
Parasitic Infestations
of the Skin
OMAR Y. ABDULLAH

Scabies
• Human scabies is a highly contagious disease caused by
the mite Sarcoptes scabiei var. hominis which is an
obligate parasite to humans.
• Scabies is not primarily a sexually transmitted disease
but sexual transmission does occur.
• Scabies spreads in households and neighborhoods in
which there is a high frequency of intimate personal
contact or sharing of inanimate objects.
• Dogs and cats may be infested by almost identical
organisms; these sometimes may be a source for
human infestation.
• Scabies is endemic in many developing countries and is
usually associated with overcrowding, low
socioeconomic standards, and poor hygiene.

ANATOMIC FEATURES
• The adult mite is ⅓-mm
long and has a flattened,
oval body with wrinklelike,
transverse corrugations
and eight legs.
• The digestive tract fills a
major portion of the body.
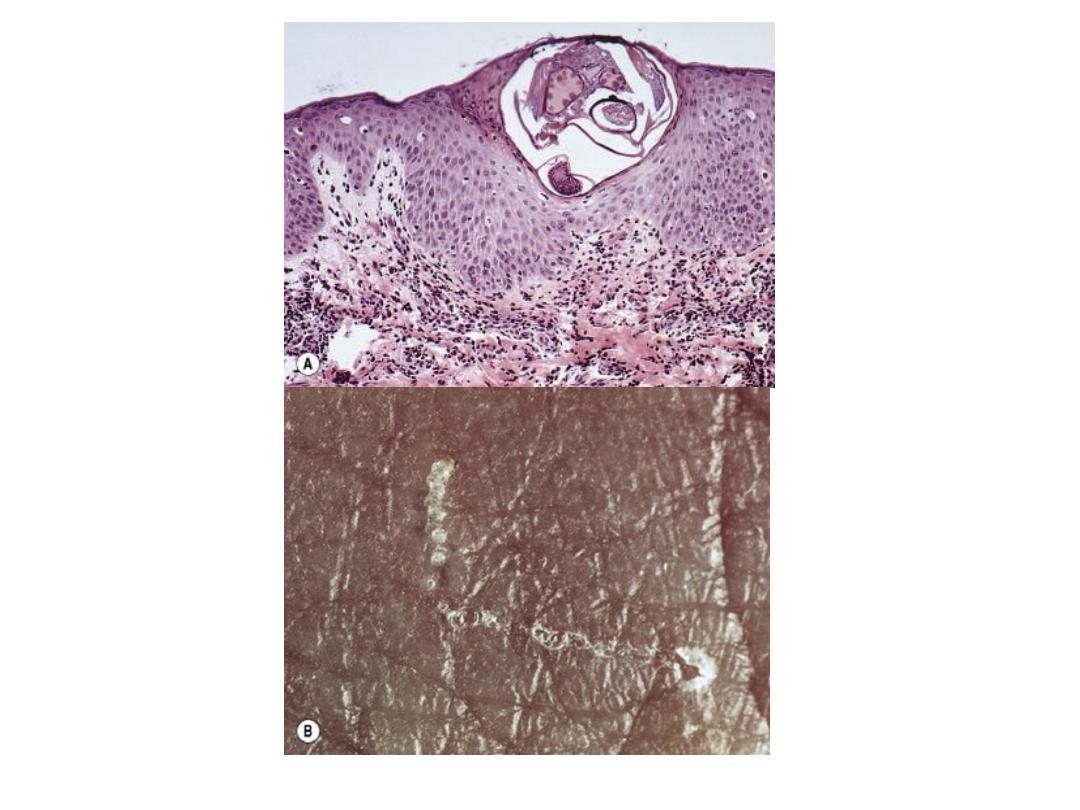

Infestation and life cycle
• Infestation begins when a fertilized female mite arrives on
the skin surface.
• Within an hour, the female excavates a burrow in the
stratum corneum.
• During the mite’s 30-day life cycle, the burrow extends
from several mms to few cms in length.
• The burrow does not enter the underlying epidermis except
in the case of hyperkeratotic Norwegian scabies.
• Eggs are laid at the rate of 2-3 a day and fecal pellets
(scybala) are deposited in the burrow.
• Scybala are dark, oval masses that are seen easily when
burrow scrapings are examined under a microscope.
• Scybala may act as an irritant and may be responsible for
some of the itching.
• The larvae hatch, leaving the egg casings in the burrow, and
reach maturity in 2-3 weeks.

