conjunctiva
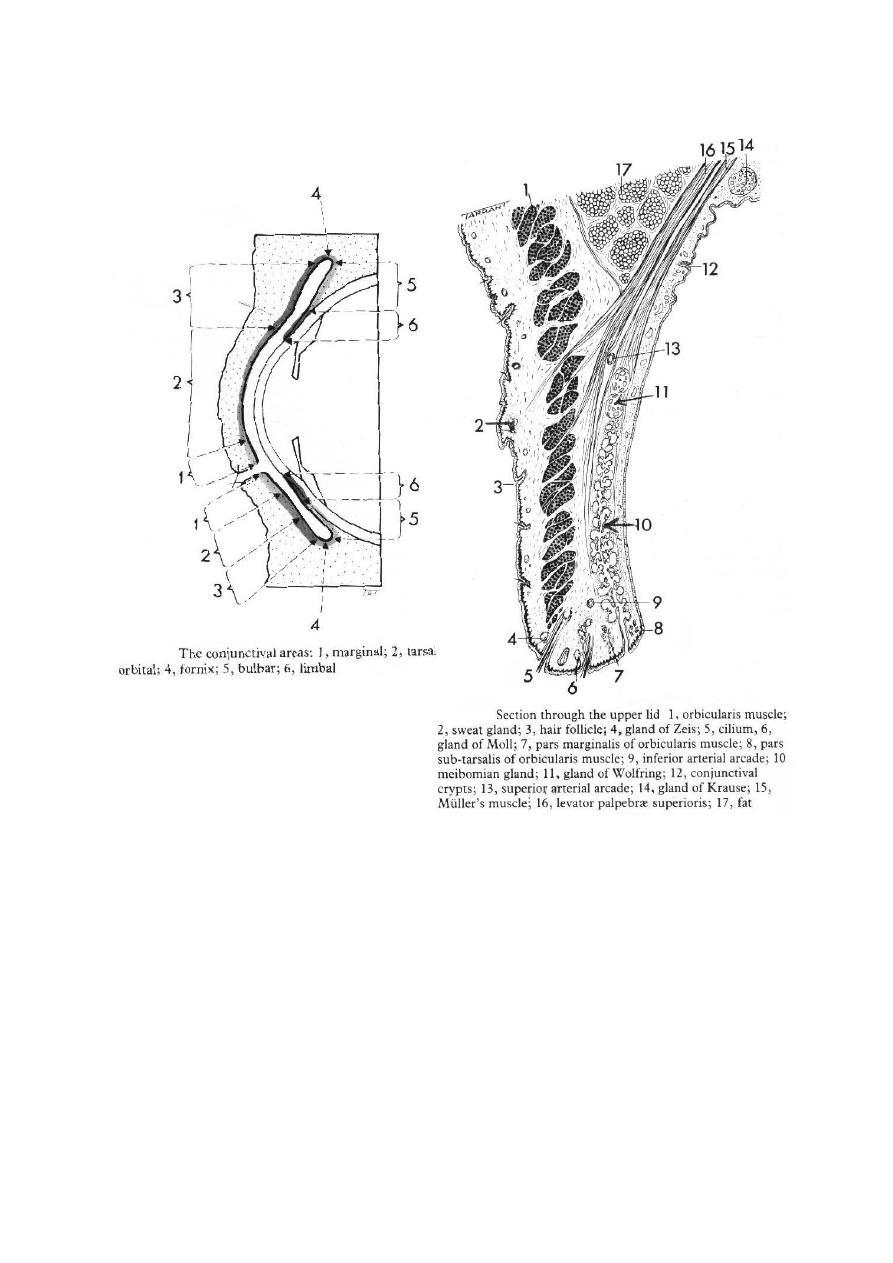
Applied anatomy:
Conjunctiva is a transparent layer. It consists of two layers:
1- Epithelium: 2-5 cell layers, basal cells are cuboidal and superficial cells are
flattened polyhydral.
2- Stroma (substantia propria): It is a richly vascularized connective tissue,
which is separated from epithelium by a basement membrane. Stroma is made
of two layers:
a- superficial adenoid layer: It is not developed until about three months
after birth.
* When conjunctiva infected at three months or less, there is no lymph tissue
developed yet, so there is no follicular reaction.
b- Deep thicker fibrous tissue.
3- Mucin secretors: They are of three types:
a- Goblet cells.
b- Crypts of Henle: Found at upper part of tarsal plate.
c- Glands of Manz.
Function: Lubrication.
4- Accessory lacrimal glands:
a- Krause.
b- Wolfring.
They are found deep in stroma mainly at fornices.
* Plus these accessory lacrimal glands, there is the main lacrimal gland that
resides in the superotemporal orbit, partially within a shallow bony fossa in the
lateral angular process of the frontal bone (fossa glandula lacrimalis).
5- Clinical parts:
a- Palpebral: starts at the mucocutaneous junction, it is firmly adherent to
the tarsal plate.
b- Forniceal: loose, redundant part, it swells easily.
c- Bulbar: it covers the anterior surface of sclera.
dr.Imad
2
Clinical Evaluation of conjunctival inflammation:
The differential diagnosis of conjunctival inflammation depends on:
1- Symptoms:
Conjunctivitis: Has non-specific symptom such as: lacrimation, irritation,
stinging, burning and photophobia (visual acuity is not affected as
conjunctivitis is away from visual axis).
If it is associated with keratitis, there will be pain foreign body sensation and
sometimes blurred vision (as cornea is affected).
In allergic conditions, the hallmark is itching, which also occurs in
blepharitis (inflammation of lymph margin) and keratoconjunctivitis sicca.

