Pleural Disease
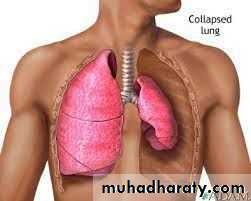
PneumothoraxClassification
• Spontaneous
• PSP
• SSP
• Acquired
• Blunt trauma
• Penetrating trauma
• Barotrauma
• Iatragenic injury
Pathophysiology
• Primary Spontaneous Pneumothorax (PSP)
• Young men (teens – mid 20s)• Tall and thin
• Families
• Smokers
• Secondary Spontaneous Pneumothorax (SSP)
• Older people (45 – 64 years)
• Pre-existing lung disease
• Higher incidence of respiratory failure
• Higher mortality rate
Clinical presentation
1. Asymptomatic2. Symptomatic
• a. Pain (PSP)• b. Dyspnea (SSP)
• c. Orthopnea, hemoptysis, cough
On examination
Inspection: Dyspnea ± cyanosis
• Decrease or absence chest wall movement
Palpation: Apex shifted to the other side
• Trachea shifted to the other side
• Decreased chest wall expansion
• Decreased or absent tactile vocal fremitus
Percussion: Hyper-resonance (tympanic)
Auscultation: Decrease or absent breath sounds
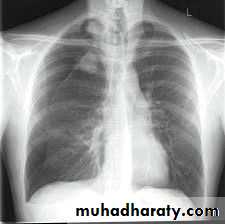
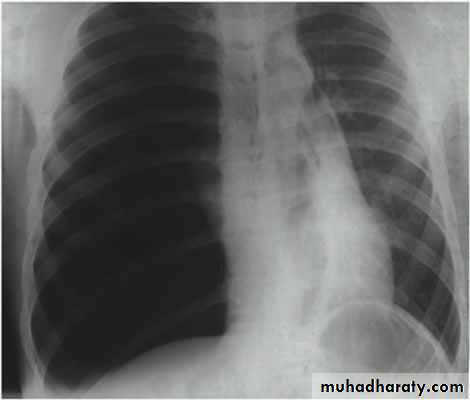
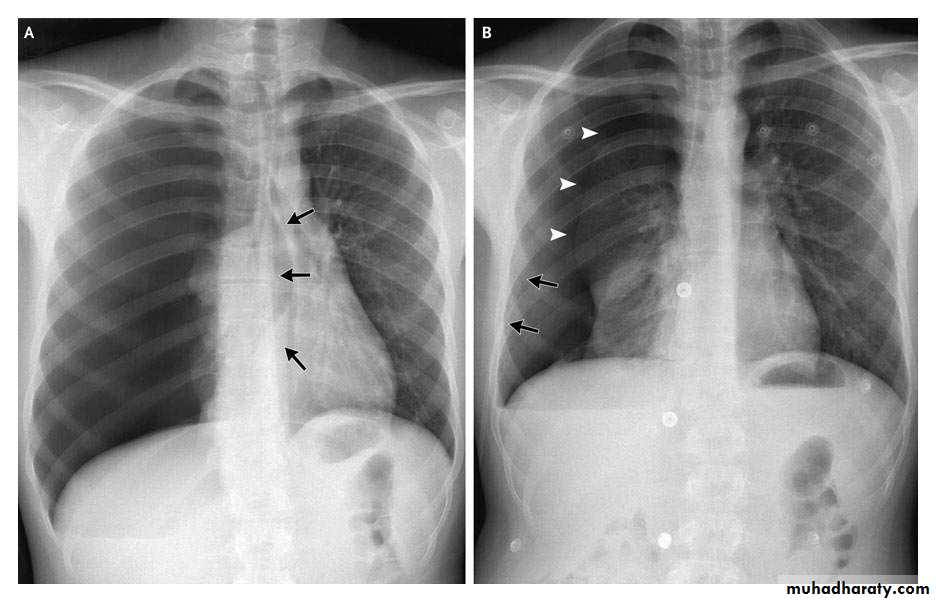
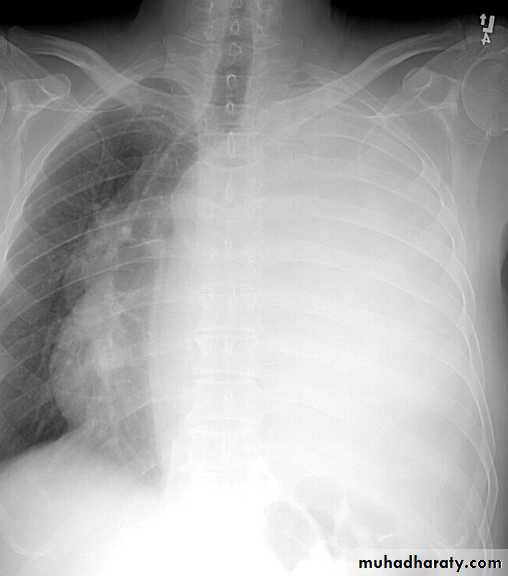
