
Mohannad Al-Fallouji
, PhD (London), FRCS, FRCSI
University Staff
and
Consultant Surgeon
Baghdad’s Medical City
Teaching
Hospitals
Director:
www.ihams.org

1992
1986
1998
Speaker’s
Background
خلفية المحاضر

I Love You
(in Hebrew)
2012 - 2013
Magnum Opus

1. To reveal details of Cervical LNs’ Surgical Anatomy.
2. To know the causes of Lymphadenopathy.
3. To handle enlarged Supraclavicular LN management.
4. How to diagnose the Cervical Lymphadenopathy.
5. How to treat Tuberculous Lymphadenopathy.
Objectives of Cervical LNs
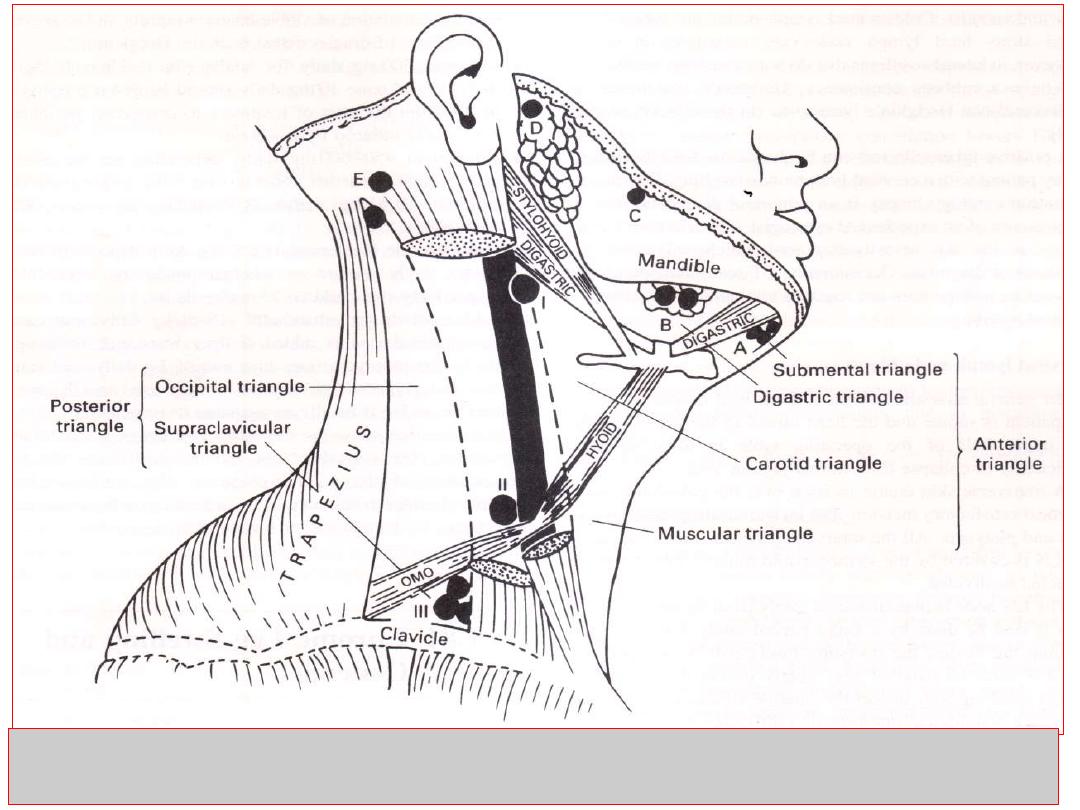
Cervical Lymph Nodes
.

Surgical Anatomy:
Cervical Lymph Nodes:
The human body contains about 800 lymph nodes (LN), of
which 300 are located in the neck.
About 150 are in the Mesentery.
The lymphatic drainage of the head and neck is arranged
into superficial and deep.
The superficial group has 2 'circles‘:
the inner circle
the outer circle.