3
2- discharge:
It is exudates filtered through conjunctival epithelium from dilated blood
vessels with additional epithelial debris, mucus and tear (all mentioned are the
contents of the discharge).
a- Watery: Serous exudates and reflexly secreted tear.
- Acute viral conjunctivitis.
- Allergic conjunctivitis.
b- Mucoid: Associated with:
- Vernal conjunctivitis.
- Keratoconjunctivitis sicca.
c- Purulent: Severe acute bacterial conjunctivitis.
d- Mucopurulent: - Mild bacterial conjunctivitis.
- Chlamydial infections.
3- Conjunctival Appearance:
a- Conjunctival injection: Can give a clue in diagnosis although it is a non-
specific feature, in which, the beefy-red conjunctiva suggests a bacterial
cause (especially in the inferior fornix).
b- Subconjunctival haemorrhages: mostly associated with:
- Viral infection, e.g.: Adenovirus, Acute haemorrhagic conjunctivitis.
- Bacterial infection, e.g. Streptococcus pneumoniae.
* It may occur with sneezing, coughing, trauma, systemic diseases (blood
disorders as leukaemia).
c- Follicular reaction: It is
seen by magnification by slit-
lamp, consists of hyperplasia of
lymphoid tissue within the
stroma, commonly occurs in
(inferior) forniceal conjunctiva.
*
The
main
causes
are
(differential diagnosis):
- Viral infections.
- Chlamydial infections.
- Hyper sensitivity to topical
medications.
d- Papillary reaction: It is of
less diagnostic value than
follicular
reaction.
It
is
hyperplasia
of
conjunctival

