The Circulatory System
Prof. Dr. Malak A. Al-yawerObjectives
The common structural plan seen in most components of the cardiovascular system, and how their common structure is modified and adapted to fulfill different functions in these different parts of the cardiovascular system.The structure of the heart, arteries and veins, how to recognise the different types of arteries, veins, and capillaries, and the essential differences are between arteries and veins.
The structure of three different types of capillaries, and how their structure is related to their function.
The circulatory system
Lymphatic vascular systemsBlood vascular systems
There are two major components of the circulatory system
The cardiovascular systemThe lymph vascular system
HEART
ARTERIES
ARTERIOLES
CAPILLARIES
VENULES
VEINS
1. blind ended lymphatic capillaries that collect lymph fluid from tissues
2. larger lymphatic vessels that connect with one and other and finally empty collected lymph into large veins in the neck where the lymphatic and cardiovascular systems merge.
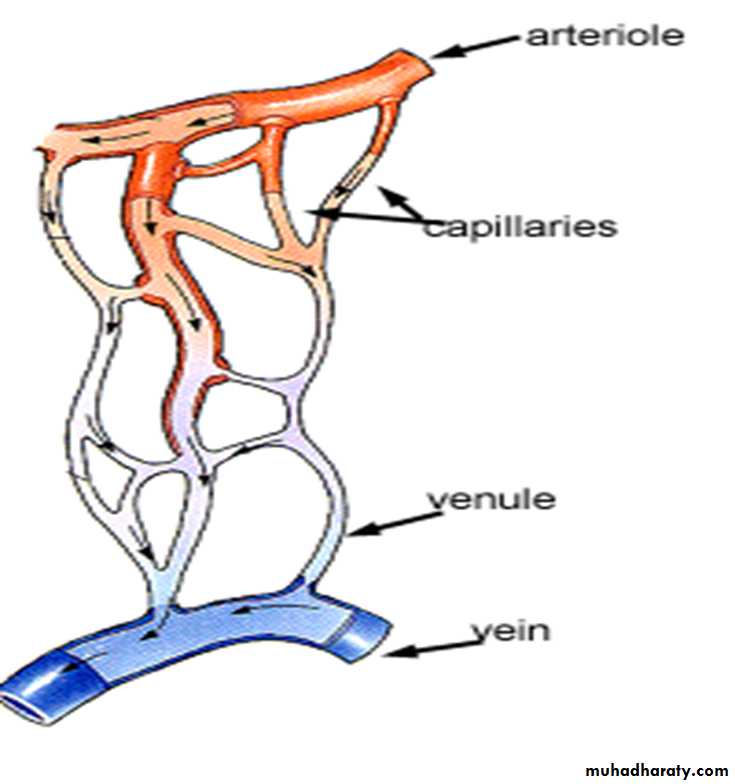
The cardiovascular system is divided into
the macrovasculaturethe microvasculature
vessels that are more than 0.1 mm in diameter
large arterioles,
muscular arteries
elastic arteries
muscular veins
visible only with a microscope
arterioles,capillaries, and
postcapillary venules
The microvasculature is particularly important as the site of interchanges between the blood and surrounding tissues under normal conditions and in the event of inflammatory processes.
The vascular wall
is composed of three basic structural constituents:The amount and arrangement of these tissues within the blood circulatory system are influenced by
• the endothelium,
• the muscular tissue, and
• the connective tissue, which includes elastic elements
mechanical factors(blood pressure), and
metabolic factors (reflect the local needs of the tissues).
These tissues are all present in different proportions in the vascular wall, except for capillaries and postcapillary venules( the only structural elements represented are the endothelium, its basal lamina, and pericytes).
Endothelium
Single layer of a squamous epithelium
functions of endothelial cells
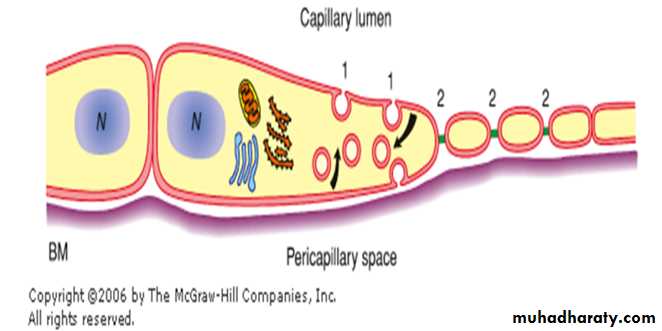
They are flat polygonal cells connected to each other by junctional complexes.They have numerous pinocytotic vesicles V and specialised membrane-bound organelles called Weibel-Palade bodies WP which store Von Willebrand factor.
Synthesise collagen and proteoglycans for basement membrane maintenance.
Synthesise and secrete molecules which promote protective thrombus formation, e.g. von Willebrand factor (Factor VIII).Synthesise and secrete molecules which minimise pathological thrombus formation, e.g. prostacyclin, thrombomodulin, nitrous oxide (which inhibits platelet adhesion and aggregation).