Immunology
A hypersensitivity reaction rather than a foreign
body response may be responsible for the
lesions.

Clinical manifestations
• The disease begins insidiously.
• Symptoms are minor at first?
• Scratching destroys burrows (and other primary
lesions) and removes mites, providing initial
relief.
• Scratching also spreads mites to other areas and
after 6 to 8 weeks the once localized area of
minor irritation has become a widespread,
intensely pruritic eruption.
• Lesions are pleomorphic and tend to remain
discrete and small.

Lesions of scabies
PRIMARY LESIONS
• Burrow
• Vesicles
• Papules
Mites are found in burrows and at the edge of vesicles but rarely in papules.
SECONDARY LESIONS
• Pinpoint erosions
• Pustules
• Eczematous changes
• Nodules
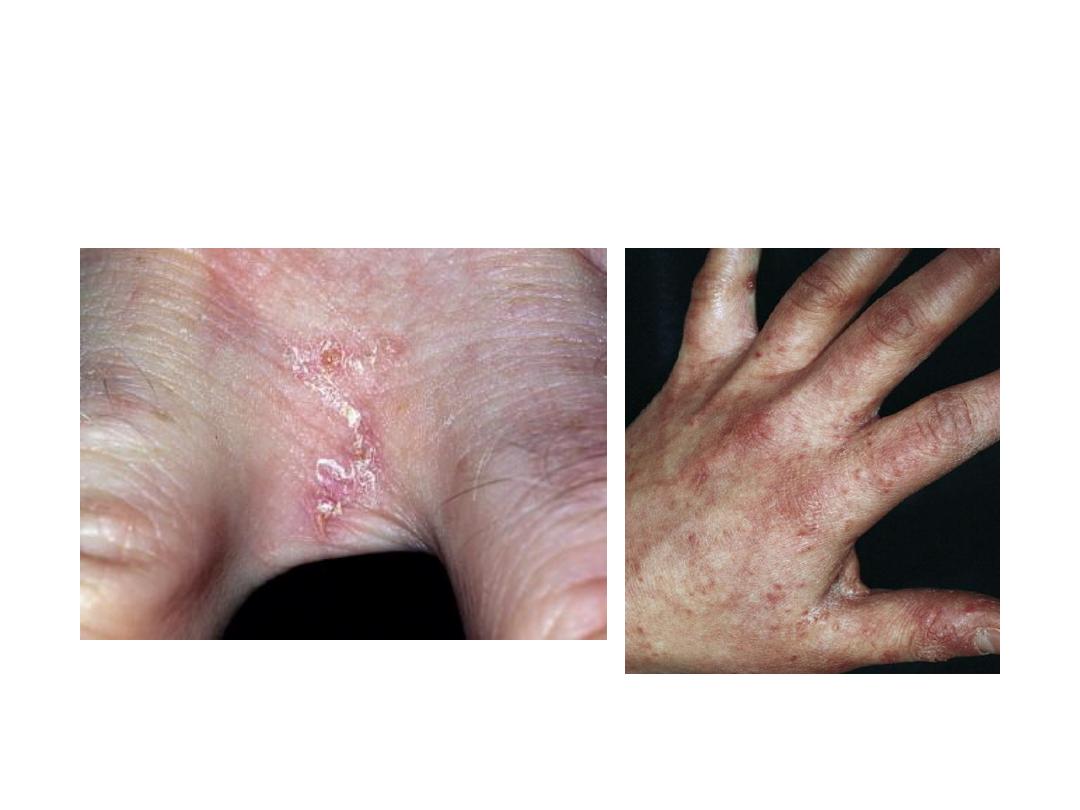
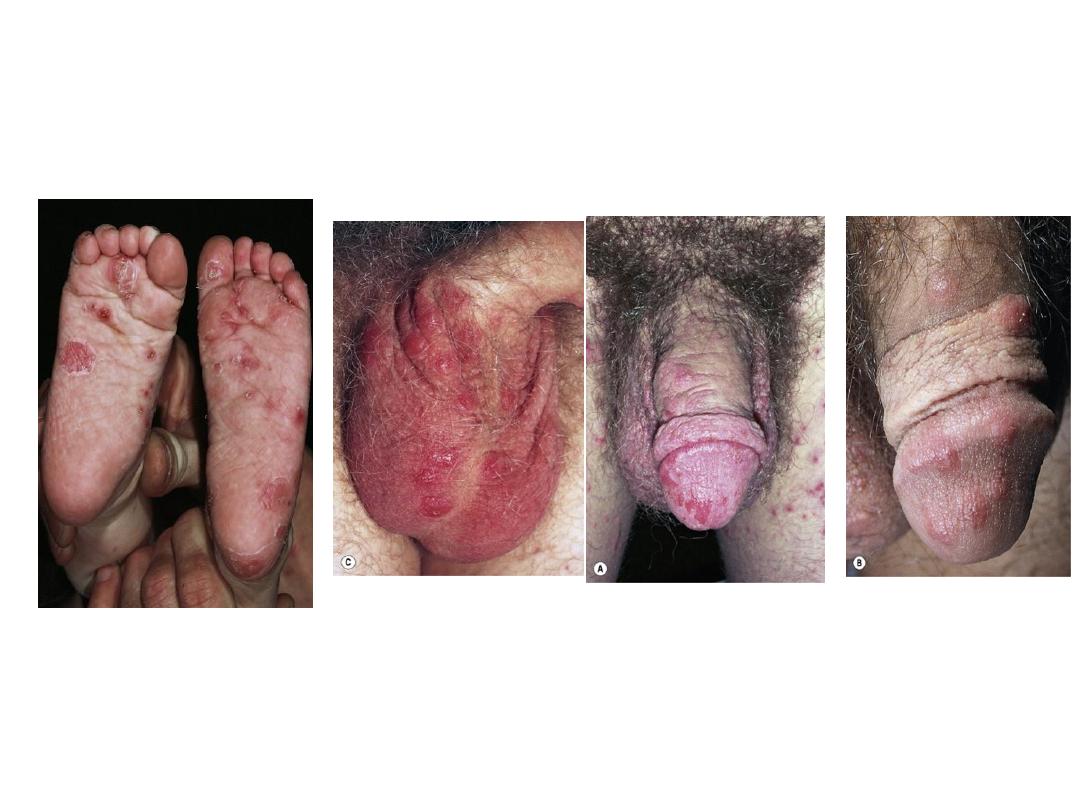