The Superficial Lymph Nodes
comprise following elements.
Outer circle of nodes from chin to occiput is made up of:
A: The submental nodes:
three or four nodes lie just beneath the chin.
They drain the tip of the tongue. floor of the mouth lingual and labial gum.
They drain into the submandibular group but a few efferents pass direct to the
jugulo-omohyoid node.
B: The submandibular nodes
drain a wide area from the centre of the
forehead. nose and nearby cheek. upper lip and the anterior two-thirds of the
tongue, floor of mouth and gums. They receive lymph from the upper and
lower teeth, from the anterior half of the nasal cavity and from the frontal
and maxillary and middle and anterior ethmoidal sinuses. Most of the
submandibular nodes drain into the jugulo-omohyoid node; a few drain into
the jugulo-diagastric node.
C: Buccal and mandibular nodes:
a small node lies isolated on the
baccinator muscle, another on the lower border of the mandible at the
anterior border of the masseter. They drain part of the cheek and lower
eyelid. Their efferents pass to the jugulo-digastric node.

The Superficial Lymph Nodes
Outer circle of nodes (continued)
D: Pre-auricular nodes:
these lie on and within the parotid gland: one
or two are subcutaneous. The subcutaneous nodes drain the skin of the
temple and vertex. forehead and eyelids. pinna and external acoustic
meatus.
These drain through the deep cervical fascia into supraclavicular nodes.
The deep nodes receive from the back of the orbit, from the infratemporal
fossa, and from the parotid gland itself.
They drain into the deep members of the deep group.
E. Occipital nodes:
these drain the posterior part of the scalp and
auricle. The efferents pass to the supraclavicular nodes.

The inner circle lies within the surrounding larynx,
trachea, and pharynx.
It comprises pre-tracheal, para-tracheal and
retro-pharyngeal LNs.
The pre-tracheal LNs drain the lower larynx,
trachea and thyroid isthmus.
The retro-pharyngeal LNs drain the soft palate,
posterior parts of hard palate and nose, as well as the
pharynx itself.
Tonsils, lingual tonsil, palatine tonsil and adenoids
sometimes called inner ring of waldeyer.
These then drain into the Deep Cervical LNs.

Deep Cervical Lymph Nodes:
found around the internal jugular vein from the base of the
skull to the root of the neck. They are formed of 3 groups:
I.
The jugulo-digastric
node lies below the posterior belly
of the digastric between the angle of the mandible and
the anterior border of sternomastoid.
II. The jugulo-omohyoid
node lies above the inferior belly
of the omohyoid, behind the jugular vein.
III. The supraclavicular
lymph nodes extend behind the
border of sternomastoid into the posterior triangle.
Lymph from the deep cervical nodes is collected into
the jugular lymph trunk.
This joins the thoracic duct on the left side: on the right
side, it usually opens independently into the internal
jugular or brachiocephalic vein.

Causes of cervical lymphadenopathy
1. Infection
Acute pyogenic (tonsillitis, dental extraction, middle ear infections, parotitis,
scalp infections)
Chronic
Non-specific (viral infection)
Specific
o Glandular fever (infectious mononucleosis, EBV infection)
o Tuberculosis
o Syphilis
o Toxoplasmosis
o Cat scratch fever
2. Neoplastic
• Metastatic secondary tumours from primary tumours of :
squamous carcinoma of nasopharynx, skin of head, neck, chest, and abdomen.
• Primary tumours:
Hodgkin's lymphoma (adult)
Non-Hodgkin's lymphoma (elderly)
Leukaemia (usually children and young adults)
3. Miscellaneous
Sarcoidosis