Secrete vasoactive factors controlling blood flow, e.g. nitrous oxide, prostacyclin, vasoactive peptides such as endothelin.
Produce molecules which mediate the acute inflammatory reaction, e.g. interleukins 1, 6 and 8, cell adhesion molecules.
Produce some growth factors, e.g. fibroblast growth factor, platelet-derived growth factor, blood cell colony stimulating factor.
Vascular Smooth Muscle
Present in all vessels except capillaries and pericytic venules.Arranged in helical layers in the tunica media of the blood vessels.
Each muscle cell is enclosed by a basal lamina and by variable amounts of connective tissue.
Frequently connected by communicating (gap) junctions
Vascular Connective Tissue
Collagen fiber:
–Collagen IV basement membranes
–Collagen III tunica media
–Collagen I adventitia
Elastic fibers
–Predominate in large arteries
Ground substance
–Contributes to the physical properties of the walls of the vessels
–The concentration of glycosaminoglycans is higher in arterial than in venous tissue.
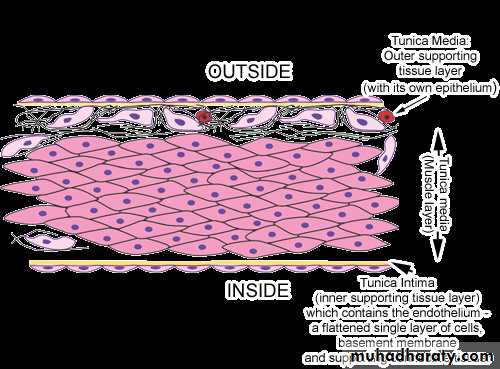
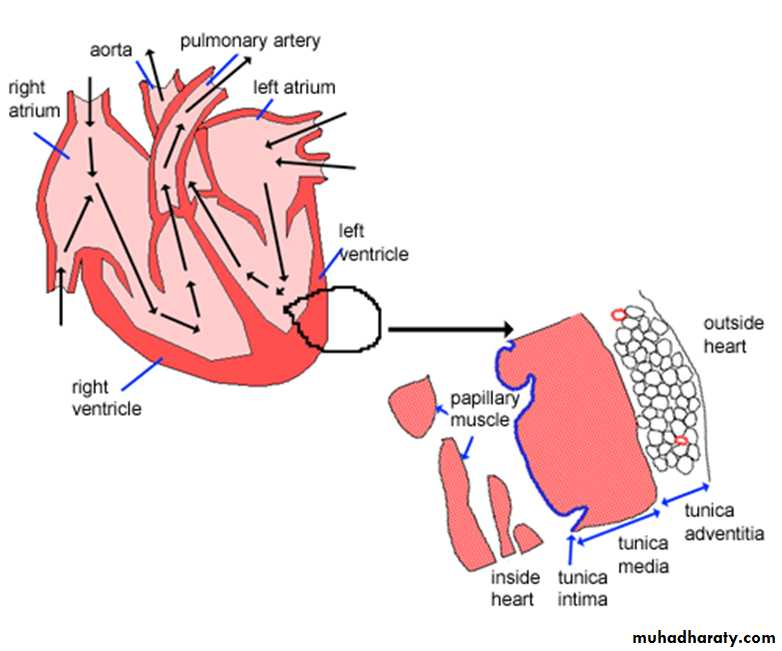
Basic common structureof all the blood vessels (except the capillaries) that make up the cardiovascular system consists of these three layers.
• Tunica intima
• Tunica media• Tunica adventitia
Blood vessels are usually composed of the following layers, or tunics (L. tunica, coat),
• Tunica Intima consists of• A layer of simple squamous epithelium called endothelium
• subendothelial layer of loose connective tissue containing occasional smooth muscle cells.
• internal elastic lamina (separating the intima from the media) present in some blood vessels .
• composed of elastin,
• has gaps (fenestrae) that allow the diffusion of substances to nourish cells deep in the vessel wall.
• generally has an undulating appearance in tissue sections(the absence of blood pressure and the contraction of the vessel at death).
2. Tunica Media
consists primarily ofconcentric layers of helically arranged smooth muscle cells.
variable amounts of elastic fibers and lamellae, reticular fibers (collagen type III), proteoglycans, and glycoproteins which interposed among smooth muscle cells . Smooth muscle cells are the cellular source of this extracellular matrix.
In arteries, the media has a thinner external elastica lamina, which separates it from the tunica adventitia.
3. Tunica Adventitia
This is the outermost coat. It consists of• a simple squamous epithelium,
• basement membrane,
• connective tissue collagen and elastic fibers . Collagen in the adventitia is type I.
• blood vessels, and
• sometimes smooth muscle cells.