Symptoms and signs of scabies
• Rash present for 4 to 8 weeks has suddenly become
worse.
• Generalized, severe itching
• Nocturnal itching
• Pinpoint erosions and crusts on the buttocks
• Vesicles in the finger webs
• Diffuse eruption sparing the face
• Nodules on the penis and scrotum
• Patient becomes better, then worse, after treatment
with topical steroids.
• Rash is present in several members of the same
family.
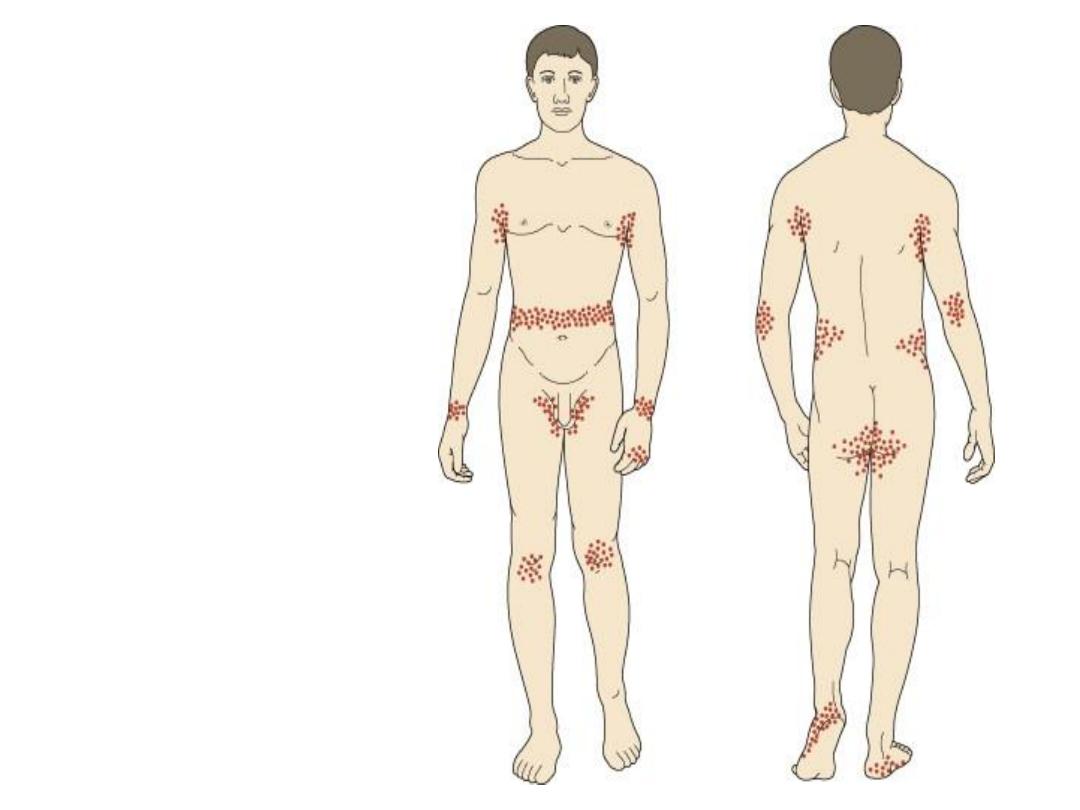
Distribution