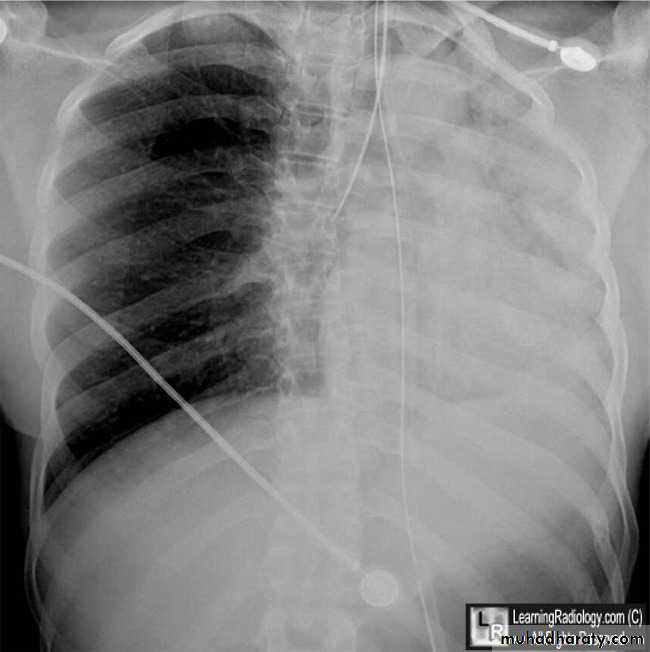
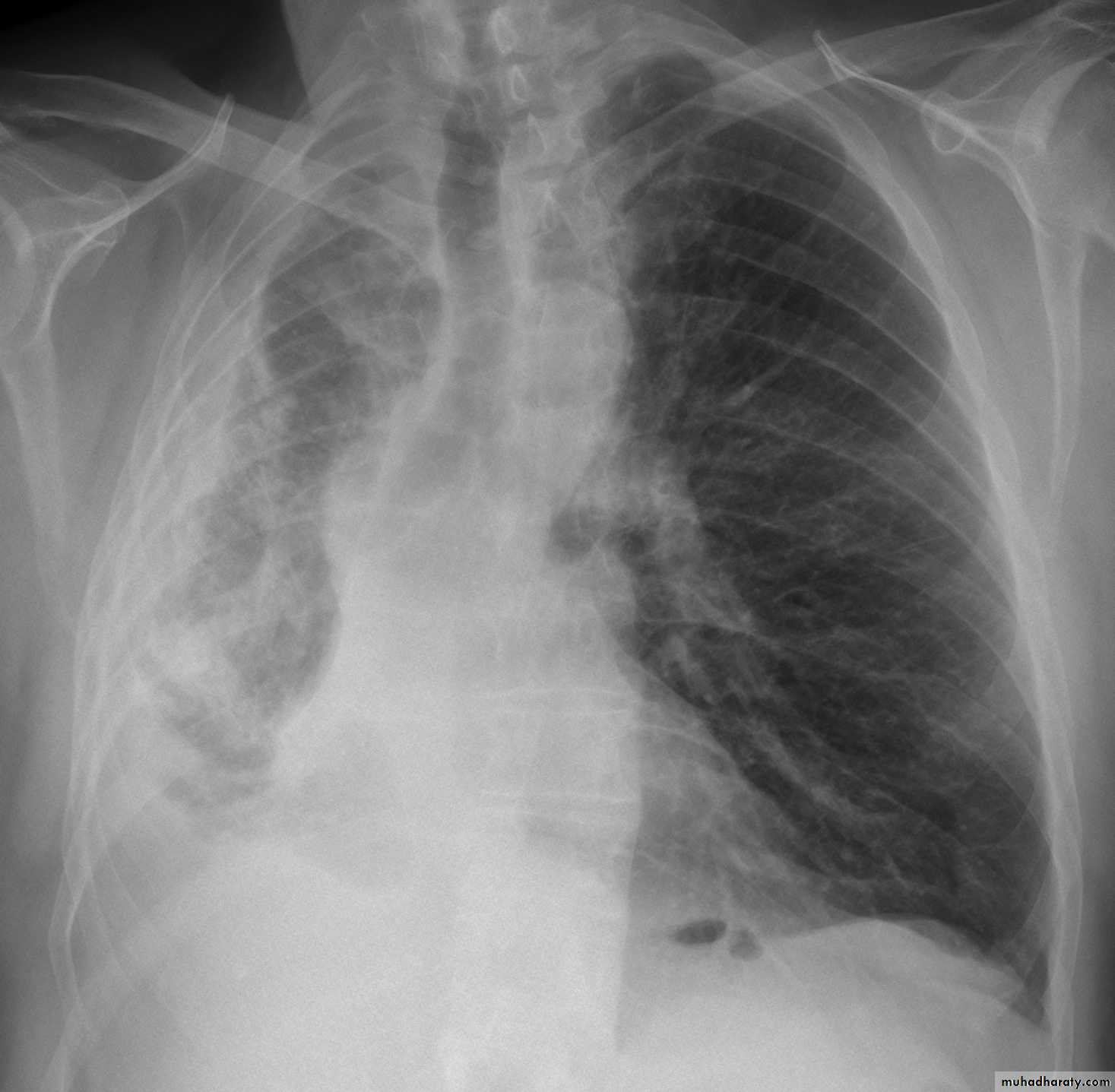
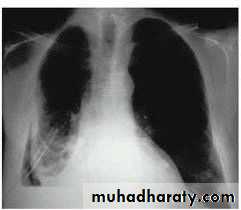
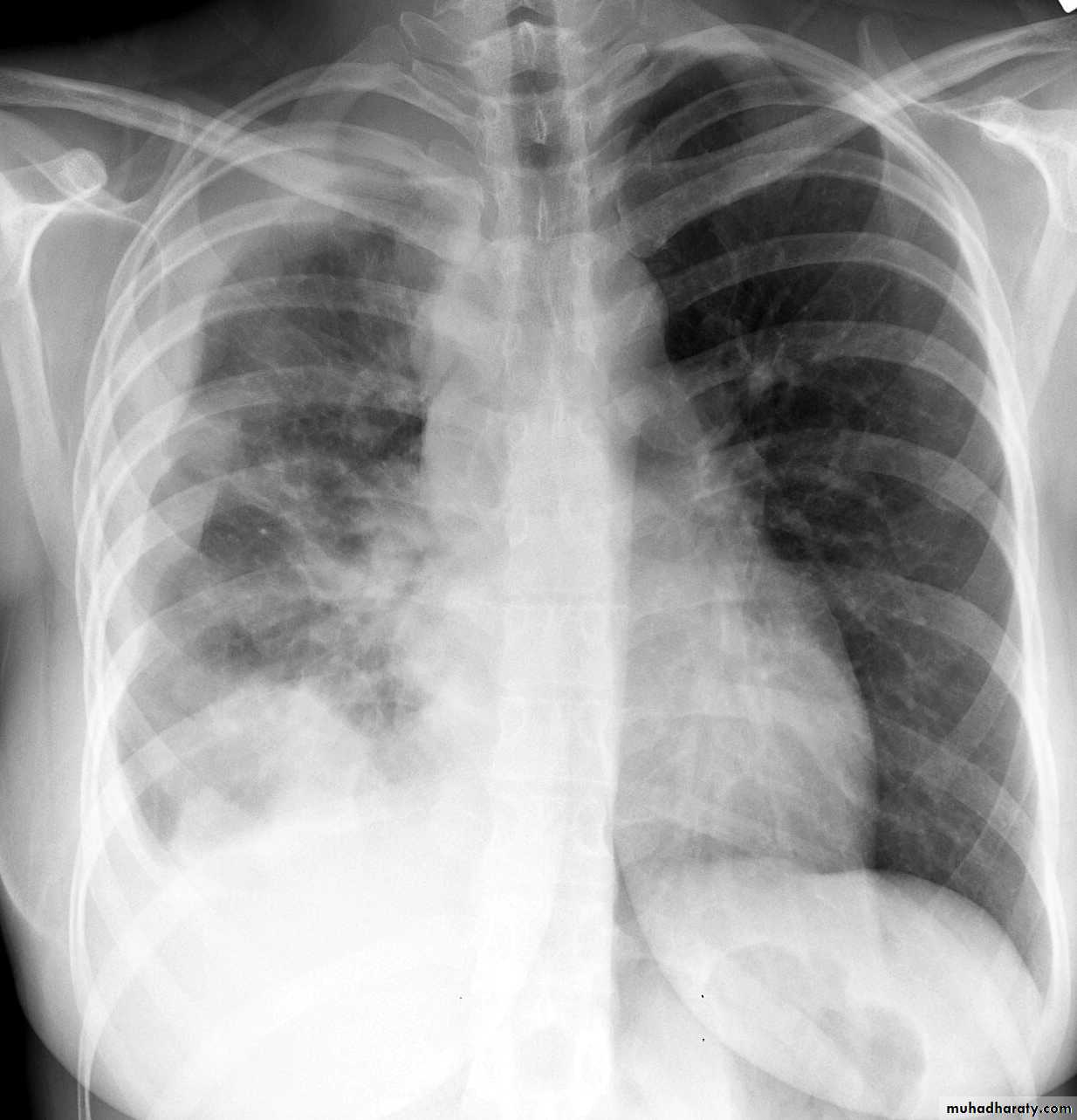
CXR:
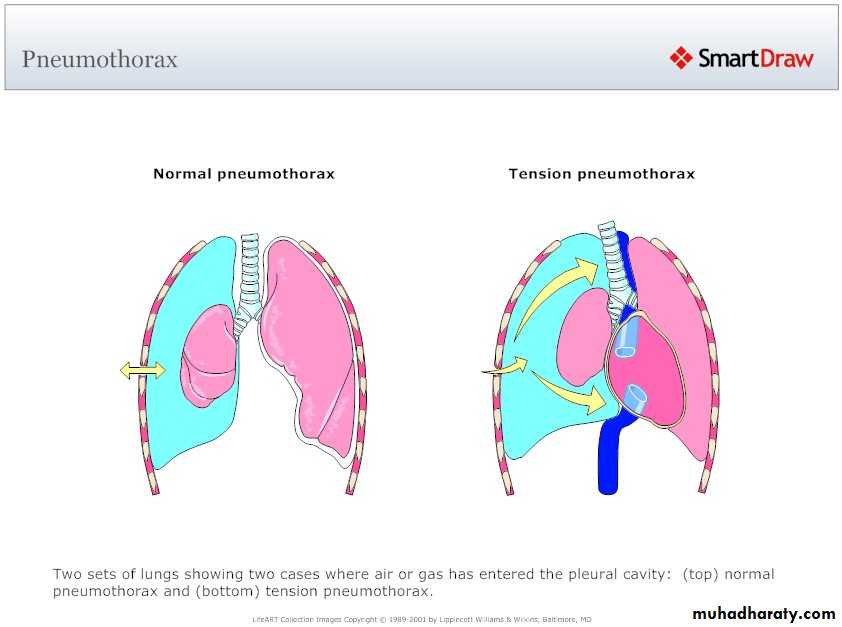
closed Pneumothorax
Tension Pnenmothorax
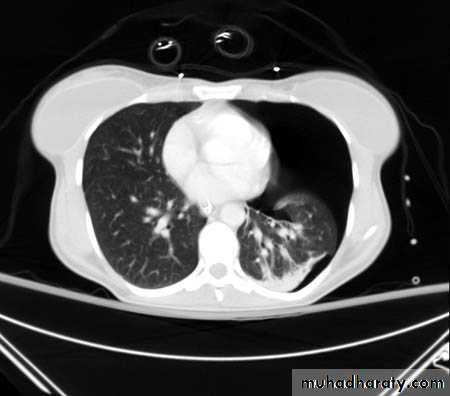
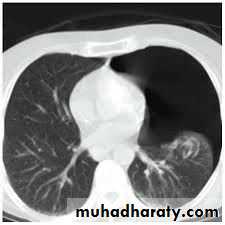
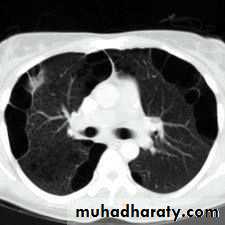
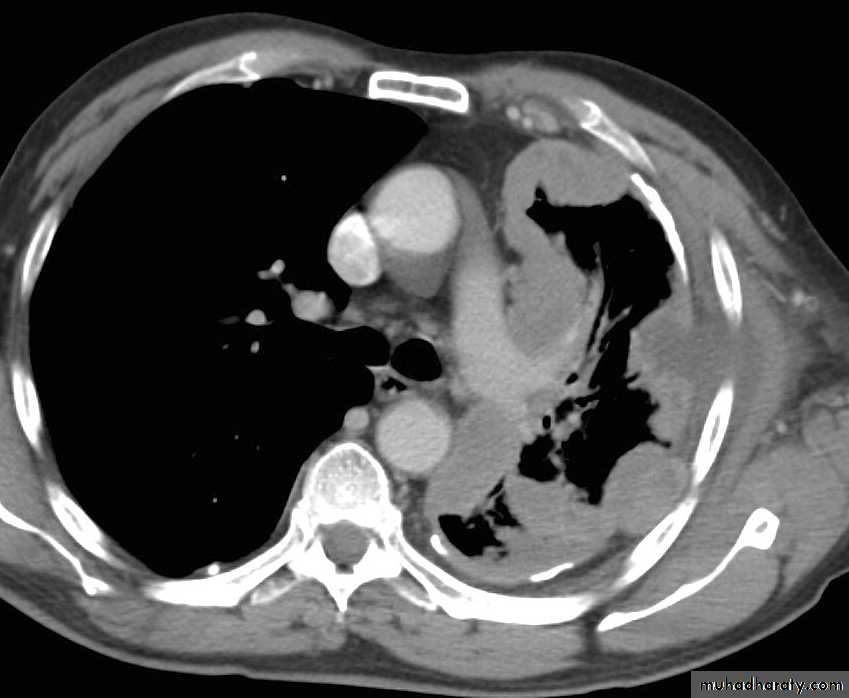
What is the difference??CT scan
BronchoscopyPneumothorax
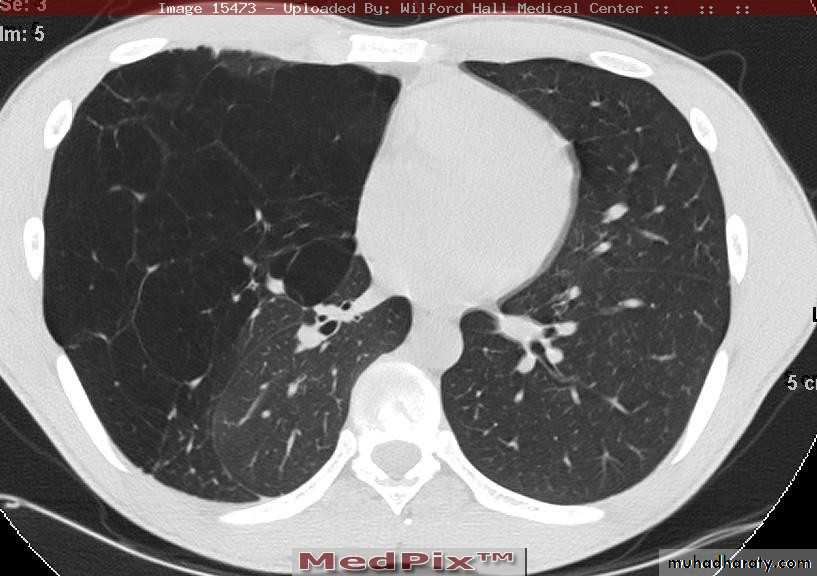