The adventitial layer gradually becomes continuous with the connective tissue of the organ through which the vessel runs.
Vasa Vasorum("vessels of the vessel")
Large vessels usually have vasa vasorum, which are arterioles, capillaries, and venules that branch profusely in the adventitia and the outer part of the media. The vasa vasorum provide metabolites to the adventitia and the media, since in larger vessels the layers are too thick to be nourished solely by diffusion from the blood in the lumen.They are more frequent in veins than in arteries.
ArteriesThere are three main types of arteries:
• Elastic arteries• Muscular arteries
• Arterioles
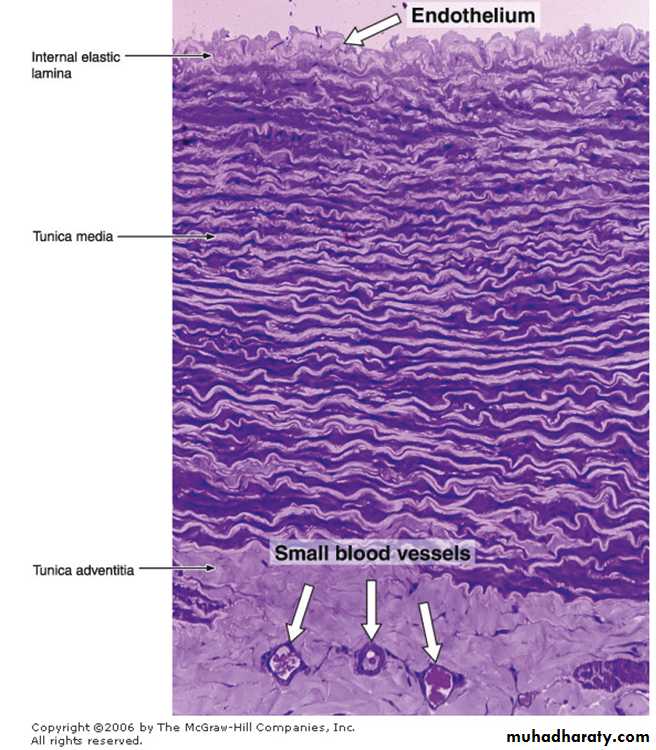
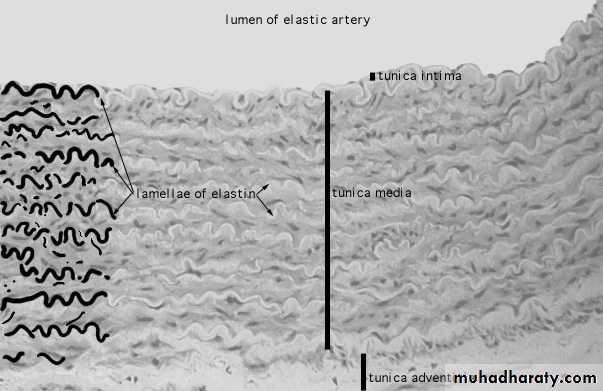
Large Elastic Arteriesinclude the aorta and its large branches.
They have a yellowish color from the accumulation of elastin in the media.The intima is thicker than the corresponding tunic of a muscular artery. An internal elastic lamina, although present, may not be easily discerned, since it is similar to the elastic laminae of the next layer.
The media consists of elastic fibers and a series of concentrically arranged, perforated elastic laminae whose number increases with age (there are 40 in the newborn and 70 in the adult). Between the elastic laminae are smooth muscle cells, reticular fibers, proteoglycans, and glycoproteins.
The tunica adventitia is relatively underdeveloped
Medium (Muscular) Arteries
The intima have a subendothelial layer that is somewhat thicker than that of the arterioles. The internal elastic lamina, the most external component of the intima, is prominent, andthe tunica media may contain up to 40 layers of smooth muscle cells. These cells are intermingled with various numbers of elastic lamellae (depending on the size of the vessel) as well as reticular fibers and proteoglycans, all synthesized by the smooth muscle fibers. An external elastic lamina, the last component of the media, is present only in the larger muscular arteries.
The adventitia consists of connective tissue. Lymphatic capillaries, vasa vasorum, and nerves are also found in the adventitia, and these structures may penetrate to the outer part of the media.
small muscular artery
the diameter is approximately 0.5 to 2 mm anda thin but distinct internal elastic lamina is present
but there is usually little or no external elastic lamina.
The tunica media has 3-10 concentric layers of smooth muscle and contains almost no elastic fibres.
the tunica adventitia is very thin.