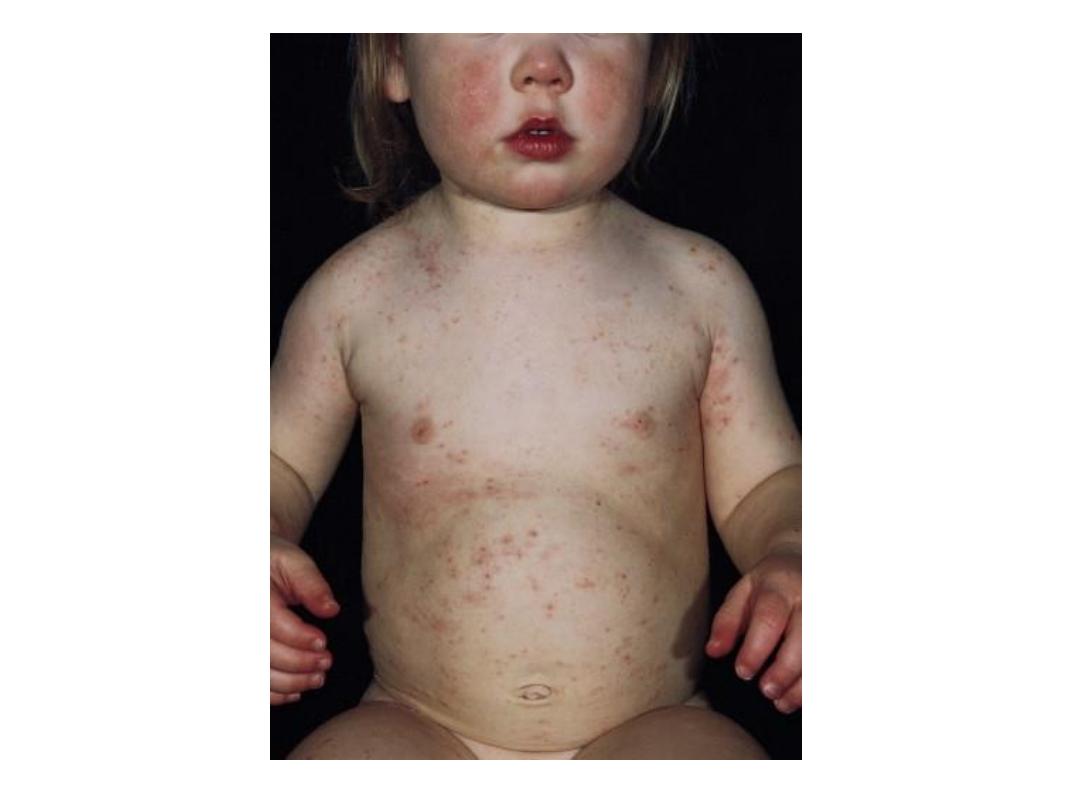
Scabies in infants
• Widespread involvement usually due to misdiagnosis and Rx.
• Sometimes the face and scalp are affected.
• Vesicles are common on the palms and soles (characteristic).
• Secondary eczematization and impetiginization are common.
• Burrows are difficult to find.
• Nodules may be seen in the axillae and diaper area.
Scabies in the elderly
• The decreased immunity associated with advanced age may allow
the mites to multiply and survive in great numbers.
• Therefore, few cutaneous lesions (other than excoriations, dry skin,
and scaling) are present.
• Eventually papules and nodules appear and may become
numerous.
• Itching is intense.