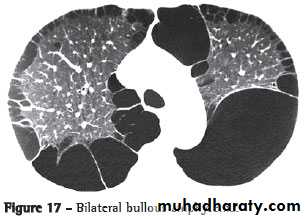
Emphysema
Complications• Pleural effusion
• Hemothorax due to torn pleural adhesions
• Empyema
• Trapped lung (fibrothorax) due to failure of re-expansion
• Tension pneumothorax
Treatment
• Observation• Pleurocenthesis or thoracocenthesis
• Chest tube thoracostomy
• Surgery
• Massive air leak
• Persistent air leak
• Recurrent pneumothorax
• Bilateral pneumothorax
• Previous pneumonectomy
• Occupational hazard
• Pleurodesis
Malignant pleural effusion
Causes
• lung cancer
• pleural malignancy
• mediastinal LN malignancy
Treatment of pleural effusion→physician or oncologist
• When to reffer to a surgeon →recurrent &/or a suspicion of being a malignant effusionWhy reffer →biopsy + prevent reccurence of effusion
Biopsy:• Cytology of pleural effusion
• Abram's needle
• CT or U/S guided biopsy
• VATS biopsy
• Open biopsy
Prevent recurrence
• Repeated thoracocenthesis• Chemical pleurodesis
• Surgical pleurodesis/pleurectomy
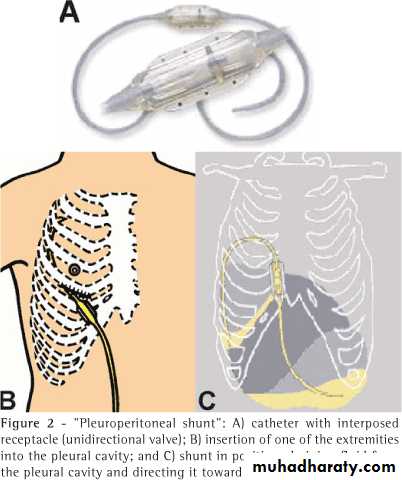
• Pleuro-peritoneal shunt (Denver's shunt)
Denver’s Shunt
What is the difference??