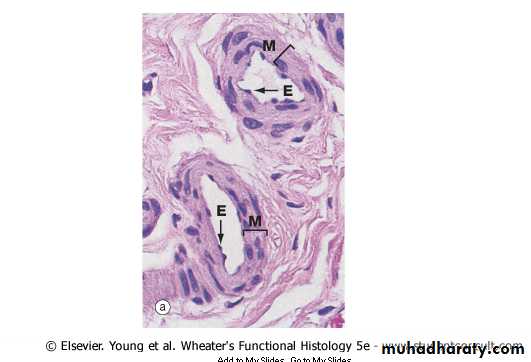
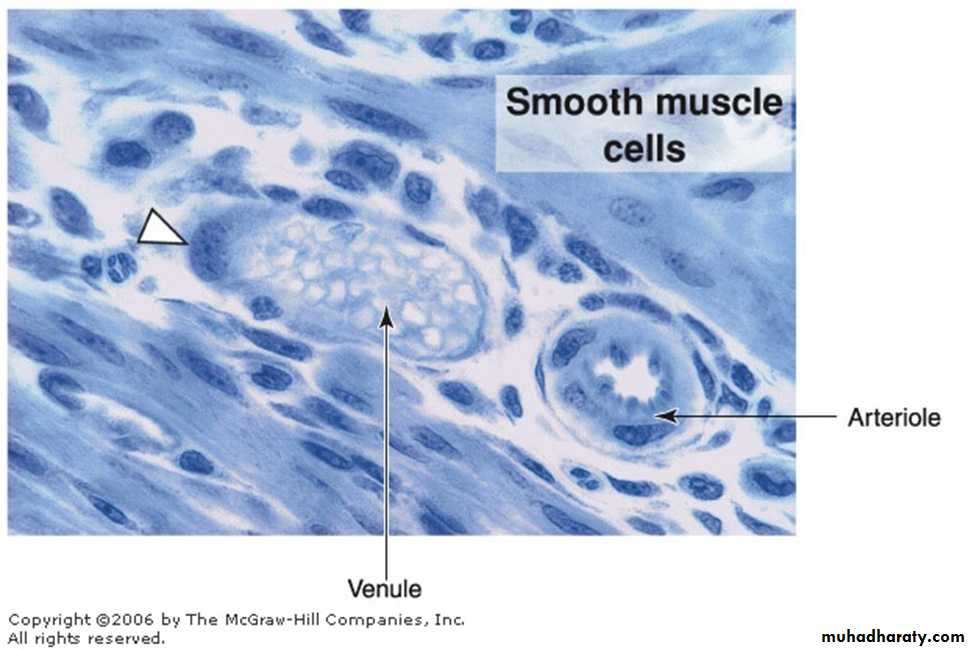
Arterioles
The arterioles are generally less than 0.5 mm in diameter and have relatively narrow lumens.The subendothelial layer is very thin. In the very small arterioles, the internal elastic lamina is absent, and
the media is generally composed of one or two circularly arranged layers of smooth muscle cells; it shows no external elastic lamina.
the tunica adventitia is very thin.
Small muscular arteries give way to large arterioles, which eventually become small arterioles. These transitions are gradual, with no sharp demarcations, and involve loss of the internal elastic lamina, and progressive reduction of the number of muscle layers in the media. The adventitia is thin and merges imperceptibly with surrounding supporting collagenous fibrous tissue.
Capillaries
usually 7-9 um in diameter, but may be as small as 5 um or as large as 12 um in diameter (sinusoidal capillaries may be larger)Capillaries
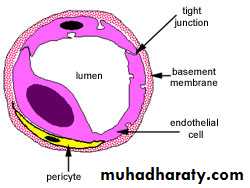
Its wall consists of a simple squamous epithelium called endothelium.surrounded by a basal lamina.
cells called pericytes may be sporadically found between the basal lamina and the endothelial cells.
Pericytes
are cells of mesenchymal origin with long cytoplasmic processes that partly surround the endothelial cells at various locations along capillariesThe presence of myosin, actin, and tropomyosin in pericytes strongly suggests that these cells also have a contractile function.
After tissue injuries, pericytes proliferate and differentiate to form new blood vessels and connective tissue cells, thus participating in the repair process.
They have their own basal lamina which may fuse with the basal lamina of the endothelial cells that form the capillary wall.