Treatment and management
Permethrin
(cream)
• Is the drug of choice for the treatment of scabies in
children and adults of all ages including pregnant and
lactating women.
• Two applications 1 week apart, apply from head/neck
to toe and wash after 8-12 hours (for permethrin and
lindane).
Lindane
(cream, shampoo, and lotion)
• Is a central nervous system stimulant that produces
seizures and death in the scabies mite.
• It accumulates in fat and binds to brain tissue,
therefore excessive use can be dangerous.
• No pre-bathing in lindane.

BENZYL BENZOATE
• The 25% lotion is the most common preparation.
• Application is just like sulfur
CROTAMITON
• Once-a-day application for 2 to 5 days.
• It has antipruritic properties.
SULFUR
• The pharmacist mixes 5% to 10% precipitated sulfur in petrolatum.
• The compound is applied to the entire body below the neck once
each day for 3 days and the patient is instructed to bathe 24 hours
after each application.
• These preparations are messy, have an unpleasant odor, stain, and
cause dryness.
• Sulfur in petrolatum is thought to be safe for infants <2 months old
and pregnant and nursing women.

Ivermectin
• Indications?
• Dose: 200µg/kg, two doses, 2 weeks apart.
• Cure rate=95%

MANAGEMENT OF COMPLICATIONS
• ECZEMATOUS INFLAMMATION
• PYODERMA
• POST-SCABIETIC PRURITUS
Pruritus may persist for weeks after treatment (may be due to
hypersensitivity response to remaining dead mites and mite
products).
• NODULAR SCABIES

ENVIRONMENTAL MANAGEMENT
• Intimate contacts and all family members in
the same household should be treated.
• Mites can live in dust , chairs, and bed linens
for several days.
• Wash all clothing, towels, and bed linen (in a
normal washing machine cycle) that have
touched the skin.

Pediculosis
• Lice are obligate human parasites that cannot
survive off their host.
• Three kinds of lice infest humans:
Pediculus humanus var. capitis (head louse)
Pediculus humanus var. corporis (body louse)
Phthirus pubis (pubic or crab louse)

• Lice feed approximately five times each day by
piercing the skin with their claws, injecting
irritating saliva, and sucking blood that makes
them rust colored (characteristic).
• Lice feces appear on the skin as small, rust-
colored flecks.
• Saliva and fecal material can induce a
hypersensitivity reaction and inflammation.
• Lice are active and can travel quickly, which
explains why they can be transmitted so easily.
• The life cycle from egg to egg is approximately 1
month.
• Transmission is by close personal contact and
contact with objects such as combs, hats,
clothing, and bed linen.

Nits
• The female lays approximately six eggs, or
nits, each day for up to 1 month, and then
dies.
• Nits are 0.8 mm long and are firmly cemented
to the bases of hair shafts close to the skin to
acquire adequate heat for incubation.
• Nits are very difficult to remove from the hair
shafts.