4
epithelium (surrounding a core of blood vessels) thrown into numerous folds
or projections. Commonly occurs in the upper palpebral conjunctiva.
Clinically seen as a fine mosaic-like pattern of elevated polygonal hyperemic
areas separated by paler channels. Main causes are:
- Chronic blepharitis.
- Allergic conjunctivitis.
- Bacterial conjunctivitis.
- Contact lens-related problems.
e- Oedema (chemosis): whenever the conjunctiva is severely inflamed. It is
transudation of fibrin and protein-rich fluid through the walls of the damaged
blood vessels producing a translucent swelling of the conjunctiva.
f- Scarring: its causes are:
- Trachoma.
- Ocular cicatricial pemphigoid.
- Atopic conjunctivitis.
- Prolonged use of topical medications.
4- Conjunctival membranes:
a- Pseudomembranes:
Coagulated exudates adherent to the inflamed conjunctival epithelium,
peeled off leaving the epithelium intact (or healthy).
- Severe adenoviral infection.
- Gonococcal conjunctivitis.
- Steven-Johnson syndrome.
b- True membranes:
When inflammatory exudates permeates the conjunctival epithelium.
Removal of membranes may be accompanied tearing of the epithelium and
bleeding.
- Beta-haemolytic Streptococci.
- Diphtheria.
5- Lymphadenpathy:
The upper and lower lids with eye ball and other structures drains to the
preauricular and submandiblar lymph nodes. These lymph nodes are swollen in
these cases:
- Viral infections.
- Chlamydial infections.
- Severe Gonoccocal infections.
* ALL THE PREVIOUS WAS ONLY AN INTRODUCTION!!

5
Bacterial Conjunctivitis
1- Simple bacterial conjunctivitis:
It is a common disease, and usually it is self-limiting condition. Common
causative organisms are:
- Staphylococcus epidermidis.
- Staphylococcus aureus.
- Other like Strptococcus pneumoniae, H. influenzae.
Symptoms:
- Acute onset of redness.
- Grittiness ) .(خشونة أو رمل بالعين
- Burning.
- Discharge.
- On morning, eyelids are stuck together due to accumulation of exudates
during the night.
- Both eyes are usually involved.
Signs:
- The eyelids are crusted and oedematous (mild oedema).
- Mucopurulent discharge.
- Beefy-red injection, maximally in the fornices.
- Membranes in severe cases.
- Corneal involvement is uncommon.
* Blurred vision may occur due to mucus not due to corneal involvement.
Treatment:
- Usually resolves within 10-14 days and laboratory tests are not routinely
performed.
- Bathe all discharge away.
-Topical drops (Antibiotics): Chloramphenicol, ciprofloxacin, ofloxacin,
gentamicin, neomycin, tobramycin.
- Antibiotic ointments: higher concentration for long period and we give it at
night because it causes blurred vision, we have chloramphenicol, gentamicin,
tetracydine, framycetin.
2- Adult gonococcal keratoconjunctivitis:
- Caused by: Gram-negative diplococcus Neisseria gonorrhoea.
- It is a rare condition.
Symptoms:
- Hyperacute presentation.
- Profuse and thick creamy (purulent) pus.
Signs:
- Eyelids are oedematous and tender.
- Discharge is profuse and purulent.

6
-Intense
hyperaemia
(conjunctival
injection),
chemosis
and
pseudomembranes format.
- Preauricular lymphadenopathy and sometimes suppuration of nodes.
- Keratitis may occur in severe cases.
Treatment:
- Hospitalization (we should admit this patient to hospital).
- Cultures.
- Eye irrigation with saline (frequent)
- Antibiotics:
i- Systemic antibiotics:
*cefotaxime 500mg * 4 i.v for 1 day incase of conjunctivitis only or for
3-5 days if it is associated with keratitis.
* Spectinomycin in penicillin-resistant cases.
ii- Topical Antibiotics:
* Gentamicin, or
* Bacitracin.
3- Neonatal Keratoconjunctivitis:
* Ophthalmia neonatorum is any infection of the eye within one month from
birth.
- Usually appears at 1-3 days of life.
- Rare condition.
Signs:
- Hyperacute presentation.
- Chemosis.
- Pseudomembranes.
- Corneal involvement.
Treatment: Systemic and tropical.
Viral Conjunctivitis
1- Adenoviral keratoconjunctivitis:
- It is a highly contagious virus.
- Transmission is via respiratory or ocular secretion.
- Dissemination is by contaminated towels or equipments.
- Incubation period is 4-10 days; it is an occupational hazard of
ophthalmologists (due to contamination of the hands).
Clinically there are two ocular syndromes:
a- Pharyngoconjunctival fever (PCF):
- Caused by serotypes 3 & 7.
- Typically affects children and causes URT infection (systemic
manifestations as pharyngitis, fever and pre-auricular lymphadenopathy).
- Keratitis develops in about 30%.