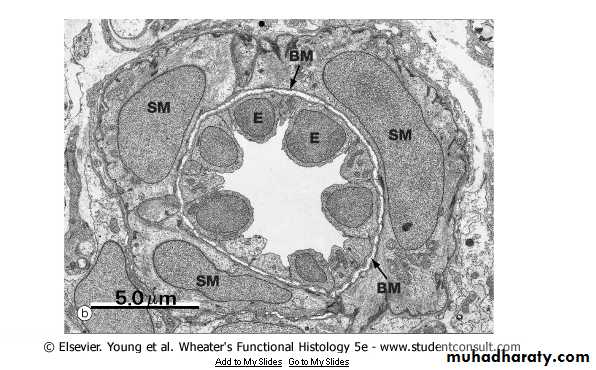
Capillaries
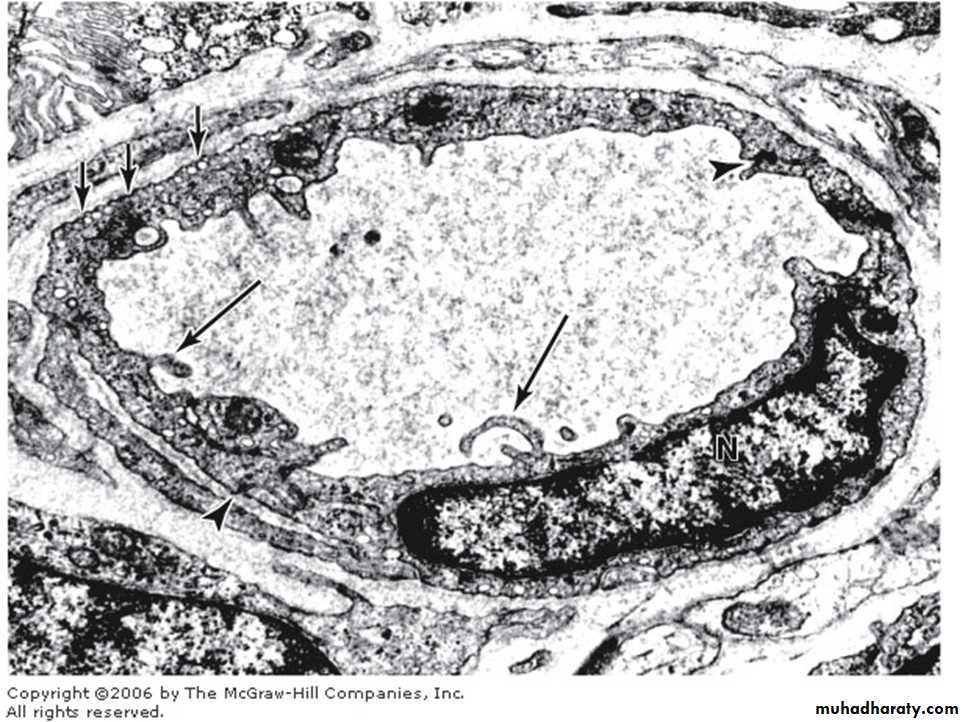
In transverse (cross-) sections we find that the circumferential wall of a capillary is generally formed by 2-3 squamous cells held together by occluding or gap junctions. Nuclei of the cells buldge into the capillary lumen.
Capillaries
can be grouped into three types, depending on the continuity of boththe endothelial sheet and
the basal lamina.
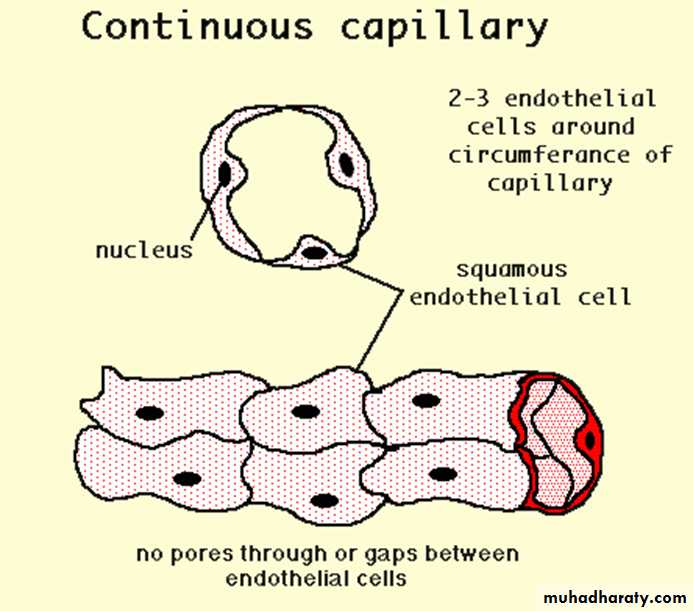
1. The continuous, or somatic, capillaries
are characterized by the absence of fenestrae in their wall.most capillaries are of this type. They are found in all types of muscle tissue, connective tissue, exocrine glands, and nervous tissue.
The continuous capillaries
In some places, but not in the nervous system, numerous pinocytotic vesicles are present on both surfaces of endothelial cells.Pinocytotic vesicles appear as isolated vesicles in the cytoplasm of these cells. They can also fuse forming transendothelial channels, responsible for the transport of macromolecules in both directions across the endothelial cytoplasm.