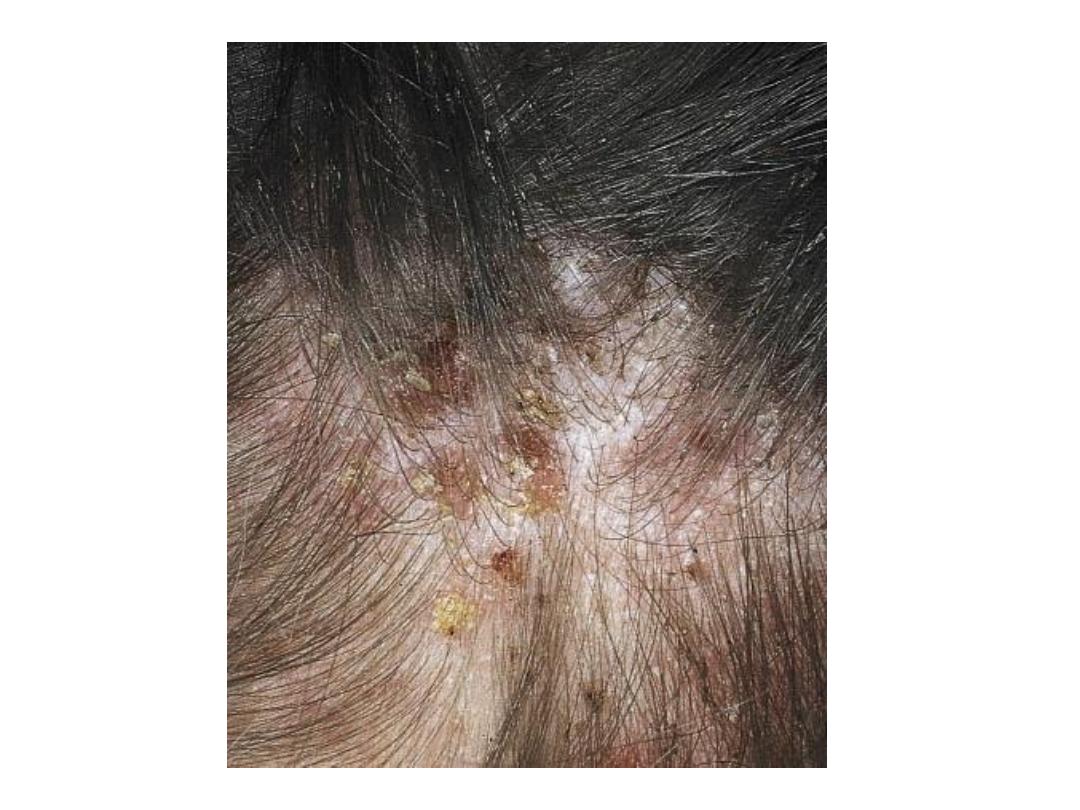
Clinical manifestations of Pediculosis capitis
• Lice infestation of the scalp is most common in children.
• More girls than boys are afflicted.
• Commonly seen on the back of the head and neck and behind the
ears.
• The average patient carries less than 20 adult lice.
• Scratching causes inflammation and secondary bacterial infection,
with pustules, crusting, and cervical lymphadenopathy.
• Posterior cervical adenopathy without obvious disease is
characteristic of lice.
• Sensitization to the lice toxin, feces, or body parts lasts for 3 - 8
months and is a cause of pruritus.
• Eyelashes may be involved, causing blepharitis.
• Head lice can survive away from the human host for about 3 days,
and nits can survive for up to 10 days.
• Transmission is by direct contact and also by fomite transmission.
• Head lice do not carry any human disease.

Diagnosis
• Scalp will be apparent to those who carefully
examine individual hairs.
• Finding nits does not indicate active infestation
and may persist for months after successful
treatment
• Combing the hair with a fine-toothed comb.
• Lice and nits can be seen easily under a
microscope.
• Nits fluoresce and can be detected easily by
Wood’s light examination. Nits that contain an
unborn louse fluoresce white. Nits that are empty
fluoresce gray.

Treatmant
• Permethrin (1% and 5%) is the most effective
treatment. It paralyzes the nerves that allow the
lice to breathe.
• Remains active for 2 weeks.
• Only apply to dry hair.
• It is insecticidal and ovicidal.
• Two applications (10 min. each) one week apart.
• Permethrin has a clinical efficacy of 95%.
• Lindane and pyrethrin have cure rates less than
90%.

Malathion
• Malathion is rapidly pediculicidal and ovicidal
and is useful for lice resistant to pyrethrins
and permethrin.
• It binds to hair and has residual activity.
• A 1% shampoo is applied to the scalp and
washed out 10 minutes later and repeated in
1 week.
• It is not recommended for infants and
neonates.

Other measures
• Ivermectin
• Co-trimoxazole (480mg twice daily for 3 days), and
repeated after 1 week.
• Shaving the head
• Nit removal (Combing)
• Fomite control
• Eye infestation: Baby shampoo or Vaseline;
Ivermectin.