7
b- Epidemic keratoconjunctivitis (EKC):
- Caused by serotypes 8 & 19.
- Usually not associated with systemic symptoms.
- Keratitis occurs in about 80%, so it is more serious due to affection of
visual acuity.
Conjunctivitis:
Presentation: acute onset of watery discharge, redness, discomfort and
photophobia, both eyes are affected in 60% of cases.
Signs:
- Eyelids are oedematous.
- Watery discharge.
- Mild chemosis to moderate.
- Follicular reaction.
- Subconjunctival haemorrhages.
- Pseudomembranes.
- Lymphadenopathy is tender.
Keratitis:
Stage I: Within 7 days of onset, diffuse epithelial keratitis .
Stage II: after 7 days, focal (patchy multiple foci)sub epithelial keratitis.
Stage III: anterior stromal infilterate
If they are untreated, they may persist for months or years.
Treatment:
a- Avoid transmission following examination of patients:
- Washing of hands.
- Meticulous disinfection of ophthalmologic instruments.
- Infected hospital personnel should not be in contact with patients.
b- Medications:
i- For conjunctivitis:
- Spontaneous resolution occurs within 2 weeks.
- Antiviral agents are ineffective (has no role).
- Topical steroids are indicated only in very severe inflammations and
when Herpes simplex infection has been excluded (if steroids are used
for Herpes simplex infection, they will lead to inevitable blindness) and
the treatment with steroids is symptomatic and supportive (not used
routinely).
ii- For keratitis:
- topical steroids, which are indicated only if the eye is uncomfortable or
there is diminishing of the visual acuity by stage III lesions, all that after
exclusion of Herpes simplex infection.
Note:
Steroids do not shorten the natural course of the disease but suppress
the inflammation and relief symptoms.

8
2- Herpes simplex conjunctivitis:
Conjunctivitis may occur in patients with primary Herpes simplex infection.
- when the person catches the infection for the first time it is primary, after
treatment, the virus get dormant in the trigeminal nerve ganglia, for any reason
if the person get immune-compromised, then secondary infection is developed.
Signs:
- The eyelids and periorbital skin show unilateral herpetic vesicles, which
may be associated with oedema.
- Watery discharge.
- Ipsilateral follicular reaction.
- Lymphadenopathy is tender.
- Keratitis is uncommon.
- Herpes simplex infection is very severe and it can lead to dendritic ulcer of
the cornea.
- No subconjunctival haemorrhage.
Treatment: Antiviral agent (as Acyclovir "Zovirax™") for 21 days to prevent
keratitis.
3- Molluscum contagiosum conjunctivitis:
- It is an oncogenic virus that produces characteristic lesions on the skin and
less commonly on the mucus membranes (e.g. conjunctiva).
- It spread by close contact.
- Typically affects adolescent children and young adults.
- Also it is common in the patients with AIDS (i.e. immune-compromised).
Signs:
- Small, pale, waxy and umbilicated nodule in the eyelid margin.
- Follicular conjunctival reaction.
- In longstanding cases, there is associated epithelial keratitis
Treatment:
Destruction of lesions by shave excision (surgical shaving), cryotherapy or
cauterization.
Chlamydial Conjunctivitis
1- Adult chlamydial keratoconjunctivitis:
It is a sexually transmitted disease caused by the obligate intracellular
bacterium Chlamydia trachomatis (serotypes D, E, F, G, H, I, J & K).
- Patients are usually young and at least 50% have a concomitant genital
infection (cervicitis in ♀ or urethritis in ♂).
Mode of transmission:
- Autoinoculated from genital secretions.
- Eye to eye spread is rare.