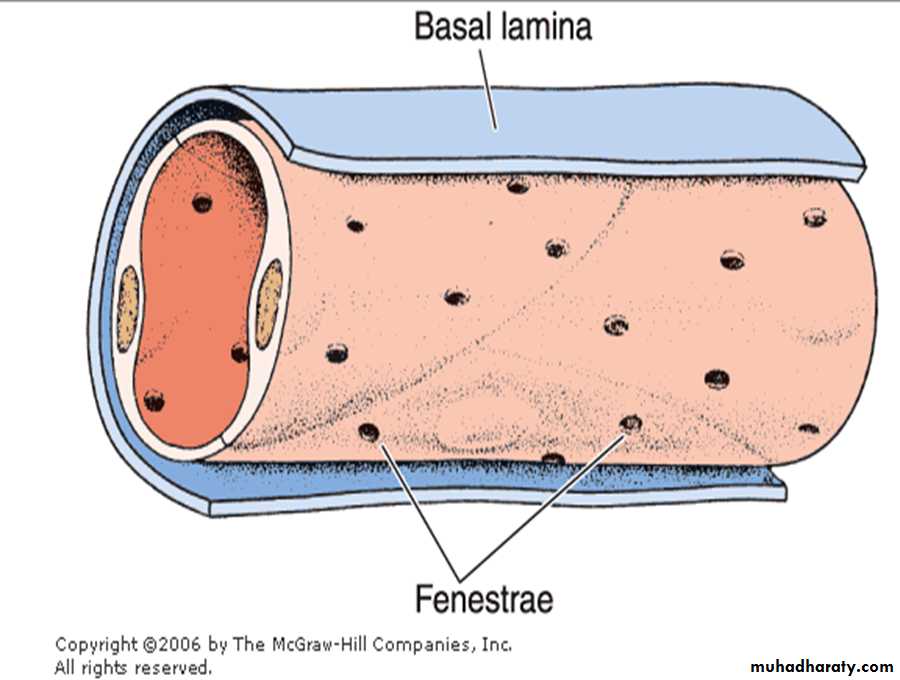
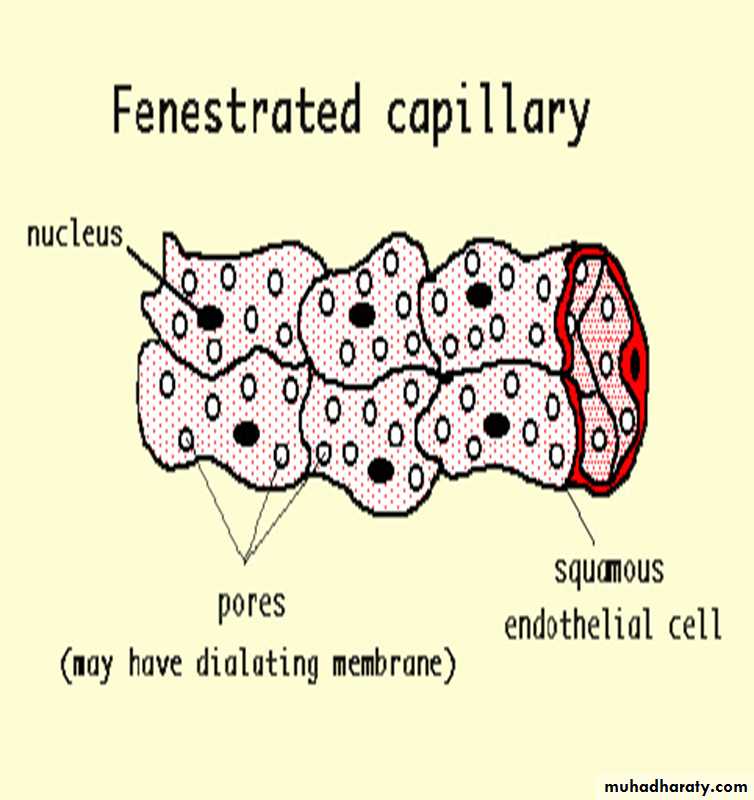
2. The fenestrated, or visceral,capillaries
These are found in some tissues where there is extensive molecular exchange with the blood such as the small intestine, endocrine glands and the kidney. The 'fenestrations' are pores that will allow larger molecules though.These capillaries are more permeable than continuous capillaries.
are characterized by the presence of several circular transcellular openings in the endothelium membrane called fenestrae.
The fenestrated, or visceral,capillaries
Fenestrae are limited by the cell membrane, resulting in a continuous cell membrane channel from the blood front to the tissue front. Each fenestra is obliterated by a diaphragm that is thinner than a cell membrane
The diaphragm does not have the trilaminar structure of a unit membrane. The exact chemical nature of the diaphragm is still unknown. The hydrophobic barrier may be absent in these diaphragms. The basal lamina of the fenestrated capillaries is continuous.