Enlarged Supraclavicular Lymph Nodes
take the name of the German
pathologist
Virchow
(1821-1902): the classical enlarged supraclavicular LN (of
Virchow) following metastasis from underlying gastric carcinoma is termed
Troisier's sign
(named after a French professor of pathology, 1844-1919).
Enlarged supraclavicular LN
is of great surgical interest. since it is usually due to
neoplastic lesions more than infective ones (the commonest cause of infective
enlargement of supraclavicular lymph nodes is pulmonary tuberculosis).
While most upper limb infection can cause epitrochlear and axillary LN enlargement,
infection of the middle finger and dorsum of the hand passes directly into the
supraclavicular LNs.
Other causes of enlargement include bronchogenic carcinoma (Pancoast tumor),
breast carcinoma, thyroid carcinoma(wrongly called ectopic thyroid),
oesophageal carcinoma, pharyngolaryngeal carcinoma, Hodgkin's and non-
Hodgkin's lymphoma. pancreatic carcinoma and testicular carcinoma
(particularly choriocarcinoma). Hypernephroma can also give rise to enlarged
supraclavicular nodes.
Superficial and Deep cervical lymph nodes ultimately drain into supraclavicular
lymph nodes. So any enlargement of these glands (due to infections or neoplasms
in the head and neck and upper limbs) will result in enlargement of the
supraclavicular lymph nodes. Enlargement of supraclavicular may be part of a
generalised lymphadenopathy due to leukemia, lymphoma and AIDS.
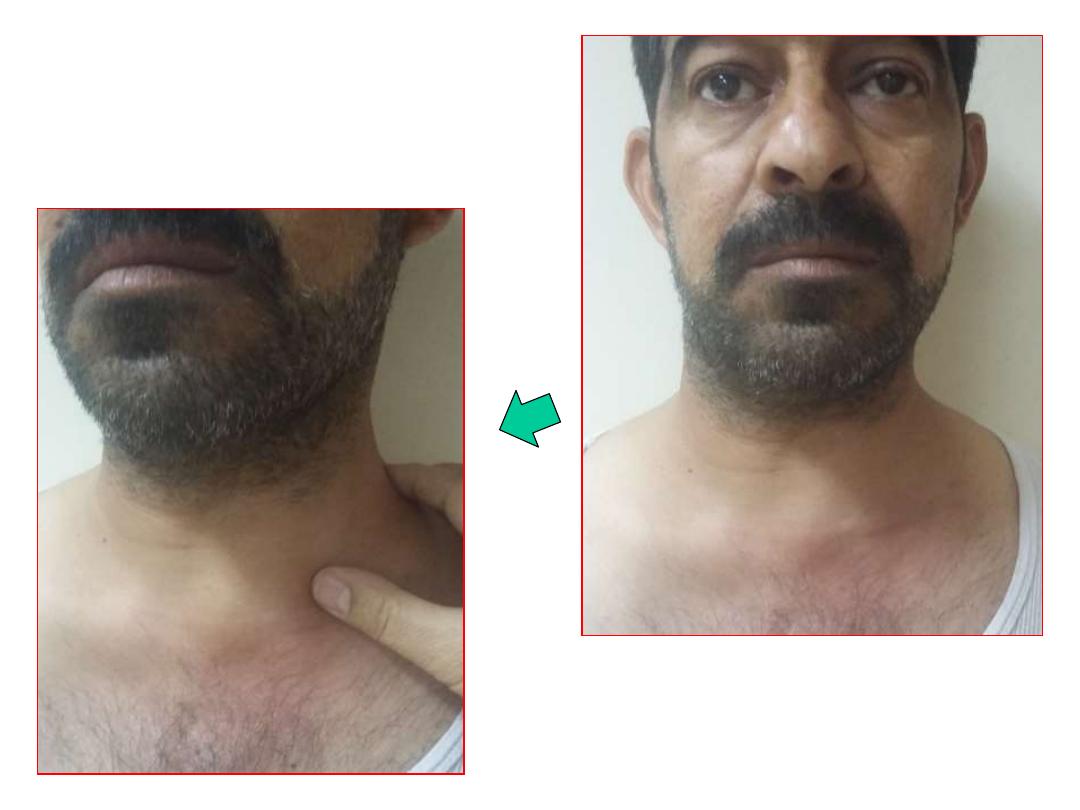
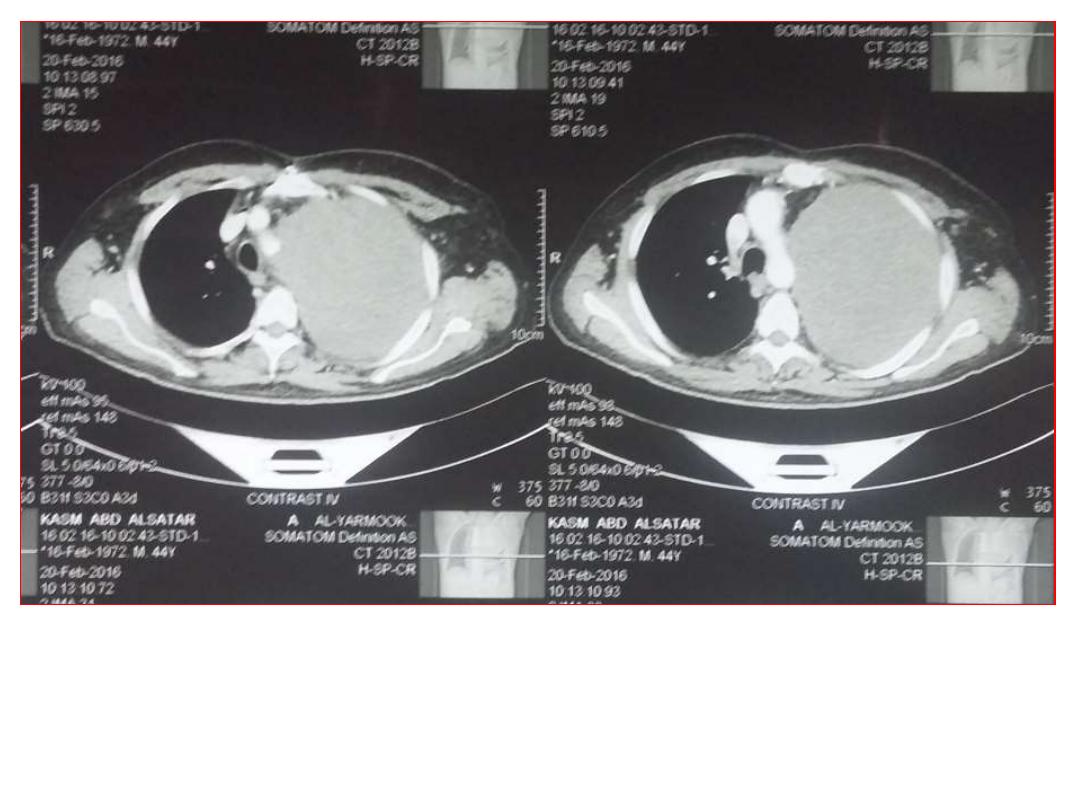