Cutaneous Leishmaniasis
• The leishmaniases are a group of diseases caused by
several species of the genus Leishmania.
• Each species tends to occupy a particular
zoogeographical zone and the disease is endemic in 88
countries.
• It has been estimated that 1.5 million new cases of
cutaneous leishmaniasis occur annually and >80% of
the total of cases are in developing countries.
• Brazil, Iran, Syria, Iraq, Afghanistan and Sudan suffer
the highest prevalence.
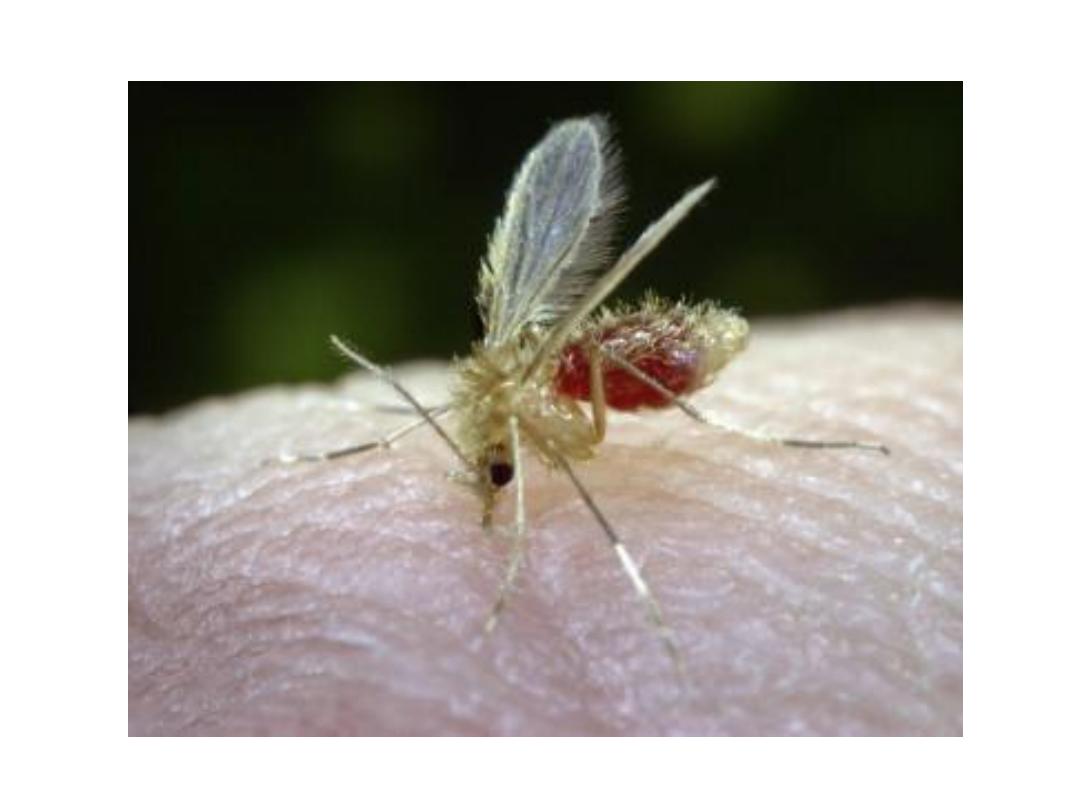
• Leishmania spp. undergo a cycle of development in the
gut of female sandflies, of the genera Phlebotomus in
the Old World.

• In its vertebrate host (Dogs, Gerbils, Humans),
the amastigote form of the parasite is found in
cells of the reticuloendothelial system or in
the dermis following infection.
• It is round or oval, 2–3 µm in diameter, with
no protruding flagellum.
• While in the sandfly and in culture media,
Leishmania spp. are the elongated
promastigote stage, motile with an anterior
flagellum.

Old World cutaneous leishmaniasis
Synonyms
• Oriental sore
• Delhi boil
• Baghdada boil
• Aleppo boil
Cutaneous leishmaniasis of the Old World is due to L. major, L. tropica,
L. aethiopica and L. donovani infantum.
Pathogenesis
• Sandflies inoculate the infective promastigotes when taking a blood meal
into the dermis, then promastigotes are taken up by histiocytes, in which
they multiply.
• Only a minority of parasite inoculations result in localized or disseminated
cutaneous leishmaniasis.
• After a period of time, the overlying epidermis becomes hyperkeratotic
and breaks down, causing an ulcer covered with a crust.