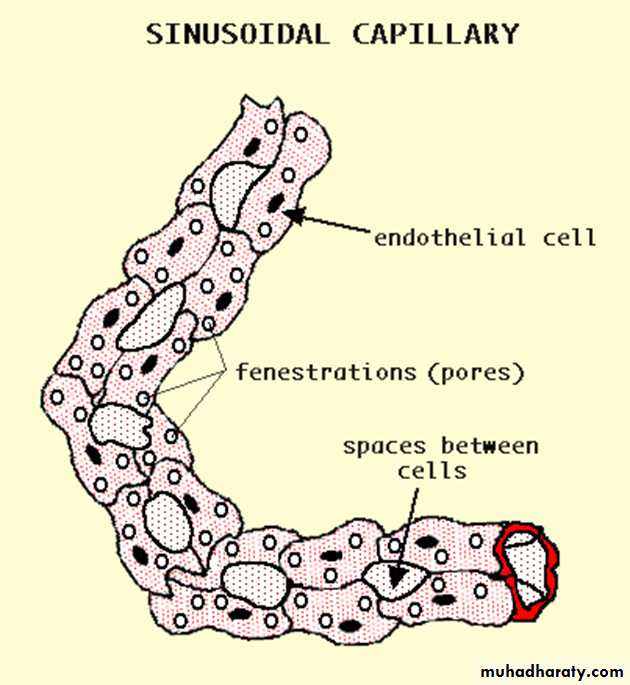
3. The discontinuous sinusoidal capillaries,
have the following characteristics:a. The capillaries have a tortuous path and greatly enlarged diameter (30-40 micrometer), which slows the circulation of blood.
b. The endothelial cells form a discontinuous layer and are separated from one another by wide spaces.
c. The cytoplasm of the endothelial cells has multiple fenestrations without diaphragms.
d. Macrophages are located either among or outside the cells of the endothelium.
e. The basal lamina is discontinuous.
Sinusoidal capillaries are found mainly in the liver and in hematopoietic organs such as the bone marrow and spleen. The interchange between blood and tissues is greatly facilitated by the structure of the capillary wall.
venules
1. 0.2 - 1 mm in diameter2. intima lacks a subendothelial layer of connective tissue
3. thin media consisting of a few smooth muscle fibers (collecting venules). As venule size increases, the amount of muscle increases (muscular venules).4. well developed adventitia rich in collagen fibers.
5. despite tunic investments, blood cells such as moncytes can still pass through the walls of venulessmall or medium-sized veins
From venules, the blood is collected in veins of increased size, arbitrary classified as small, medium, and large.The majority of veins are small or medium-sized, with a diameter of 1-9 mm.
The intima usually has a thin subendothelial layer, which may be absent at times.
The media consists of small bundles of smooth muscle cells intermixed with reticular fibers and a delicate network of elastic fibers.
The collagenous adventitial layer is well developed.
Large veins
The big venous trunks, close to the heart, are large veins.
Large veins
Have a well-developed tunica intima,
the media is much thinner, with few layers of smooth muscle cells and abundant connective tissue.
The adventitial layer is the thickest and best-developed tunic in veins; it frequently contains longitudinal bundles of smooth muscle .
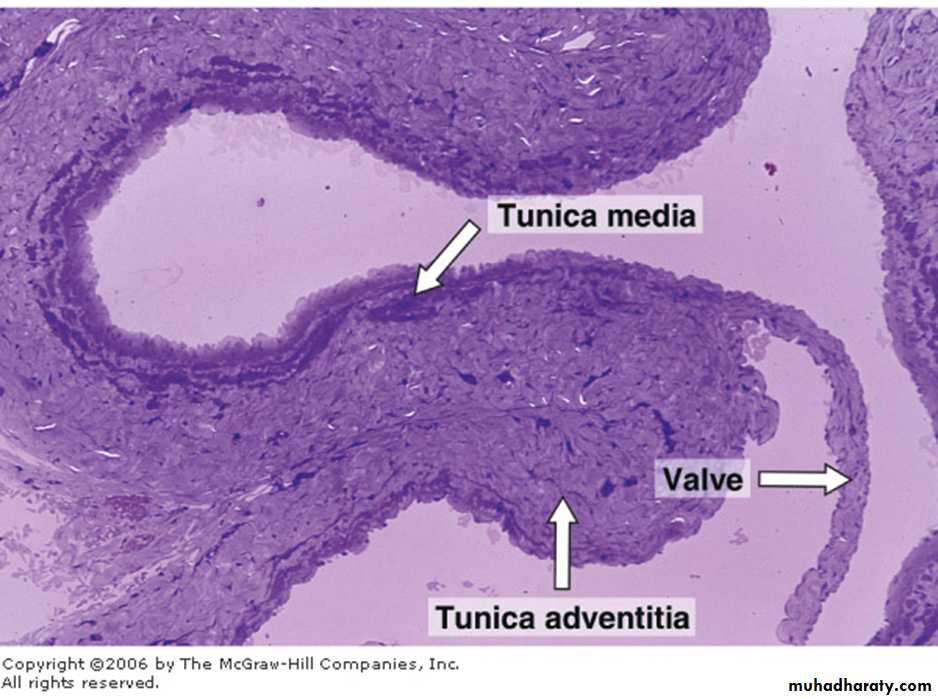
These veins, particularly the largest ones, have valves in their interior .