Massive effusion
Whole lung atelectasisEmpyema
Causes:• Complication of pulmonary infection
• Following chest trauma
• Extrapulmonary spread
• Complication of pneumothorax
• Non sterile aspiration of pleural fluid
Pathogenesis
1. Acute or exudative phase
Thin pus, Thin pleura, Expandable lungs
Antibiotics and drainage
2. Transitional or fibrinopurulent phase
Pus thicker, fibrin deposition, lung less expandable
Antibiotics and drainage
3. Chronic or organization phase
Thick pus, thick pleura with fibrous coat, non expandable lungs
Surgery (decortication)
Clinical presentation
• fever, maliase, anorexia, weight loss• pleuretic chest pain
• dyspnea, cough, purulent sputum
O/E: signs of infection + signs of pleural effusion
Investigations:
• CXR• Thoracocenthesis
• CT scan
CXR:
Treatment
Objectives:• Control infection
• Drain purulent material
• Restore lung function
Treatment line
• Chest tube thoracostomy + physiotherapy• Decortication / pleurectomy
• Open drainage e.g., Eloesser's flap
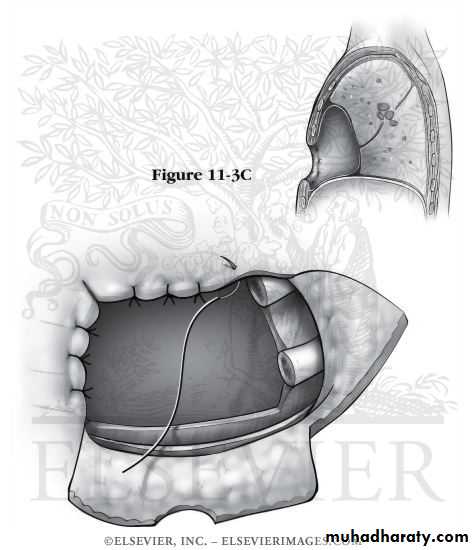
Decortication
• Eloesser’s flap
ChylothoraxEtiology:
Disruption or tear in the thoracic duct during its coarse in the chest.
• Trauma including penetrating, blunt or iatrogenic injury
• Neoplasm with invasion of the thoracic duct• Infection
Clinical presentation
• Dyspnea, orthopnea, and cough• Malnutrition
• Dehydration
• Decreased immunity
Investigations:
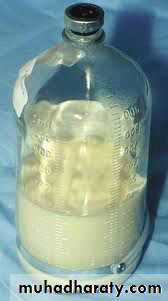
• 1. Pleural fluid analysis: odorless milky white appearance with a creamy layer on standing.• 2. Lymphangiography
Treatment
1. Conservative treatmenta. Chest tube drainage
b. Correct dehydration
c. Correct electrolyte imbalance
d. Nutritional support by TPN or fat free oral diet
2. Surgical repair or ligation of thoracic duct
3. Denver's shunt (pleuro-peritoneal shunt)Pleural malignancy
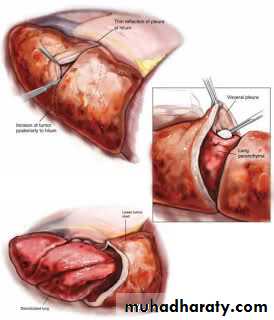
• Primary pleural tumors are rare• The most common primary tumor malignant mesothelioma (usually as a consequence of asbestos exposure).
• Poor prognosis
• Respiratory failure or symptoms of invasion of nearby organ.
• CXR: lung surrounded by thick irregular pleura with multiple nodules with extension to nearby structures.
• Curative treatment is surgery (extrapleural pneumonectomy).
• Both radiotherapy and chemotherapy are weakly effective.