9
Incubation period: 1 week.
Presentation:
Subacute onset of unilateral or bilateral mucopurulent discharge.
Signs:
- Eyelids are lightly oedematous.
- Mucopurulent discharge.
- Conjunctival reaction: At first, there is papillary hypertrophy then large
follicles are formed at the inferior fornix but may involve upper tarsal
conjunctiva.
- Lymphadenopathy (not tender).
- Keratitis is uncommon.
- Conjunctival scarring + Pannus (neovascular or fibrovascular membrane
involving superficial part of cornea, i.e. affects the cornea not the
conjunctiva).
Treatment:
a- Topical therapy: Tetracycline ointment *4 for 6 weeks.
b- Systemic therapy: One of the following:
i- Doxycycline: 100mg *1 for 1-2 weeks.
ii- Tetracycline: 250mg *4 for 6 weeks.
iii- Erythromycin: 250mg *4 for 6 weeks.
2- Neonatal chlamydial conjunctivitis:
- The most common cause of neonatal conjunctivitis.
- It may be associated with systemic infection, e.g. otitis, rhinitis or
pneumonitis.
- It is transmitted from the mother during delivery.
Presentation:
The child is usually presented between 5 & 19 days after birth.
Signs:
- Papillary conjunctivitis (there is no follicular reaction as the lymphoid
tissue develops after3 months after).
- Mucopurulent discharge.
Complications (if not treated):
Conjunctival scarring and superior corneal pannus.
Treatment:
a- Topical Tetracycline.
b- Oral Erythromycin, 250mg/kg body weight daily for 14 days.
3- Trachoma:
- It is an infection caused by serotypes A, B, B
a
and C of Chlamydia
trachomatis.

10
- It is a disease of underprivileged populations with poor conditions of
hygiene (low socioeconomic status).
Transmission:
Common fly is the major vector, currently trachoma is the leading cause of
preventable blindness in the world.
Presentation: is usually during childhood.
Signs:
- Follicular reaction associated with diffuse papillary reaction but under age
of 2 years, the papillary reaction is predominant.
- Chronic conjunctival inflammation causes conjunctival scarring that
involves the entire conjunctiva but most prominent on the upper tarsus.
- Progressive conjunctival scarring: if it is severe lead to:
* Destruction of lids.
* Trichiasis: Misdirection of eyelashes towards the cornea causing
rubbing of cornea, it is either true trichiasis (due to affection of hair
follicles) or pseudo (due to entropion of lid margin).
* Entropion: the inward turning of the eyelid.
* Dry eyes, due to destruction of goblet cells and lacrimal ducts.
- End-stage trachoma:
* Corneal ulceration (due to dry eye and trichiasis, superficial cornel
ulcers usually heal by regeneration so the cornea remains transparent,
while deep ulcers do not regenerate but heal by fibroblasts to fibrous
tissue leading to opacification)and opacification, which lead to
diminished visual acuity or blindness.
World Health Organization (WHO) grading:
TF: Trachoma follicles (5 or more follicles in the superior tarsal conjunctiva).
TI: Trachomatous intense inflammation diffusely involving the tarsal
conjunctiva.
TS: Trachomatous conjunctival scarring.
TT: Trachomatous trichiasis touching the cornea.
CO: Corneal opacity.
Treatment of trachoma:
-indicated for stages I & II (TF & TI), as there is no benefit from treating
stages III, IV &V as there is no active organism (and even the medications
used or applied may cause scarring).
- Preventive measures: strict personal hygiene, especially washing the face
of young children .
- Single dose of Azithromycin plus systemic erythromycin.

11

12