Clinical features
• The incubation period is usually measured in
months, but ranges from a few days to over a
year.
• One or more lesions occur on unclothed body
parts, particularly the face, neck and arms.
• The natural history of the lesions caused by
the four spp. is different but there is much
overlap and the sequence of nodule, crusting,
ulceration and healing with scar formation is
common to all.
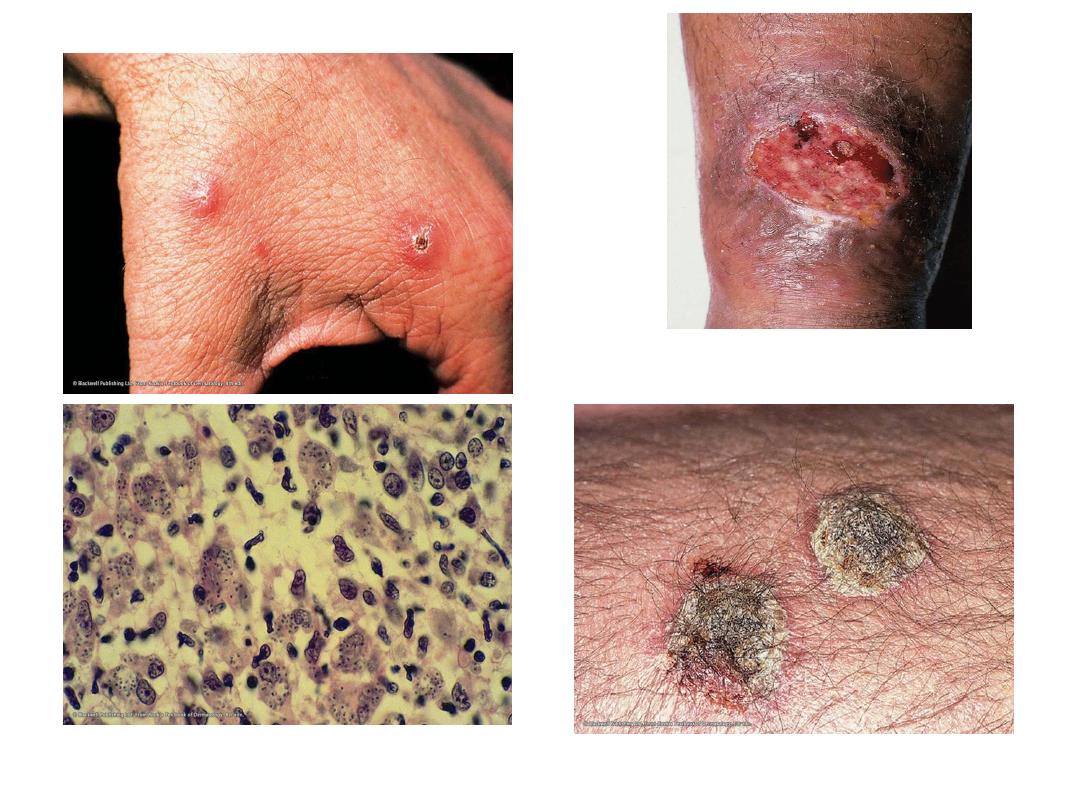

Diagnosis
• History of travel (or living) to an endemic area in the
previous weeks or months.
• History of insect (sandfly) bites in the previous weeks
or months.
• History of high-risk activities such as sleeping outdoors.
• Non-healing chronic nodular, violaceous ulcer for 4–6
weeks or longer.
• Demonstration of amastigotes in Giemsa-stained
smears from infected skin by direct microscopy.
• Demonstration of intracellular amastigotes in the
dermis of H & E skin sections.
• Growth of promastigotes in Nicolle–Novy–MacNeal
(NNN) culture medium from lesional specimens
• Demonstration of leishmanial DNA by PCR.

Treatment
• Try topical treatment methods for simple
sores.
• Reserve the systemic use of pentavalent
antimonials for problematic sores: these
include:
1. Sores where scarring would be disabling or
severely disfiguring.
2. Sores that will not heal easily (on shin or over
a joint).
3. Sores involving mucosa or cartilage.

• Weekly intralesional sodium
stibogluconate PLUS daily oral
itraconazole 100 mg (or allopurinol) for 6
to 8 weeks.
• IM sodium stibogluconate in a single
daily dose of 20 mg/kg for 15–21 days.
• Severe scarring may require plastic
repair.
• After healing, patients are normally
immune to reinfection with the same
species.