Careful history and meticulous physical examination can give the diagnosis in the
majority of cases. Complete ENT examination of postnasal space, oral cavity,
oropharynx and fibreoptic laryngoscopy. Examine other sites (axilla, epitrochlear,
inguinal, spleen, and liver).
Lymph nodes are tender and hot with evidence of infection (of the respiratory tract
and mouth). Cold matted lymph nodes are tuberculous.
Fixed stony-hard lymph nodes are metastatic in origin.
However, in lateral painless swellings that do not move with swallowing and have
a rubbery consistency, Hodgkin's lymphoma (in adults) and non-Hodgkin's
lymphoma (in the elderly) is most likely.
High ESR, Chest x-ray findings can be confirmed by Positive tuberculin test can
be diagnostic for tuberculosis in any patient with a cervical lymph node swelling. Past
infection with Eptein-Barr virus plays a role in some Hodgkin’s lymphoma patients.
Fine needle aspiration cytology biopsy is an important diagnostic tool, in the
presence of an experienced cytologist.
Cervical lymph node biopsy is the last investigative tool which will solve the
problems of diagnosis. CT scan, ultrasound, radioactive isotope scan, and
positron emission tomography (PET) may be required to elucidate the nature of
cervical swelling, staging, assessment of response, and direction of treatment..
Diagnosis of a Cervical Swelling
(due to Lymph Node enlargement)
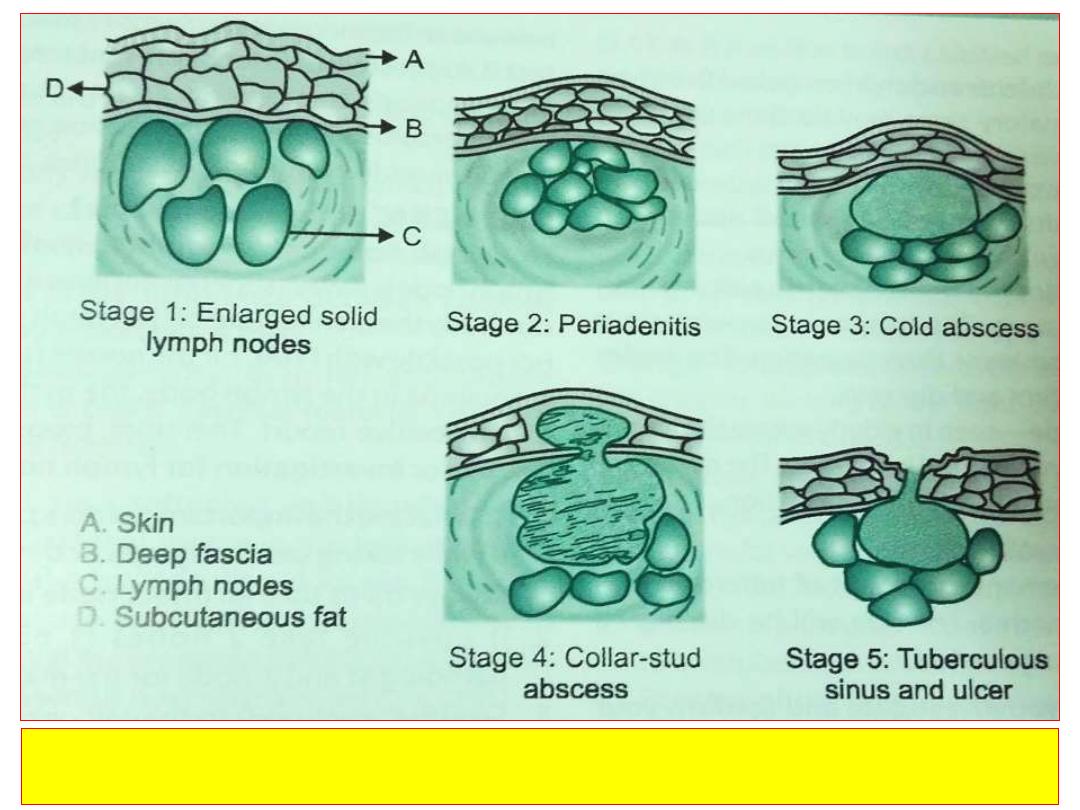
Tuberculosis lymphadenitis stages in order