The venous valves
consist of 2 semilunar folds of the tunica intima that project into the lumen.
They are composed of connective tissue rich in elastic fibers and are lined on both sides by endothelium.The valves, which are especially numerous in veins of the limbs, direct the venous blood toward the heart.
Heart
A. The heart is composed of1. 3 layers or tunics
a. endocardium
b. myocardium
c. epicardium
2. a fibrous connective tissue skeleton
3. valves
4. an electrical impulse conducting system
endocardium
in a sense, simply a continuation of tunica intimaconsists of 3 parts
* endothelium resting on a basal lamina and associated thin layer of collagen fibers
* a deeper, denser layer of connective tissue containing elastic fibers and a few smooth muscle cells
* the subendocardial zone of loose connective tissue that contains small blood vessels and nerves. In the ventricle, the subendocardial zone may contain scattered Purkinje fibers
Myocardium – consists of 2 components
a. fascicles of cardiac muscle cells that connect to the fibrous connective tissue skeleton of the heartb. non-contactile, modified muscle cells that form the impulse generating and conducting system of the heart. Purkinje fibers (in the ventricle) are scattered along the innermost portion of the myocardium, next to the endocardium
Epicardium (visceral pericardium)
– epithelium and connective tissue covering of hearta. squamous to cuboidal epithelial external lining - a continuation of the epithelium that lines the pericardial cavity
b. below this is a layer of connective tissue with high concentration of elastic fibers
c. between the elastic layer and myocardium is the subepicardial layer that consists of loose connective tissue containing nerves, veins, and adipose tissue.
The fibrous skeleton of the heart
is composed of dense connective tissue with thick collagen fibers oriented in various directions.Septum membranaceum
Trigona fibrosa
Annuli fibrosi.
The cardiac valves
consist of a central core of dense fibrous connective tissue containing both collagen and elastic fibersLined on both sides by endothelial layers.
The bases of the valves are attached to the annuli fibrosi of the fibrous skeleton.
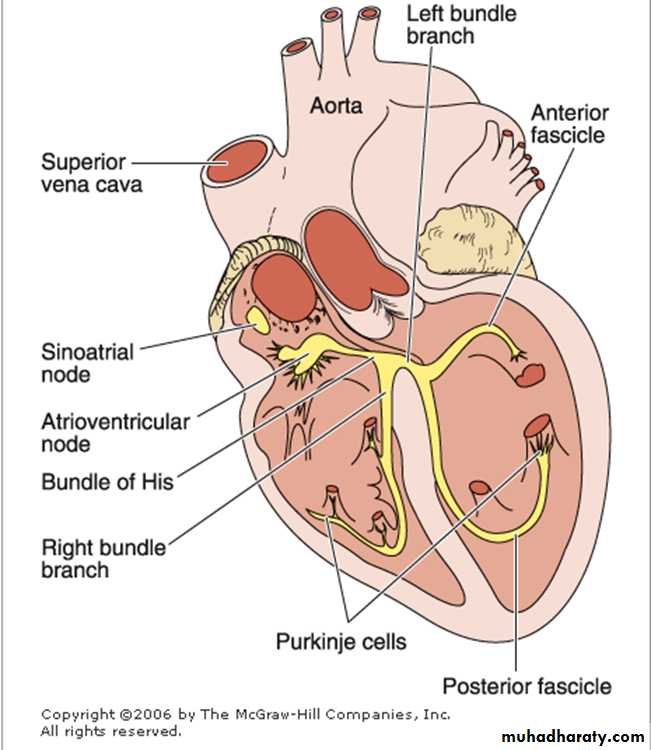
The conducting system of the heart
A specialized system to generate a rhythmic stimulus that is spread to the entire myocardium.1. Sino-atrial node.
2. Atrio-ventricular node.
3. Atrio-ventricular bundle.
4. Right and left bundle branches.
5. Purkinje cells larger than ordinary cardiac muscle cells and acquire a distinctive appearance.
•Have one or two central nuclei
•Their cytoplasm is rich in mitochondria and glycogen.
•The myofibrils are sparse and are restricted to the periphery of the cytoplasm
lymphatic vessels
System of thin walled vessels that runs throughout the body.These vessels are lined with endothelium.
They begin with blind-ended lymphatic capillaries that originate in connective tissue of nearly all parts of body.These lymphatic capillaries and associated small lymph vessels converge into larger vessels that return fluid expressed from arteries and veins into tissues to the venous component of the blood circulatory system.
The lymph vessels carry fluid that eventually drains into 2 large ducts, the thoracic duct and the smaller right lymphatic duct that connect to large veins in the neck.
Larger lymphatic vessels are similar in structure to veins except with thinner walls and with no clear-cut separation between the 3 tunics (intima, media, adventitia).
The lymph vessels are also a pathway by which various cells of the immune system can enter or leave the blood circulatory system and tissues.