Treatment of tuberculosis: in 2 phases
Initial phase for 2 months.
At least 3 drugs are used to reduce the population of
viable bacteria rapidly and to prevent the emergence of drug-resistant bacteria.
Drugs are: Isoniazid 300 mg daily for adults(for children 10 mg/k daily).
Pyridoxine 10mg daily should be given prophylactically from the start of treatment to
counteract peripheral neuropathy induced by isoniazid .
Rifampicin 450 mg daily, depending on the adult's body weight whether under or
over 50 kg respectively (for children 10 mg/kg daily). Rifampicin may cause liver
dysfunction.
Pyrazinamide (bactericidal) 1.5-2 g daily depending on an adult's body weight
whether under or over 50 kg respectively(for children 35 mg/kg daily).
Additional drugs: ethambutol (15 mg/kg daily: can cause colour blindness) is
added if drug resistance is thought likely. Streptomycin (i.m. injection of 1 g daily;
can cause oto- and nephrotoxicity) is now rarely used in UK, but it may be added if
bacilli are resistant to isoniazid.
Continuation phase for 4 months.
Two drugs, isoniazid and rifampicin(for a
total of six months each), are the key components of the second phase of any
antituberculosis regimen. Longer treatment may be necessary for bone and joint
infections, for meningitis, or for resistant organisms.

Thanks for Participation
